| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| Other Sizes |
|
| 靶点 |
Ileal bile acid transporter/IBAT (IC50 = 0.53 nM); IL-6; TNF-α/β
Elobixibat reduces BA reabsorption in the terminal ileum, resulting in increased BA excretion in stool and higher BA concentration in the colon, which enhances the secretion of water and electrolytes into the colon, improves intestinal motility, and eases colonic transit.[2] Elobixibat (formerly A3309) is a first-in-class ileal bile acid transporter (IBAT) inhibitor for treatment of chronic idiopathic constipation (CIC; syn functional constipation). CIC affects up to 25% of the general population; and up to a half are unsatisfied with current therapies. There is an unmet need for safe and effective drugs to treat CIC.Elobixibat provides a novel approach to treat chronic constipation via IBAT inhibition with enhanced delivery of bile acids to the colon. [1] |
|---|---|
| 体外研究 (In Vitro) |
Elobixbat(原A3309)可减少BA在回肠末端的重吸收,导致粪便中BA排泄量增加,结肠中BA浓度升高,从而促进水和电解质向结肠的分泌,改善肠道动力,缓解结肠运输[2]。
Elobixbat(原A3309)是一种一流的回肠胆汁酸转运蛋白(IBAT)抑制剂,用于治疗慢性特发性便秘(CIC;Syn功能性便秘)。多达25%的人口受CIC影响;多达一半的人对目前的治疗方法不满意。目前对安全有效的CIC治疗药物的需求还没有得到满足。依洛比昔巴提供了一种新的方法,通过IBAT抑制,增强胆汁酸向结肠的输送,治疗慢性便秘。[1] 在使用过表达哺乳动物胆汁酸转运蛋白的HEK-293细胞进行的竞争性抑制实验中,Elobixibat 能以浓度依赖的方式抑制30 µM放射性标记的甘氨胆酸通过回肠胆汁酸转运蛋白(IBAT)的细胞内积聚。这证实了其对IBAT的强效和选择性抑制。[1] |
| 体内研究 (In Vivo) |
Elobixibat治疗可降低血清BA,增加粪便BA浓度,改善肝脏炎症和纤维化。它还降低了肝脏和mln中促炎因子的表达以及肝脏中转化生长因子-β的表达。最后,elobixibat使肠道紧密连接蛋白水平和肠道微生物群组成正常化。
结论:elobixibat改善mcd喂养小鼠NASH相关组织病理学,降低细胞因子表达,并使肠道微生物组成正常化,这表明它可能是治疗NASH的有希望的候选药物。[3]
两组均出现肝脏脂肪堆积和纤维化,两组间差异无统计学意义。然而,使用elobixibat的小鼠肝脏肿瘤较少。血清总胆汁酸水平,包括游离胆汁酸、牛磺酸偶联胆汁酸、糖偶联胆汁酸和牛磺酸-α/β-胆酸,在elobixibat治疗后显著降低。伊洛比西巴治疗组粪便中革兰氏阳性菌比例(5.4%)显著低于未治疗组(33.7%)。 结论:elobixibat通过抑制胆汁酸重吸收,降低血清和肝脏中总胆汁酸和原胆汁酸水平来抑制肿瘤生长。此外,胆汁酸在结肠中的存在可能导致革兰氏阳性菌的比例显著减少,可能导致继发性胆汁酸合成减少[2]。 药效学研究表明,它能加速CIC患者的结肠运输,增加大便频率,使大便粘稠度变松,缓解便秘相关症状。这些有益效果至少可以连续治疗8周。elobixibat具有最小的吸收和较低的全身生物利用度,通常耐受性良好,并且可能通过胆汁酸消耗提供改善血清脂质谱的额外益处。[1] 在健康比格犬的肉类诱导便秘临床前模型中,口服Elobixibat(剂量为1.5、5和15 µmol/kg/天)可增加粪便重量。5和15 µmol/kg/天的剂量使粪便重量增加近3.5倍,与溶剂对照组相比具有统计学显著性。[1] 在犬类中,连续28天口服Elobixibat(剂量为5、25和200 µmol/kg/天)可剂量依赖性增加肝脏胆汁酸合成,该效应通过血浆中胆汁酸合成中间体7α-羟基-4-胆甾烯-3-酮(C4)的水平来测量。C4水平的升高在给药后24小时即可检测到,并在28天内持续维持。[1] 在一项涉及30名CIC患者的I期人体研究中,连续14天每日服用3 mg和10 mg的Elobixibat 与安慰剂相比,显著加速了结肠传输时间(CTT),主要加速部位在左半结肠。血浆C4水平升高,总胆固醇和低密度脂蛋白胆固醇剂量依赖性降低。观察到自发排便次数增加和粪便变软的趋势,特别是在10 mg剂量组。[1] 在一项涉及36名女性功能性便秘患者的IIa期人体研究中,连续14天每日服用15 mg和20 mg的Elobixibat 显著加速了结肠传输(20 mg剂量在8、24和48小时均加速;15 mg剂量在48小时加速)。粪便稠度显著变软,排便费力程度减轻,排便通畅感改善。血清C4水平剂量依赖性升高(15 mg组约2倍,20 mg组约3倍)。[1] 在一项涉及190名CIC患者的IIb期人体试验中,连续8周每日服用10 mg和15 mg的Elobixibat 与安慰剂相比,显著增加了每周自发排便次数相对于基线的变化。增加效果是剂量依赖性的,并在8周治疗期内持续存在。首次自发排便的时间显著缩短。粪便变软,排便费力减轻,腹胀严重程度改善(15 mg组)。血浆C4水平升高,总胆固醇和低密度脂蛋白胆固醇在10 mg和15 mg剂量组均下降。[1] |
| 动物实验 |
三周龄雄性C57BL/6J小鼠被随机分为两组(图1a):(1)CDHF饮食+DEN(对照组)和(2)CDHF饮食+DEN+elobixibat(elobixibat组)。小鼠在3周龄时接受单次腹腔注射25 mg/kg DEN。之后,小鼠饲喂标准饲料直至8周龄。接下来的20周,对照组小鼠饲喂CDHF饮食(60 kcal%脂肪),而elobixibat组小鼠饲喂添加了elobixibat的CDHF饮食。动物饲养于动物房内受控环境(温度 23 ± 1 °C,湿度 50 ± 10%,12 小时光照/黑暗循环),并可自由获取食物和水。[2]
elobixibat 的剂量设定[2] 计算得出 elobixibat 的剂量为 0.27 mg/kg/天。本研究使用的动物(平均体重 23 g)是根据先前发表的数据确定的。人 IBAT 的 50% 抑制浓度为 0.53 nmol/L,小鼠 IBAT 的 50% 抑制浓度为 0.13 nmol/L。因此,小鼠的抑制活性是人类的四倍。小鼠体内 elobixibat 的 70% 有效剂量浓度为 2.7 mg/kg;而 50% 有效剂量浓度为 0.27 (70% × [0.023/60])0.33 = 2.23 mg/kg;对于体重50公斤的人来说,这相当于每天110毫克,是正常用量的11倍。因此,我们将有效容量设定为50%:0.27 (50%) × [0.023/60])0.33 = 0.223毫克/公斤。根据平均预期体重和预期食物摄入量,我们配制并使用了一种CDHF+elobixibat饮食,其中每公斤CDHF饮食含有3毫克elobixibat。[2] 在该研究阶段的最后4周,小鼠每天服用1.2毫克/公斤elobixibat(elobixibat组)。研究结束时,小鼠通过吸入二氧化碳安乐死。[2] 通过灌胃法,每周5天,连续4周给予小鼠0.2、0.6或1.2毫克/公斤的elobixibat。对照组和MCD-NASH组均按相同方案通过灌胃给予PBS。0.2 mg/kg和0.6 mg/kg剂量未见明显效果(数据未显示),但1.2 mg/kg/天剂量观察到有益效果。该浓度是人体剂量的4-6倍。根据“依洛比西巴药物访谈表”,依洛比西巴对人IBAT具有强抑制活性,约为小鼠IBAT的四倍。因此,小鼠1.2 mg/kg/天的剂量相当于人体0.3 mg/kg/天的剂量。我们评估了该剂量对小鼠NASH严重程度、细胞因子生成、肠道菌群和肠道紧密连接的影响。在饲养期间未观察到腹泻,且在实验结束时,NASH组和elobixibat组的体重无差异。[2] 在临床前便秘模型中,健康比格犬被喂食牛肉饮食长达14天以诱导便秘(定义为湿粪重量<30克/天)。elobixibat以1.5、5和15 µmol/kg/天的剂量口服给药。粪便重量被测量作为评估泻药效果的主要终点。[1] 在另一项为期28天的犬药效学研究中,elobixibat以5、25和200 µmol/kg/天的剂量连续口服给药。在治疗后24小时和28天等不同时间点采集血样,以测量血浆中7α-羟基-4-胆甾烯-3-酮(C4)的水平,C4是肝脏胆汁酸合成的生物标志物。[1] |
| 药代性质 (ADME/PK) |
在一项人体 I 期临床试验中,口服Elobixibat后,血浆药物浓度极低。在 0.1 和 0.3 mg/天的剂量下,该药物无法检测到;在 1 至 10 mg/天的剂量范围内,仅能检测到皮摩尔浓度。观察到的最高血浆浓度为 0.76 nmol/L。[1]
达峰时间 (Tₘₐₓ) 在给药后 4 小时内出现。[1] 血浆消除在给药后 24 小时内完成。[1] 口服后,Elobixibat 在胃肠道的吸收极少,导致其全身生物利用度极低。[1] 在血浆中未检测到母体化合物及其代谢物。[1] Elobixibat 在血浆中的蛋白结合率很高 (>99%)。 [1] 血浆半衰期 (t½) 小于 4 小时。[1] 依洛昔巴在体外可抑制细胞色素 P450 酶 CYP2C9 和 CYP3A4,IC₅₀ 值分别为 10.3 µM 和 6.0 µM。然而,由于其全身吸收极少,口服给药后通过此机制发生具有临床意义的药物相互作用的风险被认为较低。[1] |
| 毒性/毒理 (Toxicokinetics/TK) |
在 I 期和 II 期临床试验中,未报告与Elobixibat相关的严重不良事件。[1]
最常见的不良事件为胃肠道反应。在一项 IIa 期研究中,与安慰剂组(13 例患者中 0 例)相比,15 mg 组(12 例患者中有 4 例)和 20 mg 组(12 例患者中有 6 例)更常出现轻度至中度腹部痉挛或疼痛。这种疼痛通常发生在排便之前,并在排便后缓解。[1] 腹泻在高剂量组中更常见(在 IIa 期研究中,20 mg 组有 4 例,而 15 mg 组和安慰剂组各有 1 例)。所有因不良事件而退出研究的患者均与腹泻有关。[1] 在一项为期 8 周的 IIb 期研究中,15 mg 组的治疗中断率(23%)高于安慰剂组和较低剂量组(约 13%)。总体而言,54% 的患者报告了不良事件,其中 7% 为严重不良事件。3 例患者发生了严重不良事件,但被认为与研究药物无关。[1] 理论上存在一种担忧,即增加胆汁酸向结肠的输送可能会增加结直肠癌的风险,尽管对具有类似情况(例如,部分回肠旁路术后)的患者进行的长期研究并未显示发病率增加。[1] 理论上,Elobixibat 消耗胆汁酸可能会改变胆汁中胆固醇与胆汁酸的比例,从而可能增加胆固醇结石形成的风险。[1] |
| 参考文献 |
[1]. Elobixibat for the treatment of constipation. Expert Opin Investig Drugs. 2013 Feb; 22(2):277-84.
[2].Impact of elobixibat on liver tumors, microbiome, and bile acid levels in a mouse model of nonalcoholic steatohepatitis. Hepatol Int. 2023 Dec;17(6):1378-1392. [3].Elobixibat, an ileal bile acid transporter inhibitor, ameliorates non-alcoholic steatohepatitis in mice. Hepatol Int. 2021 Apr;15(2):392-404. |
| 其他信息 |
依洛昔巴已用于血脂异常、便秘、慢性便秘、功能性便秘和慢性特发性便秘的治疗及基础科学研究的临床试验中。
药物适应症 治疗慢性便秘 依洛昔巴是一种首创的口服回肠胆汁酸转运体 (IBAT) 抑制剂,用于治疗慢性特发性便秘 (CIC)。[1] 其作用机制是局部抑制回肠对胆汁酸的重吸收,从而增加胆汁酸向结肠的输送。在结肠中,胆汁酸刺激肠道蠕动和分泌,从而加速结肠转运,使大便稀薄,并改善便秘症状。 [1] 通过抑制回肠重吸收,Elobixibat可上调肝脏利用胆固醇合成新的胆汁酸,从而可能对血脂谱产生有益影响,例如降低低密度脂蛋白胆固醇(LDL-C)。[1] 临床试验已证实,Elobixibat可在治疗的第一周内有效增加自发性排便次数、软化粪便性状、减少排便费力并加速结肠转运,且疗效至少可持续8周。[1] 其低全身吸收使其安全性总体良好,主要副作用为胃肠道反应(腹痛、腹泻),这些反应通常与剂量相关,被认为是其药理作用的延伸。[1] 截至本文发表日期(2013年),Elobixibat尚未在任何国家提交监管部门批准申请,预计将开展III期临床试验。[1] |
| 分子式 |
C36H45N3O7S2
|
|---|---|
| 分子量 |
695.8884
|
| 精确质量 |
695.27
|
| 元素分析 |
C, 62.14; H, 6.52; N, 6.04; O, 16.09; S, 9.21
|
| CAS号 |
439087-18-0
|
| 相关CAS号 |
Elobixibat hydrate;1633824-78-8; 439087-68-0 (S-isomer)
|
| PubChem CID |
9939892
|
| 外观&性状 |
Typically exists as White to off-white solid at room temperature
|
| LogP |
8.964
|
| tPSA |
182.77
|
| 氢键供体(HBD)数目 |
3
|
| 氢键受体(HBA)数目 |
9
|
| 可旋转键数目(RBC) |
16
|
| 重原子数目 |
48
|
| 分子复杂度/Complexity |
1140
|
| 定义原子立体中心数目 |
1
|
| SMILES |
S1(C2=C([H])C(=C(C([H])=C2N(C2C([H])=C([H])C([H])=C([H])C=2[H])C([H])([H])C(C([H])([H])C([H])([H])C([H])([H])C([H])([H])[H])(C([H])([H])C([H])([H])C([H])([H])C([H])([H])[H])C1([H])[H])SC([H])([H])[H])OC([H])([H])C(N([H])[C@@]([H])(C(N([H])C([H])([H])C(=O)O[H])=O)C1C([H])=C([H])C([H])=C([H])C=1[H])=O)(=O)=O
|
| InChi Key |
XFLQIRAKKLNXRQ-UUWRZZSWSA-N
|
| InChi Code |
InChI=1S/C36H45N3O7S2/c1-4-6-18-36(19-7-5-2)24-39(27-16-12-9-13-17-27)28-20-30(47-3)29(21-31(28)48(44,45)25-36)46-23-32(40)38-34(26-14-10-8-11-15-26)35(43)37-22-33(41)42/h8-17,20-21,34H,4-7,18-19,22-25H2,1-3H3,(H,37,43)(H,38,40)(H,41,42)/t34-/m1/s1
|
| 化学名 |
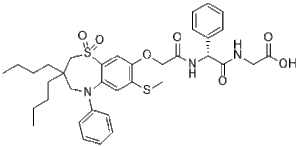
(R)-(2-(2-((3,3-dibutyl-7-(methylthio)-1,1-dioxido-5-phenyl-2,3,4,5-tetrahydrobenzo[b][1,4]thiazepin-8-yl)oxy)acetamido)-2-phenylacetyl)glycine
|
| 别名 |
AZD-7806; AZD 7806; AZD7806; A 3309; 439087-18-0; AZD7806; AZD-7806; A3309; 865UEK4EJC; A-3309; 2-[[(2R)-2-[[2-[(3,3-dibutyl-7-methylsulfanyl-1,1-dioxo-5-phenyl-2,4-dihydro-1lambda6,5-benzothiazepin-8-yl)oxy]acetyl]amino]-2-phenylacetyl]amino]acetic acid; A3309; A-3309; AJG-533
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
DMSO : ~250 mg/mL (~359.25 mM)
|
|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: ≥ 2.08 mg/mL (2.99 mM) (饱和度未知) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。
例如,若需制备1 mL的工作液,可将100 μL 20.8 mg/mL澄清DMSO储备液加入400 μL PEG300中,混匀;然后向上述溶液中加入50 μL Tween-80,混匀;加入450 μL生理盐水定容至1 mL。 *生理盐水的制备:将 0.9 g 氯化钠溶解在 100 mL ddH₂O中,得到澄清溶液。 配方 2 中的溶解度: 2.08 mg/mL (2.99 mM) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (这些助溶剂从左到右依次添加,逐一添加), 悬浊液; 超声助溶。 例如,若需制备1 mL的工作液,可将 100 μL 20.8 mg/mL澄清DMSO储备液加入900 μL 20% SBE-β-CD生理盐水溶液中,混匀。 *20% SBE-β-CD 生理盐水溶液的制备(4°C,1 周):将 2 g SBE-β-CD 溶解于 10 mL 生理盐水中,得到澄清溶液。 View More
配方 3 中的溶解度: ≥ 2.08 mg/mL (2.99 mM) (饱和度未知) in 10% DMSO + 90% Corn Oil (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.4370 mL | 7.1850 mL | 14.3701 mL | |
| 5 mM | 0.2874 mL | 1.4370 mL | 2.8740 mL | |
| 10 mM | 0.1437 mL | 0.7185 mL | 1.4370 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。