| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| 1g |
|
||
| 2g |
|
||
| 5g |
|
||
| 10g |
|
||
| Other Sizes |
|
| 靶点 |
Endogenous Metabolite; PPARβ/δ (Kd = 17 nM); PPARα (Kd = 103 nM); PPARγ (Kd = 178 nM); PPARα (IC50 = 14 nM); PPARγ (IC50 = 14 nM); RARβ (IC50 = 14 nM)
|
|---|---|
| 体外研究 (In Vitro) |
视黄酸/retinoic acid,也称为全反式视黄酸,或 ATRA,是维生素 A 的高效衍生物,几乎是所有重要的生理过程和功能所必需的。它在 530 多个不同基因的转录控制中发挥作用。视黄酸的作用机制是通过其作为核视黄酸受体 (RARα-γ) 的激活配体的作用,与视黄酸 X 受体 (RXRα-γ) 结合形成异二聚体[1]。视黄酸 (RA) 的 Kd 值在 100 至 200 nM 之间,以低亲和力与 PPARα 和 PPARγ 结合。另一方面,视黄酸与 PPARβ/δ 结合时表现出高亲和力和同种型选择性,Kd 为 17 nM [2]。视黄酸 (RA) 受体 RARα、RARβ、RARγ 和 PPARβ/δ 以及视黄酸结合蛋白 CRABP-II 和 FABP5 由未分化的 P19 细胞表达。用视黄酸处理细胞诱导分化导致 CRABP-II 短暂过度表达和 FABP5 下调,这在相关蛋白质和 mRNA 水平上检测到。经过最初的下降后,成熟神经元中的 FABP5 蛋白和 mRNA 水平与未分化的 P19 细胞相比上升了 2-2.5 倍。 PPARβ/δ和RARα的水平没有受到分化诱导的显着影响。到第 4 天,RARγ mRNA 水平下降了近 5 倍,并且在成熟神经元中保持较低水平 [3]。视黄酸 (RA) 是由视黄醇(维生素 A)产生的一种形态发生素,在细胞发育、分化和器官发生中发挥着至关重要的作用。视黄酸与视黄酸受体 (RAR) 和视黄酸 X 受体 (RXR) 相互作用,调节靶基因的表达 [4]。
UAB30是一种RXR选择性激动剂,已被证明具有潜在的癌症化学预防特性。由于其疗效高、毒性低,目前正由国家癌症研究所在人体I期临床试验中进行评估。虽然UAB30显示出作为低毒化学预防药物的前景,但其作用机制尚不清楚。在这项研究中,我们研究了UAB30对人类器官型皮筏培养物和小鼠表皮基因表达的影响。这项研究的结果表明,用UAB30治疗会导致负责全反式视黄醇摄取和代谢为全反式-视黄酸/retinoic acid(ATRA)的基因上调,ATRA是RAR核受体的天然激动剂。与这些基因表达的增加一致,ATRA在人类皮肤筏中的稳态水平升高。在紫外线B(UVB)照射的小鼠皮肤中,发现ATRA靶基因的表达减少。在UVB诱导的鳞状细胞癌和基底细胞癌小鼠模型的表皮中也观察到ATRA敏感基因的表达减少。然而,在UVB照射前用UAB30治疗小鼠皮肤可以防止UVB诱导的一些ATRA反应基因表达的降低。考虑到UAB30对表皮中的ATRA信号的积极作用及其低毒性,它可以作为一种化学预防剂用于治疗非毛细胞瘤皮肤癌症,特别是在器官移植受者和其他高危人群中。[1] 维甲酸/retinoic acid(RA)调节许多靶基因的转录,从而调节无数的生物过程。众所周知,RA通过激活视黄酸受体(RAR)发挥作用,RAR反过来控制细胞分化、增殖和凋亡。然而,已经发表了关于RA各种不同且有时相反的行为的令人困惑的报道。因此,虽然RA在某些情况下诱导细胞凋亡并抑制细胞生长,但在其他情况下,它会增强增殖并充当抗凋亡剂。这些观察结果提出了除RAR之外的信号通路可能参与调节RA活动的可能性。在这里,我们表明RA是另一种核受体的高亲和力配体,即孤儿受体过氧化物酶体增殖物激活受体(PPAR)β/δ。我们证明,虽然RA不激活PPARα和PPARγ,但它以纳摩尔亲和力与PPARβ/δ结合,调节受体的构象,促进与辅激活子SRC-1的相互作用,并有效激活PPARβ/δ介导的转录。因此,RA的转录信号传导是通过双重途径发挥的,为理解对这种激素的不同细胞反应提供了理论基础。[2] 维甲酸/retinoic acid(RA)通过激活核受体维甲酸受体(RAR)和过氧化物酶体增殖物激活受体(PPAR)β/δ及其各自的同源脂质结合蛋白CRABP-II和FABP5来调节基因转录。RA诱导神经元分化,但激素的两种转录途径对这一过程的贡献尚不清楚。在这里,我们表明RA诱导的P19干细胞向神经元祖细胞的承诺是由CRABP-II/RAR通路介导的,FABP5/PPARβ/δ通路可以通过诱导RAR阻遏物SIRT1和Ajuba来抑制这一过程。与神经发生早期阶段的抑制活性相反,FABP5/PPARβ/δ通路促进神经元祖细胞向成熟神经元的分化,这一活性部分由PPARβ/δ靶基因PDK1介导。因此,RA诱导的神经元分化在早期通过RAR介导,在晚期通过PPARβ/δ介导。RA信号传导的转换是通过RARβ的瞬时上调来实现的,同时伴随着分化早期CRABP-II/FABP5比值的瞬时增加。根据这些结论,与野生型动物相比,FABP5缺失小鼠的海马体显示出神经元祖细胞的过度积累和成熟神经元的缺陷。[3] 视黄酸(RA)是一种来源于视黄醇(维生素a)的形态发生因子,在细胞生长、分化和器官发生中起着重要作用。从视黄醇生产RA需要两组不同脱氢酶催化的连续酶促反应。视黄醇首先被氧化成视网膜,然后被氧化成RA。RA与视黄酸受体(RAR)和视黄酸X受体(RXR)相互作用,然后调节靶基因表达。在这篇综述中,我们讨论了RA的代谢和RA信号通路的重要组成部分,并强调了目前对RA在早期胚胎发育中功能的理解。[4] 维甲酸/retinoic acid(RA)通过激活RA受体(RAR)这一转录因子家族,对细胞生长和分化产生多效作用。这些受体存在三种亚型,RARα、RARβ和RARγ。受体在不同的细胞类型和发育阶段有不同的表达,这表明它们可能调节不同的基因集。我们已经鉴定出一种具有选择性RARα拮抗剂特征的合成维甲酸。这种拮抗剂可以抵消RA对HL-60细胞分化和B淋巴细胞多克隆活化的影响。除了其潜在的实际相关性外,这种和其他特定的拮抗剂将有助于剖析RAR系统,并将许多RA调节的功能分配给一个给定的受体。[5] 异硫氰酸盐和酚类抗氧化剂可以通过激活Nrf2(NF-E2 p45-相关因子2)来预防癌症,Nrf2是一种通过抗氧化反应元件(ARE)增强子控制细胞保护基因表达的转录因子。使用人乳腺MCF7-衍生的AREc32报告细胞系,我们现在报告全反式视黄酸(ATRA)和其他视黄酸受体α(RARAalpha)激动剂显著降低Nrf2介导癌症化学预防剂诱导ARE驱动基因的能力,所述化学预防剂包括丁基羟基茴香醚的代谢产物,叔丁基氢醌(tBHQ)。在AREc32细胞中,由Nrf2调节的醛酮还原酶(AKR)AKR1C1和AKR1C2基因的基础和tBHQ诱导表达也受到ATRA的抑制。RARalpha的拮抗剂增强了tBHQ对ARE驱动基因表达的诱导,使用RNAi敲除RARalpha也是如此[6]。 |
| 体内研究 (In Vivo) |
将浓度为 0.3 μM 的视黄酸 (GMP) 应用于浸入含视黄酸的鱼缸水中的胚胎后,斑马鱼在 24 和 48 小时后表现出更快的视杆细胞分化[6]。
RA抑制小鼠小肠中ARE基因库的表达。[6] 为了研究视黄酸/RA是否在体内抑制ARE调节基因的表达,将Nrf2-/-和Nrf2+/+小鼠置于维生素a缺乏(VAD)饮食中。已知通过Nrf2调节的蛋白质的蛋白质印迹显示,VAD饮食的WT小鼠小肠中Gstm5、GCLC、NQO1和Gsta1/2的水平显著增加(图6)。在VAD饮食的Nrf2−/-小鼠中,这些蛋白质的水平没有增加。对VAD饮食的WT小鼠施用维甲酸/ATRA(10mg/kg,2周腹腔注射)几乎完全阻断了小肠中Gstm5、GCLC、NQO1和Gsta1/2蛋白的增加(图6,泳道5),表明维甲酸在体内抑制Nrf2功能。对对照饮食的WT小鼠施用ATRA不影响Gstm5、GCLC、NQO1或Gsta1/2的表达(数据未显示)。 |
| 酶活实验 |
荧光滴定法[2]
细菌表达的mPPARα-LBD、mPPARβ/δ-LBD和mPPARγ-LBD(0.2-1μm)直接在试管中用溶于乙醇的视黄酸/RA滴定。乙醇浓度通常低于1%,从不超过2%。为了确保蛋白质和配体之间的平衡,监测荧光,直到达到恒定值。通过跟踪伴随RA结合的蛋白质固有荧光(激发,280 nm;发射,340 nm)的降低来监测滴定的进展。配体的内部过滤,由蛋白质饱和后观察到的线性斜率反映,如所述进行了校正。对校正后的数据进行分析,以获得平衡离解常数(Kd)。通过将数据拟合到从简单结合理论导出的方程(1)中进行分析, (方程式1) 其中F是观察到的荧光,F 0和F∞分别是无配体和饱和时的荧光,P T和R T分别是蛋白质和RA/视黄酸的总浓度,Ka是缔合常数(Ka=1/Kd)。 |
| 细胞实验 |
皮肤Raft中维甲酸/ATRA的检测[1]
将UAB30在DMSO(50 mM)中的浓缩溶液的等分试样加入培养基中,使最终浓度达到2μM。每隔一天更换一次培养基,并补充新鲜的UAB30。对照样品的培养基仅补充DMSO。收获后,将筏培养物的表皮从下面的胶原蛋白床上剥离。将UAB30处理或DMSO处理的培养物合并到三个样品中,每个样品包含五个筏,并基本上按照[52]中所述提取维甲酸。在黑暗中,将每个样品在0.5mL冰冷的磷酸盐缓冲盐水(PBS)中均质化,转移到硅化玻璃管中,并与0.5mL含有0.025M氢氧化钾的乙醇混合。用2mL己烷提取非极性维甲酸,在氮气流下干燥有机相,在50μL己烷:乙腈(70:30)中复溶,并如前所述通过反相HPLC进行分析。通过加入45μL 4M盐酸酸化剩余的水相,并用另外2mL己烷提取极性维甲酸(包括ATRA和UAB30)。将提取物干燥并在400μL乙腈中复溶。 组织样本中视黄酸/ATRA的LC-MS-MS分析基本上如前所述进行,但有一些修改。为了量化干燥提取物中存在的ATRA或UAB30的浓度,将50-μL等分试样注入岛津LC-10AD HPLC(包括脱气器),该HPLC与Applied Biosystems 4000 Q Trap质谱仪连接。用于所有分析的柱是SUPELCOSIL ABZ PLUS(10 cm x 2.1 mm,3μm)。使用梯度程序将含有40%乙腈、30%甲醇和30%超纯水的流动相A与含有55%乙腈、30%甲烷和15%超纯水的移动相B混合。每个流动相含有0.01%v/v的甲酸。用于混合流动相的梯度程序为:0至5分钟,100%A至100%B;5至19分钟,100%B;19至20分钟,100%B至100%A;20至30分钟,100%A.流动相的流速保持恒定在200μL/min。质谱仪在Analyst 1.4.2软件控制的多反应监测中使用大气压化学电离(APCI)源运行。ATRA和UAB30的停留时间为40ms。最佳阳性APCI检测条件为:幕气10、喷雾器气3、碰撞气6、离子源70和温度350°C。 每个样品注射三次,三次注射的平均值用于估算其视黄酸/ATRA或UAB30浓度。对于ATRA,四极杆1(Q1)中选择了301 m/z,四极杆3(Q3)中定量了123 m/z的离子碎片离子。对于UAB30,第一季度选择295 m/z,第三季度选择165 m/z。在分析之前,使用Analyst中的优化子程序对每个峰的去簇潜力、入口潜力、碰撞能量和碰撞单元出口潜力进行了优化。 为了定量ATRA水平,使用每种浓度3次注射的0.0-1.6 pmol/50μL视黄酸/ATRA注射液(7种浓度,变化2倍)进行校准曲线。将123m/z峰的总离子电流面积(TIC)拟合为线性方程,以建立校准曲线。将123m/z峰的TIC面积测量三次并取平均值。使用平均峰面积和线性校准曲线测定样品中ATRA的内源性浓度。除了校准曲线和定量使用165 m/z片段峰,以及在构建校准曲线时使用不同浓度范围(0.0-1.0 pmol/50μL UAB30注射液)外,UAB30使用了相同的方法。 Transient Transfection。[6] 使用Lipofectamine 2000试剂(Life Technologies)在70-80%融合率下用Nrf2表达载体转染AREc32细胞。转染后5小时,在有或没有1μM维甲酸/ATRA的情况下,用含有10μM tBHQ的新鲜DMEM替换培养基。对于对照实验,向培养基中加入模拟转染(无质粒DNA)和单独的载体(0.1%体积/体积DMSO)。在收获和分析细胞之前,将细胞放置24小时以对外源性物质产生反应。在对照实验中,将不含DNA的转染试剂单独加入细胞中,用DMSO处理2小时。 对于AREc32细胞中的RAR敲除实验,从Ambion购买了靶向RARαmRNA不同区域的两个预连接siRNA序列1(5′-GGAAUUGUGCUGUUAUUtt-3′)和2(5′GCUCACAUCAUCUCAUCATT-3′)。类似地,使用特异性靶向人RARγ的预先验证的siRNA(5′-GGAAGUGUGCGAAAUGACtt-′)转染AREc32细胞。在这些情况下,siRNA(每孔200 pmol)和Lipofectamine 2000试剂(每孔10μl)在六孔板中用1 ml Optimum稀释,并在20°C下孵育20分钟。此后,4×105个细胞在4 ml不含抗生素的生长培养基中稀释,并直接分配到每个孔中。孵育24小时后,用10μM tBHQ、1μM视黄酸/ATRA或10μM tBHQ加1μM ATRA在新鲜DMEM中处理细胞24小时。 |
| 动物实验 |
本研究使用了纯合子Nrf2基因敲除小鼠。实验采用2月龄C57BL/6 Nrf2−/−和Nrf2+/+雄性小鼠。所有动物实验均在英国政府内政部许可和当地伦理委员会批准下进行。Nrf2−/−和Nrf2+/+小鼠(n = 2–3)分别饲喂维生素A缺乏症(VAD,特殊饮食服务)或对照饮食6周后处死。Nrf2+/+小鼠也饲喂VAD饮食6周;在最后两周,分别给予以下处理:不进行任何处理、每日腹腔注射10 mg/kg的维甲酸/全反式维甲酸(ATRA)或等体积的玉米油。处死小鼠后,取出小肠,清洗后置于液氮中冷冻。[6]
|
| 药代性质 (ADME/PK) |
吸收、分布和排泄
局部应用维A酸预计会停留在角质层,全身吸收极少。一项研究表明,局部应用放射性标记的维A酸28天后,经皮总吸收率为2%。该研究还考察了每日一次使用1.9克维A酸与过氧化苯甲酰的复方制剂,持续14天后的吸收情况。在第14天达到稳态时,维A酸的平均Cmax为0.15-0.19 ng/mL,其代谢产物4-酮-13-顺式维A酸的平均Cmax为0.27-0.34 ng/mL,13-顺式维A酸的平均Cmax为0.13-0.28 ng/mL。不同年龄组(儿童、青少年和成人)的Cmax值存在差异。相应的平均AUC0-24范围分别为0.63-2.06、2.39-2.89和0.96-1.99 ng·h/mL。口服给药后,维A酸的绝对生物利用度约为50%。虽然食物对维A酸的影响尚不明确,但食物会增加维甲酸类药物的口服吸收。当每日两次口服22.5 mg/m²的维A酸时,首次给药后平均±标准差Cmax为394±89 ng/mL,连续治疗一周后为138±139 ng/mL。首次给药后曲线下面积(AUC)为537±191 ng·h/mL,连续治疗一周后为249±185 ng·h/mL。达峰时间(Tmax)为1至2小时。维A酸代谢物经胆汁和尿液排泄。分别给予2.75 mg和50 mg放射性标记的维A酸(分别为基于1.7 m²体表面积的批准推荐剂量的0.53倍和9.6倍)后,约63%的放射性物质在72小时内从尿液中回收,31%在6天内从粪便中回收。口服维A酸后,其能迅速且广泛分布于组织,但不能穿过血脑屏障。静脉注射维A酸的表观分布容积(Vd)与剂量相关,低剂量时Vd显著增大。 0.0125 mg/kg剂量后,Vd为0.52 ± 0.12 L/kg;0.25 mg/kg剂量后,Vd为0.21 ± 0.05 L/kg。 暂无相关信息。 /乳汁/ 尚不清楚局部应用的维A酸是否会分泌到人乳中。 放射性标记药物的研究表明,口服2.75 mg和50 mg剂量的维A酸后,超过90%的放射性物质从尿液和粪便中回收。根据3名受试者的数据,约63%的放射性物质在72小时内从尿液中排出,31%在6天内从粪便中排出。 对急性早幼粒细胞白血病(APL)患者单次口服45 mg/m²(约80 mg)剂量后,平均峰值维A酸浓度为347 ± 266 ng/mL。达峰时间为1至2小时。 维A酸的表观分布容积尚未确定。维A酸在血浆中的结合率超过95%,主要与白蛋白结合。在 10 至 500 ng/mL 的浓度范围内,血浆蛋白结合率保持不变。 有关全反式维甲酸(共 12 种)的更多吸收、分布和排泄(完整)数据,请访问 HSDB 记录页面。 代谢/代谢物 维甲酸迅速代谢形成各种氧化和结合代谢物。它形成多种代谢产物,包括立体异构化衍生物(9-顺式-维甲酸或[阿利维甲酸]和13-顺式-维甲酸或[异维甲酸])、氧化衍生物(4-羟基维甲酸、4-氧代维甲酸、18-羟基维甲酸、5,6-环氧维甲酸、3,4-二脱氢维甲酸和视黄酸牛磺酸)、立体异构化和氧化衍生物(13-顺式-4-氧代-维甲酸)、葡萄糖醛酸化衍生物(视黄酰β-葡萄糖醛酸苷、13-顺式-视黄酰β-葡萄糖醛酸苷、4-氧代-视黄酰β-葡萄糖醛酸苷、5,6-环氧维甲酸β-葡萄糖醛酸苷和13-顺式-4-氧代-视黄酸)。维甲酸的代谢产物包括β-葡萄糖醛酸苷、维甲酸的非极性代谢物以及维甲酸酯。维甲酸由多种CYP酶代谢,包括CYP3A4、CYP2C8和CYP2E。它还可通过UGT2B7进行葡萄糖醛酸化。代谢产物4-氧代维甲酸和4-氧代反式维甲酸葡萄糖醛酸苷的药理活性约为母体化合物的三分之一。连续治疗一周后,当血浆浓度降至第一天浓度的三分之一时,维甲酸会诱导自身代谢。有证据表明,维甲酸会诱导自身代谢。在接受每日45 mg/m²维甲酸治疗的急性早幼粒细胞白血病(APL)患者中,连续治疗2-6周后,尿液中4-氧代反式维甲酸葡萄糖醛酸苷的排泄量增加了约十倍,提示维甲酸代谢增加可能是导致持续给药期间血浆药物浓度降低的主要机制。持续每日给药导致维甲酸清除率增加的可能机制包括CYP酶或氧化辅因子的诱导以及细胞维甲酸结合蛋白表达的增加。增加维甲酸剂量以补偿明显的自身诱导作用并未显示出能提高治疗反应。血浆维甲酸浓度降低与复发和临床耐药相关,一些研究者认为,维甲酸的临床治疗失败可能与长期治疗期间药物有效浓度的维持不足有关。 已在血浆和尿液中检测到维甲酸代谢物。细胞色素P450酶参与了维甲酸的氧化代谢。代谢产物包括13-顺式维甲酸、4-氧代反式维甲酸、4-氧代顺式维甲酸和4-氧代反式维甲酸葡萄糖醛酸苷。在急性早幼粒细胞白血病(APL)患者中,每日皮下注射45 mg/m²剂量的维甲酸,连续给药2至6周后,尿液中4-氧代反式维甲酸葡萄糖醛酸苷的排泄量较基线值增加了约十倍。 乙醇喂养的大鼠表现出微粒体维甲酸代谢增强(50%),同时微粒体细胞色素P450含量增加(34%)。长期摄入乙醇后,肝微粒体细胞色素 P450 依赖性维甲酸代谢增加,可能导致体内维甲酸分解代谢加速。 给大鼠腹腔注射高剂量 15-(14)C- 和 10,11-(3)H- 标记的维甲酸后,通过柱色谱、薄层色谱和高效液相色谱从粪便中分离出 3 种主要代谢物,含量为微克级。质谱分析鉴定出其为全反式-4-氧代维甲酸、全反式-5'-羟基维甲酸和7-反式-9-顺式-11-反式-13-反式-5'-羟基维甲酸。 有关全反式维甲酸(共8种代谢物)的更多代谢/代谢物(完整)数据,请访问HSDB记录页面。 维甲酸已知的代谢物包括5,6-环氧维甲酸、全反式维甲酸葡糖醛酸苷、18-羟基维甲酸和4-羟基维甲酸。 维甲酸是视黄醛的已知代谢物。 肝脏 半衰期:0.5-2小时 生物半衰期 首次给药后,维甲酸的末端消除半衰期为在急性早幼粒细胞白血病(APL)患者中,0.5 至 2 小时。 在接受口服维甲酸治疗的急性早幼粒细胞白血病(APL)患者中,据报道,首次给药后末端消除半衰期为 0.5-2 小时。 维生素 A 的代谢和全反式维甲酸的生成 [4] 维生素 A 是正常发育和视力所必需的膳食维生素。早在 1881 年,尼古拉·卢宁就暗示了维生素 A 的重要性,他发现,除非在饮食中添加牛奶,否则纯化的蛋白质、脂肪和碳水化合物无法维持小鼠的正常生长。 1917年,埃尔默·弗纳·麦科勒姆(Elmer Verner McCollum)确定,牛奶中的关键成分实际上是一种“脂溶性因子A”,与之前发现的“水溶性因子B”(即维生素B)形成对比。这些发现使得丹麦儿科医生卡尔·爱德华·布洛赫(Carl Edvard Bloch)能够确定维生素A缺乏是夜盲症(或干眼症)的病因。虽然维生素A是必需的膳食维生素,但它本身并非发挥其功能的主要生物活性介质。维生素A发挥功能的关键介质被确定为全反式维甲酸(atRA)和11-顺式视黄醛。atRA是基因转录的调节因子,而11-顺式视黄醛则作为视觉功能的生色团。在本节中,我们将回顾维生素A转化为各种类视黄醇的代谢过程,重点介绍atRA的生成(图1)。 |
| 毒性/毒理 (Toxicokinetics/TK) |
毒性概述
识别和用途:全反式维甲酸(维A酸)适用于局部治疗寻常痤疮。维A酸胶囊适用于诱导急性早幼粒细胞白血病患者缓解。人体研究:接受维A酸治疗的患者中,6%发生心力衰竭,3%发生心脏骤停、心肌梗死、中风和肺动脉高压。在维A酸治疗的第一个月内,存在发生累及任何器官系统的动脉或静脉血栓形成的风险。接受维A酸治疗的患者曾报告发生血栓栓塞事件,包括致命性肺栓塞。一名接受维A酸治疗的患者在同时接受抗纤溶药物治疗期间发生致命性血栓栓塞。据报道,在接受维甲酸治疗期间服用羟基脲的患者中,曾出现骨髓坏死,有时甚至致命。接受维甲酸治疗的患者中罕见血小板增多症的报道。约40%接受维甲酸治疗的患者会出现快速进展性白细胞增多症。维甲酸-急性早幼粒细胞白血病(RA-APL)综合征(也称为APL分化综合征)的特征是发热、呼吸困难、急性呼吸窘迫、体重增加、肺部浸润、胸腔和心包积液、水肿、肝功能衰竭、肾功能衰竭和多器官功能衰竭,约25%接受维甲酸治疗APL的患者会出现该综合征。RA-APL综合征有时伴有心肌收缩力减弱和阵发性低血压,可伴有或不伴有白细胞增多症。在严重病例中,可能出现进行性低氧血症,需要气管插管和机械通气,并有因进行性低氧血症和多器官衰竭导致的死亡报道。动物研究:当小鼠局部应用每日0.025 mg/kg剂量的维A酸时,未发现致癌性证据。当小鼠局部应用0.017%和0.035%的维A酸制剂时,部分雌性小鼠在治疗区域观察到皮肤鳞状细胞癌和乳头状瘤,雄性小鼠则观察到剂量相关的肝脏肿瘤。体外培养的大鼠胚胎实验表明,维A酸是一种直接作用的畸形发生剂。主要缺陷涉及鳃弓和体节。类维生素A诱导的人类和啮齿动物颌骨、耳部、面部、颅骨、眼部和心脏畸形是众所周知的。在妊娠第9或11天单次口服100 mg/kg维A酸,并在妊娠第17天处死的小鼠中,90%的胎儿出现骨骼缺陷(四肢)和腭裂。有证据表明,大鼠每日局部应用剂量超过1 mg/kg的维A酸具有致畸性(尾巴缩短或弯曲)。另有报道称,大鼠每日皮肤应用10 mg/kg维A酸也会出现骨骼异常。局部应用维A酸乳膏与兔腭裂和脑积水发生率增加相关。在接受局部维A酸治疗的兔中,部分胎儿出现圆顶头和脑积水,这是该物种中维甲酸类药物诱导胎儿畸形的典型表现。在小鼠中,剂量高于0.7 mg/kg/天时,会出现明显的外部、软组织和骨骼改变;在大鼠中,剂量高于2 mg/kg/天时,剂量高于7 mg/kg/天时,剂量高于7 mg/kg/天时,剂量高于10 mg/kg/天时,剂量高于10 mg/kg/天时,剂量高于10 mg/kg/天时,均会出现明显的外部、软组织和骨骼改变。皮下注射给兔子时,维A酸在2 mg/kg/天的剂量下具有致畸性,但在1 mg/kg/天的剂量下则不具有致畸性。体内和体外(Ames试验)试验均未证实维A酸具有致突变性。然而,该药物微球制剂中的成分已显示出潜在的遗传毒性和致畸性。生态毒性研究:在孵化后6-9天的日本比目鱼(Paralichthys olivaceus)中,维A酸在所有受检维A酸异构体中引起的骨骼畸形最为严重。 维A酸可与α、β和γ维A酸受体(RAR)结合。RAR-α和RAR-β分别与急性早幼粒细胞白血病和鳞状细胞癌的发生发展相关。RAR-γ与类维生素A对皮肤黏膜组织和骨骼的影响有关。尽管维A酸的确切作用机制尚不清楚,但现有证据表明,维A酸治疗痤疮的有效性主要归因于其能够改善异常的毛囊角化。粉刺形成于角化上皮细胞过多的毛囊中。维A酸促进角质细胞脱落,并加速毛囊角质细胞的脱落。通过增加毛囊上皮细胞的有丝分裂活性,维A酸还能提高薄而松散附着的角质细胞的更新率。通过这些作用,粉刺内容物被排出,并减少了微粉刺(寻常痤疮的前体病变)的形成。维A酸并非细胞溶解剂,而是在体外培养和体内诱导急性早幼粒细胞白血病(APL)细胞分化并抑制其增殖。当全身性给予APL患者维A酸治疗时,维A酸治疗首先促进源自白血病克隆的原始早幼粒细胞成熟,随后在达到完全缓解(CR)的患者中,正常的、多克隆的造血细胞重新填充骨髓和外周血。维甲酸在急性早幼粒细胞白血病(APL)中的确切作用机制尚不清楚。 相互作用 本研究采用小鼠乳腺器官培养技术,探讨了包括反式维甲酸在内的类维生素A对催乳素诱导的乳腺结构分化的影响。用类固醇预处理的BALB/c小鼠的胸腺在胰岛素和催乳素存在下,6天内即可分化为肺泡结构。反式维甲酸抑制催乳素诱导的腺体结构变化。 为了确定2,3,7,8-四氯二苯并二恶英和维甲酸是否会增强或拮抗另一种化合物的致畸作用,在妊娠第10或12天,对C57BL/6N雌鼠进行口服给药,每公斤体重给予10毫升玉米油,其中含有2,3,7,8-四氯二苯并二恶英(0-18微克/公斤)、维甲酸(0-200毫克/公斤)或两种化合物的组合。在妊娠第18天处死雌鼠,并评估其毒性和致畸性。2,3,7,8-四氯二苯并二恶英和维甲酸的联合给药对母体或胎儿的毒性没有超出单独使用任一化合物的预期。在妊娠第10天,较低剂量的维甲酸即可诱发腭裂,而在妊娠第12天,较低剂量的2,3,7,8-四氯二苯并二恶英即可诱发腭裂,而在妊娠第12天,较低剂量的2,3,7,8-四氯二苯并二恶英即可诱发腭裂。妊娠第10天和第12天,2,3,7,8-四氯二苯并二恶英诱发的肾积水的敏感性相似。仅在妊娠第10天给予维甲酸时观察到肢芽缺陷,而妊娠第12天给予时未观察到。其他软组织或骨骼畸形与2,3,7,8-四氯二苯并二恶英或维甲酸的给药无关。未观察到2,3,7,8-四氯二苯并二恶英对维甲酸诱导的肢芽缺陷的发生率或严重程度的影响,维甲酸也未影响2,3,7,8-四氯二苯并二恶英诱导的肾积水的发生率或严重程度。然而,异生素与维生素联合用药显著增加了腭裂的发生率。在妊娠第10天和第12天,腭裂诱导的剂量反应曲线平行,提示两种化合物的作用机制可能存在一些相似之处。然而,联合治疗产生了协同效应,这种效应随发育阶段而变化,且具有组织特异性。接受维甲酸治疗的患者发生假性脑瘤(颅内高压)的风险增加。同时使用其他已知可引起假性脑瘤或颅内高压的药物,例如四环素类药物,可能会增加接受维A酸治疗的患者发生这种情况的风险。 同时使用对S期细胞具有细胞毒性的羟基脲和诱导细胞进入S期的维A酸,可能会产生协同效应,导致大量细胞溶解。已有报道称,在接受维A酸治疗期间服用羟基脲的患者出现骨髓坏死,有时甚至致命。尽管一些临床医生已将羟基脲与维甲酸联合用于降低白细胞增多症,但这种做法的安全性和有效性尚未确定,因此建议在接受维甲酸治疗的患者中使用羟基脲时应谨慎。 有关全反式维甲酸(共14种)的更多相互作用(完整)数据,请访问HSDB记录页面。 非人类毒性值 大鼠口服LD50:1960 mg/kg 大鼠腹腔注射LD50:96 mg/kg 大鼠皮下注射LD50:53 mg/kg 大鼠静脉注射LD50:78 mg/kg 有关全反式维甲酸(共12种)的更多非人类毒性值(完整)数据,请访问HSDB记录页面。 |
| 参考文献 |
[1]. Retinoid X Receptor Agonists Upregulate Genes Responsible for the Biosynthesis of All-Trans-Retinoic Acid in Human Epidermis. PLoS One. 2016 Apr 14;11(4):e0153556.
[2]. Retinoic acid is a high affinity selective ligand for the peroxisome proliferator-activated receptor beta/delta. J Biol Chem. 2003 Oct 24;278(43):41589-92. [3]. Retinoic acid induces neurogenesis by activating both retinoic acid receptors (RARs) and peroxisomeproliferator-activated receptor β/δ (PPARβ/δ). J Biol Chem. 2012 Dec 7;287(50):42195-205. [4]. Retinoic acid synthesis and functions in early embryonic development. Cell Biosci. 2012 Mar 22;2(1):11. [5]. A retinoic acid receptor alpha antagonist selectively counteracts retinoic acid effects. Proc Natl Acad Sci U S A. 1992 Aug 1;89(15):7129-33. [6]. Identification of retinoic acid as an inhibitor of transcription factor Nrf2 through activation of retinoic acid receptor alpha. Proc Natl Acad Sci U S A. 2007 Dec 4;104(49):19589-94 |
| 其他信息 |
治疗用途
抗肿瘤药 角质溶解药 /临床试验/ ClinicalTrials.gov 是一个注册库和结果数据库,收录了全球范围内由公共和私人机构资助的人体临床研究。该网站由美国国家医学图书馆 (NLM) 和美国国立卫生研究院 (NIH) 维护。ClinicalTrials.gov 上的每条记录都包含研究方案的摘要信息,包括:疾病或病症;干预措施(例如,正在研究的医疗产品、行为或程序);研究的标题、描述和设计;参与要求(资格标准);研究开展地点;研究地点的联系方式;以及其他健康网站相关信息的链接,例如 NLM 的 MedlinePlus(用于提供患者健康信息)和 PubMed(用于提供医学领域学术文章的引文和摘要)。反式维甲酸已收录于数据库中。 维甲酸凝胶和乳膏适用于治疗寻常痤疮的局部外用。该产品长期用于治疗其他疾病的安全性和有效性尚未确定。/已包含在美国产品标签中;维甲酸,外用/ 维甲酸以0.05%或0.1%乳膏的形式外用,用于缓解光损伤相关的皮肤变化(例如,细纹、色素沉着斑驳、粗糙)。/未包含在美国产品标签中;维甲酸,外用/ 有关全反式维甲酸(共9种)的更多治疗用途(完整)数据,请访问HSDB记录页面。 药物警告 /黑框警告/ 经验丰富的医生和机构。急性早幼粒细胞白血病 (APL) 患者本身风险较高,服用维甲酸胶囊可能出现严重不良反应。因此,维甲酸胶囊仅应在经验丰富的急性白血病治疗医师的严格监督下,于具备足够实验室和支持服务的医疗机构内用于 APL 患者,以便监测药物耐受性,并保护和维持因药物毒性(包括呼吸功能损害)而受损的患者。使用维甲酸胶囊的前提是,医师必须认为患者的潜在获益大于以下已知的治疗不良反应。/维甲酸,全身用药/ /黑框警告/ 维甲酸-APL 综合征。约25%接受维A酸胶囊治疗的急性早幼粒细胞白血病(APL)患者会出现一种称为维A酸-APL(RA-APL)综合征的症状,其特征为发热、呼吸困难、急性呼吸窘迫、体重增加、肺部X线浸润、胸腔积液和心包积液、水肿以及肝、肾和多器官功能衰竭。该综合征有时伴有心肌收缩力减弱和阵发性低血压。可伴有或不伴有白细胞增多。部分病例因进行性低氧血症需要气管插管和机械通气,一些患者因多器官功能衰竭而死亡。该综合征通常发生在治疗的第一个月内,也有报道称在首次服用维A酸胶囊后即出现该综合征。该综合征的治疗方案尚未明确,但一旦怀疑类风湿关节炎相关急性早幼粒细胞白血病(RA-APL)综合征,立即给予大剂量糖皮质激素治疗似乎可以降低发病率和死亡率。一旦出现提示该综合征的早期症状(不明原因的发热、呼吸困难和/或体重增加、胸部听诊异常或影像学异常),无论白细胞计数如何,都应立即开始大剂量糖皮质激素治疗(地塞米松10 mg,静脉注射,每12小时一次,持续3天或直至症状缓解)。大多数患者在RA-APL综合征治疗期间无需停用维A酸胶囊。然而,对于中重度RA-APL综合征患者,应考虑暂时中断维A酸胶囊治疗。/维A酸,全身用药/ /黑框警告/ 维A酸胶囊治疗期间,约40%的患者会出现快速进展性白细胞增多症。诊断时白细胞计数高(>5×10⁹/L)的患者,其白细胞计数进一步快速升高的风险增加。快速进展的白细胞增多症与危及生命的并发症风险增加相关。如果出现类风湿关节炎合并急性早幼粒细胞白血病(RA-APL)综合征的体征和症状,并伴有白细胞增多症,应立即开始大剂量糖皮质激素治疗。一些研究者在患者初诊时白细胞计数>5×10⁹/L,或治疗开始时白细胞减少且白细胞计数快速升高的情况下,常规在维甲酸胶囊治疗的基础上加用化疗,并报告RA-APL综合征的发生率较低。对于白细胞计数 >5×10⁹/L 的患者,可考虑在第 1 或 2 天,在维甲酸胶囊治疗的基础上加用全剂量化疗(如无禁忌症,可加用蒽环类药物);对于白细胞计数 <5×10⁹/L 的患者,若白细胞计数在第 5 天达到 ≥ 6×10⁹/L,或在第 10 天达到 ≥ 10×10⁹/L,或在第 28 天达到 ≥ 15×10⁹/L,则可立即加用全剂量化疗。/维甲酸,全身用药/ /黑框警告/ 致畸作用。妊娠期用药分级为 D 级。妊娠期间服用维甲酸胶囊有很高的风险导致胎儿严重畸形。然而,如果确定维A酸胶囊是孕妇或育龄妇女的最佳治疗方案,则必须确保患者已充分了解并被告知如果怀孕可能对胎儿造成的风险以及避孕失败的风险,并已被告知在治疗期间和停药后1个月内需要同时使用两种可靠的避孕方法,且患者已确认理解使用双重避孕的必要性,除非选择禁欲。在开始服用维A酸胶囊治疗前1周内,应采集患者的血液或尿液样本进行血清或尿妊娠试验,灵敏度至少为50 mIU/mL。如果可能,应推迟维A酸胶囊治疗,直至获得阴性结果。如果无法推迟治疗,则应立即开始使用两种可靠的避孕方法。在整个维A酸胶囊治疗期间,应每月重复进行妊娠测试和避孕咨询。/维A酸,全身用药/ 有关全反式维A酸(共44条)的更多药物警告(完整)数据,请访问HSDB记录页面。 药效学 维A酸是一种维生素A衍生物,可促进细胞生成、增殖和分化。局部使用时,维A酸可调节表皮细胞更新和胶原蛋白生成。它还可以防止胶原蛋白流失,减轻炎症,并抑制基质金属蛋白酶(MMP)的诱导,MMP是一种破坏胶原蛋白和弹性纤维的酶。在短期和长期研究中,局部应用浓度为0.001%至0.1%的维A酸与光老化和细纹的临床症状改善、表皮增厚、角质层致密化和黑色素含量降低相关。它还能改善黑素细胞的分化和分布,促进表皮增生和血管生成。口服维甲酸具有抗肿瘤活性。研究表明,维甲酸能诱导肿瘤细胞分化。它能诱导细胞分化,并降低体外培养和体内急性早幼粒细胞白血病(APL)细胞的增殖。在APL患者中,维甲酸促进了源自白血病克隆的原始早幼粒细胞的初始成熟,随后在达到完全缓解的患者中,骨髓和外周血被正常的、多克隆的造血细胞重新填充。 |
| 分子式 |
C20H28O2
|
|---|---|
| 分子量 |
300.4
|
| 精确质量 |
300.208
|
| 元素分析 |
C, 79.96; H, 9.39; O, 10.65
|
| CAS号 |
302-79-4
|
| 相关CAS号 |
Retinoic acid-d5;78996-15-3;Retinoic acid;302-79-4;11-cis-Retinoic Acid-d5;Retinoic acid-d6;2483831-72-5
|
| PubChem CID |
444795
|
| 外观&性状 |
Yellow to light-orange crystalline powder
Crystals from ethanol |
| 密度 |
1.0±0.1 g/cm3
|
| 沸点 |
462.8±14.0 °C at 760 mmHg
|
| 熔点 |
179-184ºC
|
| 闪点 |
350.6±11.0 °C
|
| 蒸汽压 |
0.0±2.5 mmHg at 25°C
|
| 折射率 |
1.556
|
| LogP |
6.83
|
| tPSA |
37.3
|
| 氢键供体(HBD)数目 |
1
|
| 氢键受体(HBA)数目 |
2
|
| 可旋转键数目(RBC) |
5
|
| 重原子数目 |
22
|
| 分子复杂度/Complexity |
567
|
| 定义原子立体中心数目 |
0
|
| SMILES |
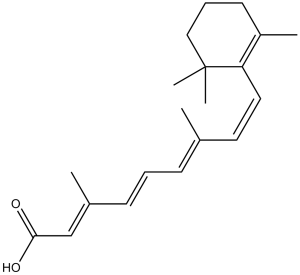
CC1(C)C(/C=C/C(C)=C/C=C/C(C)=C/C(O)=O)=C(C)CCC1
|
| InChi Key |
SHGAZHPCJJPHSC-YCNIQYBTSA-N
|
| InChi Code |
InChI=1S/C20H28O2/c1-15(8-6-9-16(2)14-19(21)22)11-12-18-17(3)10-7-13-20(18,4)5/h6,8-9,11-12,14H,7,10,13H2,1-5H3,(H,21,22)/b9-6+,12-11+,15-8+,16-14+
|
| 化学名 |
(2E,4E,6E,8E)-3,7-dimethyl-9-(2,6,6-trimethylcyclohexen-1-yl)nona-2,4,6,8-tetraenoic acid
|
| 别名 |
All-trans Retinoic Acid; Ro 5488; Ro-5488; tretinoin; ATRA; Renova; Aknefug; Atralin; Retin-A Micro; Tretinoina; ...; 302-79-4; Vitamin A acid; ATRA; TRA; Ro5488; alltrans vitamin A acid; betaretinoic acid; retinoic acid; TRA; trans retinoic acid; trans vitamin A acid; tretinoinum; Trade names: Avita; Renova; Aberel; Aknoten; RetinA; RetinA MICRO; Vesanoid. Foreign brand names: Airol; Eudyna; RetisolA; StievaA; Cordes Vas; Dermairol; EpiAberel; StievaA Forte; Vitinoin
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month 注意: 请将本产品存放在密封且受保护的环境中(例如氮气保护),避免吸湿/受潮和光照。 |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
|
|||
|---|---|---|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: 2.5 mg/mL (8.32 mM) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (这些助溶剂从左到右依次添加,逐一添加), 悬浮液; 超声和加热处理
例如,若需制备1 mL的工作液,可将100 μL 25.0 mg/mL澄清DMSO储备液加入到400 μL PEG300中,混匀;然后向上述溶液中加入50 μL Tween-80,混匀;加入450 μL生理盐水定容至1 mL。 *生理盐水的制备:将 0.9 g 氯化钠溶解在 100 mL ddH₂O中,得到澄清溶液。 配方 2 中的溶解度: ≥ 2.5 mg/mL (8.32 mM) (饱和度未知) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (这些助溶剂从左到右依次添加,逐一添加), 悬浮液。 例如,若需制备1 mL的工作液,可将 100 μL 25.0 mg/mL澄清DMSO储备液加入900 μL 20% SBE-β-CD生理盐水溶液中,混匀。 *20% SBE-β-CD 生理盐水溶液的制备(4°C,1 周):将 2 g SBE-β-CD 溶解于 10 mL 生理盐水中,得到澄清溶液。 View More
配方 3 中的溶解度: ≥ 2.5 mg/mL (8.32 mM) (饱和度未知) in 10% DMSO + 90% Corn Oil (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 配方 4 中的溶解度: 2.5 mg/mL (8.32 mM) in 5% DMSO + 40% PEG300 + 5% Tween80 + 50% Saline (这些助溶剂从左到右依次添加,逐一添加), 悬浊液; 超声助溶。 *生理盐水的制备:将 0.9 g 氯化钠溶解在 100 mL ddH₂O中,得到澄清溶液。 配方 5 中的溶解度: 2.5 mg/mL (8.32 mM) in 5% DMSO + 95% (20% SBE-β-CD in Saline) (这些助溶剂从左到右依次添加,逐一添加), 悬浊液; 超声助溶。 *生理盐水的制备:将 0.9 g 氯化钠溶解在 100 mL ddH₂O中,得到澄清溶液。 配方 6 中的溶解度: 5 mg/mL (16.64 mM) in 50% PEG300 50% PBS (这些助溶剂从左到右依次添加,逐一添加), 悬浮液; 需要超声助溶并加热至 40°C。 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 3.3289 mL | 16.6445 mL | 33.2889 mL | |
| 5 mM | 0.6658 mL | 3.3289 mL | 6.6578 mL | |
| 10 mM | 0.3329 mL | 1.6644 mL | 3.3289 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT06358677 | Not yet recruiting NEW | Drug: Larotrectinib Sulfate Procedure: Bone Scan |
Metastatic Colon Cancer Metastatic Rectum Cancer |
NCT06358677 | July 2024 | Phase 2 |
| NCT04724473 | Completed | Drug: Tretinoin Cream 0.025% | Acne Vulgaris | Taro Pharmaceuticals USA | December 10, 2019 | Early Phase 1 |
| NCT03200847 | Active, not recruiting Has Results | Drug: Pembrolizumab with All-Trans Retinoic Acid |
Stage IV Melanoma Stage III Melanoma |
University of Colorado, Denver | October 31, 2017 | Phase 1 Phase 2 |
| NCT06213987 | Recruiting | Drug: 0.025% Tretinoin | Acanthosis Nigricans Hyperpigmentation |
Srinakharinwirot University | February 1, 2024 | Phase 3 |