| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| 1g |
|
||
| 2g |
|
||
| 5g |
|
||
| Other Sizes |
|
| 靶点 |
Bexarotene (LGD-1069) is a selective agonist of retinoid X receptors (RXRs), including RXRα, RXRβ, and RXRγ. It exhibits EC50 values of 23 nM for human RXRα, 15 nM for RXRβ, and 27 nM in a RXR-responsive luciferase reporter assay, with no significant activity on retinoic acid receptors (RARs, EC50 > 1000 nM) [1]
|
|---|---|
| 体外研究 (In Vitro) |
Bexarotene 优先结合并激活 RXR 同工型,对于 RXRα、RXRβ 和 RXRγ 同工型,Kd=14±2 nM、21±4 nM 和 29±7 nM [1]。 Bexarotene 可有效减少白血病 (HL-60) 细胞的增殖。 Bexarotene 在 1 μM 时可抑制 HL-60 细胞增殖 37% [1]。 Bexarotene 作为单药处理细胞,在高剂量下显示出抗增殖作用,IC50 为 40.62±0.45 μM (PC3) 和 50.20±4.10 μM (DU145) [2]。 Bexarotene(20 和 40 μM)和多西紫杉醇(5 和 10 μM)在抑制 PC3 和 DU145 细胞生长方面表现出协同作用 [2]。 Bexarotene(20 和 40 μM)抑制 PC3 和 DU145 细胞中细胞周期蛋白 D1 和细胞周期蛋白 D3 的表达 [2]。
RXR激活实验:在转染RXRα/β/γ表达质粒和RXR响应性荧光素酶报告基因的HEK293细胞中,贝沙罗汀(Bexarotene,LGD-1069)(1-1000 nM)呈剂量依赖性诱导荧光素酶活性。100 nM浓度下,较溶媒对照组,RXRα介导的荧光素酶活性升高8.2倍,RXRβ升高7.5倍,RXRγ升高6.8倍,证实其RXR特异性激动作用[1] - 前列腺癌细胞抗增殖实验:在人前列腺癌细胞系(PC-3、LNCaP、DU145)中,贝沙罗汀(Bexarotene,LGD-1069)(0.1-10 μM)单药处理72小时(MTT法),IC50分别为1.2 μM(PC-3)、0.8 μM(LNCaP)和1.5 μM(DU145)。与多西他赛(1 nM)联合使用时,协同增强抗增殖效应:联合组PC-3细胞活力降至22%(单药贝沙罗汀组为48%,单药多西他赛组为55%),胱天蛋白酶-3/7活性(凋亡标志物,荧光法检测)升高3.1倍[2] - 肺癌细胞实验:在小鼠Lewis肺癌(3LL)细胞和人非小细胞肺癌(NSCLC)A549细胞中,贝沙罗汀(Bexarotene,LGD-1069)(0.5-20 μM)抑制集落形成(克隆形成实验):5 μM浓度下,3LL细胞集落数减少65%,A549细胞集落数减少58%。Western blot显示,5 μM贝沙罗汀处理的3LL细胞中,细胞周期抑制剂p21表达升高2.4倍,细胞周期促进因子Cyclin D1表达降低42%[3] |
| 体内研究 (In Vivo) |
在帕金森病 (PD) 大鼠模型中,贝沙罗汀(1 mg/kg/天)可有效预防行为缺陷和多巴胺神经元变性的发生,从而显着降低血清 T4 和甘油三酯的变化 [1]。贝沙罗汀是一种能有效阻止肺部肿瘤发展和扩散的药物。在所有三种基因型(p53wt/wtK-raswt/wt、p53val135/wtK-raswt/wt 或 p53wt/wtK-rasko/wt)的小鼠中,贝沙罗汀(灌胃法 100mg/kg)抑制肿瘤多样性和肿瘤体积。贝沙罗汀使 p53wt/wtK-rasko/wt 中腺瘤进展为腺癌的速度降低了约 50%。以及 p53wt/wtK-raswt/wt 的小鼠 [3]。
前列腺癌异种移植模型:雄性裸鼠(BALB/c nu/nu,6-8周龄)皮下注射5×10⁶个PC-3细胞,待肿瘤达100-150 mm³时,随机分为4组(每组n=6):溶媒组(0.1% DMSO+生理盐水)、贝沙罗汀(Bexarotene,LGD-1069)单药组(100 mg/kg/天,口服灌胃)、多西他赛单药组(5 mg/kg/周,腹腔注射)、联合组(贝沙罗汀+多西他赛)。治疗21天后,联合组肿瘤体积减少最显著(78%,从850 mm³降至187 mm³),单药贝沙罗汀组减少42%,单药多西他赛组减少38%。肿瘤组织TUNEL实验显示,联合组凋亡细胞数增加5.2倍[2] - 小鼠肺癌模型: 1. A/J小鼠(雌性,6-8周龄)腹腔注射100 mg/kg乌拉坦诱导肺肿瘤,4周后分为2组(每组n=10):对照组(标准啮齿类饲料)、贝沙罗汀(Bexarotene,LGD-1069)组(饲料中掺入贝沙罗汀,按100 mg/kg体重/天给药,根据日均进食量计算)。喂养16周后安乐死小鼠,取肺组织用10%福尔马林固定,解剖显微镜下计数表面肿瘤数量和大小:贝沙罗汀组肺肿瘤数量减少52%(从18.3个/鼠降至8.8个/鼠),肿瘤体积减少45%(平均直径从1.2 mm降至0.66 mm)[3] 2. 携带皮下3LL肿瘤(200-250 mm³)的C57BL/6小鼠,口服贝沙罗汀(Bexarotene,LGD-1069)(50 mg/kg/天)持续14天,肿瘤体积减少48%(从920 mm³降至478 mm³),中位生存期延长30%(从26天延长至33.8天)[3] |
| 酶活实验 |
RXR响应性荧光素酶报告基因实验:HEK293细胞以5×10⁴细胞/孔接种于24孔板,含10% FBS的DMEM培养24小时。用转染试剂共转染0.5 μg人RXRα/β/γ表达质粒、0.5 μg RXR响应性荧光素酶报告质粒(含DR1型RXR结合元件)和0.1 μg β-半乳糖苷酶质粒(内参)。转染24小时后,更换为含贝沙罗汀(Bexarotene,LGD-1069)(1、10、100、1000 nM)或溶媒(0.1% DMSO)的无血清DMEM,继续孵育24小时。用报告基因裂解缓冲液裂解细胞, luminometer检测荧光素酶活性,比色法检测β-半乳糖苷酶活性以校正转染效率,非线性回归计算EC50[1]
|
| 细胞实验 |
细胞增殖测定[2]
细胞类型:人 PCa 雄激素非依赖性细胞系 PC3 和 DU145 测试浓度:5、10、20、30 , PC3 细胞为 40 μM; DU145 细胞为 1、5、10、20、40 μM。 孵育持续时间:24和48小时 实验结果:证明具有抗增殖作用,IC50分别为40.62±0.45 µM (PC3)和50.20 ±4.10 µM (DU145)。 细胞活力测定[2] 细胞类型: PC3 和 DU145 细胞 测试浓度: 20 和 40 µM <孵化持续时间:24或48小时 实验结果:24小时处理后细胞周期蛋白D1和细胞周期蛋白E2减少。治疗 48 小时后,不仅减少了细胞周期蛋白 D1 和细胞周期蛋白 E2 的表达,而且抑制了细胞周期蛋白 B1 和 CDK1 的表达。 前列腺癌细胞增殖与凋亡实验: 1. PC-3、LNCaP、DU145细胞分别以2×10³细胞/孔(PC-3/DU145)或3×10³细胞/孔(LNCaP)接种于96孔板,含10% FBS的RPMI 1640培养24小时。加入贝沙罗汀(Bexarotene,LGD-1069)(0.1-10 μM)单药或与多西他赛(1 nM)联合处理,孵育72小时。加入20 μL MTT(5 mg/mL),4小时后用DMSO溶解甲瓒结晶,570 nm处测吸光度计算细胞活力[2] 2. 凋亡检测:PC-3细胞以2×10⁵细胞/孔接种于6孔板,用贝沙罗汀(5 μM)+多西他赛(1 nM)处理48小时后裂解,使用荧光底物(Ac-DEVD-AMC)检测胱天蛋白酶-3/7活性,酶标仪检测荧光强度(激发380 nm,发射460 nm)[2] - 肺癌细胞克隆形成实验:3LL和A549细胞以500细胞/孔接种于6孔板,培养24小时后加入贝沙罗汀(Bexarotene,LGD-1069)(0.5-20 μM),孵育14天(3LL)或18天(A549)形成集落。4%多聚甲醛固定,0.1%结晶紫染色,计数>50个细胞的集落,以溶媒对照组为基准计算抑制率[3] - 细胞周期蛋白Western blot检测:3LL细胞(10 cm培养皿中2×10⁶细胞/皿)用5 μM 贝沙罗汀(Bexarotene,LGD-1069)处理48小时,含蛋白酶抑制剂的RIPA缓冲液裂解,BCA法测蛋白浓度。30 μg蛋白经10% SDS-PAGE电泳后转移至PVDF膜,一抗孵育p21、Cyclin D1和β-肌动蛋白(内参),HRP标记二抗结合后ECL显色,ImageJ定量条带灰度[3] |
| 动物实验 |
动物/疾病模型: UL53-3 小鼠(p53wt/wtK-raswt/wt、p53val135/wtK-raswt/wt 或 p53wt/wtK-rasko/wt)[3]
剂量: 100 mg/kg 给药途径: 使用 18 号灌胃针灌胃,每只小鼠每天 0.1 mL,每周 5 次,持续 12 周 实验结果: 抑制了所有三种基因型小鼠的肿瘤数量和肿瘤体积。 前列腺癌异种移植模型 (PC-3):雄性 BALB/c nu/nu 小鼠(6-8 周龄,20-22 g)饲养于 SPF 级条件下(22±2°C,12 小时光照/黑暗循环,小鼠可自由获取食物/水)。将 5×10⁶ PC-3 细胞(悬浮于 100 μL PBS + 50 μL Matrigel 中)皮下注射到小鼠右侧腹部。当肿瘤体积达到 100-150 mm³ 时,将小鼠随机分为 4 组(每组 n=6): - 赋形剂组:0.1% DMSO + 生理盐水,每日灌胃一次; - 贝沙罗汀(LGD-1069)单药组:100 mg/kg/天,溶于 0.1% DMSO + 生理盐水,每日灌胃一次; - 多西他赛单药组:5 mg/kg/周,溶于生理盐水,每周腹腔注射一次; - 联合用药组:贝沙罗汀(100 mg/kg/天,口服)+ 多西他赛(5 mg/kg/周,腹腔注射)。 治疗持续 21 天。每 3 天测量一次肿瘤体积(体积 = 长 × 宽² / 2)。第21天,处死小鼠,收集肿瘤组织进行TUNEL检测,并收集血清进行细胞因子分析[2] - 小鼠肺癌模型: 1. A/J小鼠氨基甲酸乙酯诱导肺肿瘤模型:将100 mg/kg氨基甲酸乙酯(溶于生理盐水)腹腔注射到6-8周龄、18-20 g的雌性A/J小鼠体内。四周后,将小鼠分为两组(每组n=10):对照组(标准啮齿动物饲料)和贝沙罗汀(LGD-1069)组(饲料中添加100 mg/kg体重/天的贝沙罗汀,根据平均每日食物摄入量计算)。小鼠分别饲喂上述饲料16周后处死。取出肺脏,用10%福尔马林固定,并在解剖显微镜下计数表面肿瘤的数量和大小[3] 2. C57BL/6小鼠3LL异种移植模型:将1×10⁶个3LL细胞皮下注射到6-8周龄雌性C57BL/6小鼠右侧腹部。当肿瘤体积达到200-250 mm³时,将小鼠随机分为两组(每组n=8):对照组(0.5%羧甲基纤维素钠,CMC-Na,10 mL/kg/天,灌胃)和贝沙罗汀(LGD-1069)组(50 mg/kg/天,溶于0.5% CMC-Na,灌胃)。持续治疗直至小鼠达到安乐死标准(肿瘤体积>2000 mm³或体重减轻>15%)。每日记录生存时间,每2天测量一次肿瘤体积[3] |
| 药代性质 (ADME/PK) |
吸收、分布和排泄
贝沙罗汀及其已知代谢物的排泄途径较少(<1%的给药剂量)。 口服后,贝沙罗汀被吸收,达峰时间(Tmax)约为两小时。……对晚期恶性肿瘤患者的研究表明,在治疗范围内,单次给药的药物浓度呈近似线性关系,多次给药后药物蓄积量较低。与葡萄糖溶液相比,摄入含脂肪食物后,75至300 mg剂量贝沙罗汀的血浆AUC和Cmax值分别升高35%和48%。贝沙罗汀与血浆蛋白的结合率很高(>99%)。贝沙罗汀结合的血浆蛋白尚未明确,贝沙罗汀置换与血浆蛋白结合的药物以及药物置换贝沙罗汀结合的能力也尚未研究。 在2型糖尿病患者中检测了贝沙罗汀及其代谢物的肾脏排泄情况。贝沙罗汀及其代谢物均未在尿液中大量排出。贝沙罗汀被认为主要通过肝胆系统排泄。 代谢/代谢物 已在血浆中鉴定出四种贝沙罗汀代谢物:6-羟基贝沙罗汀、7-羟基贝沙罗汀、6-氧代贝沙罗汀和7-氧代贝沙罗汀。体外研究表明,细胞色素P450 3A4是负责氧化代谢物形成的主要细胞色素P450,并且这些氧化代谢物可能发生葡萄糖醛酸化。这些氧化代谢物在类视黄醇受体激活的体外试验中具有活性,但母体化合物及其代谢物对贝沙罗汀疗效和安全性的相对贡献尚不清楚。 贝沙罗汀已知的人体代谢物包括6-羟基贝沙罗汀、7-羟基贝沙罗汀和7-氧代贝沙罗汀。 生物半衰期 7小时 贝沙罗汀的终末半衰期约为7小时。 贝沙罗汀(LGD-1069)在大鼠中的口服生物利用度约为40%,在人体中的口服生物利用度约为35%。大鼠口服100 mg/kg后,血浆峰浓度(Cmax)为2.8 μg/mL,达峰时间(Tmax)为2小时,消除半衰期(t1/2)为7.5小时。该药与血浆蛋白高度结合(>99%),并分布于多种组织,其中肝脏、脂肪组织和皮肤(皮肤T细胞淋巴瘤的靶组织)中的浓度最高[1]。代谢:贝沙罗汀(LGD-1069)主要在肝脏中通过细胞色素P450酶(CYP3A4和CYP2C8)代谢,产生无活性代谢物,这些代谢物主要通过粪便(≈60%)和尿液(≈30%)在72小时内排出[1]。 |
| 毒性/毒理 (Toxicokinetics/TK) |
肝毒性
接受贝沙罗汀治疗的患者中,约有5%会出现血清转氨酶升高,但这些异常通常较轻微、短暂,且不伴有症状或黄疸。然而,已有贝沙罗汀治疗导致临床表现明显的肝损伤并伴有黄疸的病例报道,其中一些病例病情严重甚至致命。肝毒性似乎在高剂量治疗中更为常见。目前尚未对贝沙罗汀引起的肝损伤的临床特征进行详细描述,也未见相关的肝毒性病例报告发表。然而,产品标签提及肝毒性,并建议定期监测肝功能。 可能性评分:D(可能但不常见,是临床上明显的肝损伤的原因)。 蛋白结合率 >99% 药物相互作用 由于贝沙罗汀由细胞色素P450 3A4代谢,因此酮康唑、伊曲康唑、红霉素、吉非贝齐、葡萄柚汁和其他细胞色素P450 3A4抑制剂预计会导致血浆贝沙罗汀浓度升高。此外,利福平、苯妥英钠、苯巴比妥和其他细胞色素P450 3A4诱导剂可能导致血浆贝沙罗汀浓度降低。 贝沙罗汀胶囊与吉非贝齐合用可显著升高血浆贝沙罗汀浓度,这可能至少部分与吉非贝齐抑制细胞色素P450 3A4有关。在类似条件下,阿托伐他汀合用对贝沙罗汀浓度无影响。不建议贝沙罗汀胶囊与吉非贝齐合用。 根据中期数据,贝沙罗汀胶囊与他莫昔芬合用可导致血浆他莫昔芬浓度降低约35%,这可能是由于诱导细胞色素P450 3A4所致。基于这种已知的相互作用,贝沙罗汀理论上可以提高其他经细胞色素 P450 3A4 代谢的底物的代谢速率,并降低其血浆浓度,包括口服或其他全身性激素避孕药。 如果贝沙罗汀与引起血液疾病的药物同时或近期接受治疗,且这些药物也会引起相同的白细胞减少和/或血小板减少作用,则贝沙罗汀的白细胞减少和/或血小板减少作用可能会增强;如有必要,应根据血细胞计数调整骨髓抑制剂的剂量。 有关贝沙罗汀(共 10 项)的更多相互作用(完整)数据,请访问 HSDB 记录页面。 小鼠/大鼠临床前毒性: - 每日口服贝沙罗汀 (LGD-1069)(50-200 mg/kg),持续 4 周,可引起剂量依赖性不良反应:皮肤干燥(100 mg/kg 剂量下 80% 的小鼠出现)、高脂血症(150 mg/kg 剂量下甘油三酯升高 2.3 倍,胆固醇升高 1.8 倍)和轻度肝肿大(200 mg/kg 剂量下肝脏重量增加 10%)。未观察到明显的肾毒性(血清 BUN/肌酐未改变)或骨髓抑制(外周血细胞计数正常)[1] - 在 3LL 异种移植模型[3]中,小鼠接受 50 mg/kg/天贝沙罗汀治疗 14 天后,出现轻度体重减轻(<5% 的基线)和短暂的皮肤鳞屑,停药后消退;未检测到肝脏/肾脏的组织病理学变化[3] - 临床毒性(文献[1]总结):皮肤 T 细胞淋巴瘤 (CTCL) 患者的常见不良事件包括皮肤反应(皮肤干燥、瘙痒、皮疹,65-75%)、血脂异常(高甘油三酯血症,50-60%;高胆固醇血症,30-40%)和头痛(20-25%)。 3/4级毒性反应(发生率<10%)包括严重高甘油三酯血症(需要使用降脂药物)和肝毒性(短暂性ALT/AST升高)[1] |
| 参考文献 |
|
| 其他信息 |
贝沙罗汀是一种维甲酸类药物,属于苯甲酸类和萘类化合物。它是一种抗肿瘤药物。
贝沙罗汀(Targretin)是一种抗肿瘤药物,已获美国食品药品监督管理局 (FDA) 批准用于治疗皮肤T细胞淋巴瘤。它也曾被用于治疗肺癌、乳腺癌和卡波西肉瘤等非适应症疾病。 贝沙罗汀是一种维甲酸类药物。 贝沙罗汀是一种维甲酸类似物,用于治疗皮肤T细胞淋巴瘤 (CTCL) 的皮肤表现。贝沙罗汀治疗与较高的血清酶升高率相关,但罕见情况下会出现临床上明显的急性肝损伤。 贝沙罗汀是一种合成维甲酸类药物,具有潜在的抗肿瘤、化学预防、致畸和胚胎毒性。贝沙罗汀选择性地结合并激活维甲酸X受体(RXR),从而诱导基因表达改变,导致细胞分化、细胞增殖减少、某些癌细胞类型凋亡以及肿瘤消退。(NCI04) 一种雷西诺类药物(RXR结合配体)、四氢萘衍生物和维甲酸X受体拮抗剂,用于治疗皮肤T细胞淋巴瘤。 药物适应症 口服用于治疗对至少一种既往全身治疗无效的皮肤T细胞淋巴瘤(CTCL)患者的皮肤表现。也可用于治疗早期(IA期和IB期)皮肤T细胞淋巴瘤(CTCL)患者的皮肤病变,尤其适用于对其他疗法无效或病情持续存在,或无法耐受其他疗法的患者。 FDA标签 Targretin胶囊适用于治疗对至少一种全身治疗无效的晚期皮肤T细胞淋巴瘤(CTCL)患者的皮肤表现。 作用机制 贝沙罗汀选择性地与视黄酸X受体亚型结合并激活它们。视黄酸X受体共有三个亚型:RXRα、RXRβ和RXRγ。贝沙罗汀治疗皮肤T细胞淋巴瘤(CTCL)的确切作用机制尚不清楚,但该药物对CTCL的所有临床阶段均有效。 贝沙罗汀选择性地结合并激活视黄酸X受体亚型(RXRα、RXRβ、RXRγ)。RXR可与多种受体形成异二聚体,例如视黄酸受体(RAR)、维生素D受体、甲状腺受体和过氧化物酶体增殖激活受体(PPAR)。激活后,这些受体作为转录因子,调节控制细胞分化和增殖的基因表达。贝沙罗汀在体外可抑制某些造血和鳞状细胞来源的肿瘤细胞系的生长。在某些动物模型中,它还能诱导体内肿瘤消退。贝沙罗汀治疗皮肤T细胞淋巴瘤(CTCL)的确切作用机制尚不清楚。 治疗用途 治疗类别:抗肿瘤药 贝沙罗汀适用于治疗至少一种其他既往全身治疗无效的皮肤T细胞淋巴瘤患者的皮肤表现。/美国产品标签包含/ 药物警告 可能对胎儿造成伤害;动物实验已证实其具有致畸性和胚胎致死性。目前尚无充分且对照良好的临床研究。治疗期间应避免妊娠。如果在妊娠期间使用,应告知孕妇潜在的胎儿风险。……接受该药物治疗的男性患者在与怀孕或可能怀孕的女性发生性行为时应使用避孕套。 在开始治疗前一个月、治疗期间以及停药后至少一个月内,必须采取有效的避孕措施;除非选择禁欲,否则建议同时使用两种可靠的避孕方法。贝沙罗汀可能诱导代谢酶,从而理论上降低口服或其他全身性激素避孕药的血浆浓度。在II-III期临床研究中,79%接受口服贝沙罗汀治疗的患者出现高脂血症。超过一半接受300 mg/m²或更高剂量贝沙罗汀治疗的患者出现空腹甘油三酯和胆固醇升高以及高密度脂蛋白胆固醇降低。脂质异常通常在2-4周内出现,停药后可逆转。如果空腹甘油三酯升高或在治疗期间升高,应开始降脂治疗,并减少或停用贝沙罗汀。据报道,一些接受贝沙罗汀治疗的患者出现急性胰腺炎,其中至少有一例患者死亡。生产商指出,患有皮肤T细胞淋巴瘤(CTCL)且存在胰腺炎风险因素(例如,既往胰腺炎病史、未控制的高脂血症、过量饮酒、未控制的糖尿病、胆道疾病或服用与胰腺毒性相关的药物或已知可升高甘油三酯浓度的药物)的患者通常不应接受贝沙罗汀治疗。 有关贝沙罗汀(共15条)的更多药物警告(完整)数据,请访问HSDB记录页面。 药效学 贝沙罗汀属于选择性激活维甲酸X受体(RXR)的维甲酸亚类药物。这些维甲酸受体的生物活性与维甲酸受体(RAR)不同。贝沙罗汀适用于治疗对至少一种既往全身治疗无效的皮肤T细胞淋巴瘤患者的皮肤表现。贝沙罗汀选择性地结合并激活视黄酸X受体亚型(RXRα、RXRβ、RXRγ)。RXR可与多种受体形成异二聚体,例如视黄酸受体(RAR)、维生素D受体、甲状腺受体和过氧化物酶体增殖激活受体(PPAR)。激活后,这些受体作为转录因子,调节控制细胞分化和增殖的基因表达。贝沙罗汀在体外抑制某些造血和鳞状细胞来源的肿瘤细胞系的生长。它还能在某些动物模型中诱导体内肿瘤消退。作用机制:贝沙罗汀(LGD-1069)激活RXR,RXR可与其他核受体(例如PPARγ、LXRα)形成同源二聚体或异源二聚体。激活的RXR二聚体与靶基因启动子中的特定DNA反应元件(例如DR1、DR5)结合,调节参与细胞周期阻滞(例如p21)、细胞凋亡(例如Bax)和脂质代谢(例如ABCA1)的基因的转录[1,3]。治疗应用:贝沙罗汀(LGD-1069)已获得FDA批准,用于治疗IIB-IV期难治性皮肤T细胞淋巴瘤(CTCL)患者。临床前研究[2,3]支持其在其他癌症(前列腺癌、肺癌)中的潜力,当与化疗药物(例如多西他赛)联合使用或作为化学预防剂时[1,2,3] - 与多西他赛的协同机制[2]:贝沙罗汀(LGD-1069)可使PC-3细胞中ABCB1(一种多药耐药泵)的表达下调45%,从而减少多西他赛的外排并增加细胞内药物的积累。它还能通过上调 p21 来增强多西他赛诱导的 G2/M 期细胞周期阻滞(在 PC-3 细胞中从 32% 提高到 58%)[2] - 肺癌化学预防[3]:贝沙罗汀 (LGD-1069) 通过减少癌症干细胞 (CSC) 的富集来抑制肺肿瘤进展:它将 3LL 肿瘤中 CD133⁺ CSC 的百分比从 12% 降低到 4%,并将 CSC 相关基因(例如 SOX2、Nanog)的表达下调 50-60% [3] |
| 分子式 |
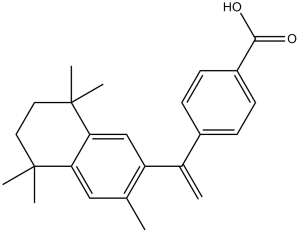
C24H28O2
|
|---|---|
| 分子量 |
348
|
| 精确质量 |
348.208
|
| CAS号 |
153559-49-0
|
| 相关CAS号 |
Bexarotene-d4;2182068-00-2
|
| PubChem CID |
82146
|
| 外观&性状 |
White to off-white solid powder
|
| 密度 |
1.0±0.1 g/cm3
|
| 沸点 |
489.7±44.0 °C at 760 mmHg
|
| 熔点 |
230-231ºC
|
| 闪点 |
229.5±23.1 °C
|
| 蒸汽压 |
0.0±1.3 mmHg at 25°C
|
| 折射率 |
1.556
|
| LogP |
8.55
|
| tPSA |
37.3
|
| 氢键供体(HBD)数目 |
1
|
| 氢键受体(HBA)数目 |
2
|
| 可旋转键数目(RBC) |
3
|
| 重原子数目 |
26
|
| 分子复杂度/Complexity |
551
|
| 定义原子立体中心数目 |
0
|
| InChi Key |
NAVMQTYZDKMPEU-UHFFFAOYSA-N
|
| InChi Code |
InChI=1S/C24H28O2/c1-15-13-20-21(24(5,6)12-11-23(20,3)4)14-19(15)16(2)17-7-9-18(10-8-17)22(25)26/h7-10,13-14H,2,11-12H2,1,3-6H3,(H,25,26)
|
| 化学名 |
4-[1-(3,5,5,8,8-pentamethyl-6,7-dihydronaphthalen-2-yl)ethenyl]benzoic acid
|
| 别名 |
LGD1069; LGD 1069; LG 100069; Ro26-445; LGD-1069; SR-11247; Ro 26 445; Targretin Ro 26-445; SR 11247; SR11247; 3-methyl TTNEB. Bexarotene; US trade name: Targretin.
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
|
|||
|---|---|---|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: 2.62 mg/mL (7.52 mM) in 5% DMSO + 40% PEG300 + 5% Tween80 + 50% Saline (这些助溶剂从左到右依次添加,逐一添加), 悬浮液;超声助溶。
*生理盐水的制备:将 0.9 g 氯化钠溶解在 100 mL ddH₂O中,得到澄清溶液。 配方 2 中的溶解度: 2.62 mg/mL (7.52 mM) in 5% DMSO + 95% (20% SBE-β-CD in Saline) (这些助溶剂从左到右依次添加,逐一添加), 悬浊液; 超声助溶。 *20% SBE-β-CD 生理盐水溶液的制备(4°C,1 周):将 2 g SBE-β-CD 溶解于 10 mL 生理盐水中,得到澄清溶液。 View More
配方 3 中的溶解度: ≥ 2.08 mg/mL (5.97 mM) (饱和度未知) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 配方 4 中的溶解度: ≥ 2.08 mg/mL (5.97 mM) (饱和度未知) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 例如,若需制备1 mL的工作液,可将100μL 20.8mg/mL澄清的DMSO储备液加入到900μL 20%SBE-β-CD生理盐水中,混匀。 *20% SBE-β-CD 生理盐水溶液的制备(4°C,1 周):将 2 g SBE-β-CD 溶解于 10 mL 生理盐水中,得到澄清溶液。 配方 5 中的溶解度: ≥ 2.08 mg/mL (5.97 mM) (饱和度未知) in 10% DMSO + 90% Corn Oil (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 例如,若需制备1 mL的工作液,可将100 μL 20.8 mg/mL 澄清 DMSO 储备液加入到 900 μL 玉米油中并混合均匀。 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.8736 mL | 14.3678 mL | 28.7356 mL | |
| 5 mM | 0.5747 mL | 2.8736 mL | 5.7471 mL | |
| 10 mM | 0.2874 mL | 1.4368 mL | 2.8736 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT05296304 | Recruiting | Drug: Bexarotene Radiation: Total Skin Electron Beam (TSEB) |
Cutaneous T-cell Lymphoma | Memorial Sloan Kettering Cancer Center |
March 16, 2022 | Phase 1 |
| NCT03323658 | Completed Has Results | Drug: Bexarotene Other: Questionnaire Administration |
Breast Atypical Ductal Hyperplasia Breast Atypical Lobular Hyperplasia |
National Cancer Institute (NCI) | June 15, 2018 | Phase 1 |
| NCT00153842 | Terminated Has Results | Drug: Bexarotene (targretin) | Carcinoma, Non-small-cell Lung | Dartmouth-Hitchcock Medical Center | August 2001 | Phase 1 Phase 2 |
| NCT01782742 | Completed Has Results | Drug: Bexarotene Drug: Placebo |
Alzheimer's Disease | The Cleveland Clinic | February 2013 | Phase 2 |