| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 10 mM * 1 mL in DMSO |
|
||
| 1mg |
|
||
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| Other Sizes |
|
| 靶点 |
BTK (IC50 = 5.69 nM)
Pirtobrutinib (LOXO-305) targets Bruton's tyrosine kinase (BTK), including wild-type BTK (Ki = 0.5 nM; IC50 = 1.6 nM for kinase activity) and C481S-mutant BTK (Ki = 0.6 nM; IC50 = 2.1 nM for kinase activity) [3] Pirtobrutinib (LOXO-305) shows high selectivity for BTK over other TEC family kinases (ITK: IC50 = 45 nM; TEC: IC50 = 62 nM; BMX: IC50 = 78 nM) and non-TEC kinases (EGFR: IC50 > 1000 nM; SRC: IC50 > 1000 nM; JAK3: IC50 = 510 nM) [3] Pirtobrutinib (LOXO-305) inhibits clinically relevant BTK mutations, including C481R (IC50 = 3.2 nM), C481F (IC50 = 2.8 nM), and L528W (IC50 = 4.5 nM) [3] |
|---|---|
| 体外研究 (In Vitro) |
Pirtobrutinib(LOXO-305)是下一代布鲁顿酪氨酸激酶(BTK)抑制剂,具有高度选择性、非共价性,并与WT BTK和几个BTK C481取代突变表现出强平衡结合。它还有效地抑制BTK C481S、T和R突变的细胞活性。[2]
在BTK依赖性B细胞恶性肿瘤细胞系(套细胞淋巴瘤MCL:Jeko-1、Mino;慢性淋巴细胞白血病CLL:MEC-1、OSU-CLL)中,Pirtobrutinib (LOXO-305) 抑制细胞增殖,IC50值范围为3.7 nM(Jeko-1)至12.5 nM(OSU-CLL)[3] - 在表达C481S突变型BTK的细胞系(Jeko-1-C481S、MEC-1-C481S)中,该药物具有抗增殖活性,IC50分别为4.2 nM和5.8 nM,显著优于伊布替尼(两者IC50均>1 μM)[3] - Western blot分析显示,在Jeko-1和Jeko-1-C481S细胞中以剂量依赖性方式抑制BTK磷酸化(pBTK)及下游信号分子(AKT、ERK1/2、PLCγ2);50 nM浓度下实现最大抑制率(>90%)[3] - 诱导CLL和MCL细胞系发生半胱天冬酶依赖性凋亡(Annexin V/PI染色显示,100 nM浓度处理72小时后,35–45%的细胞发生凋亡)[3] - 对伊布替尼耐药的C481S突变患者来源的原代CLL细胞,Pirtobrutinib (LOXO-305)(100 nM)可抑制>85%的pBTK,并降低60%的细胞活力[3] - 在BTK非依赖性细胞系(Raji、Daudi)中无显著抗增殖活性,IC50 > 1000 nM[3] |
| 体内研究 (In Vivo) |
吡妥布替尼在体内显著抑制人淋巴瘤异种移植物的肿瘤生长。[3]
在Jeko-1(野生型BTK)皮下异种移植小鼠模型中,口服给予Pirtobrutinib (LOXO-305)(25 mg/kg,每日两次,连续21天),与溶媒对照组相比,肿瘤生长抑制率达83%;肿瘤组织中pBTK和pAKT水平降低[3] - 在Jeko-1-C481S(突变型BTK)异种移植模型中,Pirtobrutinib (LOXO-305)(30 mg/kg,口服,每日两次)实现78%的肿瘤生长抑制,而伊布替尼(50 mg/kg)仅为22%[3] - 在C481S突变型CLL患者来源异种移植(PDX)模型中,Pirtobrutinib (LOXO-305)(20 mg/kg,口服,每日两次)实现75%的肿瘤生长抑制,并将中位生存期延长50%[3] - 在携带L528W BTK突变的MCL PDX模型中,Pirtobrutinib (LOXO-305)(30 mg/kg,口服,每日两次)抑制肿瘤生长72%[3] |
| 酶活实验 |
在HotSpot激酶测定(反应生物学,Malvern,PA)中,通过监测[33P]-三磷酸腺苷(ATP)中[33P]-PO4掺入聚谷氨酸-酪氨酸(poly-EY)肽底物来测定Pirtobrutinib对BTK、BTK C481S和选定的非BTK激酶的活性。25使用标准曲线拟合方法分析数据。使用HotSpot激酶测定和Km-ATP浓度测试了Pirtobrutinib(1μM)对371种人类激酶的激酶活性抑制。使用HotSpot激酶测定法在10μM ATP的浓度下测试Pirtobrutinib、ibrutinib,zanubrutinib和acalabrutinib(100 nM)。计算每种酶的对照活性百分比。[3]
LOXO-305和伊布替尼均能有效抑制IgM诱导的磷酸化BTK,LOXO-30的IC50值为1.34±1.23 nM(n=7,p<0.0001),伊布替尼为1.04±1.26 nM(n=7,p>0.0001)。我们还发现BTK的直接下游效应物PLCγ2(Y1217)的磷酸化显著降低(每种药剂的IC50为33 nM,n=7,LOXO-305的p=0.02,伊布替尼的p=0.0017)。[1] BTK激酶活性测定:将重组野生型或突变型BTK(C481S、C481R)与ATP(10 μM)和荧光标记肽底物在系列稀释的Pirtobrutinib (LOXO-305)存在下共同孵育。30°C孵育60分钟后,通过均相时间分辨荧光(HTRF)检测磷酸化底物,采用非线性回归计算IC50值[3] - 表面等离子体共振(SPR)结合实验:将BTK蛋白固定在传感器芯片上,向芯片上注射系列稀释的Pirtobrutinib (LOXO-305)。通过测量折射率变化确定结合亲和力(Ki),数据采用1:1结合模型分析[3] - 激酶选择性面板测定:将Pirtobrutinib (LOXO-305)(100 nM)对468种激酶进行筛选;仅BTK及密切相关的TEC家族激酶显示>50%的抑制率,证实其高靶点选择性[3] |
| 细胞实验 |
在加入原钒酸盐之前,用LOXO-305、伊布替尼或阿克拉布替尼处理瞬时表达WT BTK和BTK C481取代突变的HEK293T细胞系30分钟。在2小时的孵育期后,裂解细胞,并使用MesoScale(C481R)或免疫印迹(BTK-WT、C481S和C481T)鉴定总BTK和磷酸化的Y223-BTK。使用GraphPad Prism,对频带和MSD信号进行量化,并计算IC50值。
细胞增殖实验:将BTK依赖性或非依赖性癌细胞接种于96孔板(5 × 103个细胞/孔),用Pirtobrutinib (LOXO-305)(0.1 nM–10 μM)处理72小时。使用四唑盐类试剂评估细胞活力,在490 nm波长下读取吸光度值。从剂量-反应曲线推导IC50值[3] - 信号抑制Western blot检测:用Pirtobrutinib (LOXO-305)(0.5–50 nM)处理Jeko-1或Jeko-1-C481S细胞2小时后,用冰浴裂解缓冲液裂解细胞。裂解物经SDS-PAGE分离后转移至PVDF膜,用pBTK、总BTK、pAKT、pERK1/2及GAPDH抗体进行免疫印迹。通过光密度法量化条带强度[3] - 凋亡实验:用Pirtobrutinib (LOXO-305)(100 nM)处理CLL或MCL细胞72小时后,收集细胞并与Annexin V-FITC/PI染色。通过流式细胞术分析凋亡细胞,合并早期和晚期凋亡细胞进行计数[3] - 原代CLL细胞实验:分离患者来源的原代CLL细胞,用Pirtobrutinib (LOXO-305)(10–1000 nM)处理48小时。通过台盼蓝排斥法测量细胞活力,Western blot检测pBTK水平[3] |
| 动物实验 |
将OCI-Ly10细胞皮下植入雄性非肥胖糖尿病/重症联合免疫缺陷小鼠体内,并使其肿瘤生长至约150至200 mm³的体积。根据肿瘤大小将小鼠随机分组,并每日两次(BID)口服给予10或50 mg/kg的吡托布替尼(每组12只小鼠)或载体(每组11只小鼠),持续28天。在研究期间每周测量三次肿瘤体积,并在给药后额外测量35天(Axis Bioservices,英国科尔雷恩)。在TMD8研究中,将细胞皮下注射到Balb/c SCID小鼠体内,并使其生长19天,直至平均肿瘤体积达到400 mm³。根据肿瘤大小将小鼠随机分组,并分别口服给予15或30 mg/kg的吡托布替尼(每组10只小鼠),每日两次,持续18天;或口服给予载体(每组10只小鼠),持续14天。每周测量三次肿瘤体积。将REC-1细胞皮下注射到雌性无胸腺裸鼠体内,培养18天,直至平均肿瘤体积达到150 mm³。根据肿瘤体积将小鼠随机分组,并分别口服给予10、30或50 mg/kg的吡托布替尼(每组6只小鼠),每日两次,持续21天;或口服给予载体(每组10只小鼠)。每周测量两次肿瘤体积。将表达BTK C481S的TMD8细胞注射到雌性Balb/c SCID小鼠体内,培养12天,直至平均肿瘤体积达到150 mm³。根据肿瘤大小将小鼠随机分组,并分别以3、10和30 mg/kg的剂量(每组10只小鼠)或载体(每组14只小鼠)每日两次口服给药,持续14天。每周测量肿瘤体积2或3次。OCI-Ly10异种移植瘤研究的动物实验操作均遵循英国1986年《动物(科学程序)法》的指导原则。TMD8和TMD8 BTK C481S研究中使用的小鼠按照国际实验动物评估和认证协会(AAALAC)的指南进行处理,实验方案已获得法国教育、高等研究和研究部的批准。 REC-1异种移植研究中使用的所有程序均符合美国农业部《动物福利法》(9 CFR 第1、2和3部分)以及《实验动物饲养和使用指南》(美国国家科学院出版社,华盛顿特区,实验动物研究所)[3]。
异种移植肿瘤模型:将5 × 10⁶个Jeko-1或Jeko-1-C481S细胞皮下注射到6-8周龄的雌性裸鼠体内。当肿瘤体积达到100-150 mm³时,将小鼠随机分为载体组和治疗组(每组n = 8)。Pirtobrutinib (LOXO-305)配制成0.5%羟丙基甲基纤维素/0.1% Tween 80的口服混悬液,每日两次,每次25-30 mg/kg,连续给药21天。每3天测量一次肿瘤体积[3] - PDX模型:将患者来源的CLL或MCL组织皮下植入NSG小鼠体内。当肿瘤体积达到150–200 mm³时,小鼠接受Pirtobrutinib (LOXO-305)(20–30 mg/kg,口服,每日两次)治疗28天。记录肿瘤重量和体积,并收集肿瘤组织进行Western blot分析[3] - 药代动力学研究:小鼠、大鼠和犬单次口服Pirtobrutinib (LOXO-305)(小鼠10 mg/kg,大鼠和犬5 mg/kg)。在预定时间点采集血样,并通过LC-MS/MS测定血浆药物浓度,以计算PK参数[3] |
| 药代性质 (ADME/PK) |
吸收、分布和排泄
单次口服剂量为 300 mg 至 800 mg(相当于批准推荐剂量的 1.5 至 4 倍)或每日一次口服剂量为 25 mg 至 300 mg(相当于推荐剂量的 0.125 至 1.5 倍)时,吡托替尼的药代动力学特征呈剂量比例关系。每日一次给药 5 天内,吡托替尼达到稳态浓度,基于 200 mg 剂量后的 AUC,其累积比率为 1.63。在推荐剂量下,吡托替尼的稳态 AUC 和 Cmax 分别为 91300 h⋅ng/mL 和 6460 ng/mL。在第 1 个治疗周期的第 8 天,吡托替尼的 AUC0-24 为 81800 h⋅ng/mL,Cmax 为 3670 ng/mL。吡托替尼在大约 2 小时后达到血浆峰浓度 (tmax)。单次口服 200 mg 吡托替尼后,其绝对生物利用度为 85.5%。对健康受试者给予高脂高热量餐后,吡托替尼的药代动力学未见临床意义上的显著影响。高脂餐使吡托替尼的 Cmax 降低了 23%,tmax 延迟了 1 小时,但对 AUC 无影响。 吡托替尼主要经尿液和粪便排泄。在健康受试者单次服用 200 mg 放射性标记的吡托布替尼后,57% 的剂量从尿液中回收(10% 为原形),37% 从粪便中回收(18% 为原形)。 吡托布替尼的表观中心分布容积为 32.8 L。 吡托布替尼的表观清除率为 2.02 L/h。 代谢/代谢物 体外研究表明,吡托布替尼主要通过 CYP3A4 代谢,并通过 UGT1A8 和 UGT1A9 直接进行葡萄糖醛酸化。 生物半衰期 吡托布替尼的有效半衰期约为 19 小时。 在人体中,口服吡托布替尼(LOXO-305)(每日一次,每次 200 mg)显示出生物利用度。达 82 ± 7%,给药后 2 小时达到血浆峰浓度 (Cmax) 为 3.8 ± 0.5 μM [3] - 血浆半衰期 (t1/2) 为 18.2 ± 2.3 小时(人),12.5 ± 1.8 小时(大鼠),15.7 ± 2.1 小时(狗);人体的 AUC0–24h 为 42.6 ± 5.8 μM·h [3] - 小鼠组织分布分析显示,药物在脾脏(组织/血浆比值 = 4.7 ± 0.6)、淋巴结(4.2 ± 0.5)和肿瘤(3.8 ± 0.4)中高度蓄积,在肝脏(2.3 ± 0.3)和肾脏(2.1 ± 0.2)中分布中等 [3] - 人肝微粒体代谢研究表明,Pirtobrutinib (LOXO-305) 主要通过 CYP3A4 代谢,CYP2C19 和 CYP2D6 的贡献较小 [3] - 肾脏排泄约占人体药物总清除量的 12%,粪便排泄约占 78% [3] |
| 毒性/毒理 (Toxicokinetics/TK) |
肝毒性
在皮托布替尼治疗各种B细胞相关恶性肿瘤患者的开放标签上市前临床试验中,高达23%的皮托布替尼治疗患者出现血清转氨酶升高。这些升高通常较轻且短暂,但2%至3%的患者出现超过正常值上限(ULN)5倍以上的升高。这些升高有时会导致暂时停药,但更多时候即使不调整剂量也能自行恢复正常。在上市前研究中,未发现与皮托布替尼相关的伴有症状的急性肝损伤或黄疸病例。自皮托布替尼获批上市并广泛应用以来,尚未有与其使用相关的肝毒性报告发表。然而,其他布鲁顿酪氨酸激酶抑制剂(主要是伊布替尼)也曾报道过药物性肝损伤,包括急性肝衰竭和死亡,并且一些病例与乙型肝炎病毒再激活有关,而乙型肝炎病毒再激活可能致命。 可能性评分:E(未经证实,但怀疑是临床上明显的肝损伤以及慢性乙型肝炎再激活的罕见原因)。 妊娠和哺乳期影响 ◉ 哺乳期用药概述 目前尚无关于吡布替尼在哺乳期临床应用的信息。该药与血浆蛋白的结合率为96%,因此乳汁中的浓度可能很低。制造商建议在接受吡托布替尼治疗期间以及末次给药后1周内停止母乳喂养。 ◉ 对母乳喂养婴儿的影响 截至修订日期,未找到相关的已发表信息。 ◉ 对哺乳和母乳的影响 截至修订日期,未找到相关的已发表信息。 蛋白结合 吡托布替尼的人体蛋白结合率为96%,与体外浓度无关。吡托布替尼的血血浆比为0.79。 在一项为期28天的大鼠重复给药毒性研究中(口服剂量为10、30、100 mg/kg/天),吡托布替尼(LOXO-305) 未引起明显的体重减轻或死亡;在 100 mg/kg 剂量下观察到 ALT 轻度升高(≤1.4×正常值上限)[3] - 在犬类(28 天研究,剂量分别为 5、15 和 50 mg/kg/天)中,剂量高达 50 mg/kg/天时,未观察到对血液学参数、肾功能(BUN、肌酐)或组织病理学的不良影响[3] - 通过平衡透析法测定,Pirtobrutinib (LOXO-305) 的血浆蛋白结合率分别为 95 ± 2%(人血浆)、93 ± 3%(大鼠血浆)和 94 ± 2%(犬血浆)[3] - 在人体中,每日一次剂量高达 400 mg 时,未观察到明显的 QT 间期延长[3] - 在临床研究中,常见不良事件包括疲劳 (28%)、腹泻 (22%) 和恶心(18%),未报告3-4级毒性反应[3] |
| 参考文献 |
[1]. Blood (2019) 134 (Supplement_1): 478. [2]. Blood (2019) 134 (Supplement_1): 4644.[3]. Blood . 2023 Jul 6;142(1):62-72. doi: 10.1182/blood.2022018674. |
| 其他信息 |
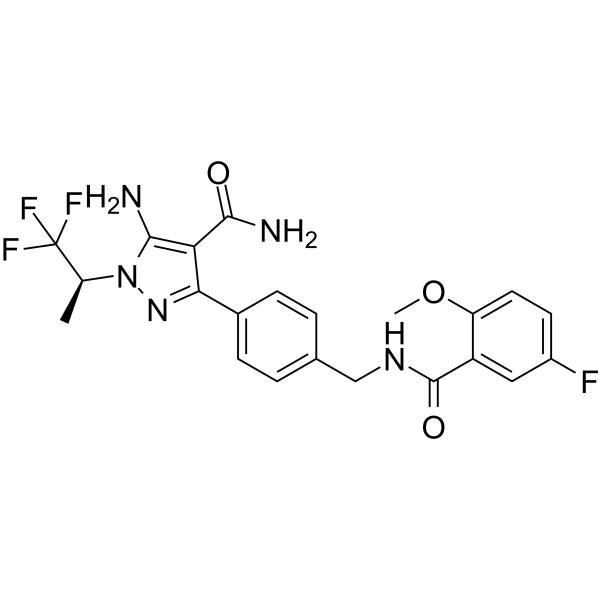
吡托布替尼是一种仲酰胺,由5-氟-2-甲氧基苯甲酸的羧基与5-氨基-3-[4-(氨甲基)苯基]-1-[(2S)-1,1,1-三氟丙-2-基]-1H-吡唑-4-甲酰胺的氨基缩合而成。它是一种BTK抑制剂,用于治疗成人慢性淋巴细胞白血病或小淋巴细胞淋巴瘤。它具有多种药理作用,包括作为EC 2.7.10.2(非特异性蛋白酪氨酸激酶)抑制剂、抗肿瘤药和细胞凋亡诱导剂。它是一种单甲氧基苯,属于单氟苯类、苯甲酰胺类、仲羧酰胺类、伯羧酰胺类、有机氟化合物、吡唑类和伯氨基化合物。
吡托布替尼是一种小分子,也是布鲁顿酪氨酸激酶 (BTK) 的高选择性非共价抑制剂。其高选择性与较低的不良事件停药率和较低的房颤发生率相关。与结合于 BTK 活性位点内半胱氨酸 481 (Cys481) 的 BTK 共价抑制剂(例如伊布替尼)不同,吡托布替尼即使在存在 Cys481 突变的情况下也能保持其抑制活性。尽管共价BTK抑制剂的耐药机制尚未完全阐明,但Cys481突变似乎是共价BTK抑制剂耐药的最常见原因。然而,其他突变也可能导致对非共价BTK抑制剂(例如吡托替尼)的耐药。2023年1月,吡托替尼获FDA加速审批途径批准用于治疗至少接受过两线系统治疗后复发或难治性套细胞淋巴瘤(MCL)。 吡托替尼是一种激酶抑制剂。吡托替尼的作用机制是作为布鲁顿酪氨酸激酶抑制剂、P-糖蛋白抑制剂、细胞色素P450 2C8抑制剂、细胞色素P450 2C19抑制剂、细胞色素P450 3A抑制剂和乳腺癌耐药蛋白抑制剂。 吡托替尼是一种口服小分子布鲁顿酪氨酸激酶抑制剂,用于治疗慢性淋巴细胞白血病和淋巴瘤。吡托替尼治疗期间通常会导致血清转氨酶水平短暂且轻微升高,但尚未发现与临床上明显的急性肝损伤病例相关。 吡托替尼是一种口服、选择性、非共价的布鲁顿酪氨酸激酶(BTK)抑制剂,具有潜在的抗肿瘤活性。口服后,吡托布替尼可选择性地、可逆地与BTK结合。这既能阻止B细胞抗原受体(BCR)信号通路的激活,又能阻止BTK介导的下游生存通路的激活,从而抑制过表达BTK的恶性B细胞的生长。LOXO-305的可逆结合可能在某些获得性耐药突变(包括C481突变的BTK)存在的情况下保持抗肿瘤活性,并限制抑制其他非BTK激酶相关的毒性。BTK是Src相关BTK/Tec家族胞质酪氨酸激酶的成员,在B细胞恶性肿瘤中过表达或发生突变。它在B淋巴细胞的发育、激活、信号传导、增殖和存活中发挥着重要作用。 药物适应症 Pirtobrutinib适用于治疗至少接受过两线系统治疗(包括BTK抑制剂)后复发或难治性套细胞淋巴瘤(MCL)的成人患者。 套细胞淋巴瘤(MCL)的治疗 作用机制 布鲁顿酪氨酸激酶(BTK)是一种位于细胞质中的酪氨酸激酶,激活后被募集到细胞质中。在B细胞中,BTK参与B细胞抗原受体(BCR)信号传导和细胞因子受体通路的激活,这两个通路对于B细胞的发育、功能、黏附和迁移都至关重要。因此,抑制BTK是治疗B细胞肿瘤的重要靶点。吡托布鲁替尼以非共价方式与布鲁顿酪氨酸激酶 (BTK) 结合并抑制其活性。与其他以共价方式与 BTK 活性位点结合的 BTK 抑制剂不同,即使该区域存在突变(例如 Cys481 突变),吡托布鲁替尼的抑制活性仍然得以维持。在非临床研究中,吡托布替尼抑制了BTK介导的B细胞CD69表达,并抑制了恶性B细胞增殖。 吡托布替尼(LOXO-305)是一种非共价、高选择性的BTK抑制剂,旨在克服B细胞恶性肿瘤对共价BTK抑制剂(伊布替尼、阿卡替尼)的耐药性[3] - 该药物可逆地与BTK(野生型和突变型)的ATP结合口袋结合,抑制激酶活性和下游B细胞受体(BCR)信号通路,这些通路对肿瘤细胞存活至关重要[3] - 2023年获得FDA批准,用于治疗复发或难治性套细胞淋巴瘤(MCL)和慢性淋巴细胞白血病(CLL)/小淋巴细胞淋巴瘤(SLL)成人患者[3] -在临床试验中,Pirtobrutinib (LOXO-305) 在 C481S 突变型 CLL 患者中总缓解率 (ORR) 为 73%,在复发/难治性 MCL 患者中总缓解率为 58% [3] |
| 分子式 |
C22H21F4N5O3
|
|---|---|
| 分子量 |
479.4356
|
| 精确质量 |
479.1581
|
| 元素分析 |
C, 55.12; H, 4.42; F, 15.85; N, 14.61; O, 10.01
|
| CAS号 |
2101700-15-4
|
| 相关CAS号 |
(R)-Pirtobrutinib;2101700-14-3
|
| PubChem CID |
129269915
|
| 外观&性状 |
White to yellow solid powder
|
| 密度 |
1.44±0.1 g/cm3
|
| 沸点 |
619.2±55.0 °C
|
| LogP |
3.3
|
| tPSA |
125Ų
|
| 氢键供体(HBD)数目 |
3
|
| 氢键受体(HBA)数目 |
9
|
| 可旋转键数目(RBC) |
7
|
| 重原子数目 |
34
|
| 分子复杂度/Complexity |
719
|
| 定义原子立体中心数目 |
1
|
| SMILES |
FC([C@H](C)N1C(=C(C(N)=O)C(C2C=CC(CNC(C3C=C(C=CC=3OC)F)=O)=CC=2)=N1)N)(F)F
|
| InChi Key |
FWZAWAUZXYCBKZ-NSHDSACASA-N
|
| InChi Code |
InChI=1S/C22H21F4N5O3/c1-11(22(24,25)26)31-19(27)17(20(28)32)18(30-31)13-5-3-12(4-6-13)10-29-21(33)15-9-14(23)7-8-16(15)34-2/h3-9,11H,10,27H2,1-2H3,(H2,28,32)(H,29,33)/t11-/m0/s1
|
| 化学名 |
5-amino-3-[4-[[(5-fluoro-2-methoxybenzoyl)amino]methyl]phenyl]-1-[(2S)-1,1,1-trifluoropropan-2-yl]pyrazole-4-carboxamide
|
| 别名 |
Pirtobrutinib; LY-3527727; Jaypirca; LOXO-305; LY 3527727; LOXO305; LY3527727; LOXO 305; JAYPIRCA; RXC-005; LY3527727; JNA39I7ZVB
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month 注意: 请将本产品存放在密封且受保护的环境中(例如氮气保护),避免吸湿/受潮。 |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
DMSO: 50~96 mg/mL (104.3~200.2 mM)
Ethanol: ~48 mg/mL (~100.1 mM) |
|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: 2.75 mg/mL (5.74 mM) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (这些助溶剂从左到右依次添加,逐一添加), 悬浮液;超声助溶。
例如,若需制备1 mL的工作液,可将100 μL 27.5 mg/mL澄清DMSO储备液加入900 μL 20% SBE-β-CD生理盐水溶液中,混匀。 *20% SBE-β-CD 生理盐水溶液的制备(4°C,1 周):将 2 g SBE-β-CD 溶解于 10 mL 生理盐水中,得到澄清溶液。 配方 2 中的溶解度: ≥ 2.75 mg/mL (5.74 mM) (饱和度未知) in 10% DMSO + 90% Corn Oil (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 例如,若需制备1 mL的工作液,可将 100 μL 27.5 mg/mL 澄清 DMSO 储备液加入900 μL 玉米油中,混合均匀。 View More
配方 3 中的溶解度: ≥ 2.5 mg/mL (5.21 mM) (饱和度未知) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 配方 4 中的溶解度: ≥ 2.5 mg/mL (5.2 mM) in 10% DMSO + 40% PEG300 + 5% Tween80 + + 45% Saline ≥ 2.5 mg/mL (5.2 mM) in 10% DMSO + 90% (20% SBE-β-CD in saline) ≥ 2.5 mg/mL (5.2 mM) in 10% DMSO + 90% Corn oil 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.0858 mL | 10.4288 mL | 20.8577 mL | |
| 5 mM | 0.4172 mL | 2.0858 mL | 4.1715 mL | |
| 10 mM | 0.2086 mL | 1.0429 mL | 2.0858 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT05024045 | Active Recruiting |
Drug: Pirtobrutinib Drug: LOXO-338 |
Multiple Myeloma B-cell Lymphoma |
Eli Lilly and Company | September 30, 2021 | Phase 1 |
| NCT03740529 | Active Recruiting |
Drug: Pirtobrutinib Drug: Venetoclax |
B-cell Lymphoma Mantle Cell Lymphoma |
Loxo Oncology, Inc. | November 16, 2018 | Phase 1 Phase 2 |
| NCT05529069 | Recruiting | Drug: Pirtobrutinib Drug: Venetoclax |
Mantle Cell Lymphoma Non Hodgkin Lymphoma |
M.D. Anderson Cancer Center | January 25, 2023 | Phase 2 |
| NCT05734495 | Active Recruiting |
Drug: Pirtobrutinib Drug: Venetoclax |
Waldenstrom Macroglobulinemia | Dana-Farber Cancer Institute | May 2, 2023 | Phase 2 |
| NCT05317936 | Recruiting | Drug: Pirtobrutinib Drug: Venetoclax |
Chronic Lymphocytic Leukemia Small Lymphocytic Lymphoma |
M.D. Anderson Cancer Center | November 16, 2022 | Phase 2 |