| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 10 mM * 1 mL in DMSO |
|
||
| 1mg |
|
||
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| Other Sizes |
|
| 靶点 |
MMP-3 (IC50 = 3 nM); MMP-1 (IC50 = 5 nM); MMP-2 (IC50 = 6 nM); MMP-14 (IC50 = 9 nM); MMP-7 (IC50 = 13 nM)
Marimastat (BB-2516) is a broad-spectrum oral matrix metalloproteinase (MMP) inhibitor, with IC50 values in cell-free assays: MMP-1 (collagenase-1): 3 nM, MMP-2 (gelatinase A): 1.5 nM, MMP-3 (stromelysin-1): 2 nM, MMP-9 (gelatinase B): 2.5 nM [1] - It inhibits membrane-type MMPs (MT1-MMP/MMP-14) with an IC50 of 4 nM, and shows no significant activity against serine proteases (trypsin, plasmin) or cysteine proteases (cathepsin B) at concentrations up to 1 μM [3,5] |
|---|---|
| 体外研究 (In Vitro) |
Marimastat (100 nM) 显着抑制 U251、U87、GBM39 和 GBM43 肿瘤细胞中 MMP14 的表达。 Marimastat 特异性抑制神经胶质瘤细胞的生长,但对正常人星形胶质细胞 (NHA) 没有影响。 Marimastat 早期下调 Notch 靶基因的表达,例如 Hes1 和 Hes5。激酶测定:用 1 mM 乙酸 4-氨基苯汞在 37°C 下激活重组人 MMP2 1 小时。 1 μM 淬灭荧光 MMP 底物 (7-甲氧基香豆素-4-基)乙酰基-Pro-Leu-Gly-Leu-[3-(2,4-二硝基苯基)-L-2,3-二氨基丙酰基] 的裂解率-Ala-Arg-NH2 在 96 孔荧光板中于 37°C 下使用 320 nm 激发滤光片和 405 nm 100 mM Tris-HCl (pH 7.5)、100 mM NaCl、10 mM CaCl2、0.05% Brij 35 进行测量存在增加抑制剂浓度的情况下的发射过滤器。使用 GraphPad Prism 5.0 软件完成曲线拟合和 IC50 计算。细胞测定:在源自人神经胶质瘤细胞系 U251 和 GaMG 的肿瘤球体与 RBA 的共培养中,marimastat 在 10 μM 浓度下强烈抑制肿瘤侵袭。 Marimastat (10 μM) 可显着降低细胞增殖 54%,并且在 50 μM 的浓度下可在 6 天内完全抑制细胞生长。此外,marimastat (10 μM) 可使 U251 球体生长减少 65%。
在人非小细胞肺癌A549细胞中:50 nM Marimastat 处理72小时可抑制细胞增殖约75%(MTT法),诱导约35%细胞凋亡(Annexin V-FITC/PI染色),使Bcl-2蛋白减少约60%(Western blot);100 nM可使caspase-9活性增加约2.2倍[2] - 在人乳腺癌MDA-MB-231细胞中:25 nM Marimastat 处理48小时可抑制细胞侵袭约80%(Matrigel Transwell实验),阻断MMP-9明胶酶活性约75%(酶谱法);50 nM可下调MMP-14 mRNA约65%(qRT-PCR)[3] - 在小鼠黑色素瘤B16F10细胞中:75 nM Marimastat 处理24小时可抑制细胞迁移约70%(划痕愈合实验),减少MMP-2分泌约60%(ELISA)[5] - 在人胰腺癌PANC-1细胞中:100 nM Marimastat 处理96小时可减少肿瘤球形成(癌症干细胞标志物)约55%(软琼脂实验),下调CD44表达约50%(流式细胞术)[4] - 在人结直肠癌HCT116细胞中:50 nM Marimastat 处理72小时可抑制TNF-α诱导的NF-κB激活约60%(荧光素酶实验),减少IL-8分泌约55%(ELISA)[6] |
| 体内研究 (In Vivo) |
在原位口腔鳞状细胞癌种植模型中,通过渗透泵给予马马司他(150 mg/kg/天,po)显着抑制颈部淋巴结转移和MMP-2的激活,并且比对照组具有显着更好的生存率。 Marimastat 降低多囊人和大鼠胆管细胞的 MMP 过度活跃,并阻止 PCK 胆管细胞的囊性扩张。用马马司他长期治疗 8 周大的 PCK 大鼠可抑制肝囊肿发生和纤维化。
在荷A549异种移植瘤的裸鼠(皮下注射5×10⁶个细胞)中:每日两次口服25 mg/kg Marimastat,持续28天,肿瘤体积较溶剂对照组减少约50%,重量减少约45%;免疫组化显示活化caspase-3阳性细胞增加约60%[2] - 在B16F10肺转移模型C57BL/6小鼠(静脉注射1×10⁵个细胞)中:每日一次口服20 mg/kg Marimastat,持续21天,肺转移灶减少约80%(苏木精-伊红染色计数)[5] - 在HCT116肝转移模型裸鼠(脾内注射2×10⁶个细胞)中:每日一次口服30 mg/kg Marimastat,持续35天,肝转移结节减少约70%,肿瘤中MMP-9表达减少约65%(Western blot)[6] - 在原位胰腺癌(AR42J细胞)大鼠模型中:每日两次口服25 mg/kg Marimastat,持续21天,抑制肿瘤向周围胰腺侵袭约60%(组织病理学分析)[4] |
| 酶活实验 |
在 37°C 下,用 1 mM 4-氨基苯汞乙酸盐激活重组人 MMP2 1 小时。测量了猝灭荧光 MMP 底物 1-甲氧基香豆素-4-基的裂解率。 Gly-Leu-乙酰基-Pro-Leu-[3-(2,4-二硝基苯基)-L-2,3-二氨基丙酰基] 在 37°C 下,在 96 孔荧光测定板中进行 Ala-Arg-NH2 的测量。在抑制剂浓度不断增加的情况下,使用 320 nm 激发滤光片和 405 nm 发射滤光片对 100 mM Tris-HCl (pH 7.5)、100 mM NaCl、10 mM CaCl2 和 0.05% Brij 35 进行测试。 GraphPad Prism 5.0软件用于IC50计算和曲线拟合。
MMP-2/MMP-9明胶酶活性检测流程(基于[1]):人重组MMP-2/MMP-9在缓冲液(50 mM Tris-HCl pH 7.5,10 mM CaCl₂,0.05% Brij-35)中用APMA(对氨基苯汞乙酸)激活。酶与荧光明胶底物(DQ-gelatin)及Marimastat(0.1~10 nM)在37°C孵育2小时。检测激发波长485 nm/发射波长535 nm处的荧光强度,经剂量-反应拟合计算IC50[1] - MT1-MMP激酶实验流程(基于[3]):人重组MT1-MMP与荧光肽底物(Mca-Arg-Pro-Lys-Pro-Tyr-Ala-Nva-Trp-Met-Lys(Dnp)-NH₂)混合于缓冲液(50 mM HEPES pH 7.5,10 mM CaCl₂)中。加入Marimastat(0.5~10 nM),37°C孵育1小时。检测荧光强度,通过四参数回归确定IC50[3] |
| 细胞实验 |
在人胶质瘤细胞系 U251 和 GaMG 与浓度为 10 μM 的 RBA 的肿瘤球体共培养物中,Marimastat 显着减弱肿瘤侵袭。 Marimastat (10 μM) 在 50 μM 浓度下可在六天内完全抑制细胞生长,并显着降低 54% 的细胞增殖。此外,marimastat (10 μM) 65% 抑制 U251 球体的生长。
A549细胞凋亡实验流程(基于[2]):A549细胞以2×10⁴细胞/孔接种,用10~200 nM Marimastat 处理72小时。收集细胞,用Annexin V-FITC/PI染色,流式细胞术量化凋亡细胞;用荧光试剂盒(激发400 nm/发射505 nm)检测caspase-9活性[2] - MDA-MB-231细胞侵袭实验流程(基于[3]):MDA-MB-231细胞用含5~100 nM Marimastat 的无血清DMEM重悬,以5×10⁴细胞/孔接种于Matrigel包被的Transwell上室,下室加入10% FBS(趋化因子)。48小时后去除上室未侵袭细胞,固定并结晶紫染色,显微镜下计数侵袭细胞[3] - HCT116细胞NF-κB实验流程(基于[6]):HCT116细胞转染NF-κB-荧光素酶质粒。转染24小时后,用10~100 nM Marimastat 处理细胞1小时,再用10 ng/mL TNF-α刺激6小时。裂解细胞后检测荧光素酶活性,归一化至β-半乳糖苷酶(内参)[6] |
| 动物实验 |
使用套管针将2 mm²的已建立的SCC-1组织皮下注射到3月龄雌性裸鼠的侧腹部。当肿瘤直径达到5-6 mm时进行治疗。将小鼠随机分为8组,分别接受以下四种治疗:(1)对照组,(2)单独使用马立马司他组,(3)顺铂联合放疗组,(4)马立马司他+顺铂+放疗联合组。每只小鼠均使用含有二甲基亚砜(DMSO)的渗透泵,持续14天,作为溶剂和渗透泵的对照。使用同一渗透泵,将200 μL马立马司他与DMSO混合,在治疗开始10天后,对接受马立马司他治疗的小鼠每日给予8.7 mg/kg的剂量。在第 8、12、16 和 20 天,铅屏蔽动物接受 8 Gy 的 60Co 辐射照射,分 4 次照射。由于先前的研究表明 7.5 Gy (7,500 rad) 的剂量可以抑制肿瘤生长但不足以治愈,因此选择 8 Gy 的剂量。在每次照射前 1 小时,腹腔注射顺铂 (3 mg/kg),共注射 4 次。在接下来的 32 天内,每两周测量一次肿瘤大小。通过小鼠体重来追踪潜在的治疗毒性。在每个治疗组中,测量肿瘤大小(表面积等于两个最大直径的乘积)和消退率。32 天后,取出肿瘤进行免疫组织化学分析。选择第32天进行统计分析,是因为对照组动物死亡,以及出现临床症状的动物被实施安乐死。裸鼠A549异种移植模型(引自[2]):将5×10⁶个A549细胞(0.1 mL PBS + 50% Matrigel)皮下注射到6-8周龄雌性裸鼠的右侧腹部。当肿瘤体积达到约100 mm³时,将小鼠分为两组:(1)马立马司他组:25 mg/kg马立马司他溶于0.5%甲基纤维素溶液中,每日两次灌胃;(2)载体组:0.5%甲基纤维素溶液。每3天测量一次肿瘤体积(V=0.5×长×宽²)。小鼠于第 28 天处死,用于肿瘤重量和免疫组织化学分析 [2]
- 小鼠 B16F10 转移模型(引自 [5]):雄性 C57BL/6 小鼠(8-10 周龄)经静脉注射 1×10⁵ 个 B16F10 细胞(0.2 mL PBS)。注射 24 小时后,小鼠每日口服一次马立马司他(Marimastat,20 mg/kg,溶于 10% 乙醇 + 90% 生理盐水),持续 21 天。对照组小鼠口服 10% 乙醇 + 90% 生理盐水。第 22 天处死小鼠;肺组织经固定、切片后进行转移灶计数[5] - 裸鼠HCT116肝转移模型(引自[6]):将2×10⁶个HCT116细胞(0.1 mL PBS)脾内注射到6-8周龄的雌性裸鼠体内。注射后7天,小鼠每日口服一次马立马司他(Marimastat,30 mg/kg,溶于0.5%羧甲基纤维素),持续35天。对照组小鼠口服0.5%羧甲基纤维素。于第42天处死小鼠;收集肝脏进行转移结节计数和Western blot(MMP-9)分析[6] |
| 药代性质 (ADME/PK) |
在健康人类志愿者中:口服Marimastat(10 mg,每日两次)的口服生物利用度约为25%,血浆消除半衰期(t₁/₂)约为6.5小时,血浆峰浓度(Cmax)为0.8 μg/mL(给药后1.5小时达到)[1]
- 在雄性Sprague-Dawley大鼠中:口服Marimastat(25 mg/kg)的t₁/₂约为4.8小时,分布容积(Vd)约为2.2 L/kg,总清除率约为0.3 L/h/kg[1] - Marimastat由肝细胞色素P450 3A4(CYP3A4)代谢;口服剂量约60%以代谢物形式经粪便排出,约15%经尿液排出(原药:<5%)[1] - 在携带A549异种移植瘤的裸鼠中,Marimastat的肿瘤/血浆浓度比约为8:1(口服给药后2小时测定)[2] |
| 毒性/毒理 (Toxicokinetics/TK) |
在一项为期 28 天的大鼠毒性研究中(口服 Marimastat,剂量分别为 5、25、100 mg/kg/天):未观察到不良反应剂量 (NOAEL) 为 25 mg/kg/天;在 100 mg/kg/天时,6 只大鼠中有 4 只出现轻度关节僵硬(可逆),血清 ALT/AST、肌酐或 BUN 无变化 [1]
- 在人体 II 期试验中:常见不良事件 (AE) 包括肌肉骨骼疼痛 (28%)、疲劳 (18%) 和恶心 (12%);无严重肝毒性或肾毒性[1,2] - 在人正常细胞(MRC-5成纤维细胞、HUVECs)中:浓度高达500 nM的Marimastat处理72小时未见明显细胞毒性(细胞活力>90% vs. 溶剂对照组,MTT法)[2,6] - Marimastat在人和大鼠中的血浆蛋白结合率约为95%(超滤法)[1] |
| 参考文献 | |
| 其他信息 |
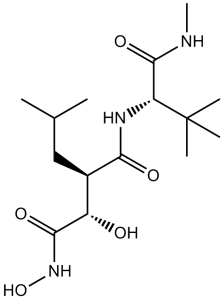
马立马司他是一种仲酰胺,由(2R)-2-[(1S)-1-羟基-2-(羟基氨基)-2-氧代乙基]-4-甲基戊酸的羧基与N,3-二甲基-L-缬氨酰胺的α-氨基发生甲氧基缩合反应生成。它是一种抗肿瘤药物和基质金属蛋白酶抑制剂。它是一种仲酰胺和羟肟酸类化合物。
马立马司他用于癌症治疗,是一种血管生成和转移抑制剂。作为血管生成抑制剂,它限制血管的生长和生成。作为抗转移药物,它阻止恶性细胞突破基底膜。 马立马司他是一种口服有效的合成羟肟酸类药物,具有潜在的抗肿瘤活性。马立马司他与基质金属蛋白酶 (MMP) 活性位点中的锌(II)离子共价结合,从而抑制MMP的活性,诱导细胞外基质降解,并抑制血管生成、肿瘤生长、侵袭和转移。该药物还可能抑制肿瘤坏死因子-α转化酶 (TACE),TACE是一种参与肿瘤坏死因子-α (TNF-α) 生成的酶,TNF-α可能在某些恶性肿瘤以及关节炎和脓毒症的发生发展中发挥作用。(NCI04) 药物适应症 用于治疗多种癌症 作用机制 马立马司他是一种广谱基质金属蛋白酶抑制剂。它模拟天然MMP底物的肽结构,并与基质金属蛋白酶结合,从而阻止这些蛋白酶对基底膜的降解。这种抗蛋白酶作用可阻止形成新血管所需的内皮细胞迁移。抑制MMPs还能阻止肿瘤细胞进入和离开现有血细胞,从而阻止转移。 药效学 用于癌症治疗,它是一种血管生成和转移抑制剂。作为血管生成抑制剂,它限制血管的生长和生成。作为一种抗转移药物,它能阻止恶性细胞突破基底膜。 Marimastat (BB-2516) 是一种口服广谱 MMP 抑制剂,是 Batimastat 的第二代替代药物(克服了 Batimastat 口服生物利用度低的问题)[1,5] - 其作用机制包括与 MMP 的含 Zn²⁺ 活性位点结合,抑制细胞外基质 (ECM) 降解,并阻断肿瘤细胞的侵袭、迁移和血管生成[1,2,5] - 它已进入非小细胞肺癌、胰腺癌和黑色素瘤的 III 期临床试验;然而,由于剂量限制性肌肉骨骼毒性(关节僵硬)以及与化疗相比疗效不佳,该药物的研发被迫中止[1,2,5]。 - Marimastat 与吉西他滨具有协同作用:50 nM Marimastat + 10 nM 吉西他滨可使 PANC-1 细胞活力降低约 85%(而单独使用吉西他滨时约为 40%)[4]。 |
| 分子式 |
C15H29N3O5
|
|
|---|---|---|
| 分子量 |
331.41
|
|
| 精确质量 |
331.21
|
|
| 元素分析 |
C, 54.36; H, 8.82; N, 12.68; O, 24.14
|
|
| CAS号 |
154039-60-8
|
|
| 相关CAS号 |
|
|
| PubChem CID |
119031
|
|
| 外观&性状 |
White to off-white solid powder
|
|
| 密度 |
1.1±0.1 g/cm3
|
|
| 熔点 |
148℃
|
|
| 折射率 |
1.499
|
|
| LogP |
-0.16
|
|
| tPSA |
127.76
|
|
| 氢键供体(HBD)数目 |
5
|
|
| 氢键受体(HBA)数目 |
5
|
|
| 可旋转键数目(RBC) |
8
|
|
| 重原子数目 |
23
|
|
| 分子复杂度/Complexity |
431
|
|
| 定义原子立体中心数目 |
3
|
|
| SMILES |
O([H])[C@]([H])(C(N([H])O[H])=O)[C@]([H])(C(N([H])[C@]([H])(C(N([H])C([H])([H])[H])=O)C(C([H])([H])[H])(C([H])([H])[H])C([H])([H])[H])=O)C([H])([H])C([H])(C([H])([H])[H])C([H])([H])[H]
|
|
| InChi Key |
OCSMOTCMPXTDND-OUAUKWLOSA-N
|
|
| InChi Code |
InChI=1S/C15H29N3O5/c1-8(2)7-9(10(19)13(21)18-23)12(20)17-11(14(22)16-6)15(3,4)5/h8-11,19,23H,7H2,1-6H3,(H,16,22)(H,17,20)(H,18,21)/t9-,10+,11-/m1/s1
|
|
| 化学名 |
(2R,3S)-N-[(2S)-3,3-dimethyl-1-(methylamino)-1-oxobutan-2-yl]-N',3-dihydroxy-2-(2-methylpropyl)butanediamide
|
|
| 别名 |
BB 2516; TA-2516; Marimastat; BB-2516; BB2516; TA2516; TA 2516
|
|
| HS Tariff Code |
2934.99.9001
|
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
|
|||
|---|---|---|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: ≥ 2.5 mg/mL (7.54 mM) (饱和度未知) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。
例如,若需制备1 mL的工作液,可将100 μL 25.0 mg/mL澄清DMSO储备液加入到400 μL PEG300中,混匀;然后向上述溶液中加入50 μL Tween-80,混匀;加入450 μL生理盐水定容至1 mL。 *生理盐水的制备:将 0.9 g 氯化钠溶解在 100 mL ddH₂O中,得到澄清溶液。 配方 2 中的溶解度: ≥ 2.5 mg/mL (7.54 mM) (饱和度未知) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 例如,若需制备1 mL的工作液,可将 100 μL 25.0 mg/mL澄清DMSO储备液加入900 μL 20% SBE-β-CD生理盐水溶液中,混匀。 *20% SBE-β-CD 生理盐水溶液的制备(4°C,1 周):将 2 g SBE-β-CD 溶解于 10 mL 生理盐水中,得到澄清溶液。 View More
配方 3 中的溶解度: ≥ 2.5 mg/mL (7.54 mM) (饱和度未知) in 10% DMSO + 90% Corn Oil (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 配方 4 中的溶解度: 50% DMSO+PBS: 30mg/mL 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 3.0174 mL | 15.0871 mL | 30.1741 mL | |
| 5 mM | 0.6035 mL | 3.0174 mL | 6.0348 mL | |
| 10 mM | 0.3017 mL | 1.5087 mL | 3.0174 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT00003011 | Completed | Drug: marimastat Drug: Placebo |
Lung Cancer | NCIC Clinical Trials Group | January 31, 1997 | Phase 3 |
| NCT00002911 | Completed | Drug: marimastat | Lung Cancer | ILEX Oncology Services, Incorporated |
December 1996 | Phase 3 |
| NCT00003010 | Completed | Drug: marimastat | Breast Cancer | Eastern Cooperative Oncology Group |
December 2, 1997 | Phase 3 |
| NCT00261391 | Completed | Drug: Marimastat | Vascular Anomalies | Boston Children's Hospital | October 2000 | Phase 1 |