| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| Other Sizes |
|
| 体外研究 (In Vitro) |
结核分枝杆菌的 KatG 细菌过氧化氢酶-过氧化物酶是激活前药异烟肼 (INH) 所必需的 [1]。当 KatG 将异烟酰与 NADH 结合时,会产生异烟酰-NADH 复合物。该复合物可抑制天然烯烃聚酰亚胺-AcpM 底物和植物制造的酶,该复合物与基于烯烃聚酰亚胺的载体化妆品还原酶(称为 InhA)牢固结合。在此过程中,分枝杆菌培养基的细胞壁必须回流。一氧化氮是异烟肼被 KatG 激活时产生的序列之一,也被证明对另一种抗分枝杆菌前药 PA-824 的活性至关重要 [2] [3]。对于分裂速度快的分枝杆菌,异烟肼有杀菌作用;对于生长缓慢的分枝杆菌,具有抑菌作用[4]。
|
|---|---|
| 药代性质 (ADME/PK) |
吸收、分布和排泄
口服后易于吸收;然而,可能经历显著的首过代谢。异烟肼与食物同服会降低其吸收和生物利用度。 24小时内,50%至70%的异烟肼剂量经尿液排出。 异烟肼易于扩散至所有体液和细胞。在胸膜液和腹水中可检测到显著浓度的药物;脑脊液中的浓度与血浆中的浓度相似。异烟肼能很好地渗透到干酪样物质中。药物在血浆和肌肉中的初始浓度高于感染组织,但后者能长时间保持药物浓度,且远高于抑菌所需浓度。 异烟肼剂量的75%至95%在24小时内经尿液排出,主要以代谢物形式排出。 口服后易于吸收;但可能经历显著的首过代谢。异烟肼与食物同服会降低其吸收和生物利用度。 广泛分布于所有体液和组织,包括脑脊液、胸膜液和腹水、皮肤、痰液、唾液、肺、肌肉和干酪样组织。异烟肼可通过胎盘排出,并可分泌至乳汁中。 有关异烟肼(共10种)的更多吸收、分布和排泄(完整)数据,请访问HSDB记录页面。 代谢/代谢物 主要在肝脏代谢。异烟肼经N-乙酰转移酶乙酰化为N-乙酰异烟肼;然后生物转化为异烟酸和单乙酰肼。单乙酰肼经细胞色素P450混合氧化酶系统N-羟基化后形成活性中间代谢物,从而导致肝毒性。乙酰化速率由基因决定。慢乙酰化者的特征是肝脏N-乙酰转移酶相对缺乏。 异烟肼在肝脏中主要通过乙酰化和脱肼作用失活。该药物的代谢产物包括乙酰异烟肼、异烟酸、单乙酰肼、二乙酰肼和异烟酰甘氨酸。 在人体中,尿液中异烟肼最重要的代谢产物是1-乙酰-2-异烟酰肼(乙酰异烟肼)、N-乙酰-N'-异烟酸、异烟酰甘氨酸、丙酮酸异烟酰腙和α-酮戊二酸异烟酰腙。 在兔体内,异烟肼的代谢产物是异烟酸和氨,氨来源于肼基的快速分解。乙酰异烟肼的乙酰化反应生成单乙酰肼,后者已被证实是动物体内一种强效肝毒素。单乙酰肼在动物体内的微粒体代谢会产生一种活性酰化物质,该物质能够与组织大分子(例如肝蛋白)共价结合,进而导致肝细胞坏死。有关异烟肼(共6种代谢物)的更多代谢/代谢产物(完整)数据,请访问HSDB记录页面。异烟肼已知的代谢产物包括3,4,5-三羟基-6-[2-(吡啶-4-羰基)肼基]氧杂环己烷-2-羧酸和N-乙酰异烟肼。主要在肝脏代谢。异烟肼经N-乙酰转移酶乙酰化生成N-乙酰异烟肼;异烟肼随后生物转化为异烟酸和单乙酰肼。单乙酰肼在细胞色素P450混合氧化酶系统的N-羟基化作用下,会形成一种活性中间代谢物,从而导致肝毒性。乙酰化速率由基因决定。慢乙酰化者的特征是肝脏N-乙酰转移酶相对缺乏。 消除途径:50%至70%的异烟肼剂量在24小时内经尿液排出。 半衰期:快乙酰化者:0.5至1.6小时。慢乙酰化者:2至5小时。 生物半衰期 快乙酰化者:0.5至1.6小时。慢速乙酰化者:2 至 5 小时。 成人(包括老年患者)- 快速乙酰化者:0.5 至 1.6 小时。慢速乙酰化者:2 至 5 小时。急性和慢性肝病:半衰期可能延长(6.7 小时,对照组为 3.2 小时)。 儿童(1.5 至 15 岁)- 2.3 至 4.9 小时。 新生儿- 7.8 小时,经胎盘给予异烟肼的新生儿半衰期为 19.8 小时。半衰期长可能是由于新生儿乙酰化能力有限所致。 |
| 毒性/毒理 (Toxicokinetics/TK) |
肝毒性
尽管异烟肼的使用有限,但它仍然是美国导致严重特异性肝损伤的最常见原因之一。异烟肼治疗会导致10%至20%的患者出现短暂的血清转氨酶升高,3%至5%的患者转氨酶水平超过正常值上限(ULN)的5倍。这些酶升高通常无症状,即使不调整剂量继续治疗,也常常会自行消退(病例1和2)。 此外,异烟肼还可能引起临床上明显的急性肝损伤,伴有黄疸,发生率在0.5%至1%之间,死亡率在0.05%至0.1%之间。已发表的文献中,肝损伤的发生率差异很大。造成这种差异的主要因素可能是年龄。异烟肼引起的临床显性肝炎发生率估计为:20至35岁患者0.5%,35至50岁患者1.5%,50岁以上人群3%或更高。异烟肼肝毒性在儿童中罕见(但仍有发生,且可能致命)。其他危险因素包括既往肝病(乙型或丙型肝炎)、同时服用利福平或吡嗪酰胺,以及可能的酗酒、黑人种族和遗传因素。损伤的典型发病时间为2周至6个月,但最长可达1年,最短可达1周。起病通常隐匿,类似于急性病毒性肝炎,前驱期表现为恶心、厌食、腹部不适和乏力,随后出现尿色加深和黄疸(病例3和4)。肝酶升高模式通常为肝细胞性,ALT 水平显著升高(>10 倍正常值上限),碱性磷酸酶值轻微升高(通常 可能性评分:A(已确立的临床明显肝损伤病因)。 妊娠和哺乳期影响 ◉ 哺乳期用药概述 由于母乳中异烟肼含量低,且可安全直接用于婴儿,因此不太可能引起婴儿不良反应,但应监测婴儿是否出现罕见的黄疸。在婴儿最长睡眠时间之前给母亲服用每日一次的剂量,可以减少婴儿的摄入剂量。母乳中的异烟肼含量不足以治疗母乳喂养婴儿的结核病。如果母乳喂养的婴儿接受异烟肼治疗,还应每日服用吡哆醇 1 mg/kg。美国疾病控制与预防中心和其他专业机构指出,服用异烟肼的女性不应被劝阻进行母乳喂养。 所有服用异烟肼的哺乳期母亲均应每日口服25毫克吡哆醇。一项针对同时感染HIV和结核病的非洲哺乳期母亲的研究发现,服用异烟肼的母亲患烟酸缺乏症(糙皮病)的风险增加。作者建议,在营养不良的人群中,异烟肼治疗期间补充多种维生素可能是有益的。 ◉ 对母乳喂养婴儿的影响 在一项非对照研究中,研究人员测量了10名男婴的6β-羟基皮质醇水平。这些男婴的母亲患有结核病,每日服用1克乙胺丁醇和300毫克异烟肼;同时,研究人员还测量了10名男婴的母亲(显然没有结核病)所生的婴儿的6β-羟基皮质醇水平,这些母亲未接受任何长期药物治疗。结果显示,服用抗结核药物的母亲所生的婴儿在8次测量中,其6β-羟基皮质醇水平始终低于服用抗结核药物的母亲所生的婴儿。从出生后90天到195天,每隔15天检测一次,但这些差异仅在第120天和第195天具有统计学意义。作者将较低的皮质醇水平归因于乳汁中的抗结核药物抑制了肝脏将皮质醇代谢为6β-羟基皮质醇的过程。然而,已知乙胺丁醇不会抑制药物代谢,因此如果出现这种影响,更可能是由异烟肼引起的。 一位妇女在孕期每日服用利福平450毫克、异烟肼300毫克和乙胺丁醇1200毫克,并在哺乳期前7个月每日服用利福平450毫克和异烟肼300毫克(未说明服用剂量)。该婴儿出生时血清肝酶轻度升高,持续1年(丙氨酸转氨酶)至2年(天冬氨酸转氨酶),但未出现其他不良反应。 异烟肼是作为……的一部分使用的。两名孕妇在妊娠中晚期及产后接受了多重耐药结核病的多药联合治疗方案。她们的两个婴儿均接受了母乳喂养(喂养程度和持续时间未说明)。两个孩子分别在3.9岁和4.6岁时发育正常,其中一个孩子有轻微的语言发育迟缓。 土耳其的两名母亲分别在妊娠30周和34周时被诊断出患有结核病。她们立即开始服用异烟肼300毫克、利福平600毫克和吡哆醇50毫克,每日一次,持续6个月;同时加用吡嗪酰胺25毫克/公斤和乙胺丁醇25毫克/公斤,每日一次,持续2个月。两名母亲均进行了母乳喂养(喂养程度未说明)。她们的婴儿接受了异烟肼5毫克/公斤,每日一次,持续3个月的预防性治疗。3个月后结核菌素皮肤试验结果为阴性,两个婴儿在1岁时均未患结核病。年龄。未提及药物的不良反应。 ◉ 对哺乳和母乳的影响 截至修订日期,未找到相关的已发表信息。 蛋白质结合 极低 (0-10%) |
| 参考文献 |
|
| 其他信息 |
异烟肼为无臭无色或白色结晶或白色结晶性粉末。初尝略甜,后苦。1%水溶液pH值为5.5-6.5,5%水溶液pH值为6-8。(NTP,1992)
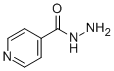
异烟肼是一种碳酰肼,由吡啶-4-羧酸和肼缩合而成。它是一种抗结核药物,也是一种药物过敏原。其结构与异烟酸类似。 异烟肼是一种处方抗菌药,经美国食品药品监督管理局(FDA)批准用于预防和治疗结核病(TB)。 结核病可能是HIV感染的机会性感染(OI)。 主要用作抑结核病的抗菌药物。异烟肼仍然是结核病的首选治疗药物。 异烟肼是一种抗分枝杆菌药物。 异烟肼是治疗结核病最可靠、最常用的药物。异烟肼治疗通常会导致血清转氨酶水平轻微、短暂且无症状的升高,但更重要的是,异烟肼是导致急性肝损伤的已知原因,这种肝损伤可能很严重,有时甚至致命。 据报道,异烟肼可感染赭曲霉、巨型灵芝和其他一些有相关数据的微生物。 异烟肼是烟酸的合成衍生物,具有抗分枝杆菌活性。尽管其作用机制尚不完全清楚,但异烟肼似乎能阻断分枝杆菌细胞壁主要成分——分枝菌酸的合成。该药物仅对活跃生长的分枝杆菌有效,因为它是一种前药,需要在易感分枝杆菌中激活才能发挥作用。异烟肼还会干扰分枝杆菌对维生素B6的代谢。耐药性的产生是由于细菌细胞壁穿透力下降。(NCI04) 主要用作抑结核病的抗菌药物。它仍然是治疗结核病的首选药物。 主要用作抑结核病的抗菌药物。它仍然是治疗结核病的首选药物。 另见:异烟肼;利福平(成分);甜叶菊叶(部分);异烟肼;吡嗪酰胺;利福平(成分)。 药物适应症 异烟肼用于治疗所有对异烟肼敏感的结核病。它还可与利福平和吡嗪酰胺联合使用。 用于1日龄雏鸡的主动免疫,以减少由堆型艾美球虫、布氏艾美球虫、巨型艾美球虫、坏死艾美球虫和柔嫩艾美球虫引起的球虫病相关的临床症状(腹泻)、肠道病变和卵囊排出。 作用机制 异烟肼是一种前药,必须经细菌过氧化氢酶激活。具体而言,激活过程与肼还原分枝杆菌的铁KatG过氧化氢酶-过氧化物酶,并与氧气反应形成氧合亚铁酶复合物有关。激活后,异烟肼抑制分枝杆菌细胞壁重要成分——分枝菌酸的合成。异烟肼在治疗浓度下对活跃生长的细胞内和细胞外结核分枝杆菌具有杀菌作用。具体而言,异烟肼通过与NAD辅因子形成共价加合物来抑制结核分枝杆菌的烯酰还原酶InhA。正是这种INH-NAD加合物作为InhA的缓慢、紧密结合的竞争性抑制剂发挥作用。尽管异烟肼的作用机制尚不完全清楚,但已提出了几种假设。这些假设包括其对脂质、核酸生物合成和糖酵解的影响。……有人认为,异烟肼的主要作用是抑制分枝杆菌细胞壁重要成分——分枝菌酸的生物合成。由于分枝菌酸是分枝杆菌特有的,因此这种作用可以解释异烟肼抗菌活性的高度选择性。异烟肼会导致微生物的抗酸性丧失和甲醇可提取脂质含量降低。 异烟肼对“休眠”状态的结核杆菌具有抑菌作用,但对快速分裂的微生物具有杀菌作用。其最低抑结核浓度为0.025至0.05微克/毫升。 |
| 分子式 |
C6H7N3O
|
|---|---|
| 分子量 |
137.1393
|
| 精确质量 |
137.058
|
| CAS号 |
54-85-3
|
| 相关CAS号 |
Isoniazid-d4;774596-24-6
|
| PubChem CID |
3767
|
| 外观&性状 |
White to off-white solid powder
|
| 密度 |
1.2±0.1 g/cm3
|
| 熔点 |
171-173 °C(lit.)
|
| 闪点 |
>250°C
|
| 折射率 |
1.584
|
| LogP |
-0.89
|
| tPSA |
68.01
|
| 氢键供体(HBD)数目 |
2
|
| 氢键受体(HBA)数目 |
3
|
| 可旋转键数目(RBC) |
1
|
| 重原子数目 |
10
|
| 分子复杂度/Complexity |
120
|
| 定义原子立体中心数目 |
0
|
| InChi Key |
QRXWMOHMRWLFEY-UHFFFAOYSA-N
|
| InChi Code |
InChI=1S/C6H7N3O/c7-9-6(10)5-1-3-8-4-2-5/h1-4H,7H2,(H,9,10)
|
| 化学名 |
pyridine-4-carbohydrazide
|
| 别名 |
Isoniazid HyzydIsovitIsonicotinylhydrazideNydrazidHydra
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month 注意: 本产品在运输和储存过程中需避光。 |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
DMSO : ~50 mg/mL (~364.59 mM)
H2O : ~33.33 mg/mL (~243.04 mM) |
|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: 150 mg/mL (1093.77 mM) in PBS (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液; 超声助溶。
请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 7.2918 mL | 36.4591 mL | 72.9182 mL | |
| 5 mM | 1.4584 mL | 7.2918 mL | 14.5836 mL | |
| 10 mM | 0.7292 mL | 3.6459 mL | 7.2918 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT02043314 | COMPLETED | Drug: Isoniazida | Tuberculosis | Oswaldo Cruz Foundation | 2008-10 | Phase 1 |
| NCT00397709 | TERMINATED | Drug: I ( isoniazid), II (isoniazid + rifampin ) | Tuberculosis | Hospital Virgen de la Luz | 1996-03 | Phase 4 |
| NCT00571753 | TERMINATED | Drug: isoniazid Drug: isoniazid |
Pulmonary Tuberculosis | University of Cologne | 2008-06 | Phase 3 |
| NCT00164281 | COMPLETED | Drug: Isoniazid | HIV Infections Tuberculosis |
Centers for Disease Control and Prevention | 2004-11 | Phase 4 |
| NCT02980016 | COMPLETED | Drug: rifapentine + isoniazid Drug: Isoniazid |
HIV Tuberculosis |
The Aurum Institute NPC | 2016-11 | Phase 3 |