| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| Other Sizes |
|
| 靶点 |
In patch clamp hERG tests, betrixaban (PRT054021) exhibits an IC50 of 8.9 μM[1]. Betrixaban exhibits an IC50 and a Ki for plasma kallikrein of 6.3 μM and 3.5 μM, respectively[1]. Compared to all other drugs (hERG Ki⩽0.5 μM), betrixaban (hERG Ki 1.8 μM) shows noticeably less hERG activity[1]. Betrixaban inhibits the production of thrombin (5–25 ng/mL)[3].
|
|---|---|
| 体外研究 (In Vitro) |
在膜片钳 hERG 测试中,betrixaban (PRT054021) 的 IC50 为 8.9 μM[1]。 Betrixaban 对血浆激肽释放酶的 IC50 和 Ki 分别为 6.3 μM 和 3.5 μM[1]。与所有其他药物 (hERG Ki⩽0.5 μM) 相比,betrixaban (hERG Ki 1.8 μM) 显示出明显较低的 hERG 活性[1]。 Betrixaban 抑制凝血酶的产生 (5–25 ng/mL)[3]。
在全血凝血酶原酶抑制实验中,Betrixaban显示出剂量依赖性的对血小板介导的凝血酶原酶活性的抑制,这与其作为直接FXa抑制剂的作用机制一致。 在组织因子诱导的凝血酶生成实验中,浓度为5–25 ng/mL的Betrixaban对凝血酶生成的抑制程度,与磺达肝癸钠2.5 mg达到的谷浓度和峰浓度水平相当。 使用膜片钳技术的临床前毒理学研究表明,Betrixaban不是hERG钾通道的强效抑制剂(IC50 = 8.9 μM)。其hERG IC50与人体预期峰血浆浓度的比值提供了30倍的安全边际,防止了显著的hERG通道抑制。 [3] |
| 体内研究 (In Vivo) |
在犬中,贝曲西班的口服生物利用度为 51.6%(0.5 mg/kg,静脉注射;2.5 mg/kg,口服)[1]。在猴子中,贝曲西班的口服生物利用度为 58.7%(0.75 mg/kg,静脉注射;7.5 mg/kg,口服)[1]。 R-Antidote 可逆转贝曲西班介导的全血 INR 升高。 30 分钟静脉输注后,贝曲西班的总血浆浓度为 0.2±0.01 μM,其中 40%±7.2% 的抑制剂保持未结合。 r-Antidote 递送后,未结合抑制剂的比例下降至 0.3%±0.1%,而总血浆浓度上升至 2.0±0.4 μM[2]。当用于棉线上血栓积聚的兔腹部腔静脉模型时,贝曲西班 (3 mg/kg) 对血栓质量的抑制作用与依诺肝素 1.6 mg/kg 几乎相同(76% 与 96% 抑制作用)[3]。在大鼠颈动脉的氯化铁损伤模型中,贝曲西班 (19.1 mg/kg) 至少与依诺肝素 7.6 mg/kg 和氯吡格雷 3 mg/kg/d 一样有效(90% vs. 70% vs. 80% 通畅率)分别)保持通畅[3]。
在兔腹部下腔静脉血栓形成模型中,3 mg/kg剂量的Betrixaban对血栓质量的抑制(76%)与依诺肝素1.6 mg/kg(96%)几乎相当。 在啮齿动物氯化铁颈动脉损伤模型中,19.1 mg/kg的Betrixaban在维持动脉通畅性方面(90%)至少与依诺肝素7.6 mg/kg(70%)和氯吡格雷3 mg/kg/天(80%)同样有效。 在狒狒动静脉分流血栓形成模型中,Betrixaban显示出对静脉侧和动脉侧放射性标记血小板沉积的剂量依赖性抑制。0.05–0.49 mg/kg的剂量范围产生的血浆浓度为7–83 ng/mL,导致分流静脉侧血小板沉积抑制30%–90%。 [3] |
| 酶活实验 |
使用体外凝血实验评估了Betrixaban的抗凝作用及机制。在全血中,测量了其抑制凝血酶原酶活性(将凝血酶原转化为凝血酶的复合物)的能力,显示出剂量依赖性的抑制。
在血浆中进行了组织因子诱导的凝血酶生成实验。将Betrixaban以指定浓度(5–25 ng/mL)加入,测量随时间推移对凝血酶生成的抑制,并与标准剂量磺达肝癸钠的效果进行比较。 使用重组酶进行酶学测定,确定了Betrixaban对因子Xa的抑制常数(Ki)和半数抑制浓度(IC50)。Betrixaban显示出对FXa的强效和选择性抑制。 [3] |
| 动物实验 |
1 mg/kg;口服 大鼠 在三种动物模型中评估了贝曲沙班的抗血栓疗效。在兔腹腔静脉模型中,在棉线上诱导血栓形成,然后静脉注射药物。在啮齿动物氯化铁颈动脉损伤模型中,通过局部应用氯化铁诱导血栓形成,然后给药。在狒狒动静脉分流模型中,在股动脉和股静脉之间放置外部分流管,并在静脉给药后使用放射性标记血小板监测血小板沉积。未提供具体的药物制剂信息。[3] |
| 药代性质 (ADME/PK) |
吸收、分布和排泄
贝曲沙班在80毫克剂量下吸收迅速。健康人口服给药后3-4小时内即可达到血浆峰浓度。口服生物利用度为34%,且会因进食而降低。具体而言,与空腹状态相比,低脂餐后Cmax和AUC平均分别降低70%和61%,高脂餐后则分别降低50%和48%,这种影响在进食后6小时内仍然明显。 据报道,贝曲沙班主要经胃肠道排泄,研究表明,高达85%的贝曲沙班经粪便排出,仅有11%经尿液排出。 表观分布容积为32 L/kg。 贝曲沙班的肾清除率极低(仅为给药剂量的5-7%)。 代谢/代谢物 贝曲沙班的主要特点之一是其肝脏代谢极低(<1%),从而避免了肝功能损害时可能发生的药物蓄积。在人血浆中,原形贝曲沙班是主要存在形式,其次是两种不依赖CYP水解酶的非活性代谢物(15-18%)。由于肝脏代谢极少,因此不太可能与CYP450抑制剂或激动剂发生药物相互作用。 生物半衰期 贝曲沙班的半衰期较长,为19-27小时。 健康志愿者口服80毫克贝曲沙班后,贝曲沙班迅速吸收,3-4小时内达到血浆峰浓度(Tmax)。 口服生物利用度为34%。同时摄入脂肪类食物会使峰浓度 (Cmax) 和曲线下面积 (AUC) 降低约 50%。 约 60% 的贝曲沙班与血浆蛋白结合。 贝曲沙班主要以原形经肝胆途径排泄至粪便(占给药剂量的 82%–89%),可能由 P-糖蛋白 (P-gp) 外排泵介导。肾清除率极低,仅占口服剂量的 5%–7%。 贝曲沙班经细胞色素 P450 (CYP450) 酶的肝脏代谢极少 (<1%),且不诱导或抑制 CYP450。 末端消除半衰期 (t1/2) 为 37 小时。贝曲沙班的药效半衰期(抗凝血作用减弱50%所需的时间)约为20小时。 贝曲沙班的血浆峰谷浓度比值较低。[3] |
| 毒性/毒理 (Toxicokinetics/TK) |
肝毒性
在注册研究中,接受贝曲沙班治疗的患者中有 1% 至 2% 出现血清转氨酶升高超过正常值上限 (ULN) 3 倍,接受依诺肝素治疗的对照组受试者中也有类似比例出现这种情况。同样,接受贝曲沙班治疗的对照组受试者中有 0.6% 出现转氨酶水平升高超过 ULN 5 倍,接受依诺肝素治疗的对照组受试者中有 0.4% 出现这种情况。 可能性评分:E(未经证实但怀疑是临床上明显的肝损伤的罕见原因)。 妊娠和哺乳期用药 ◉ 哺乳期用药概述 贝曲沙班已停止在美国销售。由于目前尚无关于哺乳期使用贝曲沙班的信息,且该药物可口服吸收,因此建议选择其他药物,尤其是在哺乳新生儿或早产儿时。 ◉ 对母乳喂养婴儿的影响 截至修订日期,未找到相关的已发表信息。 ◉ 对泌乳和母乳的影响 截至修订日期,未找到相关的已发表信息。 蛋白结合 据报道,贝曲沙班的蛋白结合率约为 60%。 抗凝剂的主要毒性风险是出血。在 II 期临床试验中,贝曲沙班组的临床相关出血发生率低于对照组(依诺肝素或华法林)。在 EXPLORE-Xa 试验中,与华法林相比,贝曲沙班组(尤其是 80 mg 剂量组)胃肠道不良事件(包括腹泻、恶心、消化不良和呕吐)的发生率更高。大多数不良事件为轻度。未观察到明显的肝毒性信号。在 II 期研究中,贝曲沙班组丙氨酸氨基转移酶升高(>正常值上限 3 倍)的发生率不高于对照组,且升高为短暂性。未报告胆红素升高病例。 尽管贝曲沙班源自具有hERG通道抑制潜力的化合物类别,但对健康志愿者进行的全面QTc间期研究以及临床试验中的心电图监测表明,贝曲沙班(单次剂量高达140 mg)不会引起超过监管阈值的具有临床意义的QTc间期延长。 作为P-gp的底物,与强效P-gp抑制剂(例如酮康唑)合用可使贝曲沙班的血浆浓度增加约两倍。[3] |
| 参考文献 |
|
| 其他信息 |
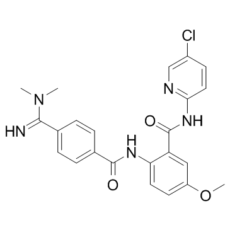
贝曲沙班是一种仲酰胺类化合物,由4-(N,N-二甲基氨基甲酰亚胺基)苯甲酸的羧基与2-氨基-N-(5-氯吡啶-2-基)-5-甲氧基苯甲酰胺的氨基缩合而成。它是一种合成抗凝血剂,靶向凝血级联反应中的活化因子Xa。它既是抗凝血剂,也是EC 3.4.21.6(凝血因子Xa)抑制剂。它属于胍类、苯甲酰胺类、仲酰胺类、单氯吡啶类和单甲氧基苯类化合物。
贝曲沙班是一种非维生素K拮抗剂口服抗凝血剂,其作用机制是通过竞争性可逆抑制因子Xa。由于其对hERG通道的亲和力低,同时又能保持其因子Xa抑制能力,因此在所有先导化合物中脱颖而出。贝曲沙班(Betrixaban)目前由Portola Pharmaceuticals Inc.公司研发,用于预防中度至重度活动受限或存在其他静脉血栓栓塞(VTE)风险的成年患者发生VTE。VTE可表现为深静脉血栓形成或肺栓塞,是住院患者可预防死亡的主要原因之一。 贝曲沙班是一种Xa因子抑制剂。其作用机制是作为Xa因子抑制剂。 贝曲沙班是一种口服抗凝剂,也是Xa因子的直接抑制剂,用于降低因急性疾病住院且静脉血栓形成风险高的患者发生深静脉血栓形成和肺栓塞的风险。贝曲沙班与治疗期间血清转氨酶升高发生率较低有关,但尚未发现与临床上明显的肝损伤病例相关。 贝曲沙班是一种口服有效的凝血因子Xa(活化因子X)抑制剂,具有抗凝血活性。贝曲沙班主要以原形经胆汁排泄,半衰期约为19小时。 药物适应症 贝曲沙班适用于中度至重度活动受限患者或符合静脉血栓栓塞症(VTE)风险标准的患者,用于预防VTE。 FDA标签 预防静脉血栓栓塞症 预防静脉血栓栓塞症 作用机制 贝曲沙班是一种不依赖辅因子的Xa因子直接抑制剂,可抑制游离的和与凝血酶原酶结合的Xa因子。 药效学 贝曲沙班是一种口服抗凝剂,其作用机制是通过抑制凝血酶生成,而不直接影响血小板聚集。 贝曲沙班是一种口服、直接且选择性凝血因子Xa (FXa) 抑制剂。 其最显著的药理学特征是肾脏排泄极少、经CYP450肝脏代谢极少以及半衰期长(约37小时)。 它已在II期临床试验中评估了其在全膝关节置换术后预防静脉血栓栓塞症(EXPERT试验)和在房颤患者中预防卒中(EXPLORE-Xa试验)的疗效。 目前正在进行一项III期临床试验(APEX),评估长期使用贝曲沙班(每日一次,每次80 mg,持续35-42天)与短期使用依诺肝素在急性重症高危内科患者中预防静脉血栓栓塞症的疗效。 由于其肾脏清除率极低,贝曲沙班有望用于严重肾功能不全(肌酐清除率<30 mL/min)的患者,这类患者通常被排除在其他新型口服抗凝药(NOAC)试验之外。 目前尚无获批的解毒剂。 贝曲沙班。其较长的半衰期可能会在出血或需要紧急手术的情况下造成问题,不过目前正在共同研发一种解毒剂(安德沙奈特α)。[3] |
| 分子式 |
C23H22CLN5O3
|
|---|---|
| 分子量 |
451.91
|
| 精确质量 |
451.141
|
| CAS号 |
330942-05-7
|
| 相关CAS号 |
Betrixaban-d6;2098655-51-5;Betrixaban maleate;936539-80-9;Betrixaban hydrochloride;2099719-47-6
|
| PubChem CID |
10275777
|
| 外观&性状 |
Light yellow to yellow solid powder
|
| 密度 |
1.3±0.1 g/cm3
|
| 熔点 |
200-212 ºC
|
| 折射率 |
1.629
|
| LogP |
2.93
|
| tPSA |
110.9
|
| 氢键供体(HBD)数目 |
3
|
| 氢键受体(HBA)数目 |
5
|
| 可旋转键数目(RBC) |
7
|
| 重原子数目 |
32
|
| 分子复杂度/Complexity |
668
|
| 定义原子立体中心数目 |
0
|
| InChi Key |
XHOLNRLADUSQLD-UHFFFAOYSA-N
|
| InChi Code |
InChI=1S/C23H22ClN5O3/c1-29(2)21(25)14-4-6-15(7-5-14)22(30)27-19-10-9-17(32-3)12-18(19)23(31)28-20-11-8-16(24)13-26-20/h4-13,25H,1-3H3,(H,27,30)(H,26,28,31)
|
| 化学名 |
N-(5-Chloropyridin-2-yl)-2-((4-(N,N-dimethylcarbamimidoyl)benzoyl)amino)-5- methoxybenzamide
|
| 别名 |
PRT054021; PRT-021; MK-4448; MLN-1021; PRT 054021; PRT-054021; MK4448; MLN 1021; PRT 021; PRT021; MK 4448; MLN1021; trade name Bevyxxa
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
|
|||
|---|---|---|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: ≥ 2.5 mg/mL (5.53 mM) (饱和度未知) in 10% DMSO + 40% PEG300 +5% Tween-80 + 45% Saline (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。
例如,若需制备1 mL的工作液,可将100 μL 25.0 mg/mL澄清DMSO储备液加入到400 μL PEG300中,混匀;然后向上述溶液中加入50 μL Tween-80+,混匀;加入450 μL生理盐水定容至1 mL。 *生理盐水的制备:将 0.9 g 氯化钠溶解在 100 mL ddH₂O中,得到澄清溶液。 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.2128 mL | 11.0641 mL | 22.1283 mL | |
| 5 mM | 0.4426 mL | 2.2128 mL | 4.4257 mL | |
| 10 mM | 0.2213 mL | 1.1064 mL | 2.2128 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
(a) Dose-dependent reversal of betrixaban, rivaroxaban and apixaban inhibition in fXa enzyme assays. (b) Reversal of the prolongation of prothrombin time (PT) produced by rivaroxaban in human plasma after incubation of rivaroxaban (1 μM) with different concentrations of r-Antidote at room temperature for 30 min before initiation of the assay.Nat Med.2013 Apr;19(4):446-51. |
|---|
(a) Whole-blood INR values (mean ± s.d.) in rats infused with rivaroxaban (0.25 mg per kg body weight h−1) or vehicle for 30 min and then treated with either vehicle or r-Antidote by i.v. bolus (4 mg) over 5 min plus infusion (4 mg h−1) for up to 90 min. (b) Whole-blood INR values (mean ± s.d.) in rats infused with betrixaban (1 mg per kg body weight h−1) or vehicle and then treated with either vehicle or r-Antidote by i.v. bolus (6 mg) over 5 min plus infusion (9 mg h−1) for up to 90 min.Nat Med.2013 Apr;19(4):446-51. |
a) Dose titration of r-Antidote for the mitigation of blood loss caused by enoxaparin-induced anticoagulation in the indicated groups. (b) Mitigation of blood loss caused by fondaparinux-induced anticoagulation with r-Antidote in the indicated groups. Treat-I, vehicle treatment alone;(c) The anti-fXa activity in fondaparinux-anticoagulated rats (shown inb) at different time points for the Treat-II (square), Treat-III (diamond) and Treat-IV (inverted triangle) groups.Nat Med.2013 Apr;19(4):446-51. |