| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 10 mM * 1 mL in DMSO |
|
||
| 1mg |
|
||
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| Other Sizes |
|
| 靶点 |
125 I-CXCL12-CXCR4 ( IC50 = 44 nM ); 125 I-CXCL12-CXCR4; HIV-1 (NL4.3 strain) ( IC50 = 9 nM ); HIV-1 ( EC50 = 1-10 nM ); HIV-2 ( EC50 = 1-10 nM )
CXCR4 receptor (Ki = 4.1 nM, human; IC50 = 7.5 nM for CXCL12 binding inhibition) [1][5] - CXCR7 receptor (Ki = 35 nM, human; weak agonist activity) [1] - No significant affinity for CXCR1/CXCR2/CXCR3 receptors (Ki > 1000 nM) [1][5] |
|---|---|
| 体外研究 (In Vitro) |
Plerixafor 抑制 CXCL12 介导的趋化作用,其效力略优于其对 CXCR4 的亲和力。 Plerixafor 还拮抗 SDF-1/CXCL12 配体结合,IC50 为 651 nM。 Plerixafor 抑制 SDF-1 介导的 GTP 结合、SDF-1 介导的钙流和 SDF-1 刺激的趋化性,IC50 分别为 27 nM、572 nM 和 51 nM。当用同源配体刺激时,Plerixafor 不会抑制针对表达 CXCR3、CCR1、CCR2b、CCR4、CCR5 或 CCR7 的细胞的钙流,Plerixafor 也不抑制 LTB4 的受体结合。 Plerixafor 本身不会诱导 CCRF-CEM 细胞中的钙流,该细胞表达多种 GPCR,包括 CXCR4、CCR4 和 CCR7。细胞测定:Plerixafor 8HCl 可抑制 I-SDF-1 配体与表达 CXCR4 的 CCRF-CEM T 淋巴母细胞的结合。 Plerixafor 8HCl 可阻断 CXCR4 激活、SDF-1 介导的钙流和 SDF-1 介导的趋化性,IC50 值分别为 27.3、572 和 51 nM。
Plerixafor 8HCl (AMD3100)(普乐沙福八盐酸盐)是选择性CXCR4拮抗剂,对CXCR7有弱结合力,与其他CXCR家族成员无交叉反应[1][5] - 在HIV-1感染的CD4+ T细胞中,Plerixafor 8HCl(0.1-10 μM)通过阻断CXCR4介导的融合抑制病毒进入,对HIV-1 X4亚型的IC50为0.8 μM[5] - 在人胶质母细胞瘤(U87)细胞中,Plerixafor 8HCl(1-100 nM)阻断CXCL12诱导的跨内皮迁移60-85%,抑制CXCR4介导的ERK1/2磷酸化[1][2] - 在大鼠肾成纤维细胞中,Plerixafor 8HCl(0.1-10 μM)减少TGF-β诱导的I型胶原蛋白表达45-65%,抑制成纤维细胞增殖(IC50 = 5.2 μM)[3] - 在小鼠小胶质细胞(BV2)中,Plerixafor 8HCl(1-5 μM)减弱CXCL12诱导的促炎细胞因子(TNF-α、IL-6)生成30-50%[2] - 对CXCR7有弱激动活性(100 nM浓度下),使细胞内cAMP水平增加1.8倍,无下游促肿瘤信号激活[1] |
| 体内研究 (In Vivo) |
单次局部应用 Plerixafor 可通过增加细胞因子的产生、动员骨髓 EPC 以及增强成纤维细胞和单核细胞/巨噬细胞的活性来促进糖尿病小鼠的伤口愈合,从而增加血管生成和血管生成。连续五天向小鼠群组施用 PBS、IGF1、PDGF、SCF 或 VEGF,并在第 5 天施用 Plerixafor。与 PDGF、SCF 和 VEGF 联合 Plerixafor 治疗组相比,IGF1 加 Plerixafor 注射小鼠的集落数量和大小最高。
在人胶质母细胞瘤(U87)异种移植裸鼠中,腹腔注射Plerixafor 8HCl(5 mg/kg/天,连续14天)减少肿瘤体积42%,降低肿瘤微血管密度38%,同时抑制小胶质细胞活化[2] - 在单侧输尿管梗阻(UUO)诱导的肾纤维化小鼠中,Plerixafor 8HCl(2 mg/kg,腹腔注射,隔天一次,连续14天)减少肾胶原蛋白沉积55%,抑制促血管生成细胞向肾脏归巢[3] - 在链脲佐菌素(STZ)诱导的糖尿病小鼠中,Plerixafor 8HCl(1 mg/kg,静脉注射,每周两次,连续8周)减轻心脏纤维化40%,改善左心室舒张功能[4] - 在HIV-1感染的人源化小鼠中,Plerixafor 8HCl(3 mg/kg,静脉注射,每周一次,连续4周)使外周血病毒载量降低1.8 log10拷贝/mL[5] |
| 酶活实验 |
对于针对 CXCR4 的竞争性结合研究,将 5 × 105 CCRF-CEM 细胞和 100 pM 125I-SDF-1α (2200 Ci/mmol) 在结合缓冲液中于 4 °C 下孵育三小时( Milipore DuraporeTM 过滤板中含有 5 mM MgCl2、1 mM Ca Cl2、0.25% BSA、pH 7.4 的 PBS。用冷 50 mM HEPES 和 0.5 M NaCl pH 7.4 洗涤后,未结合的125I-SDF-1α 被消除。在表达重组 BLT1 的 CHO-S 细胞膜上进行竞争结合测定。膜制备涉及的步骤包括机械细胞裂解、高速离心、在含有 5 mM MgCl22 的 50 mm HEPES 缓冲液中重悬以及快速冷冻。检测混合物包含 50 mM Tris,pH 7.4、10 mM MgCl2、10 mM CaCl2、4 nM LTB4 以及 1 nM 3 H-LTB4 (195.0 Ci/mmol) 和 8 μg 膜与 Plerixafor 在室温下孵育一小时。过滤用于在 Millipore GF-C 型滤板上分离未结合的 3H-LTB4。
CXCR4/CXCR7受体结合实验:制备表达人CXCR4/CXCR7的CHO细胞膜制剂,与[125I]-CXCL12(0.1 nM)及不同浓度的Plerixafor 8HCl(0.01-1000 nM)在25°C孵育60分钟。在过量未标记CXCL12存在下测定非特异性结合,过滤分离结合态配体,定量放射性强度以计算Ki值[1][5] - CXCR4介导的ERK1/2磷酸化实验:U87细胞饥饿12小时后,经Plerixafor 8HCl(0.1-100 nM)预处理20分钟,再用CXCL12(10 nM)刺激10分钟。Western blot分析细胞裂解物,定量磷酸化ERK1/2水平[1][2] - HIV-1进入抑制实验:CD4+ T细胞与Plerixafor 8HCl(0.01-100 μM)孵育30分钟后,用HIV-1 X4亚型(MOI = 0.1)感染48小时。ELISA法检测上清液中病毒p24抗原水平,确定IC50[5] |
| 细胞实验 |
U87MG 细胞以 6x103 个细胞、200 μL/孔的密度接种到 96 孔板中后,用 CXCL12、Plerixafor 或肽 R 进行处理,如前面的“治疗”部分中所述。在治疗的最后两个小时内,在 24、48 和 72 小时添加 MTT (5 μg/mL)。除去细胞培养基后,添加 100 μL DMSO,并使用 LT-4000MS 酶标仪测量 595 nm 处的光密度。从三个独立的实验中进行三次重复测量[2]。
肿瘤细胞跨内皮迁移实验:人脐静脉内皮细胞(HUVECs)在Transwell小室上培养至融合。经Plerixafor 8HCl(1-100 nM)预处理30分钟的U87细胞加入上室,下室加入CXCL12(10 nM)。24小时后计数迁移细胞[1][2] - 肾成纤维细胞增殖实验:大鼠肾成纤维细胞接种于96孔板,经Plerixafor 8HCl(0.1-100 μM)联合TGF-β(10 ng/mL)处理72小时。MTT法测定细胞活力,Western blot检测I型胶原蛋白表达[3] - 小胶质细胞细胞因子生成实验:BV2小胶质细胞经Plerixafor 8HCl(1-5 μM)预处理1小时后,用CXCL12(10 nM)刺激24小时。ELISA法定量上清液中TNF-α和IL-6水平[2] |
| 动物实验 |
Mice: The mice used are male C57bl/6s, aged 6-7 weeks and weighing 20 g. After a week of a 22°C temperature and a 12 hr /12 hr light/dark cycle, the animals are acclimated to their new home in SPF. Next, they are split into three experimental groups at random, each containing eight mice: normal (no special treatment), UUO+AMD3100 (mice that underwent UUO surgery plus 2 mg/kg AMD3100), and UUO+PBS (mice that underwent UUO surgery plus the same amount of PBS). Every day until sacrifice, intraperitoneal injections of AMD3100 and PBS are given.
Rats: In the type 2 diabetic sand rat model, the CXCR4 antagonist AMD3100 dissolved in H2O is administered at a dose of 6 mg/kg per day for eight weeks. The impact of CXCR4 antagonism (AMD3100 6mg/kg/d) on the quantity of regulatory T cells is investigated in complementary investigations. For the duration of one week, the AMD3100 or vehicle is supplied via minipump for these investigations. Human glioblastoma xenograft model: Female nude mice (18-22 g) were subcutaneously inoculated with U87 cells (2×10⁶ cells/mouse). When tumors reached 100 mm³, Plerixafor 8HCl dissolved in normal saline was administered intraperitoneally at 5 mg/kg/day for 14 days. Tumor volume, microvessel density, and microglia reactivity were evaluated [2] - UUO-induced renal fibrosis model: Male C57BL/6 mice (20-25 g) underwent unilateral ureteral obstruction. Plerixafor 8HCl (2 mg/kg) dissolved in saline was injected intraperitoneally every other day for 14 days. Renal collagen deposition and pro-angiogenic cell homing were analyzed [3] - Diabetic cardiac fibrosis model: Male C57BL/6 mice were induced with STZ (50 mg/kg i.p. for 5 days). Two weeks post-diabetes induction, Plerixafor 8HCl (1 mg/kg) was administered intravenously twice weekly for 8 weeks. Cardiac fibrosis and left ventricular function were measured [4] - HIV-1 humanized mouse model: Humanized BLT mice were infected with HIV-1 X4 strain (1×10⁵ TCID50). Plerixafor 8HCl (3 mg/kg) was injected intravenously once weekly for 4 weeks. Peripheral blood viral load and CD4+ T cell counts were monitored [5] |
| 药代性质 (ADME/PK) |
Absorption
Plerixafor follows a two-compartment pharmacokinetic profile with first-order absorption and exhibits linear kinetics between 0.04 mg/kg and 0.24 mg/kg. The pharmacokinetic profile of plerixafor in healthy subjects was similar to the one observed in patients with non-Hodgkin’s lymphoma (NHL) and multiple myeloma (MM) who received plerixafor in combination with granulocyte-colony stimulating factor (G-CSF). In addition, the clearance of plerixafor has a significant relationship with creatinine clearance (CLCR). The population pharmacokinetic analysis showed that, with increasing body weight, a mg/kg-based dosage leads to a higher plerixafor exposure (AUC0-24h). However, NHL patients (<70 kg) given a fixed dose of 20 mg of plerixafor had an AUC0-10h 1.43-fold higher than the one detected in patients given 0.24 mg/kg of plerixafor. Therefore, a body weight of 83 kg was selected as an appropriate cut-off point to transition patients from fixed to weight-based dosing. Peak concentrations are reached in approximately 30-60 minutes (tmax) following subcutaneous injection. In patients given 0.24 mg/kg of plerixafor subcutaneously after receiving 4-days of G-CSF pre-treatment, the Cmax and AUC0-24 were 887 ng/ml and 4337 ng·hr/ml, respectively. Route of Elimination Plerixafor is mainly eliminated through urine. In healthy volunteers with normal renal function given 0.24 mg/kg of plerixafor, approximately 70% of the parent drug is excreted in urine in the first 24 hours. An _in vitro_ study with MDCKII and MDCKII-MDR1 cell models found that plerixafor is not a substrate or inhibitor of P-glycoprotein. Volume of Distribution Plerixafor has an apparent volume of distribution of 0.3 L/kg. Clearance Plerixafor has a total plasma clearance of 4.38 L/h, and a renal clearance of 3.15 L/h. Metabolism / Metabolites Plerixafor is not metabolized by the liver and is not a metabolism-dependent inhibitor of major cytochrome P450 enzymes, including 1A2, 2C9, 2C19, 2D6 and 3A4. In addition, it does not induce cytochrome P450 1A2, 2B6, or 3A4 enzymes. Plerixafor is metabolically stable, and _in vivo_ studies in rats and dogs showed that the non-parent radiolabelled components in plasma and urine were Cu2+ complexes with plerixafor. This is consistent with the presence of two cyclam rings in plerixafor, which may act as potential chelating sites. Biological Half-Life Plerixafor has a distribution half-life of 0.3 hours and a terminal population half-life of 5.3 hours in patients with normal renal function. In studies with healthy subjects and patients, the terminal half-life in plasma ranges between 3 and 5 hours. In patients with non-Hodgkin lymphoma, the terminal half-life of plerixafor is 4.4 hours, and in patients with multiple myeloma, the terminal half-life is 5.6 hours. Oral bioavailability: <5% in humans (poor oral absorption; administered intravenously or subcutaneously) [5] - Plasma protein binding: 20-25% in human plasma (concentration range: 0.1-10 μg/mL) [5] - Elimination half-life: 3-5 hours in humans; 2-3 hours in mice [5] - Distribution: Volume of distribution (Vd) = 0.2-0.3 L/kg in humans, with preferential distribution to bone marrow and lymphoid tissues [5] - Excretion: 70-80% of dose excreted unchanged in urine; <10% metabolized in liver [5] |
| 毒性/毒理 (Toxicokinetics/TK) |
Hepatotoxicity
Plerixafor has not been linked to instances of significant serum enzyme elevations during therapy nor to cases of clinically apparent liver injury. In multiple large prelicensure as well as postmarketing controlled trials, neither ALT elevations or acute liver injury were mentioned as adverse events or reasons for drop out, early discontinuation of therapy or dose modification. There have been no published reports of liver injury attributed to plerixafor, and it has been used as a possible means of treatment in animal models of acute liver failure. Thus, clinically apparent liver injury due to plerixafor must be rare, if it exists at all. Likelihood score: E (unlikely cause of clinically apparent liver injury). Protein Binding The human plasma protein binding of plerixafor is up to 58%. Acute toxicity: Intravenous LD50 = 200 mg/kg in mice; 150 mg/kg in rats [5] - Subchronic toxicity (28-day intraperitoneal administration in mice): No significant hepatotoxicity or nephrotoxicity at doses up to 10 mg/kg/day; mild transient neutropenia (10% reduction) at 20 mg/kg/day [3][5] - Chronic toxicity (8-week intravenous administration in diabetic mice): No significant changes in serum creatinine, BUN, or ALT/AST levels at 1 mg/kg twice weekly [4] - Clinical side effects: Mild to moderate gastrointestinal distress (nausea, diarrhea), headache, and bone pain reported in humans; no severe organ toxicity [5] - No significant drug-drug interactions with antiretroviral agents or chemotherapeutics in preclinical studies [2][5] |
| 参考文献 |
|
| 其他信息 |
See also: Plerixafor (annotation moved to).
Plerixafor 8HCl (AMD3100) is a small-molecule CXCR4 antagonist initially developed as an anti-HIV agent, later approved for hematopoietic stem cell (HSC) mobilization [5] - Its core mechanism involves blocking the interaction between CXCR4 and its ligand CXCL12 (SDF-1α), inhibiting downstream signaling (ERK1/2, PI3K/Akt) involved in cell migration, proliferation, and survival [1][4] - Research applications include inhibition of tumor metastasis (glioblastoma, breast cancer), attenuation of organ fibrosis (renal, cardiac), and modulation of immune cell trafficking [2][3][4] - FDA-approved indication: Mobilization of HSCs from bone marrow to peripheral blood for collection and autologous transplantation in patients with non-Hodgkin lymphoma or multiple myeloma [5] - Weak binding to CXCR7 may contribute to partial agonist effects, but its therapeutic actions are primarily mediated by CXCR4 antagonism [1] |
| 分子式 |
C28H54N8.8HCL
|
|
|---|---|---|
| 分子量 |
794.47
|
|
| 精确质量 |
826.281
|
|
| 元素分析 |
C, 42.33; H, 7.87; Cl, 35.70; N, 14.10
|
|
| CAS号 |
155148-31-5
|
|
| 相关CAS号 |
Plerixafor; 110078-46-1
|
|
| PubChem CID |
65014
|
|
| 外观&性状 |
White solid powder
|
|
| 密度 |
0.962g/cm3
|
|
| 沸点 |
657.5ºC at 760mmHg
|
|
| 闪点 |
361.8ºC
|
|
| 蒸汽压 |
2.85E-33mmHg at 25°C
|
|
| LogP |
8.68
|
|
| tPSA |
78.66
|
|
| 氢键供体(HBD)数目 |
14
|
|
| 氢键受体(HBA)数目 |
8
|
|
| 可旋转键数目(RBC) |
4
|
|
| 重原子数目 |
44
|
|
| 分子复杂度/Complexity |
456
|
|
| 定义原子立体中心数目 |
0
|
|
| SMILES |
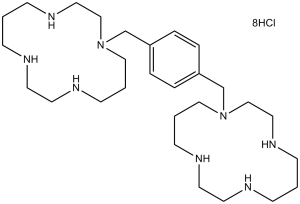
[H]Cl.[H]Cl.[H]Cl.[H]Cl.[H]Cl.[H]Cl.[H]Cl.[H]Cl.N1(CCCNCCNCCCNCC1)CC2=CC=C(C=C2)CN3CCCNCCNCCCNCC3
|
|
| InChi Key |
UEUPDYPUTTUXLJ-UHFFFAOYSA-N
|
|
| InChi Code |
InChI=1S/C28H54N8.8ClH/c1-9-29-15-17-31-13-3-21-35(23-19-33-11-1)25-27-5-7-28(8-6-27)26-36-22-4-14-32-18-16-30-10-2-12-34-20-24-36;;;;;;;;/h5-8,29-34H,1-4,9-26H2;8*1H
|
|
| 化学名 |
1-[[4-(1,4,8,11-tetrazacyclotetradec-1-ylmethyl)phenyl]methyl]-1,4,8,11-tetrazacyclotetradecane;octahydrochloride
|
|
| 别名 |
|
|
| HS Tariff Code |
2934.99.9001
|
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month 注意: 请将本产品存放在密封且受保护的环境中,避免吸湿/受潮。 |
|
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
|
|||
|---|---|---|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: 120 mg/mL (151.04 mM) in PBS (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液; 超声助溶。
配方 2 中的溶解度: Saline: 30 mg/mL 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.2587 mL | 6.2935 mL | 12.5870 mL | |
| 5 mM | 0.2517 mL | 1.2587 mL | 2.5174 mL | |
| 10 mM | 0.1259 mL | 0.6294 mL | 1.2587 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT06141304 | Active Recruiting |
Drug: Plerixafor | Relapsed Adult ALL Relapsed Adult AML |
The First Hospital of Jilin University |
September 1, 2023 | Phase 2 |
| NCT02193191 | Active Recruiting |
Drug: Plerixafor | Sickle Cell Disease | Memorial Sloan Kettering Cancer Center |
September 2014 | Phase 1 |
| NCT03182426 | Active Recruiting |
Drug: Plerixafor Drug: Alemtuzumab |
Diabetes Mellitus, Type 1 | University of Alberta | August 15, 2017 | Phase 1 Phase 2 |
| NCT03653247 | Active Recruiting |
Drug: Busulfan Biological: Plerixafor |
Sickle Cell Disease | Sangamo Therapeutics | March 6, 2019 | Phase 1 Phase 2 |
| NCT02570542 | Active Recruiting |
Drug: Plerixafor Drug: G-CSF |
Myeloma | University of Chicago | July 12, 2011 | Phase 1 |
|
|---|
|
|