| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| Other Sizes |
|

| 靶点 |
thrombin (Ki = 4.5 nM)
|
|---|---|
| 体外研究 (In Vitro) |
体外活性:Dabigatran/BIBR 953 是一种非常有效的抗凝血剂。 BIBR 953 表明末端苯基可以被更亲水的 2-吡啶基取代,而不会显着损失活性。 BIBR 953 抑制凝血酶、纤溶酶、因子 Xa、胰蛋白酶、tPA 和活化蛋白 C,Ki 分别为 4.5 nM、1.7 μM、3.8 μM、50 nM、45 μM 和 20 μM。 BIBR 953 特异性且可逆地抑制凝血酶。
达比加群是一种可逆、选择性的直接凝血酶抑制剂(DTI),作为其口服活性前药达比加群组酯正在进行高级临床开发。本研究旨在确定达比加群及其前药达比加群组酯的分子效力和抗凝功效。这是通过酶抑制和选择性分析、表面等离子体共振研究、血小板聚集、凝血酶产生和体外凝血试验实现的。这些研究表明,达比加群选择性和可逆地抑制人凝血酶(Ki:4.5 nM)以及凝血酶诱导的血小板聚集(IC(50):10 nM),而对其他血小板刺激剂没有抑制作用。以内源性凝血酶电位(ETP)测量的血小板缺乏血浆(PPP)中凝血酶的产生受到浓度依赖性抑制(IC(50):0.56微M)。达比加群在体外各种物种中表现出浓度依赖性抗凝作用,在0.23、0.83和0.18微M的浓度下,人PPP中的活化部分凝血活酶时间(aPTT)、凝血酶原时间(PT)和埃卡蛋白凝血时间(ECT)分别加倍。 |
| 体内研究 (In Vivo) |
BIBR 953/Dabigatran 在对大鼠进行静脉注射后表现出最有利的活性。达比加群酯口服给药后Dabigatran/达比加群的生物利用度为7.2%。口服治疗后达比加群主要通过粪便排泄,静脉注射治疗后达比加群主要通过尿液排泄。达比加群的平均终末半衰期约为 8 小时。口服和静脉注射给药后,达比加群酰基葡萄糖醛酸苷分别占尿液中剂量的 0.4% 和 4%。
在体内,大鼠(0.3、1和3 mg/kg)和恒河猴(0.15、0.3和0.6 mg/kg)静脉注射Dabigatran/达比加群后, 剂量依赖性地延长aPTT。对清醒大鼠(10、20和50mg/kg)或恒河猴(1、2.5或5mg/kg)口服Dabigatran/达比加群酯,观察到剂量和时间依赖性抗凝作用,分别在给药后30至120分钟观察到最大作用。这些数据表明,达比加群是一种强效的选择性凝血酶抑制剂,也是一种口服活性抗凝剂,作为前药,达比加群酯。[1] 达比加群是一种可逆的直接、选择性凝血酶抑制剂,正在作为其口服活性前药达比加群组酯进行临床开发。本试验旨在评估达Dabigatran和Dabigatran酯在静脉血栓形成大鼠模型中的抗血栓和抗凝作用。为了做到这一点,使用改良的Wessler模型来评估静脉注射(i.v.)达比加群和口服达比加群组酯的抗血栓和抗凝作用。此外,使用大鼠尾部出血时间模型来研究达比加群的抗止血作用。该研究表明,大剂量服用达比加群(0.01-0.1 mg/kg)可剂量依赖性地减少血栓形成,ED50(有效剂量的50%)为0.033 mg/kg,在0.1 mg/kg时完全抑制。相比之下,肝素(0.03-0.3 mg/kg)、水蛭素(0.01-0.5 mg/kg)和美拉加群的ED50值分别为0.07、0.15和0.12 mg/kg。口服达比加群酯(5-30mg/kg)以剂量和时间依赖的方式抑制血栓形成,在预处理后30分钟内抑制作用最强,表明作用起效迅速。静脉注射达比加群(0.1-1.0 mg/kg)后,观察到出血时间在统计学上显著延长,剂量分别比ED50和ED100(有效剂量的100%)剂量大至少15倍和5倍;在最大治疗有效剂量(0.1mg/kg)下,出血倾向没有显著增加。可以得出结论,达比加群及其口服前药达比加群组酯在血栓栓塞性疾病的治疗中显示出希望[3]。 由于其强大的体外活性和相对于相关丝氨酸蛋白酶的良好选择性(表3),对达比加群/Dabigatran/24进行了深入的生物学研究,结果证明它是一种非常有效的体内抗凝剂。在这类结构的所有抑制剂中,静脉注射给药后,它在麻醉大鼠中表现出最强的活性和最长的作用持续时间。与化合物2不同,它在这些动物中耐受性良好,最高给药剂量为10mg/kg。然而,它没有口服活性,考虑到它是一种极性很强、永久带电的分子,logP为-2.4(正辛醇/缓冲液,pH 7.4),这并不奇怪[2]。 在30天时,我们观察到无抗凝组有638±895 mg血栓,依诺肝素组有121±128 mg血栓,Dabigatran/达比加群酯组有19±31 mg血栓(P=0.01依诺肝素vs达比加群组酯)。达比加群酯组瓣膜上沉积的血小板(2.7×108)少于依诺肝素组(1.8×109,P=0.03)。未观察到重大或隐性出血或栓塞事件。通过血栓弹性分析,达比加群酯的K值延长(P=.01)和角度(P=.01)和最大振幅(P=.001)的降低均小于依诺肝素。 达比加群酯与依诺肝素在机械瓣膜短期血栓预防方面同样有效。它可以在30天内防止瓣膜血栓和血小板沉积,而不会增加不良事件。这些有希望的结果为达比加群酯作为双叶机械主动脉瓣患者华法林替代品的前瞻性临床试验奠定了基础。[4] 剂量研究[4] 每日两次口服20mg/kg的达比加群酯,可将APTT增加到正常值的2至2.5倍(图2,A)。每天两次皮下注射2.0 mg/kg依诺肝素,可将抗Xa水平可重复地提高到至少0.6(图2,B)。这些剂量用于研究的剩余时间。 抗凝治疗的测量[4] 连续的血液学检测证实了两个治疗组的适当剂量和药物效果。接受Dabigatran/达比加群酯治疗的动物APTT升高,凝血酶原时间也显著增加。(图3,A和B)。正如预期的那样,我们观察到,与未抗凝组和达比加群酯组相比,接受依诺肝素的动物在所有时间点的抗Xa水平都有所升高(图3,C)。在研究的所有3个时间点,我们观察到达比加群酯组的循环纤维蛋白原明显减少(图3,D)。 瓣膜血栓[4] 术后第6天,非抗凝组有1人因严重败血症而过早死亡。当动物被杀死时,两组之间的平均血栓重量存在统计学差异。我们观察到638±895 mg血栓,未使用抗凝药物,121±128 mg使用依诺肝素,19±31 mg使用达比加群酯(P=0.04;图4A)。这表示达比加群酯组的平均瓣膜血栓比未抗凝组减少了30倍。比较两个治疗组,我们发现接受达比加群酯治疗的动物瓣膜血栓明显减少(P=0.02;图4,B)。同样,达比加群酯组瓣膜假体上沉积的血小板平均数(2.7×108)低于依诺肝素组(1.8×109,(P=0.03;图4,C)。无抗凝、依诺肝素和达比加群酯组移植瓣膜的代表性尸检照片如图5所示。 血栓弹性成像[4] 在基线和抗凝期间进行了天然和高岭土血栓弹性测定。我们观察到,至少在体内,接受达比加群酯治疗的动物的血栓弹性凝血曲线(R和K时间、角度和最大振幅)看起来更像没有抗凝治疗的动物,而不是接受依诺肝素治疗的动物(图6)。高岭土和天然血栓弹性分析都是如此(天然数据未显示),这表明尽管血栓弹性分析结果正常,但抗凝治疗充分。 |
| 酶活实验 |
凝血酶抑制的测量。[2]
用市售的显色法测定化合物的凝血酶抑制作用(IC50)。将人凝血酶(0.042 U/mL)在37°C下与溶解在DMSO中的10种不同稀释液(浓度范围为0.003-100μM)的试验化合物或DMSO作为对照预孵育10分钟。在将预孵育混合物添加到显色底物甲苯磺酰-甘氨酰-脯氨酰-精氨酸-4-硝基苯胺乙酸酯中后,硝基苯胺被凝血酶裂解,并在分光光度计中测量与游离硝基苯胺相关的405nm处吸光度的增加。通过绘制405nm处的吸光度与测试化合物浓度的关系图,计算出诱导50%凝血酶抑制的浓度(IC50)。所有测量均进行了两次,并表示了两次测定的平均值。 aPTT的测量。[2] aPTT在凝血仪中测量,作为相应化合物抗凝血作用的量度。在柠檬酸钠溶液(终浓度0.313%)中收集血液样本。将每份天然血液样本(0.1 mL)移入预热至37°C的试管中。加入PTT试剂(0.1 mL),混合并孵育3分钟。加入预热至37°C的氯化钙溶液(0.1 mL。 |
| 动物实验 |
雄性大鼠(Wessler模型)[3]
\n0.01、0.03、0.05 和 0.1 mg/kg \n静脉注射\n \n\n30头猪接受了改良双叶机械瓣膜管道植入术,该管道绕过结扎的自体降主动脉。动物随机分为三组:不接受抗凝治疗(n = 10)、皮下注射依诺肝素2 mg/kg,每日两次(n = 10)或口服达比加群酯20 mg/kg,每日两次。主要终点为30天时瓣膜血栓的量。次要终点包括瓣膜假体上血小板沉积的定量测量、血栓弹力图以及出血和栓塞事件。 [4] \n\n剂量研究[4] \n达比加群酯是一种新型的口服直接凝血酶抑制剂达比加群的前体药物。与华法林不同,它起效迅速,剂量反应可预测。此外,目前尚未发现其与食物或药物相互作用,也无需频繁监测治疗效果。其半衰期约为12小时,且无其他活性代谢物。达比加群主要通过肾脏排泄。 \n\n为了确定达比加群酯和依诺肝素在猪体内的最佳剂量,我们首先进行了一项剂量研究。动物分别接受达比加群酯或依诺肝素给药,并在0、0.5、1、2、4、8、12、24、36、48和72小时采集相应的血液学检测样本。11 我们的目的是找到与我们动物品系治疗水平相对应的达比加群酯和依诺肝素剂量。对于达比加群酯,我们的目标是使活化部分凝血酶原时间(APTT)延长至正常值的2至2.5倍。对于依诺肝素,我们寻求在 4 小时时达到至少 0.6 的抗 Xa 水平。12\n \n\n机械瓣膜的体内血栓预防[4] \n关于这种异位主动脉瓣膜假体模型的具体细节已在其他文献中报道。9, 13 简而言之,30 头猪被随机分为 3 个术后抗凝治疗组。这些治疗包括:不进行抗凝治疗(n = 10)、皮下注射依诺肝素 2.0 mg/kg,每日两次(n = 10)以及口服达比加群酯 20 mg/kg,每日两次(n = 10)。本研究中使用的是达比加群酯的临床制剂(包覆药物的小型酒石酸颗粒,装于胶囊中)。由于在猪体内难以维持华法林的治疗窗,因此采用低分子量肝素依诺肝素作为抗凝治疗的标准药物。14 此外,低分子量肝素还用于帮助患者过渡到华法林抗凝治疗,并作为某些无法服用华法林的患者的华法林替代方案。15, 16 这些剂量是根据我们的给药研究结果确定的。动物从术后第1天开始接受分配的治疗药物。\n \n\n\n凝血谱[4] \n我们使用了多种血液学和抗凝血试验来评估达比加群酯对凝血系统的影响。在基线(瓣膜植入前)、第10天和第20天以及动物处死时(第30天),我们进行了全血细胞计数;测量了凝血酶原时间、APTT、纤维蛋白原和抗Xa水平;并进行了血栓弹力图检查。我们使用了配备天然和高岭土杯及针的TEG 5000设备(Haemoscope公司,伊利诺伊州奈尔斯市)。测量指标包括R时间(分钟)、K时间(分钟)、角度(度)和最大振幅(毫米)。R时间测量初始纤维蛋白形成所需时间,K时间测量形成牢固血栓和交联所需时间,角度测量血栓强化速度,最大振幅测量最终血栓强度。我们纳入血栓弹力图检查是因为它能够评估整个凝血系统,并且在心血管外科患者的管理中应用越来越广泛。 |
| 药代性质 (ADME/PK) |
吸收、分布和排泄
口服达比加群酯后,达比加群的绝对生物利用度约为3%至7%。达比加群酯是外排转运蛋白P-gp的底物。健康志愿者空腹口服达比加群酯后,血药浓度峰值(Cmax)出现在给药后1小时。与高脂餐同服会使达比加群达到Cmax的时间延迟约2小时,但不影响达比加群的生物利用度;达比加群可空腹或与食物同服。 与完整胶囊制剂相比,去除胶囊壳后服用达比加群酯颗粒,其口服生物利用度可提高75%。因此,达比加群胶囊在服用前不应掰开、咀嚼或打开。 达比加群与人血浆蛋白的结合率约为35%。以总放射性测量的达比加群的红细胞/血浆分配系数小于0.3。 达比加群的分布容积为50至70升。单次服用10至400毫克后,达比加群的药代动力学与剂量成正比。每日两次给药时,达比加群的蓄积因子约为2。 有关达比加群(共10项)的更多吸收、分布和排泄(完整)数据,请访问HSDB记录页面。 代谢/代谢物 口服后,达比加群酯转化为达比加群。达比加群酯经酯酶催化水解生成活性成分达比加群是主要的代谢反应。达比加群不是CYP450酶的底物、抑制剂或诱导剂。达比加群可发生结合反应,形成具有药理活性的酰基葡糖醛酸苷。达比加群酯存在四种位置异构体,分别为 1-O、2-O、3-O 和 4-O-酰基葡糖醛酸苷,每种异构体在血浆中占总达比加群酯的比例均低于 10%。 本研究在 10 名健康男性受试者中考察了直接凝血酶抑制剂达比加群酯(BIBR 953 ZW,β-丙氨酸,N-((2-(((4-(氨基亚氨基甲基)苯基)氨基)甲基)-1-甲基-1H-苯并咪唑-5-基)羰基)-N-2-吡啶基)的药代动力学和代谢情况。受试者分别口服 200 mg (14)C-达比加群酯(BIBR 1048 MS,达比加群酯的口服前药)或静脉输注 5 mg (14)C-达比加群酯。在一周内,分别检测血浆、尿液和粪便中的放射性。采用高效液相色谱-在线放射性检测法分析代谢物谱,并用质谱法鉴定代谢物结构。达比加群酯迅速转化为达比加群,血浆达比加群峰浓度在给药后约1.5小时达到……主要的代谢反应是酯酶介导的达比加群酯水解为达比加群。口服给药后,I期代谢物在尿液中占给药剂量的≤0.6%,在粪便中占给药剂量的5.8%;静脉给药后,I期代谢物在尿液中占给药剂量的≤1.5%,在粪便中占给药剂量的0.2%。口服和静脉给药后,达比加群酰基葡糖醛酸苷在尿液中分别占给药剂量的0.4%和4%。体外实验证实,达比加群酯主要由酯酶代谢,细胞色素P450酶不发挥重要作用。这些研究结果表明,口服达比加群酯后,达比加群的药理活性浓度很容易达到,并且达比加群与经细胞色素P450代谢的药物之间发生临床相关相互作用的可能性很低。 生物半衰期 达比加群在健康受试者体内的半衰期为12至17小时。 |
| 毒性/毒理 (Toxicokinetics/TK) |
肝毒性
长期使用达比加群治疗的患者中,1.5%至3%会出现中度ALT升高(超过正常值上限3倍),总体发生率略低于低分子肝素,与华法林相似。虽然尚未有达比加群导致临床明显肝损伤的病例报告发表,但在达比加群的大型上市前临床试验中,曾出现数例伴有黄疸的ALT升高。这些病例症状轻微且具有自限性,停药后即可完全恢复。然而,并非所有病例都能找到其他肝损伤原因,且肝损伤与达比加群治疗的关系尚不明确。这些病例的临床特征未被描述。在一项大型临床试验中,每2000名接受治疗的患者中约有1例出现不明原因的伴有胆红素升高的肝损伤。在随后的病例报告中,患者在开始服用达比加群酯4周内出现肝损伤,伴有黄疸和混合型血清酶升高,停药后症状迅速缓解。该患者未出现免疫过敏和自身免疫特征。世界卫生组织和美国食品药品监督管理局的监测数据库中已收到多例自发性肝损伤报告,其中一些病例死亡,但这些病例之间的关联性尚未明确。因此,达比加群引起的临床上明显的肝损伤伴黄疸虽然罕见,且通常症状较轻并可自愈。 可能性评分:D(可能是临床上明显的肝损伤的罕见病因)。 达比加群之所以受到密切关注其肝毒性证据,原因之一是最初研发并在临床试验中评估的口服直接凝血酶抑制剂是希美拉加群(ximelagatran),该药随后被发现与罕见但可能严重的肝损伤病例相关,通常在治疗1至6个月后出现,表现为肝细胞型血清酶升高,且病情可能严重甚至致命。由于对肝毒性的担忧,希美拉加群未获准在美国使用。在服用希美拉加群的患者中发现更多临床上明显的肝损伤病例后,该药也在欧洲被撤市。后来的研究表明,希美拉加群治疗期间存在血清ALT升高的风险。与 HLA-DRB107 和 DQA1-02 相关。 妊娠和哺乳期影响 ◉ 哺乳期用药概述 在成人中,达比加群酯以甲磺酸达比加群酯前药形式口服吸收率低于 7%;达比加群酯本身不被口服吸收。来自 2 名受试者的初步数据显示,达比加群酯很少分泌到母乳中,不太可能影响母乳喂养的婴儿。如果母亲需要服用达比加群酯,这并非停止母乳喂养的理由。由于数据有限,应监测早产儿或新生儿的出血迹象。 ◉ 对母乳喂养婴儿的影响 在新生儿和早产儿的血液样本中添加达比加群酯,浓度与服用 220 mg 达比加群酯后母乳中的浓度相同。依特昔酯表明不会对凝血产生影响。 ◉ 对哺乳和母乳的影响 截至修订日期,未找到相关的已发表信息。 相互作用 CYP3A4 同工酶底物(阿托伐他汀)与达比加群酯合用,对两种药物的药代动力学均无临床相关影响。同样,CYP2C9 底物(双氯芬酸)与达比加群酯合用,对两种药物的药代动力学也无临床相关影响。 服用利福平 7 天后,单次服用达比加群酯,导致达比加群酯的血浆浓度-时间曲线下面积 (AUC) 和血浆峰浓度分别下降 66% 和 67%。停用利福平 7 天内,达比加群酯的暴露量接近正常水平。预计在不同时使用利福平的情况下不会出现不良反应。应避免同时使用。 达比加群与P-糖蛋白抑制剂合用可能会增加达比加群的全身暴露量。虽然临床数据和药代动力学研究表明,达比加群与某些P-糖蛋白抑制剂(例如胺碘酮、克拉霉素、酮康唑、奎尼丁、维拉帕米)合用无需调整剂量,但生产商指出,这些结果不应推广至所有P-糖蛋白抑制剂。 肾功能不全患者同时使用P-糖蛋白转运抑制剂和达比加群预计会增加达比加群的全身暴露量,高于单独使用任一药物的情况。对于中度肾功能不全(肌酐清除率为30-50 mL/分钟)且同时接受决奈达隆或全身性利福平治疗的患者,应考虑降低达比加群的剂量。酮康唑。对于严重肾功能损害(肌酐清除率为 15-30 mL/分钟)的患者,应避免同时使用达比加群和 P-糖蛋白转运抑制剂。 有关达比加群的更多(完整)相互作用数据(共 20 项),请访问 HSDB 记录页面。 |
| 参考文献 |
|
| 其他信息 |
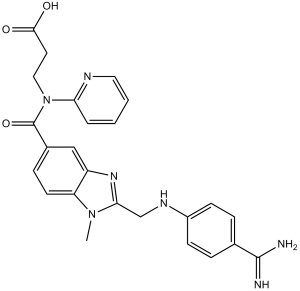
达比加群是一种芳香酰胺,由2-{[(4-氨基甲酰苯基)氨基]甲基}-1-甲基-1H-苯并咪唑-5-羧酸的羧基与N-吡啶-2-基-β-丙氨酸的仲氨基缩合而成。它是前药达比加群酯的活性代谢物,具有抗凝血作用,用于预防卒中和全身性栓塞。它是一种抗凝血剂,同时也是EC 3.4.21.5(凝血酶)抑制剂和EC 1.10.99.2 [核糖基二氢烟酰胺脱氢酶(醌)]抑制剂。它是一种芳香酰胺,属于苯并咪唑类、羧脒类、吡啶类和β-丙氨酸衍生物。
达比加群是口服生物利用度高的前药[达比加群酯]的活性形式。 达比加群是一种直接凝血酶抑制剂。达比加群的作用机制是作为凝血酶抑制剂。 达比加群是一种直接凝血酶抑制剂和抗凝剂,用于预防慢性房颤患者的卒中和静脉栓塞。达比加群治疗与较低的血清酶升高发生率相关,肝酶升高和黄疸的发生率极低。 达比加群是一种苯并咪唑类直接凝血酶抑制剂,具有抗凝活性。达比加群给药后,可逆性地与凝血酶(一种丝氨酸蛋白酶,可将纤维蛋白原转化为纤维蛋白)结合并抑制其活性。这会破坏凝血级联反应并抑制血栓形成。 达比加群是一种凝血酶抑制剂,其作用机制是通过结合并阻断血栓形成活性,从而预防血栓形成。它用于降低非瓣膜性房颤患者的卒中和全身性栓塞风险。 另见:达比加群酯(其活性部分);达比加群甲磺酸酯(其活性部分);达比加群乙酯(其活性部分)。 作用机制 达比加群及其酰基葡糖醛酸苷是竞争性直接凝血酶抑制剂。由于凝血酶(丝氨酸蛋白酶)在凝血级联反应中能够将纤维蛋白原转化为纤维蛋白,因此抑制凝血酶可以阻止血栓的形成。活性部分能够抑制游离的和与血栓结合的凝血酶,以及凝血酶诱导的血小板聚集。 ……为了评估新型直接凝血酶抑制剂达比加群的促纤溶作用,我们使用了不同的体外模型。达比加群以浓度依赖的方式降低了组织因子诱导的血浆凝块对外部组织型纤溶酶原激活剂(t-PA)纤溶的抵抗力(浊度法),在临床相关浓度(1-2 μM)下,溶解时间缩短≥50%。在低浓度(0.1和1 nM)的血栓调节蛋白存在下观察到了类似的效果,但在高浓度(10 nM)的血栓调节蛋白存在下则未观察到。达比加群加速血栓溶解与TAFI活化和凝血酶生成减少相关,而活化TAFI抑制剂——马铃薯块茎羧肽酶抑制剂——可显著(但并非完全)抵消达比加群的这种作用。对血栓粘弹性特性的评估表明,在达比加群存在下生成的血栓通透性更高、刚性更低,且纤维更粗。利用流动条件下的模型研究了这些物理变化对纤维蛋白溶解的影响,结果表明,达比加群通过一种主要不依赖于TAFI的机制,显著增强了血栓对t-PA的敏感性。在临床相关浓度下,达比加群通过降低TAFI活化和改变血栓结构,增强血浆血栓对t-PA诱导溶解的敏感性。这些机制可能有助于该药物的抗血栓活性。 治疗用途 苯并咪唑类;β-丙氨酸/类似物及衍生物 达比加群适用于降低非瓣膜性房颤患者的卒中和全身性栓塞风险。/美国产品标签包含/ 药物警告 /黑框警告/ 警告:过早停用达比加群会增加血栓事件的风险。过早停用任何口服抗凝剂,包括达比加群,都会增加血栓事件的风险。如果因病理性出血或疗程结束以外的原因停止使用达比加群酯(Pradaxa)进行抗凝治疗,请考虑使用其他抗凝药物。 /黑框警告/ 脊髓/硬膜外血肿。接受达比加群酯治疗并接受椎管内麻醉或脊髓穿刺的患者可能会发生硬膜外或脊髓血肿。这些血肿可能导致长期或永久性瘫痪。在安排患者进行脊髓手术时,应考虑这些风险。可能增加这些患者发生硬膜外或脊髓血肿风险的因素包括:使用留置硬膜外导管;同时使用其他影响止血的药物,例如非甾体类抗炎药(NSAIDs)、血小板抑制剂、其他抗凝药物;有创伤性或反复硬膜外或脊髓穿刺史;有脊柱畸形或脊柱手术史;达比加群酯(Pradaxa)给药与椎管内介入治疗之间的最佳时间尚不明确。应密切监测患者的神经功能障碍体征和症状。如发现神经功能受损,必须立即进行治疗。对于正在接受或即将接受抗凝治疗的患者,在进行椎管内介入治疗前,应权衡利弊。 美国食品药品监督管理局(FDA)正在评估达比加群酯甲磺酸盐(Pradaxa)上市后报告的严重出血事件。出血可能导致严重甚至致命的后果,是所有抗凝治疗的常见并发症。达比加群的药品说明书包含关于严重甚至致命出血的警告。在一项比较达比加群和华法林的大型临床试验(18,000名患者)中,两种药物的主要出血事件发生率相似。FDA正在努力确定,根据支持达比加群获批的大型临床试验的观察结果,服用达比加群的患者出血事件的报告是否比预期更为常见。达比加群是一种血液稀释剂(抗凝剂),用于降低非瓣膜性房颤(AF)患者的卒中风险,房颤是最常见的心律失常类型。目前,FDA 仍然认为,按说明使用达比加群具有重要的健康益处,并建议开具达比加群处方的医护人员遵循已批准的药品标签中的建议。房颤患者不应在未咨询医护人员的情况下停止服用达比加群。停止使用血液稀释剂会增加卒中风险。卒中可导致永久性残疾甚至死亡。 达比加群禁用于以下患者:活动性病理性出血;既往有达比加群严重过敏反应史(例如,过敏反应或过敏性休克)。 有关达比加群的更多药物警告(完整)数据(共 14 条),请访问 HSDB 记录页面。 血栓栓塞的临床综合征是由凝血级联反应过度激活引起的。在此过程中,丝氨酸蛋白酶凝血酶发挥着关键作用。因此,人们投入了大量精力来发现安全有效的口服凝血酶抑制剂。基于肽类凝血酶抑制剂 NAPAP 与牛凝血酶复合物的 X 射线晶体结构,我们设计了一类新型的非肽类抑制剂,其以 1,2,5-三取代苯并咪唑为中心骨架。在一系列 X 射线结构分析的支持下,我们优化了这些化合物的活性。尽管结合能主要来源于非极性疏水相互作用,但仍可在低纳摩尔浓度范围内实现凝血酶抑制。为了提高体内效力,我们通过引入羧酸基团增加了分子的整体亲水性。极性很强的化合物 24(BIBR 953/达比加群酯)在体内表现出最佳活性。该两性离子分子被转化为双前药 31(BIBR 1048),该前药在不同动物物种中均显示出强效的口服活性。基于这些结果,我们选择化合物 31 进行临床开发。[1]达比加群酯是一种新型口服直接凝血酶抑制剂,可安全有效地降低房颤患者的卒中风险。目前尚无机械心脏瓣膜置换术后的相关数据。我们利用猪异位主动脉瓣模型检验了达比加群酯在机械瓣膜血栓预防方面与肝素疗效相当的假设。[4] 新型直接凝血酶抑制剂达比加群酯在我们建立的猪模型中对机械心脏瓣膜的短期血栓预防有效。这些动物实验数据为评估达比加群酯作为华法林替代疗法,用于经适当筛选的双叶机械主动脉瓣患者的临床试验提供了进一步的支持。[4] |
| 分子式 |
C25H25N7O3
|
|
|---|---|---|
| 分子量 |
471.51
|
|
| 精确质量 |
471.201
|
|
| 元素分析 |
C, 65.05; H, 6.58; N, 15.62; O, 12.74)
|
|
| CAS号 |
211914-51-1
|
|
| 相关CAS号 |
Dabigatran-d4 hydrochloride;Dabigatran-d3;1246817-44-6;Dabigatran etexilate;211915-06-9;Dabigatran etexilate mesylate;872728-81-9;Dabigatran (ethyl ester);429658-95-7;Dabigatran-d4;1618637-32-3;Dabigatran-13C6;1210608-88-0;Dabigatran-13C,d3
|
|
| PubChem CID |
216210
|
|
| 外观&性状 |
White to light yellow solid powder
|
|
| 密度 |
1.4±0.1 g/cm3
|
|
| 沸点 |
797.1±70.0 °C at 760 mmHg
|
|
| 熔点 |
268-272ºC
|
|
| 闪点 |
435.9±35.7 °C
|
|
| 蒸汽压 |
0.0±2.9 mmHg at 25°C
|
|
| 折射率 |
1.694
|
|
| LogP |
0.79
|
|
| tPSA |
150.22
|
|
| 氢键供体(HBD)数目 |
4
|
|
| 氢键受体(HBA)数目 |
7
|
|
| 可旋转键数目(RBC) |
9
|
|
| 重原子数目 |
35
|
|
| 分子复杂度/Complexity |
757
|
|
| 定义原子立体中心数目 |
0
|
|
| SMILES |
N=C(N)C(C=C1)=CC=C1NCC2=NC3=CC(C(N(CCC(O)=O)C4=NC=CC=C4)=O)=CC=C3N2C
|
|
| InChi Key |
YBSJFWOBGCMAKL-UHFFFAOYSA-N
|
|
| InChi Code |
InChI=1S/C25H25N7O3/c1-31-20-10-7-17(25(35)32(13-11-23(33)34)21-4-2-3-12-28-21)14-19(20)30-22(31)15-29-18-8-5-16(6-9-18)24(26)27/h2-10,12,14,29H,11,13,15H2,1H3,(H3,26,27)(H,33,34)
|
|
| 化学名 |
3-[[2-[(4-carbamimidoylanilino)methyl]-1-methylbenzimidazole-5-carbonyl]-pyridin-2-ylamino]propanoic acid
|
|
| 别名 |
|
|
| HS Tariff Code |
2934.99.9001
|
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
|
|---|
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.1208 mL | 10.6042 mL | 21.2085 mL | |
| 5 mM | 0.4242 mL | 2.1208 mL | 4.2417 mL | |
| 10 mM | 0.2121 mL | 1.0604 mL | 2.1208 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
Study to Gather Information About the Safety of Oral Anticoagulation Drugs and How Well These Drugs Work in Real World for Patients With Non-valvular Atrial Fibrillation (Irregularly Heart Beats Which is Not Caused by a Heart Valve Problem)
CTID: NCT04249401
Phase: Status: Completed
Date: 2024-08-01