| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| 1g |
|
||
| 10g |
|
||
| Other Sizes |
|
| 靶点 |
Voltage-gated sodium channels (for regional anaesthesia and pain management) [1]
- miR-489-3p/SLC7A11 signaling pathway (for ferroptosis induction in gastric cancer) [2] - N-methyl-D-aspartate (NMDA) receptor-related targets (for excitotoxic neuronal death regulation)[3] |
|---|---|
| 体外研究 (In Vitro) |
Levobupivacaine(0–4 mM;24 h)抑制 HGC27 和 SGC7901 细胞的活力,但对 GES-1 细胞的活力没有影响[2]。 Levobupivacaine(2 mM;24、48 或 72 小时)可增加 Erastin 对 HGC27 和 SGC7901 细胞活力的抑制作用;它还会提高铁、Fe2+ 和脂质活性氧的水平[2]。 Levobupivacaine(2 mM;24 h)可提高 HGC27 和 SGC7901 细胞中铁和 Fe2+ 的水平,并改善 miR-489-3p 的表达[2]。
盐酸左旋布比卡因(Levobupivacaine HCl) 抑制神经元细胞膜上的电压门控钠通道,阻断钠离子内流并抑制神经冲动传导,这是其发挥区域麻醉和镇痛作用的基础 [1] - 在人胃癌细胞系中,盐酸左旋布比卡因(Levobupivacaine HCl) 通过调控miR-489-3p/SLC7A11信号通路诱导铁死亡:上调miR-489-3p表达,该microRNA直接靶向并下调SLC7A11,导致谷胱甘肽(GSH)合成减少、脂质过氧化水平升高,最终导致胃癌细胞死亡 [2] - 在原代培养的皮质神经元中,盐酸左旋布比卡因(Levobupivacaine HCl) 可减少NMDA暴露诱导的兴奋性毒性神经元死亡;与消旋布比卡因相比,其在相关浓度下表现出相当的神经保护作用 [3] |
| 体内研究 (In Vivo) |
Levobupivacaine(40 μmol/kg;IP;每日一次,持续 25 天)可增加脂质 ROS 的积累,同时显着抑制 SGC7901 细胞的发育[2]。小剂量使用时,左氧氟沙星(5 或 36 mg/kg;IP;单剂量)可延长部分性癫痫发作的潜伏期并抑制全身性癫痫发作;当大剂量使用时,它会缩短 N-甲基-d-天冬氨酸 (NMDA) 诱发的癫痫发作潜伏期并加剧癫痫发作[3]。
在动物模型和临床场景中,盐酸左旋布比卡因(Levobupivacaine HCl) 经硬膜外、脊髓、周围神经阻滞或局部浸润给药时,呈现剂量依赖性区域麻醉效果,镇痛持续时间与消旋布比卡因相当或更长 [1] - 在NMDA诱导癫痫的小鼠中,盐酸左旋布比卡因(Levobupivacaine HCl) 预处理可降低癫痫发作的严重程度和持续时间,并减轻脑组织中NMDA介导的兴奋性毒性神经元损伤,其神经保护效力与消旋布比卡因相似 [3] |
| 酶活实验 |
电压门控钠通道活性测定:采用神经元细胞膜制备物或分离的神经元,通过膜片钳技术记录钠通道电流。将盐酸左旋布比卡因(Levobupivacaine HCl) 以梯度浓度应用,分析电流幅度和门控特性的变化,以评估阻断效率 [1]
- SLC7A11活性测定:制备胃癌细胞裂解液,通过检测GSH合成效率来衡量SLC7A11的转运活性。将盐酸左旋布比卡因(Levobupivacaine HCl) 与裂解液共同孵育,定量检测GSH水平变化以反映SLC7A11的抑制情况 [2] |
| 细胞实验 |
细胞活力测定[2]
细胞类型: GES-1、HGC27 和 SGC790 测试浓度: 0、0.5、1、2 和 4 mM 孵育时间: 24 h 实验结果:不影响正常胃上皮GES-1细胞系的活力,但抑制HGC27和SGC7901细胞的活力以剂量依赖性方式。 细胞活力测定[2] 细胞类型: HGC27 和 SGC7901(与 5 μMerastin 一起孵育) 测试浓度: 2 mM 孵育时间:24、48或72小时 实验结果:增强erastin诱导的对HGC27和SGC7901细胞活力的抑制作用;诱导 Fe2+、铁和脂质 ROS 的水平。 RT-PCR[2] 细胞类型: HGC27 和 SGC7901(与 5 μMerastin 一起孵育) 测试浓度: 2 mM 孵育时间: 24 h 实验结果:增强HGC27和SGC7901细胞中miR-489-3p的表达,增加Fe2+和铁的水平。 胃癌细胞铁死亡测定:将胃癌细胞接种培养至对数生长期,用不同浓度(公开数据未明确具体范围)的盐酸左旋布比卡因(Levobupivacaine HCl) 处理24-72小时。采用CCK-8法检测细胞活力;使用脂质活性氧(ROS)探针检测脂质过氧化水平;通过比色法测定GSH含量;采用实时荧光定量PCR(qPCR)检测miR-489-3p表达;通过western blot分析SLC7A11蛋白表达 [2] - 皮质神经元兴奋性毒性测定:从胚胎小鼠中分离原代皮质神经元并进行体外培养。神经元成熟后,用盐酸左旋布比卡因(Levobupivacaine HCl) 预处理一定时间,再用NMDA诱导兴奋性毒性。通过MTT法或活/死染色评估神经元存活率,在显微镜下观察神经元形态变化 [3] - 神经元钠通道测定:培养分离的神经元,在培养基中加入梯度浓度的盐酸左旋布比卡因(Levobupivacaine HCl)。采用膜片钳技术记录钠通道电流,分析对通道活性的抑制作用 [1] |
| 动物实验 |
动物/疾病模型: CD1 小鼠(30-35 g;注射 NMDA 诱发癫痫发作)[3]
剂量: 5 或 36 mg/kg 给药途径: 腹腔注射;单次给药 实验结果: 5 mg/kg 剂量可延长部分性癫痫发作的潜伏期并预防全身性癫痫发作;36 mg/kg 剂量可缩短 NMDA 诱发癫痫发作的潜伏期并加重癫痫发作的严重程度。 动物/疾病模型: SCID裸鼠(6-8周龄;皮下注射5×10⁶个SGC7901细胞)[2] 剂量: 40 μmol/kg 给药途径: 腹腔注射;每日一次,持续25天 实验结果: 显著抑制SGC7901细胞生长,并增强脂质ROS的积累。 区域麻醉动物实验:将动物(大鼠、兔或犬)随机分为实验组和对照组。盐酸左布比卡因配制成浓度为0.25%至0.75% (w/v)的无菌水溶液。该药物可通过硬膜外、脊髓、坐骨神经阻滞或局部浸润给药,剂量为 1-10 mg/kg(剂量因动物种类和给药途径而异)。记录麻醉起效时间、运动和感觉阻滞持续时间以及恢复时间[1] - NMDA 诱导小鼠癫痫发作实验:将雄性或雌性小鼠(品系未指定)分为对照组、模型组和盐酸左布比卡因治疗组。治疗组在 NMDA 给药前 30 分钟腹腔注射或脑室内注射盐酸左布比卡因,剂量为 5-20 mg/kg。腹腔注射致痉挛剂量的 NMDA 以诱发癫痫发作。记录 24 小时内的癫痫发作次数、癫痫发作持续时间和死亡率;收集脑组织进行组织学分析,以评估神经元损伤[3] |
| 药代性质 (ADME/PK) |
盐酸左布比卡因血浆蛋白结合率高(97-98%)[1]
- 主要在肝脏通过细胞色素P450 (CYP)酶代谢,其中CYP3A4和CYP1A2是主要的代谢同工酶[1] - 硬膜外给药后,其在人体内的消除半衰期约为3-4小时[1] - 主要经肾脏排泄,仅有不到5%的原药以原形排出[1] |
| 毒性/毒理 (Toxicokinetics/TK) |
与消旋布比卡因相比,盐酸左布比卡因的心血管和中枢神经系统毒性较低;诱发心律失常、低血压或中枢神经系统抑制的阈值剂量更高[1]
- 高剂量给药可能导致动物和人类出现剂量相关的中枢神经系统效应(头晕、耳鸣、惊厥)和心血管效应(心肌抑制、心动过缓)[1] |
| 参考文献 |
|
| 其他信息 |
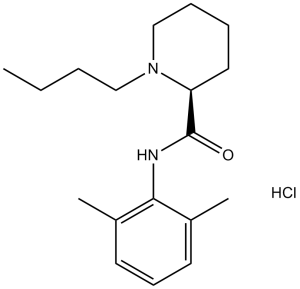
盐酸左布比卡因(无水)是左布比卡因的单盐酸盐。它是一种局部麻醉药、肾上腺素能拮抗剂、两亲分子、EC 3.1.1.8(胆碱酯酶)抑制剂和EC 3.6.3.8(Ca²⁺转运ATP酶)抑制剂。它含有左布比卡因(1+)分子。它是盐酸右布比卡因(无水)的对映异构体。
盐酸左布比卡因是左布比卡因的盐酸盐,左布比卡因是一种具有麻醉作用的酰胺衍生物。左布比卡因可逆地与电压门控钠通道结合,调节离子流,阻止神经冲动的产生和传递(稳定神经元膜),从而产生镇痛和麻醉作用。与消旋布比卡因相比,左布比卡因的血管舒张作用较弱,作用持续时间更长。 左布比卡因是布比卡因的S-对映体,可用作局部麻醉药和区域神经阻滞剂,包括硬膜外麻醉。 另见:左布比卡因(含有活性部分)。 盐酸左布比卡因是消旋布比卡因的S-对映体,是一种长效酰胺类局部麻醉药[1]。 - 其临床适应症包括区域麻醉(硬膜外、脊髓、周围神经阻滞)和术后镇痛[1]。 - 盐酸左布比卡因在胃癌细胞中诱导铁死亡的作用,为将局部麻醉药重新用于抗癌治疗提供了一个潜在的新方向[2]。它通过减轻NMDA诱导的兴奋性毒性发挥神经保护作用,这可能与谷氨酸受体信号的调节或氧化应激的减少有关[3] |
| 分子式 |
C18H28N2O.HCL
|
|
|---|---|---|
| 分子量 |
324.89
|
|
| 精确质量 |
324.196
|
|
| CAS号 |
27262-48-2
|
|
| 相关CAS号 |
Levobupivacaine;27262-47-1
|
|
| PubChem CID |
117965
|
|
| 外观&性状 |
White to off-white solid powder
|
|
| 沸点 |
423.4ºC at 760 mmHg
|
|
| 熔点 |
254 °C (dec.)(lit.)
|
|
| 闪点 |
209.9ºC
|
|
| 蒸汽压 |
2.24E-07mmHg at 25°C
|
|
| LogP |
4.74
|
|
| tPSA |
23.55
|
|
| 氢键供体(HBD)数目 |
2
|
|
| 氢键受体(HBA)数目 |
2
|
|
| 可旋转键数目(RBC) |
5
|
|
| 重原子数目 |
22
|
|
| 分子复杂度/Complexity |
321
|
|
| 定义原子立体中心数目 |
1
|
|
| SMILES |
CCCCN1CCCC[C@H]1C(=O)NC2=C(C=CC=C2C)C.Cl
|
|
| InChi Key |
SIEYLFHKZGLBNX-NTISSMGPSA-N
|
|
| InChi Code |
InChI=1S/C18H28N2O.ClH/c1-4-5-12-20-13-7-6-11-16(20)18(21)19-17-14(2)9-8-10-15(17)3;/h8-10,16H,4-7,11-13H2,1-3H3,(H,19,21);1H/t16-;/m0./s1
|
|
| 化学名 |
(2S)-1-butyl-N-(2,6-dimethylphenyl)piperidine-2-carboxamide hydrochloride
|
|
| 别名 |
|
|
| HS Tariff Code |
2934.99.9001
|
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month 注意: 请将本产品存放在密封且受保护的环境中,避免吸湿/受潮。 |
|
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
|
|||
|---|---|---|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: ≥ 3 mg/mL (9.23 mM) (饱和度未知) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。
例如,若需制备1 mL的工作液,可将100 μL 30.0 mg/mL 澄清的 DMSO 储备液加入到400 μL PEG300中,混匀;再向上述溶液中加入50 μL Tween-80,混匀;然后加入450 μL 生理盐水定容至1 mL。 *生理盐水的制备:将 0.9 g 氯化钠溶解在 100 mL ddH₂O中,得到澄清溶液。 配方 2 中的溶解度: ≥ 3 mg/mL (9.23 mM) (饱和度未知) in 10% DMSO + 90% Corn Oil (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 例如,若需制备1 mL的工作液,可将 100 μL 30.0 mg/mL 澄清 DMSO 储备液加入900 μL 玉米油中,混合均匀。 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 3.0780 mL | 15.3898 mL | 30.7796 mL | |
| 5 mM | 0.6156 mL | 3.0780 mL | 6.1559 mL | |
| 10 mM | 0.3078 mL | 1.5390 mL | 3.0780 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。