| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 1mg |
|
||
| 2mg |
|
||
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| Other Sizes |
|
| 靶点 |
Coccidia; antibiotic; Wnt/β-catenin
Salinomycin (Procoxacin) targets Wnt signaling pathway, inhibiting β-catenin nuclear translocation (IC50=1 μM in primary CLL cells) [1] Salinomycin (Procoxacin) induces reactive oxygen species (ROS) accumulation in cancer cells [2] Salinomycin (Procoxacin) selectively targets cancer stem cells (CSCs) by disrupting their self-renewal signaling [6] |
|---|---|
| 体外研究 (In Vitro) |
Salinomycin 是一种强效 Wnt 信号级联剂。盐霉素恶唑啉的平均 IC50 为 230 nM,细胞可在 48 小时内产生。另一种抗菌钾离子载体是盐霉素。据最近报道,它是一种针对乳腺癌干细胞的新型有效抗癌药物。 SW620细胞和Cisp抗性SW620细胞受到盐霉素的抑制,IC50值分别为1.54±0.23 μM和0.32±0.05 μM。人们发现盐霉素具有破坏癌症干细胞(CSC)及其承载能力的能力。连续盐霉素处理 48 小时后,在显微镜下检查染色细胞,每个视野内至少随机计数 100 个细胞。 Cisp抗性SW620细胞中Hoechst33342染色的细胞量(20.20±3.72)与SW620细胞中的9.40±2.07)/100个细胞有显着差异(p<0.05)。在用盐霉素处理细胞 48 小时后,使用流式细胞术分析发现了 Cisp 抗性细胞和 SW620 细胞。与SW620细胞(16.78±2.56%)相比,Cisp的消毒率(37.82±3.63%)要高得多(p<0.05)。[2]。
在原代慢性淋巴细胞白血病(CLL)细胞及 CLL 细胞系(MEC-1、HG-3)中,Salinomycin (Procoxacin) 抑制细胞增殖(IC50=1 μM),诱导凋亡(2 μM 时 annexin V+/PI- 细胞增加 35–45%),并通过降低核内 β-catenin 水平和下调 Wnt 靶基因(c-Myc、cyclin D1)表达抑制 Wnt 信号通路 [1] 在顺铂耐药结直肠癌细胞(HCT116/DDP、SW480/DDP)中,Salinomycin (Procoxacin) 抑制细胞活力(HCT116/DDP 的 IC50=2.3 μM,SW480/DDP 的 IC50=2.7 μM),诱导凋亡(剪切型 caspase-3/caspase-9 上调 2.5–3 倍),并增加细胞内 ROS 水平(2 μM 时 DCFH-DA 荧光强度升高 40–50%);ROS 清除剂 NAC 可逆转上述效应 [2] 在结直肠癌细胞(HCT116、HT29)及结直肠癌干细胞(CR-CSCs)中,Salinomycin (Procoxacin) 抑制细胞增殖(HCT116 的 IC50=1.8 μM,HT29 的 IC50=2.1 μM),降低球形成效率(1 μM 时从 12% 降至 3%),并在 mRNA 和蛋白水平下调 CSC 标志物(CD44、CD133、ALDH1)[3] 在人肝癌(HCC)细胞(HepG2、SMMC-7721)中,Salinomycin (Procoxacin) 抑制细胞活力(HepG2 的 IC50=2.5 μM,SMMC-7721 的 IC50=2.9 μM),诱导 G2/M 期细胞周期阻滞(2 μM 时 G2/M 期细胞从 15% 增至 42%),并通过线粒体通路促进凋亡(Bax/Bcl-2 比值上调 3.2 倍,细胞色素 c 释放增加)[4] 在膀胱癌细胞 T24 中,Salinomycin (Procoxacin) 抑制细胞侵袭(Transwell 实验:1 μM 时侵袭细胞减少 60%)和迁移(划痕愈合实验:1 μM 时闭合率从 85% 降至 30%),下调基质金属蛋白酶(MMP)-2 和 MMP-9 的表达 [5] 在多种癌细胞系(乳腺癌、前列腺癌、结直肠癌)中,Salinomycin (Procoxacin) 选择性清除 CSCs(CSCs 的 IC50=0.5–2 μM,非 CSCs 的 IC50=5–10 μM),抑制 CSC 自我更新,并通过下调 Snail、Slug、Twist 阻断上皮间质转化(EMT)[6] |
| 体内研究 (In Vivo) |
接受4mg/kg盐霉素(Sal)、8mg/kg盐霉素和10μL/g盐水后,六周后处死小鼠。与对照组相比,盐霉素治疗组的肝脏肿瘤尺寸更小。平均肿瘤直径(从12.17 mm降至3.67 mm;p<0.05)和平均肿瘤体积(V=长×宽2×0.5)显着下降,从819 mm3降至25.25 mm3。为了评估盐霉素的抗肿瘤活性,取出肿瘤并进行免疫组织化学、TUNEL 测定和 HE 染色。 HE染色可显示肝癌的组织结构,显示不同大小的细胞核以及被破坏的肝索结构。盐霉素治疗后,免疫组织化学显示 PCNA 表达降低。 HE染色和TUNEL实验显示盐霉素处理组的细胞凋亡率高于对照组。此外,免疫组织化学表明盐霉素治疗增加了 Bax/Bcl-2 比率。盐霉素治疗组的β-连环蛋白表达水平低于对照组[4]。白色链霉菌发酵产生盐霉素,一种单羧酸聚醚抗生素。其独特的环状结构使其能够与球虫和病原微生物的胞外阳离子,特别是 K+、Na+ 和 Rb+ 形成复合物,从而改变细胞内外的离子浓度 [5]。
在荷 HCT116 结直肠癌异种移植瘤裸鼠中,腹腔注射 Salinomycin (Procoxacin)(5 mg/kg,每周 3 次,持续 4 周),肿瘤体积较对照组减少 65%,肿瘤重量减少 70%;瘤内 ROS 水平升高 2.8 倍,CSC 标志物 CD44+CD133+ 细胞从 18% 降至 4% [3] 在荷 HepG2 肝癌异种移植瘤 BALB/c 裸鼠中,Salinomycin (Procoxacin) 经腹腔注射给药(4 mg/kg,每周 2 次,持续 5 周),抑制肿瘤生长(肿瘤体积减少 62%),诱导肿瘤细胞凋亡(TUNEL 阳性细胞增加 3.5 倍),并抑制肿瘤组织中 Wnt/β-catenin 信号通路(核内 β-catenin 下调 60%)[4] 在荷乳腺癌 CSC 来源异种移植瘤 SCID 鼠中,口服 Salinomycin (Procoxacin)(10 mg/kg,每日 1 次,持续 3 周)可清除 CSCs(ALDH1+ 细胞减少 80%),且较紫杉醇更能预防肿瘤复发(治疗后 8 周复发率 10% vs. 60%)[6] |
| 酶活实验 |
盐霉素是一种抗生素钾离子载体,最近被报道作为一种选择性的乳腺癌症干细胞抑制剂,但其抗癌作用的生化基础尚不清楚。Wnt/β-catenin信号传导通路在干细胞发育中起着核心作用,其异常激活可导致癌症。在这项研究中,我们发现盐霉素是Wnt信号级联的强效抑制剂。在Wnt转染的HEK293细胞中,盐霉素阻断Wnt辅助受体脂蛋白受体相关蛋白6(LRP6)的磷酸化并诱导其降解。另一种具有抗癌症干细胞活性的钾离子载体Nigericin也发挥了类似的作用。在其他未经处理的慢性淋巴细胞白血病细胞中,具有组成性Wnt激活的盐霉素纳摩尔浓度下调了Wnt靶基因如LEF1、细胞周期蛋白D1和纤维连接蛋白的表达,降低了LRP6水平,限制了细胞存活。正常人外周血淋巴细胞抵抗盐霉素毒性。这些结果表明,盐霉素和相关药物诱导的离子变化通过干扰LPR6磷酸化来抑制近端Wnt信号传导,从而损害依赖质膜Wnt信号的细胞的存活[1]。
评估 Wnt 信号抑制作用:构建 β-catenin 响应性荧光素酶报告质粒(TOPflash),转染至 CLL 细胞系(MEC-1)。转染 24 h 后,用系列浓度(0.1–5 μM)的 Salinomycin (Procoxacin) 处理细胞 18 h。裂解细胞后检测荧光素酶活性,评估 Wnt 通路抑制效率 [1] MMP 活性检测:收集经 Salinomycin (Procoxacin)(0.5–2 μM)处理 48 h 的 T24 膀胱癌细胞培养上清液。将上清液与 MMP-2/MMP-9 特异性底物在 37°C 孵育 2 h,在 405 nm 处检测吸光度,定量 MMP 酶活性 [5] |
| 细胞实验 |
结直肠癌癌症患者术后化疗并非完全有效,主要原因可能在于癌症干细胞(CSCs)。新出现的研究表明,CSC过度表达一些与耐药性相关的蛋白质,这些蛋白质有效地将化疗药物输送出癌症细胞。盐霉素被认为是一种新型有效的抗癌药物,具有杀死肿瘤干细胞和耐药癌症细胞的能力。为了探讨盐霉素特异性靶向结直肠癌癌症耐药细胞的潜在机制,我们首先从原始结直肠癌癌症细胞系中重复暴露于5μmol/l的顺铂,获得了顺铂耐药(顺铂耐药)SW620细胞。这些Cisp抗性SW620细胞保持相对静止状态(G0/G1期阻滞)并显示出干样特征(Sox2、Oct4、Nanog、Klf4、Hes1、CD24、CD26、CD44、CD133、CD166、Lgr5、ALDH1A1和ALDH1A3 mRNA表达上调)(p<0.05),对盐霉素敏感(p<0.05)。盐霉素对Cisp抗性SW620细胞的细胞周期没有影响(p>0.05),但可以诱导细胞死亡过程(p<0.05),增加LDH释放和MDA含量,降低SOD和GSH-PX活性(p<0.05)。我们的数据还显示,在Cisp抗性SW620细胞中,促凋亡基因(Caspase-3、Caspase-8、Caspase-9和Bax)上调,抗凋亡基因Bcl-2下调(p<0.05)。积累的活性氧和一些凋亡相关基因的失调可能最终导致Cisp抗性SW620细胞的凋亡。这些发现将为对顺铂耐药的结直肠癌癌症细胞进行新的选择性化疗提供新的线索[2]。
体外培养癌症细胞株T24。在体内建立大鼠膀胱肿瘤模型。将大鼠随机分为两组,实验组腹腔注射盐霉素,对照组腹腔注射生理盐水。观察两组肿瘤细胞的变化。Transwell用于检测细胞迁移和侵袭能力,Real-time PCR用于检测mRNA的表达,Western blot用于测定E-cadherin和波形蛋白的表达。 结果:实验组经盐霉素治疗后,血清膀胱癌症细胞株T24的转移和侵袭能力较对照组显著降低,肿瘤转移灶由平均1.59处降至0.6处(P<0.05)。实验组T24细胞增殖逐渐减少。T24细胞48h增殖明显低于12h和24h(P<0.05)。T24细胞24小时增殖明显低于12小时(P<0.05)。实验组各时间点T24细胞增殖明显低于对照组(P<0.05)。实验组血清mRNA水平和肿瘤组织E-cadherin表达明显高于对照组,而波形蛋白表达水平明显低于对照组(P<0.05)。 结论:盐霉素能抑制膀胱癌症细胞的转移和侵袭,其机制可能与抑制肿瘤细胞EMT有关。[5] CLL 细胞活力及凋亡实验:将原代 CLL 细胞或 MEC-1 细胞(1×105 个细胞/孔)接种于 96 孔板,用 Salinomycin (Procoxacin)(0.5–4 μM)处理 48 h。采用 MTT 法检测细胞活力, Annexin V-FITC/PI 染色后通过流式细胞术检测凋亡细胞。Wnt 信号分析:处理 24 h 后提取核蛋白和胞质蛋白,Western blot 检测 β-catenin 水平 [1] 结直肠癌细胞 ROS 检测:将 HCT116/DDP 细胞(2×105 个细胞/孔)接种于 6 孔板,用 Salinomycin (Procoxacin)(1–3 μM)处理 24 h。加入 DCFH-DA 探针(10 μM)负载 30 min,流式细胞术分析 ROS 水平。凋亡相关蛋白检测:处理 48 h 后提取总蛋白,Western blot 检测剪切型 caspase-3、caspase-9、Bax 及 Bcl-2 [2] CSC 球形成实验:从结直肠癌组织中分离 CR-CSCs,将单细胞(100 个细胞/孔)接种于超低吸附 96 孔板,加入 Salinomycin (Procoxacin)(0.5–2 μM)处理。培养 7 天后,计数球状体数量(直径 >50 μm)评估自我更新能力。处理 48 h 后采用 qPCR 检测 CD44、CD133、ALDH1 的 mRNA 表达 [3] 肝癌细胞周期分析:将 HepG2 细胞(3×105 个细胞/孔)接种于 6 孔板,用 Salinomycin (Procoxacin)(1–3 μM)处理 24 h。70% 乙醇固定细胞,碘化丙啶染色,流式细胞术分析细胞周期分布(G0/G1、S、G2/M 期)[4] 膀胱癌细胞侵袭实验:Transwell 小室上室包被 Matrigel,加入含 Salinomycin (Procoxacin)(0.5–2 μM)的 T24 细胞(5×104 个细胞/小室),下室加入含 10% 胎牛血清的培养基。孵育 24 h 后,固定并染色下室表面的侵袭细胞,显微镜下计数 [5] |
| 动物实验 |
Mice: 4 and 8 mg/kg, i.p. inection; Rat: 8 mg/kg, i.p. inection
Mice: Nude mice (nu/nu; 4-6 weeks of age) are used. HepG2 cells are suspended in 100 mL 1:1 serum-free DMEM and Matrigel. Mice are anesthetized with ketamine/xylazine and after surgically opening the abdomen, HepG2 cells are inoculated into the liver parenchyma and mice are monitored every 3 days for 35 days. Finally, 18 nude mice are divided into three groups that are intraperitoneally injected daily for 6 weeks: two Salinomycin-treated groups (4 mg/kg Salinomycin group, 8 mg/kg Salinomycin group) and the control group (saline water group) Rats: total of 10 male rats are used in the experiment. After a routine anesthesia, the abdomen is opened. After a resuspension of high glucose medium not containing serum DMEM, and matrigel, the bladder transitional cancer cell line T24 is inoculated in the parenchyma of bladder in rats, and then the abdomen is sutured. After operation, the rats are randomized into the experiment group and the control group with five in each group. After operation, the rats in the experiment group are immediately given intraperitoneal injection of Salinomycin with a dosage of 8 mg/kg, while the rats in the control group are given intraperitoneal injection of normal saline. A close observation is paid during the drug administration period. After 15 d, the rats are sacrificed by cervical dislocation, and the complete tumor tissues are stripped to observe the tumor growth and metastasis. Colorectal cancer xenograft model: Nude mice (6–8 weeks old) were subcutaneously injected with HCT116 cells (5×106 cells/mouse) to establish xenografts. When tumors reached 100 mm3, mice were randomly divided into control and treatment groups (n=6/group). Salinomycin (Procoxacin) was dissolved in DMSO and diluted with PBS (final DMSO concentration <5%), administered via intraperitoneal injection at 5 mg/kg, 3 times a week for 4 weeks. Tumor volume was measured every 3 days, and mice were euthanized at the end of treatment to collect tumors for ROS detection and CSC marker analysis [3] HCC xenograft model: BALB/c nude mice (6–8 weeks old) were subcutaneously implanted with HepG2 cells (2×106 cells/mouse). When tumors grew to 80–100 mm3, mice were assigned to control (vehicle) or treatment groups (n=5/group). Salinomycin (Procoxacin) was prepared as a 1 mg/mL suspension in 0.5% carboxymethylcellulose, administered via intraperitoneal injection at 4 mg/kg, twice a week for 5 weeks. Tumor weight and volume were recorded, and tumor tissues were collected for TUNEL assay and Western blot analysis of Wnt signaling proteins [4] CSC xenograft model: SCID mice (6–8 weeks old) were injected with breast cancer CSCs (1×105 cells/mouse) subcutaneously. After tumor formation (50 mm3), mice were treated with Salinomycin (Procoxacin) (dissolved in 0.9% NaCl) via oral gavage at 10 mg/kg, daily for 3 weeks. Tumor recurrence was monitored for 8 weeks post-treatment, and tumor tissues were analyzed for ALDH1+ CSC content [6] |
| 药代性质 (ADME/PK) |
Absorption, Distribution and Excretion
Salinomycin was administered to chickens orally and intravenously to determine blood concentration, kinetic behavior, bioavailability and tissue residues. The drug was given by intracrop and intravenous routes in a single dose of 20 mg kg-1 body-weight. The highest serum concentrations of salinomycin were reached half an hour after oral dosage with an absorption half-life (t0.5(ab)) of 3.64 hours and elimination half-life (t0.5(beta)) of 1.96 hours. The systemic bioavailability percentage was 73.02 per cent after intracrop administration, indicating the high extent of salinomycin absorption from this route in chickens. Following intravenous injection the kinetics of salinomycin can be described by a two-compartment open model with a t1/2(alpha) of 0.48 hours, Vd ss (volume of distribution) of 3.28 litre kg-1 and Cl(beta) (total body clearance) of 27.39 ml kg-1 min-1. The serum protein-binding tendency of salinomycin as calculated in vitro was 19.78 per cent. Salinomycin concentrations in the serum and tissues of birds administered salinomycin premix (60 ppm) for two weeks were lower than those after administration of a single intracrop dose of pure salinomycin (20 mg kg-1 bodyweight). The highest concentration of salinomycin residues were present in the liver followed by the kidneys, muscles, fat, heart and skin. No salinomycin residues were detected in tissues after 48 hours except in the liver and these had disappeared completely by 72 hours. Metabolism / Metabolites ... Salinomycin (SAL), a broad spectrum antibiotic and a coccidiostat has been found to counter tumour resistance and kill cancer stem cells with better efficacy than the existing chemotherapeutic agents; paclitaxel and doxorubicin. This refocused its importance for treatment of human cancers. In this study, we studied the in vitro drug metabolism and pharmacokinetic parameters of SAL. SAL undergoes rapid metabolism in liver microsomes and has a high intrinsic clearance. SAL metabolism is mainly mediated by CYP enzymes; CYP3A4 the major enzyme metabolising SAL. The percent plasma protein binding of SAL in human was significantly lower as compared to mouse and rat plasma. CYP inhibition was carried out by chemical inhibition and recombinant enzyme studies. SAL was found to be a moderate inhibitor of CYP2D6 as well as CYP3A4. As CYP3A4 was the major enzyme responsible for metabolism of SAL, in vivo pharmacokinetic study in rats was done to check the effect of concomitant administration of Ketoconazole (KTC) on SAL pharmacokinetics. KTC, being a selective CYP3A4 inhibitor increased the systemic exposure of SAL significantly to 7-fold in AUC0-a and 3-fold increase in Cmax of SAL in rats with concomitant KTC administration. Biological Half-Life ... The drug was given by intracrop and intravenous routes in a single dose of 20 mg kg-1 body-weight. The highest serum concentrations of salinomycin were reached half an hour after oral dosage with an absorption half-life (t0.5(ab)) of 3.64 hours and elimination half-life (t0.5(beta)) of 1.96 hours. ... |
| 毒性/毒理 (Toxicokinetics/TK) |
Toxicity Summary
IDENTIFICATION AND USE: Salinomycin is a veterinary drug used for the prevention of coccidiosis in broiler, roaster and replacement chickens caused by Eimeria tenella, E. necatrix, E. acervulina, E. maxima, E. brunetti and E. mivati. It is also used for the prevention of coccidiosis in quail caused by Eimeria dispersa and E. lettyae. HUMAN EXPOSURE AND TOXICITY: The cytotoxic and genotoxic effects of salinomycin were investigated in human non-malignant cells. Primary human nasal mucosa cells (monolayer and mini organ cultures) and peripheral blood lymphocytes from 10 individuals were used to study the cytotoxic effects of salinomycin (0.1-175 uM) by annexin-propidiumiodide- and MTT-test. The comet assay was performed to evaluate DNA damage. Additionally, the secretion of interleukin-8 was analyzed by ELISA. Flow cytometry and MTT assay revealed significant cytotoxic effects in nasal mucosa cells and lymphocytes at low salinomycin concentrations of 10-20 uM. No genotoxic effects could be observed. IL-8 secretion was elevated at 5 uM. Salinomycin-induced cytotoxic and pro-inflammatory effects were seen at concentrations relevant for anti-cancer treatment. ANIMAL STUDIES: There are numerous reports of fatal outcomes when salinomycin is accidently fed to various animals. A sudden outbreak of mortality in one house of 600 48-week-old male breeder turkeys on a five-house turkey breeder farm was suspected to be feed-related. The turkeys gasped and became recumbent; 21.7% of affected turkeys died. Histological lesions, limited to skeletal muscle, consisted of degeneration and necrosis and were judged compatible with ionophore toxicosis. Feed samples from the affected house were analyzed and shown to contain 13.4 to 18.4 g of salinomycin per ton of feed. To further study the effects of salinomycin on turkeys, five 7-day trials using 336, 24, 24, 40, and 40 male turkeys when 7, 11, 15, 27, and 32 weeks of age, respectively. Salinomycin became more toxic as the age of the turkeys increased. When 7-week-old turkeys were fed diets containing 44 or 66 ppm salinomycin, only 1 of 84 died; when turkeys 27 or 32 weeks of age were fed those amounts, 13 of 20 died. Salinomycin at 22 ppm tended to depress rate of growth at young ages and to prevent or decrease growth and to increase mortality at older ages. Accidental poisonings were also reported in six horses fed salinomycin. The range of signs, including anorexia, colic, weakness and ataxia bore similarities to those described in horses poisoned with the related ionophore monensin. In another poisoning, horses were fed a concentrate containing 61 mg/kg salinomycin as faulty prepared by the manufacturer. All horses developed severe clinical signs of intoxication. Despite therapy eight horses died within three to six days. Ten others became recumbent and had to be euthanized. Only six horses survived. The dominating laboratory results were very high enzyme levels and alkalosis. The most characteristic clinical change appeared as paralysis of the hindlimbs. An outbreak of toxic polyneuropathy in cats that had ingested dry cat food contaminated with salinomycin has also been reported. Epidemiologic and clinical data were collected from 823 cats, or about 1% of the cats at risk. In 21 affected cats, postmortem examination was performed. The affected cats had acute onset of lameness and paralysis of the hindlimbs followed by the forelimbs. Clinical and pathologic examination indicated a distal polyneuropathy involving both the sensory and motor nerves. The clinical signs and pathology in an outbreak of toxicity in feedlot cattle attributed to the ingestion of toxic levels of salinomycin over an extended period of 11 weeks have also been reported. Thirty-nine out of 380 cattle developed signs consistent with cardiac failure and 8 of these died. Clinical signs included dyspnea, tachypnea, tachycardia, and exercise intolerance. Two cattle were necropsied and in one there were macroscopic lesions suggestive of congestive heart failure, namely pulmonary edema, hydrothorax and hepatomegaly. Histopathology revealed a chronic cardiomyopathy characterized principally by extensive myocardial fiber atrophy with multifocal hypertrophy and interstitial and replacement fibrosis. Hepatic and pulmonary lesions were consistent with those of congestive cardiac failure. Finally, 100% mortality was reported in a herd of sheep that were given feed containing salinomycin. The morning after the feeding, 78 sheep were found dead and one of them showed convulsive seizures. Postmortem examination revealed pulmonary congestion and edema, hemorrhages in abomasum, large pale kidney and white streak lines in myocardium. Interactions Hepatocellular carcinoma (HCC) is one of the few cancers in which a continuous increase in incidence has been observed over several years. Drug resistance is a major problem in the treatment of HCC. In the present study, we used salinomycin (Sal) and 5-fluorouracil (5-FU) combination therapy on HCC cell lines Huh7, LM3 and SMMC-7721 and nude mice subcutaneously tumor model to study whether Sal could increase the sensitivity of hepatoma cells to the traditional chemotherapeutic agent such as 5-FU. The combination of Sal and 5-FU resulted in a synergistic antitumor effect against liver tumors both in vitro and in vivo. Sal reversed the 5-FU-induced increase in CD133(+) EPCAM(+) cells, epithelial-mesenchymal transition and activation of the Wnt/beta-catenin signaling pathway. The combination of Sal and 5-FU may provide us with a new approach to reverse drug resistant for the treatment of patients with HCC. Chemotherapy for soft tissue sarcomas remains unsatisfactory due to their low chemosensitivity. Even the first line chemotherapeutic agent doxorubicin only yields a response rate of 18-29%. The antibiotic salinomycin, a potassium ionophore, has recently been shown to be a potent compound to deplete chemoresistant cells like cancer stem like cells (CSC) in adenocarcinomas. Here, we evaluated the effect of salinomycin on sarcoma cell lines, whereby salinomycin mono- and combination treatment with doxorubicin regimens were analyzed. To evaluate the effect of salinomycin on fibrosarcoma, rhabdomyosarcoma and liposarcoma cell lines, cells were drug exposed in single and combined treatments, respectively. The effects of the corresponding treatments were monitored by cell viability assays, cell cycle analysis, caspase 3/7 and 9 activity assays. Further we analyzed NF-kappaB activity; p53, p21 and PUMA transcription levels, together with p53 expression and serine 15 phosphorylation. The combination of salinomycin with doxorubicin enhanced caspase activation and increased the sub-G1 fraction. The combined treatment yielded higher NF-kappaB activity, and p53, p21 and PUMA transcription, whereas the salinomycin monotreatment did not cause any significant changes. Salinomycin increases the chemosensitivity of sarcoma cell lines - even at sub-lethal concentrations - to the cytostatic drug doxorubicin. These findings support a strategy to decrease the doxorubicin concentration in combination with salinomycin in order to reduce toxic side effects. A factorial design (2 by 3) was used to evaluate the interaction between aflatoxin (0, 2.5, & 5 mg per kg) & salinomycin (1, 60 g per ton (909 kg)). There were four replicates of 10 chicks per treatment. ... No significant interaction was observed between aflatoxin & salinomycin on any of the parameters measured. This study was aimed to investigate the effect of salinomycin combined with vincristine on the proliferation and apoptosis of Jurkat cells and its possible mechanisms. The proliferation of Jurkat cells was examined by CKK-8 assay. Flow cytometry was used to assess cellular apoptosis. Levels of BCL-2, caspase-3, and caspase- 8 were measured by Western blot. The salinomycin or vincristine, either alone or in combination, inhibited the proliferation of Jurkat cells in a dose-dependent manner. Salinomycin combined with vincristine produced more obvious inhibition of cell proliferation than either compound used alone (P<0.05). Western blot analysis showed that the combined use of Sal and VCR reduced the expression of BCL-2 protein, and increased expression of caspase 3 and caspase 8 protein, more significantly. Furthermore, combination of Sal and VCR synergistally promoted apoptosis of the Jurkat cells (P<0.05). The combination of salinomycin and vincristine synergistically inhibits proliferation and promotes apoptosis of T-cell acute lymphoblastic leukemia Jurkat cells. In nude mice treated with Salinomycin (Procoxacin) (5 mg/kg, intraperitoneal injection, 3 times/week for 4 weeks), no significant changes in body weight (variation <10%) or hematological parameters (WBC, RBC, platelets) were observed; histopathological examination of liver and kidney showed no obvious drug-related lesions [3] In BALB/c nude mice receiving Salinomycin (Procoxacin) (4 mg/kg, intraperitoneal injection, twice a week for 5 weeks), serum ALT, AST, creatinine, and BUN levels remained within normal ranges, indicating no obvious hepatotoxicity or nephrotoxicity [4] In vitro, Salinomycin (Procoxacin) showed low toxicity to normal peripheral blood mononuclear cells (PBMCs) with an IC50 >10 μM, while exhibiting selective toxicity to CLL cells (IC50=1 μM) [1] In SCID mice treated with oral Salinomycin (Procoxacin) (10 mg/kg, daily for 3 weeks), mild diarrhea was observed in 20% of mice, which resolved spontaneously without treatment interruption [6] |
| 参考文献 |
|
| 其他信息 |
Therapeutic Uses
Anti-Bacterial Agents; Coccidiostats EXPL: The drug target profile proposed by the Medicines for Malaria Venture for a malaria elimination/eradication policy focuses on molecules active on both asexual and sexual stages of Plasmodium, thus with both curative and transmission-blocking activities. The aim of the present work was to investigate whether the class of monovalent ionophores, which includes drugs used in veterinary medicine and that were recently proposed as human anticancer agents, meets these requirements. The activity of salinomycin, monensin, and nigericin on Plasmodium falciparum asexual and sexual erythrocytic stages and on the development of the Plasmodium berghei and P. falciparum mosquito stages is reported here. Gametocytogenesis of the P. falciparum strain 3D7 was induced in vitro, and gametocytes at stage II and III or stage IV and V of development were treated for different lengths of time with the ionophores and their viability measured with the parasite lactate dehydrogenase (pLDH) assay. The monovalent ionophores efficiently killed both asexual parasites and gametocytes with a nanomolar 50% inhibitory concentration (IC50). Salinomycin showed a fast speed of kill compared to that of standard drugs, and the potency was higher on stage IV and V than on stage II and III gametocytes. The ionophores inhibited ookinete development and subsequent oocyst formation in the mosquito midgut, confirming their transmission-blocking activity. Potential toxicity due to hemolysis was excluded, since only infected and not normal erythrocytes were damaged by ionophores. Our data strongly support the downstream exploration of monovalent ionophores for repositioning as new antimalarial and transmission-blocking leads. EXPL: Salinomycin has been introduced as a novel alternative to traditional anti-cancer drugs. The aim of this study was to test a strategy designed to deliver salinomycin to glioblastoma cells in vitro. Salinomycin-encapsulated polysorbate 80-coated poly(lactic-co-glycolic acid) nanoparticles (P80-SAL-PLGA) were prepared and characterized with respect to particle size, morphology, thermal properties, drug encapsulation efficiency and controlled salinomycin-release behaviour. The in vitro cellular uptake of P80-SAL-PLGA (5 and 10 uM) or uncoated nanoparticles was assessed in T98G human glioblastoma cells, and the cell viability was investigated with respect to anti-growth activities. SAL, which was successfully transported to T98G glioblastoma cells via P80 coated nanoparticles (~14% within 60 min), greatly decreased (p < 0.01) the cellular viability of T98G cells. Substantial morphological changes were observed in the T98G cells with damaged actin cytoskeleton. Thus, P80-SAL-PLGA nanoparticles induced cell death, suggesting a potential therapeutic role for this salinomycin delivery system in the treatment of human glioblastoma. MEDICATION (VET): Use Sacox 60 ... for the prevention of coccidiosis in quail caused by Eimeria dispersa and E. lettyae. MEDICATION (VET): Use Sacox 60 ... for the prevention of coccidiosis in broiler, roaster and replacement chickens caused by Eimeria tenella, E. necatrix, E. acervulina, E. maxima, E. brunetti and E. mivati. Drug Warnings Do not feed to laying hens producing eggs for human consumption. May be fatal if accidentally fed to adult turkeys or to horses. Salinomycin (Procoxacin) inhibits Wnt signaling by preventing β-catenin nuclear translocation, thereby blocking the transcription of Wnt-dependent oncogenes (c-Myc, cyclin D1) in CLL cells [1] The anti-tumor activity of Salinomycin (Procoxacin) in cisplatin-resistant colorectal cancer cells is dependent on ROS accumulation, which triggers mitochondrial dysfunction and caspase-dependent apoptosis [2] Salinomycin (Procoxacin) exhibits higher selectivity for cancer stem cells compared to conventional chemotherapeutic agents (e.g., paclitaxel, cisplatin), making it a potential candidate for targeting CSC-driven tumor recurrence and metastasis [6] In HCC cells, Salinomycin (Procoxacin) synergizes with sorafenib to enhance anti-tumor efficacy, reducing the IC50 of sorafenib by 50% when combined at sub-effective concentrations [4] Salinomycin (Procoxacin) inhibits bladder cancer cell invasion by downregulating MMP-2 and MMP-9, which are key enzymes involved in extracellular matrix degradation [5] |
| 分子式 |
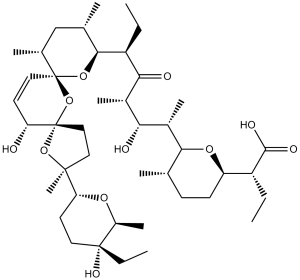
C42H70O11
|
|
|---|---|---|
| 分子量 |
751.00
|
|
| 精确质量 |
750.49
|
|
| 元素分析 |
C, 67.17; H, 9.40; O, 23.43
|
|
| CAS号 |
53003-10-4
|
|
| 相关CAS号 |
Salinomycin sodium salt;55721-31-8
|
|
| PubChem CID |
3085092
|
|
| 外观&性状 |
brown solid powder
|
|
| 密度 |
1.2±0.1 g/cm3
|
|
| 沸点 |
839.2±65.0 °C at 760 mmHg
|
|
| 熔点 |
112.5-113.5 °C(lit.)
|
|
| 闪点 |
243.2±27.8 °C
|
|
| 蒸汽压 |
0.0±0.6 mmHg at 25°C
|
|
| 折射率 |
1.547
|
|
| LogP |
6.1
|
|
| tPSA |
164.04
|
|
| 氢键供体(HBD)数目 |
4
|
|
| 氢键受体(HBA)数目 |
11
|
|
| 可旋转键数目(RBC) |
12
|
|
| 重原子数目 |
53
|
|
| 分子复杂度/Complexity |
1320
|
|
| 定义原子立体中心数目 |
18
|
|
| SMILES |
O1[C@@]2([C@@]([H])(C([H])=C([H])[C@@]3([C@]([H])(C([H])([H])[H])C([H])([H])[C@]([H])(C([H])([H])[H])[C@@]([H])([C@@]([H])(C([H])([H])C([H])([H])[H])C([C@@]([H])(C([H])([H])[H])[C@]([H])([C@]([H])(C([H])([H])[H])[C@@]4([H])[C@@]([H])(C([H])([H])[H])C([H])([H])C([H])([H])[C@]([H])([C@]([H])(C(=O)O[H])C([H])([H])C([H])([H])[H])O4)O[H])=O)O3)O2)O[H])C([H])([H])C([H])([H])[C@@]1(C([H])([H])[H])[C@@]1([H])C([H])([H])C([H])([H])[C@](C([H])([H])C([H])([H])[H])([C@]([H])(C([H])([H])[H])O1)O[H]
|
|
| InChi Key |
KQXDHUJYNAXLNZ-XQSDOZFQSA-N
|
|
| InChi Code |
InChI=1S/C42H70O11/c1-11-29(38(46)47)31-15-14-23(4)36(50-31)27(8)34(44)26(7)35(45)30(12-2)37-24(5)22-25(6)41(51-37)19-16-32(43)42(53-41)21-20-39(10,52-42)33-17-18-40(48,13-3)28(9)49-33/h16,19,23-34,36-37,43-44,48H,11-15,17-18,20-22H2,1-10H3,(H,46,47)/t23-,24-,25+,26-,27-,28-,29+,30-,31+,32+,33+,34+,36+,37-,39-,40+,41-,42-/m0/s1
|
|
| 化学名 |
(2R)-2-[(2R,5S,6R)-6-[(2S,3S,4S,6R)-6-[(3S,5S,7R,9S,10S,12R,15R)-3-[(2R,5R,6S)-5-ethyl-5-hydroxy-6-methyloxan-2-yl]-15-hydroxy-3,10,12-trimethyl-4,6,8-trioxadispiro[4.1.57.35]pentadec-13-en-9-yl]-3-hydroxy-4-methyl-5-oxooctan-2-yl]-5-methyloxan-2-yl]butanoic acid
|
|
| 别名 |
|
|
| HS Tariff Code |
2934.99.9001
|
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
|
|||
|---|---|---|---|---|
| 溶解度 (体内实验) |
配方 1 中的溶解度: ≥ 2.5 mg/mL (3.33 mM) (饱和度未知) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。
例如,若需制备1 mL的工作液,可将100 μL 25.0 mg/mL澄清DMSO储备液加入到400 μL PEG300中,混匀;然后向上述溶液中加入50 μL Tween-80,混匀;加入450 μL生理盐水定容至1 mL。 *生理盐水的制备:将 0.9 g 氯化钠溶解在 100 mL ddH₂O中,得到澄清溶液。 配方 2 中的溶解度: ≥ 2.5 mg/mL (3.33 mM) (饱和度未知) in 10% DMSO + 90% Corn Oil (这些助溶剂从左到右依次添加,逐一添加), 澄清溶液。 例如,若需制备1 mL的工作液,可将 100 μL 25.0 mg/mL 澄清 DMSO 储备液加入到 900 μL 玉米油中并混合均匀。 View More
配方 3 中的溶解度: 2.5 mg/mL (3.33 mM) in 5% DMSO + 40% PEG300 + 5% Tween80 + 50% Saline (这些助溶剂从左到右依次添加,逐一添加), 悬浊液; 超声助溶。 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.3316 mL | 6.6578 mL | 13.3156 mL | |
| 5 mM | 0.2663 mL | 1.3316 mL | 2.6631 mL | |
| 10 mM | 0.1332 mL | 0.6658 mL | 1.3316 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
 Sal inhibits HCC cell proliferationin vitro.PLoS One.2012;7(12):e50638. |
|---|
 Sal causes cell cycle arrest and induces apoptosis of HCC cellsin vitro.PLoS One.2012;7(12):e50638. |
 Sal increases intracellular Calcium levelsin vitro.PLoS One.2012;7(12):e50638. |
 Anti-tumor activity of Salin vivo.A. HE staining showed the structure of the liver cancer tissue: nuclei of different sizes, hepatic cord structure was destroyed. B. Immunohistochemistry indicates that PCNA expression is down-regulated after Sal.PLoS One.2012;7(12):e50638. |
|---|
 A. Gross observation of HepG2 cell orthotopic tumors in nude mice from the saline group or Sal groups (4 mg/kg or 8 mg/kg). B. Tendency of tumor mean diameter after injection in nude mice (*p<0.05).PLoS One.2012;7(12):e50638. |
 A. Real-time PCR was performed to examine mRNA expression of the Wnt pathway.PLoS One.2012;7(12):e50638. |