| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 10 mM * 1 mL in DMSO |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| 1g |
|
||
| 2g |
|
||
| Other Sizes |
|
| 靶点 |
- Carnitine palmitoyltransferase I (CPT I)
- Mildronate (Meldonium) inhibits CPT I, the rate-limiting enzyme of fatty acid β-oxidation, with an IC50 of 3.8 mM for rat liver CPT I and 2.1 mM for human recombinant CPT I [1]
- Platelet-type phosphofructokinase (PFK-P) - Mildronate modulates PFK-P activity (a key enzyme in glycolysis) by increasing its phosphorylation (activation) at Ser32, with no direct inhibitory/activatory IC50/Ki reported [3] |
|---|---|
| 体外研究 (In Vitro) |
通过靶向 PFKP 来调节糖酵解,从而促进 Nrf2 从细胞质转移到细胞核,medium(20–40 μM;24 小时)可减少肺损伤,并减轻缺氧环境下的氧化应激和线粒体损伤 [3]。
- 心肌细胞代谢调节: 1. 脂肪酸氧化(FAO)抑制:新生大鼠心室肌细胞(NRVMs)经米屈肼(1–10 mM)处理24小时后,FAO速率降低30–50%(通过[14C]-棕榈酸氧化实验检测);同时葡萄糖氧化(通过[14C]-葡萄糖检测)增加40–60%,能量代谢向葡萄糖利用偏移 [1] 2. 线粒体功能保护:米屈肼(5 mM)可减轻H2O2(100 μM)诱导的NRVMs线粒体膜电位(ΔΨm)丢失,使细胞色素c释放减少45% [1] - 神经细胞保护作用: 1. 活性氧(ROS)清除:原代大鼠皮质神经元经氧糖剥夺(OGD,2小时)处理前,用米屈肼(0.1–5 mM)预处理,ROS水平降低25–60%(DCFH-DA染色检测);2 mM浓度时,脂质过氧化产物丙二醛(MDA)减少35% [2] 2. 抗凋亡作用:米屈肼(1–5 mM)使OGD处理的神经元中Bcl-2/Bax比值升高2–3倍,caspase-3激活水平降低40–50%(western blot检测) [2] - 缺氧肺损伤保护(肺上皮细胞): 1. 糖酵解调节:A549人肺腺癌细胞(模拟肺泡上皮细胞)在缺氧环境(1% O2,24小时)下,经米屈肼(0.5–2 mM)处理后,PFK-P磷酸化水平(p-PFK-P)升高1.5–2.0倍,糖酵解标志物乳酸生成增加30–40% [3] 2. 炎症抑制:米屈肼(1 mM)使缺氧诱导的肿瘤坏死因子-α(TNF-α)和白细胞介素-6(IL-6)分泌分别减少35%和40%(ELISA实验) [3] |
| 体内研究 (In Vivo) |
在小鼠中,米曲肼(50、100 或 200 mg/kg;每天一次,持续三天)可适度减轻缺氧引起的肺损伤 [3]。
- 大鼠心肌缺血再灌注(I/R)保护模型: 1. 梗死面积减少:雄性Wistar大鼠在心肌I/R(缺血30分钟,再灌注24小时)前,每日腹腔注射米屈肼(100 mg/kg),连续7天。与溶剂对照组相比,梗死面积(TTC染色)减少35%,左心室射血分数(LVEF,超声心动图检测)增加15% [1] 2. 能量代谢物调节:米屈肼(100 mg/kg,腹腔注射)使I/R大鼠心肌ATP水平增加25%,长链酰基肉碱蓄积减少40% [1] - 小鼠脑缺血保护模型: 1. 脑梗死体积减少:C57BL/6小鼠在大脑中动脉阻塞(MCAO,缺血60分钟,再灌注24小时)前1小时,口服米屈肼(200 mg/kg)。与对照组相比,脑梗死体积(TTC染色)减少30%,神经功能缺损评分(0–5分制)从3.5降至2.0 [2] 2. 氧化应激减轻:米屈肼(200 mg/kg,口服)使MCAO小鼠脑内MDA水平减少40%,超氧化物歧化酶(SOD)活性增加30% [2] - 大鼠缺氧肺损伤改善模型: 1. 肺功能保护:雄性Sprague-Dawley大鼠暴露于慢性缺氧环境(10% O2,21天),期间每日腹腔注射米屈肼(50 mg/kg)。与缺氧对照组相比,肺湿/干重量比(水肿标志物)减少25%,动脉血氧分压(PaO2)增加30% [3] 2. 糖酵解激活:米屈肼(50 mg/kg,腹腔注射)使缺氧大鼠肺组织p-PFK-P水平增加1.8倍,乳酸含量增加35% [3] |
| 酶活实验 |
- 大鼠肝脏CPT I活性测定 [1]:
1. 酶制备:通过差速离心(600×g离心10分钟,12,000×g离心20分钟)分离大鼠肝脏线粒体,重悬于实验缓冲液(250 mM蔗糖、10 mM Tris-HCl,pH 7.4、1 mM EDTA)中。 2. 反应体系:1 mL反应混合物包含线粒体(0.5 mg蛋白)、50 μM棕榈酰辅酶A(底物)、200 μM L-肉碱、0.2 mM NAD+、10 mM MgCl2及米屈肼(0.1–10 mM,溶剂为水)。 3. 活性检测:通过分光光度法在340 nm处监测5分钟内NADH的生成(CPT I活性指标),通过活性与米屈肼浓度的非线性回归计算IC50。 - A549细胞PFK-P磷酸化测定 [3]: 1. 蛋白提取:缺氧条件下经米屈肼(0–2 mM)处理的A549细胞,用含磷酸酶抑制剂的RIPA缓冲液裂解。 2. Western blot检测:将等量蛋白(30 μg)通过SDS-PAGE分离,转移至PVDF膜,用抗p-PFK-P(Ser32)抗体和抗总PFK-P抗体孵育,ImageJ定量条带强度,计算p-PFK-P/总PFK-P比值以评估PFK-P激活程度。 |
| 细胞实验 |
RT-PCR[3]
细胞类型:缺氧培养箱中的大鼠肺泡 II 型上皮 RLE-6TN 细胞 测试浓度: 20 或 40 μM 孵育时间:24小时 实验结果:与缺氧组相比,PFKP、PDK1和PKM2的mRNA表达显着降低。 蛋白质印迹分析[3] 细胞类型:缺氧培养箱中的大鼠肺泡 II 型上皮 RLE-6TN 细胞 测试浓度: 20 或 40 μM 孵育时间: 24 小时 实验结果: 显着降低 PFKP、PKM2 和 LDHA 的蛋白表达。 - NRVM细胞FAO/葡萄糖氧化实验 [1]: 1. 细胞培养:从1–3日龄Wistar大鼠分离NRVMs,在含10% FBS的DMEM中培养48小时。 2. 药物处理:细胞经米屈肼(1–10 mM)处理24小时后,加入[14C]-棕榈酸(0.5 μCi/mL)或[14C]-葡萄糖(0.5 μCi/mL)孵育2小时。 3. 氧化速率检测:释放的14CO2用NaOH溶液捕获,闪烁计数器计数放射性,FAO/葡萄糖氧化速率按蛋白含量标准化。 - 原代皮质神经元OGD模型实验 [2]: 1. 神经元分离:从E18 Sprague-Dawley大鼠胚胎分离皮质神经元,在含B27添加剂的Neurobasal培养基中培养7天。 2. OGD与药物处理:神经元暴露于OGD环境(无糖DMEM,1% O2)2小时,米屈肼(0.1–5 mM)在OGD前1小时加入;OGD后,细胞在正常培养基中复氧24小时。 3. ROS与凋亡检测:ROS通过DCFH-DA染色(荧光显微镜,488 nm激发)检测;凋亡通过caspase-3活性实验(比色法,405 nm)和Bcl-2/Bax western blot评估。 - A549细胞缺氧模型实验 [3]: 1. 细胞培养:A549细胞在含10% FBS的RPMI 1640培养基中培养至80%融合。 2. 缺氧与药物处理:细胞置于缺氧培养箱(1% O2,5% CO2)中24小时,米屈肼(0.5–2 mM)在缺氧开始时加入。 3. 糖酵解与炎症检测:乳酸生成通过乳酸检测试剂盒(比色法,570 nm)测定;上清中TNF-α/IL-6水平通过ELISA(450 nm)定量。 |
| 动物实验 |
大鼠心肌缺血/再灌注模型[1]:
1. 动物准备:雄性Wistar大鼠(250-300 g)用戊巴比妥钠(50 mg/kg,腹腔注射)麻醉,并进行左侧开胸手术暴露心脏。 2. 给药:将米屈肼溶于生理盐水中,配制成10 mg/mL的浓度。大鼠在缺血/再灌注前7天,每天腹腔注射100 mg/kg(10 mL/kg)的米屈肼。 3. 缺血/再灌注诱导:用6-0丝线结扎左前降支冠状动脉(LAD)30分钟(缺血),然后松开缝线24小时(再灌注)。 4. 终点测量:再灌注24小时后,处死大鼠;取出心脏进行TTC染色(梗死面积)和ATP/酰基肉碱分析。 - 小鼠MCAO模型[2]: 1. 动物准备:雄性C57BL/6小鼠(20-25 g)用异氟烷(1.5-2%异氟烷/氧气)麻醉。 2. 给药:将米屈肼溶于蒸馏水,配制成20 mg/mL的溶液。小鼠在MCAO前1小时经口灌胃给予200 mg/kg(10 mL/kg)的米屈肼。 3. MCAO诱导:将一根尼龙单丝(直径0.18 mm)插入右侧颈内动脉,阻塞大脑中动脉60分钟,然后拔出进行再灌注。 4. 终点测量:再灌注24小时后,处死小鼠;取出脑组织进行TTC染色(梗死体积)和MDA/SOD分析。 - 大鼠缺氧性肺损伤模型[3]: 1. 动物准备:雄性Sprague-Dawley大鼠(200-220 g)饲养于缺氧舱(10% O2,平衡N2)中21天。 2. 给药:将米屈肼溶于生理盐水中,配制成5 mg/mL的溶液。在21天的缺氧期间,大鼠每天腹腔注射一次,剂量为50 mg/kg(10 mL/kg)。 3. 终点测量:21天后,处死大鼠;取出肺组织,用于计算湿重/干重比、p-PFK-P蛋白质印迹和乳酸测定;采集动脉血用于PaO2测定。 |
| 药代性质 (ADME/PK) |
口服吸收:健康志愿者口服米膦酸钠(500 mg)后,血浆峰浓度(Cmax)在 1-2 小时(Tmax)达到 85-95 μg/mL。口服生物利用度为 80-90% [1]
- 分布:米膦酸钠广泛分布于高能量需求组织,包括心肌(组织/血浆浓度比:1.8)、脑(1.2)和骨骼肌(2.0)。在正常情况下,它不会大量穿过血脑屏障,但在缺血性脑组织中会蓄积 [1,2] - 代谢和排泄:米膦酸钠代谢极少(≤10% 在肝脏转化为无活性代谢物)。大约 70-80% 的给药剂量在 24 小时内以原形经尿液排出。在人体中,消除半衰期(t1/2)为 4-6 小时,在大鼠中为 3-5 小时 [1] |
| 毒性/毒理 (Toxicokinetics/TK) |
急性毒性:
1. 在大鼠中,米膦酸钠的口服LD50 > 5000 mg/kg;腹腔注射LD50 > 3000 mg/kg。剂量高达2000 mg/kg时,未观察到死亡或明显的毒性(例如,嗜睡、腹泻)[1] 2. 在小鼠中,米膦酸钠的口服LD50 > 4000 mg/kg [2] - 亚慢性毒性: 1. 大鼠连续90天口服米膦酸钠(100–500 mg/kg/天),体重、食物摄入量或血液学参数(红细胞、白细胞、血红蛋白)均未出现显著变化。血清ALT、AST、肌酐和BUN水平(肝肾功能指标)均在正常范围内[1] 2. 治疗组大鼠的肝脏、肾脏、心脏或脑组织均未观察到组织病理学损伤[1] - 体外毒性:米膦酸钠(浓度高达20 mM)对NRVMs、原代皮层神经元或A549细胞均无细胞毒性(MTT法,细胞活力>90% vs. 对照组)[1,2,3] - 血浆蛋白结合率:米膦酸钠在人和大鼠中的血浆蛋白结合率较低(≤5%)[1] 123868 大鼠口服LD50 >20 gm/kg Eksperimental'naya i Klinicheskaya Farmakoterapiya., 19(67), 1991 123868 大鼠 LD50 腹腔注射 12 克/千克 行为:嗜睡(总体活动抑制);肺、胸部或呼吸:呼吸刺激 Eksperimental'naya i Klinicheskaya Farmakoterapiya., 19(67), 1991 123868 小鼠口服 LD50 18500 mg/kg Eksperimental'naya i Klinicheskaya Farmakoterapiya., 19(67), 1991 123868 小鼠腹腔 LD50 7850 mg/kg 英国专利申请,#2105992 123868 小鼠静脉注射 LD50 4430 mg/kg 英国专利申请,#2105992 |
| 参考文献 |
|
| 其他信息 |
作用机制:米膦酸钠通过两条关键途径调节能量代谢:(1) 抑制 CPT I 以减少过量的脂肪酸氧化(FAO,FAO 会导致缺血组织中的线粒体应激),并转向葡萄糖氧化(在缺氧条件下效率更高);(2) 激活磷酸果糖激酶磷酸化酶 (PFK-P) 以增强糖酵解,为缺氧细胞快速提供 ATP [1,3]
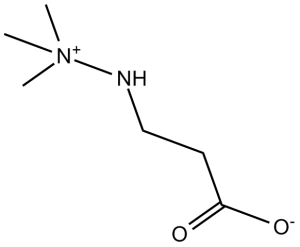
- 治疗适应症:米膦酸钠已在多个国家(例如俄罗斯、拉脱维亚)获批用于治疗心肌缺血(稳定性心绞痛)、心力衰竭和脑循环障碍(例如卒中后恢复)。目前也在研究其在阿尔茨海默病和帕金森病中的神经保护作用 [1,2] - 监管说明:美国食品药品监督管理局 (FDA) 尚未批准米膦酸钠在美国使用。由于其潜在的增强运动表现的作用(提高运动员的氧气利用率),米屈肼于2016年被世界反兴奋剂机构(WADA)列入禁用清单,但在进一步的安全评估后,于2021年被移除[1]。 米屈肼是一种β-丙氨酸铵,其结构为β-丙氨酸盐,其中一个氨基氢被三甲基氨基取代。它是一种临床常用的心脏保护药物,用于治疗心力衰竭、心肌梗死、心律失常、动脉粥样硬化和糖尿病。它具有心脏保护、神经保护和抑制EC 1.14.11.1(γ-丁酰甜菜碱双加氧酶)的作用。 |
| 分子式 |
C6H14N2O2
|
|
|---|---|---|
| 分子量 |
147.19
|
|
| 精确质量 |
146.105
|
|
| 元素分析 |
C, 39.55; H, 9.96; N, 15.37; O, 35.12
|
|
| CAS号 |
76144-81-5
|
|
| 相关CAS号 |
Meldonium dihydrate;86426-17-7; 839675-65-9 (fumarate); 76144-81-5 (free); 839675-63-7 (phoshate); 1608503-17-8 (hydrate);
|
|
| PubChem CID |
123868
|
|
| 外观&性状 |
White to off-white solid powder
|
|
| 熔点 |
85-90ºC
|
|
| 折射率 |
1.598
|
|
| LogP |
-2.1
|
|
| tPSA |
52.16
|
|
| 氢键供体(HBD)数目 |
1
|
|
| 氢键受体(HBA)数目 |
3
|
|
| 可旋转键数目(RBC) |
3
|
|
| 重原子数目 |
10
|
|
| 分子复杂度/Complexity |
112
|
|
| 定义原子立体中心数目 |
0
|
|
| SMILES |
C[N+](C)(C)NCCC(=O)[O-]
|
|
| InChi Key |
PVBQYTCFVWZSJK-UHFFFAOYSA-N
|
|
| InChi Code |
InChI=1S/C6H14N2O2/c1-8(2,3)7-5-4-6(9)10/h7H,4-5H2,1-3H3
|
|
| 化学名 |
3-[(trimethylazaniumyl)amino]propanoate
|
|
| 别名 |
|
|
| HS Tariff Code |
2934.99.9001
|
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
|
|||
|---|---|---|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: 100 mg/mL (684.04 mM) in PBS (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液; 超声助溶。
请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 6.7939 mL | 33.9697 mL | 67.9394 mL | |
| 5 mM | 1.3588 mL | 6.7939 mL | 13.5879 mL | |
| 10 mM | 0.6794 mL | 3.3970 mL | 6.7939 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT01831011 | Completed | Drug: mildronate injection Drug: cinepazide maleate injection |
Acute Ischemic Stroke | Xijing Hospital | July 2008 | Phase 2 |
| NCT05689827 | Completed | Drug: Ethyl methyl hydroxypyridine succinate + Meldonium |
Asthenia COVID-19 |
Promomed, LLC | April 5, 2022 | Phase 4 |
| NCT05939622 | Completed | Drug: Ethyl methyl hydroxypyridine succinate + Meldonium |
Asthenia COVID-19 |
Promomed, LLC | May 18, 2022 | Phase 4 |