| 规格 | 价格 | |
|---|---|---|
| 500mg | ||
| 1g | ||
| Other Sizes |
| 靶点 |
PPAR-α (IC50 = 45 nM); PPAR-δ (IC50 = 175 nM)
|
|---|---|
| 药代性质 (ADME/PK) |
吸收
每日一次给药后,elafibranor及其主要活性代谢物GFT1007分别在7天和14天内达到稳态。稳态时,elafibranor的平均(标准差)Cmax为802 (443) ng/mL,GFT1007的平均(标准差)Cmax为2058 (459) ng/mL。elafibranor的平均(标准差)AUC为3758 (1749) ng·h/mL,GFT1007的平均(标准差)AUC为11985 (7149) ng·h/mL。在PBC患者中,每日一次服用80 mg后,elafibranor和GFT1007的血浆峰浓度时间(Tmax)中位数为1.25小时(范围:0.5-2小时)。与空腹状态相比,与高脂肪高热量餐同服时,elafibranor 的达峰时间 (Tmax) 延迟 30 分钟,GFT1007 的达峰时间延迟 1 小时。进食后,elafibranor 的平均峰浓度 (Cmax) 和曲线下面积 (AUC) 分别下降 50% 和 15%,GFT1007 的平均峰浓度 (Cmax) 下降 30%,但 AUC 与空腹状态相比未受影响。该差异无临床意义。 消除途径 在健康受试者中,单次口服 120 mg(推荐剂量的 1.5 倍)14C 放射性标记的 elafibranor 后,约 77.1% 的剂量从粪便中回收,主要以 elafibranor(占给药剂量的 56.7%)及其主要代谢物 GFT1007(占给药剂量的 6.08%)的形式排出。约19.3%的药物经尿液回收,主要以葡萄糖醛酸苷结合物GFT3351的形式存在(占给药剂量的11.8%)。尿液中仅检测到极少量未代谢的elafibranor或GFT1007。大鼠口服elafibranor后,60%的药物经胆汁排泄,提示elafibranor在人体内可能经胆汁排泄。 分布容积 健康受试者空腹单次服用80 mg elafibranor后,其平均表观分布容积(Vd/F)为4731 L。 清除率 空腹单次服用80 mg elafibranor后,其平均表观总清除率(CL/F)为50.0 L/h。 蛋白结合 Elafibranor 和 GFT1007 与血浆蛋白的结合率约为 99.7%,主要与血清白蛋白结合。 代谢/代谢物 Elafibranor 可广泛代谢生成一种主要活性代谢物 GFT1007,其化学结构尚未明确。稳态下,GFT1007 的平均全身暴露量 (AUC) 是 elafibranor 的 3.2 倍。GFT3351 是一种酰基葡糖醛酸苷结合物,是主要的非活性代谢物,由四种立体异构体组成。体外研究表明,elafibranor 由胞质酶 15-酮前列腺素 13-Δ 还原酶 (PTGR1) 代谢生成 GFT1007。 Elafibranor 也通过 CYP2J2、UGT1A3、UGT1A4 和 UGT2B7 代谢。GFT1007 则进一步通过 CYP2C8、UGT1A3 和 UGT2B7 代谢。 生物半衰期 空腹单次服用 80 mg 后,elafibranor 的中位消除半衰期为 70.2 小时(范围 37.1 至 92.2 小时),主要活性代谢物 GFT1007 的中位消除半衰期为 15.4 小时(范围 9.39 至 21.7 小时)。 |
| 毒性/毒理 (Toxicokinetics/TK) |
肝毒性
在预注册临床试验中,发现elafibranor可降低相当一部分原发性胆汁性胆管炎(PBC)患者的血清转氨酶和碱性磷酸酶水平。在健康志愿者的初步剂量探索研究中,发现ALT和AST水平升高超过正常值上限(ULN)5倍与剂量相关,且在每日剂量超过120 mg的受试者中约有三分之一出现这种情况。相比之下,在每日剂量为80 mg的elafibranor治疗非酒精性脂肪性肝炎(NASH)和PBC患者的临床试验中,仅有1%至2%的患者出现ALT升高超过ULN 5倍的情况,通常发生在治疗的最初几个月内,并在不中断药物治疗、不出现黄疸或其他症状的情况下自行消退。对ALT升高病例的仔细评估得出结论,其中3例可能由药物引起的损伤所致,2例为138例PBC患者中的2例,1例为1433例NASH患者中的1例。在接受elafibranor治疗期间出现肌痛和CPK升高的患者中,一名既往患有肝硬化且同时服用他汀类药物的患者出现了黄疸(5.5 mg/dL),ALT(300 U/L)和AST(828 U/L)升高,同时伴有横纹肌溶解(CPK 12,647 U/L),随后发生肝功能失代偿。elafibranor治疗也可能增加胆结石和胆囊炎的发生率。已知其他PPARα(非诺贝特、苯扎贝特)和PPARγ(吡格列酮、罗格列酮)激动剂也会引起罕见的药物性肝损伤。 可能性评分:E(未经证实但怀疑是临床上明显的肝损伤的罕见原因)。 Elafibranor在II期临床试验中耐受性良好;它不会引起体重增加或心脏事件,但会引起血清肌酐轻微、可逆性升高(与安慰剂相比效应量:4.31 ± 1.19 μmol/L,P<0.001)[2] 与PPARγ激活药物(罗格列酮、阿格列扎)不同,Elafibranor不影响db/db小鼠的心脏重量或增加血浆脂联素浓度[3] 对食蟹猴进行长期(12个月)Elafibranor给药,未显示心脏毒性、血液学异常或骨髓毒性[3] |
| 参考文献 |
|
| 其他信息 |
Elafibranor(代号 GFT505)是一种多模式、多效合一的药物,用于治疗伴或不伴糖尿病的超重患者的致动脉粥样硬化性血脂异常。它是一种口服药物,作用于过氧化物酶体增殖物激活受体 (PPAR) 的三种亚型(PPARα、PPARγ 和 PPARδ),其中对 PPARα 的作用更为显著。截至 2016 年 2 月,Elafibranor 已完成 8 项临床试验,目前正在进行一项 III 期临床试验。
Elafibranor 是一种口服过氧化物酶体增殖物激活受体激动剂,与熊去氧胆酸联合用于治疗原发性胆汁性胆管炎。 Elafibranor 治疗期间罕见出现肝酶升高的情况,但尚未有确凿证据表明其与临床上明显的肝损伤伴黄疸病例相关。 药物适应症 已研究用于治疗动脉粥样硬化和 2 型糖尿病。 治疗原发性胆汁性胆管炎 治疗非酒精性脂肪性肝病 (NAFLD),包括非酒精性脂肪性肝炎 (NASH) 作用机制 GFT505 是一种口服药物,作用于 PPAR 的 3 种亚型(PPARα、PPARγ、PPARδ),优先作用于 PPARα。其作用机制复杂。它能够差异性地募集辅助因子至核受体,进而导致基因表达和生物学效应的差异性调控。因此,识别和分析选择性核受体调节剂 (SNuRMs) 的活性是筛选具有更高疗效和更低副作用的创新候选药物的有效方法。这些多功能分子对肥胖、胰岛素抵抗和糖尿病、动脉粥样硬化、炎症以及脂质三联体(升高高密度脂蛋白胆固醇、降低甘油三酯和低密度脂蛋白胆固醇)均有显著的积极作用。 引言:贝特类药物多年来一直用于治疗血脂异常,并且最近也被证实具有抗炎作用。它们是相对较弱的 PPAR-α 激动剂,并且确实存在一些不良反应。目前正在开发新型化合物,即选择性 PPAR 调节剂 (SPPARMs),它们具有更强的 PPAR-α 激动剂活性。这些药物可能在治疗血脂异常、胰岛素抵抗和非酒精性脂肪性肝病 (NAFLD) 方面具有优势。本文综述重点关注正在研发中的 PPAR-α 激动剂或 SPPARMs,并描述了其临床前研究和早期临床研究。信息来源于已发表的文献和近期会议摘要的检索。正在进行的临床试验则通过 Clinicaltrials.gov 数据库进行检索。专家意见:目前仍需要新的药物来治疗动脉粥样硬化性血脂异常。高效且选择性强的 PPAR-α 激动剂 K-877 已显示出对动脉粥样硬化性血脂异常的有益作用,且避免了贝特类药物的一些不良反应。双重 PPAR-α/PPAR-δ 激动剂 GFT-505 在改善动脉粥样硬化性血脂异常和胰岛素抵抗方面显示出良好的效果,并且似乎是治疗 NAFLD 的潜在候选药物。需要进行长期试验来评估这些新药对心血管和肝脏结局的安全性和有效性。[1] 非酒精性脂肪性肝炎 (NASH) 的特征是肝细胞脂肪变性并伴有肝脏炎症。尽管其发病率已达全球大流行水平,但目前尚无抗 NASH 药物获批。部分原因是由于缺乏评估潜在候选药物疗效的有效工具,导致药物研发进程放缓。本研究描述了利用源自人皮肤前体的肝细胞构建和应用一种新的 NASH 临床前模型。将这些细胞暴露于脂肪生成因子(胰岛素、葡萄糖、脂肪酸)和促炎因子(IL-1β、TNF-α、TGF-β)后,产生了典型的非酒精性脂肪性肝炎(NASH)反应,表现为细胞内脂质积累、NASH特异性基因表达调控、caspase-3/7活性增强以及炎症标志物(包括CCL2、CCL5、CCL7、CCL8、CXCL5、CXCL8、IL-1α、IL-6和IL-11)的表达和/或分泌。转录组学分析验证了所提出的NASH模型的人体相关性,结果显示体外系统与NASH患者之间存在共同调控的基因以及相同的基因类别。通过测试elafibranor(一种目前正在进行III期临床试验的有前景的抗NASH化合物),证明了该体外模型的应用潜力。 Elafibranor 在体外可减轻 NASH 的关键特征,并显著降低脂质负荷以及炎症趋化因子的表达和分泌,这些炎症趋化因子在体内负责募集免疫细胞。这种炎症反应的降低是由 NFκB 介导的。总之,这种与人体相关的体外系统被证明是研究新型抗NASH化合物的灵敏测试工具。[4] Elafibranor (GFT505) 是一种双重PPAR-α/δ激动剂,也是一种靶向肝脏的在研药物。[1][3] 目前正在进行III期临床试验,用于治疗非酒精性脂肪性肝炎 (NASH)。[4] Elafibranor在2型糖尿病模型中具有抗糖尿病作用,并能改善动脉粥样硬化性血脂异常和胰岛素抵抗,使其成为治疗NAFLD/NASH的潜在候选药物。[1][3] 其作用机制涉及调节脂质代谢、葡萄糖稳态和炎症,其抗炎作用是通过抑制NFκB通路实现的。[2][3][4] 在临床试验中,Elafibranor 120 mg/d 显示出疗效优于 80 mg/d;在按意向治疗人群中未达到预设的主要终点,但事后分析表明,在特定患者亚组中具有显著获益[2] 药效学 Elafibranor 抑制胆汁酸合成。研究还表明,它能改善胰岛素敏感性、葡萄糖稳态和脂质代谢。在原发性胆汁性胆管炎 (PBC) 患者中,elafibranor 降低了碱性磷酸酶 (ALP) 的平均水平。体外 PPAR 功能测定显示,elafibranor 和 GFT1007 均能激活 PPARα(EC50 分别为 46 nM 和 14 nM,Emax 分别为 56% 和 61%,相对于参考激动剂)。 elafibranor 和 GFT1007 对 PPAR-α 的激活效力比它们各自对 PPAR-γ 和 PPAR-δ 的激活效力高约 3 至 8 倍。 Elafibranor 是一种过氧化物酶体增殖物激活受体 (PPAR) α 和 β/δ 双重激动剂,其作用机制是抑制胆汁酸合成。2024 年 6 月 10 日,Elafibranor 获得 FDA 加速批准,用于治疗原发性胆汁性胆管炎 (PBC)。该药物也于 2024 年 9 月 23 日获得 EMA 批准。 Elafibranor 是一种过氧化物酶体增殖物激活受体激动剂。 elafibranor 的作用机制是作为过氧化物酶体增殖物激活受体激动剂和细胞色素 P450 3A4 诱导剂。 Elafibranor 是一种口服生物利用度高的过氧化物酶体增殖物激活受体 (PPAR)-α (PPARα) 和 -δ (PPARδ) 激动剂,具有降低胆汁酸活性。口服后,elafibranor 及其主要活性代谢物 GFT1007 可靶向、结合并激活肝脏中的 PPARα 和 PPARδ。这会诱导成纤维细胞生长因子 21 (FGF21) 的表达,并下调 CYP7A1(一种负责胆固醇合成胆汁酸的关键酶)。通过降低 CYP7A1 的表达,胆汁酸的合成得以减少。这可降低胆汁毒性,并减少与原发性胆汁性胆管炎 (PBC) 相关的炎症和瘢痕形成。 ELAFIBRANOR 是一种小分子药物,其临床试验阶段最高为 IV 期(涵盖所有适应症),于 2024 年首次获批,适用于胆管炎,并有 6 个在研适应症。 |
| 分子式 |
C22H24O4S
|
|---|---|
| 分子量 |
384.49
|
| 精确质量 |
384.139
|
| 元素分析 |
C, 68.73; H, 6.29; O, 16.64; S, 8.34
|
| CAS号 |
824932-88-9
|
| 相关CAS号 |
Elafibranor;923978-27-2
|
| 外观&性状 |
Typically exists as solids at room temperature
|
| 密度 |
1.2±0.1 g/cm3
|
| 沸点 |
569.0±50.0 °C at 760 mmHg
|
| 闪点 |
297.9±30.1 °C
|
| 蒸汽压 |
0.0±1.6 mmHg at 25°C
|
| 折射率 |
1.606
|
| LogP |
5.63
|
| tPSA |
88.9
|
| SMILES |
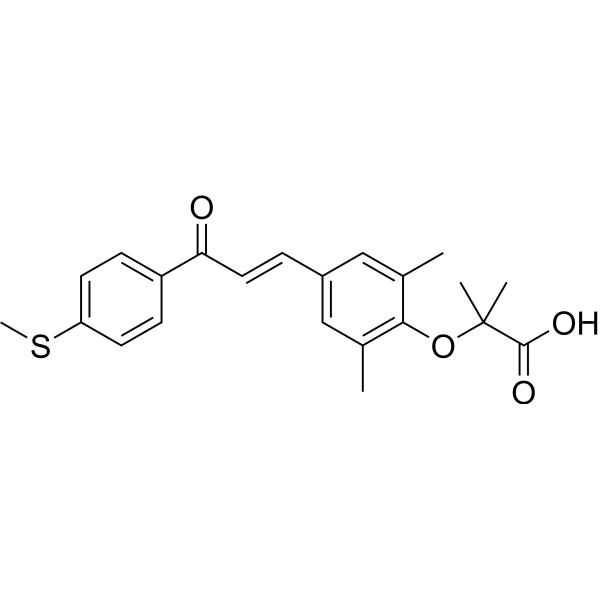
CC1=CC(=CC(=C1OC(C)(C)C(=O)O)C)C=CC(=O)C2=CC=C(C=C2)SC
|
| 别名 |
(E/Z)-GFT505; (E/Z)-Elafibranor
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples
|
|---|---|
| 溶解度 (体内实验) |
注意: 如下所列的是一些常用的体内动物实验溶解配方,主要用于溶解难溶或不溶于水的产品(水溶度<1 mg/mL)。 建议您先取少量样品进行尝试,如该配方可行,再根据实验需求增加样品量。
注射用配方
注射用配方1: DMSO : Tween 80: Saline = 10 : 5 : 85 (如: 100 μL DMSO → 50 μL Tween 80 → 850 μL Saline)(IP/IV/IM/SC等) *生理盐水/Saline的制备:将0.9g氯化钠/NaCl溶解在100 mL ddH ₂ O中,得到澄清溶液。 注射用配方 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (如: 100 μL DMSO → 400 μL PEG300 → 50 μL Tween 80 → 450 μL Saline) 注射用配方 3: DMSO : Corn oil = 10 : 90 (如: 100 μL DMSO → 900 μL Corn oil) 示例: 以注射用配方 3 (DMSO : Corn oil = 10 : 90) 为例说明, 如果要配制 1 mL 2.5 mg/mL的工作液, 您可以取 100 μL 25 mg/mL 澄清的 DMSO 储备液,加到 900 μL Corn oil/玉米油中, 混合均匀。 View More
注射用配方 4: DMSO : 20% SBE-β-CD in Saline = 10 : 90 [如:100 μL DMSO → 900 μL (20% SBE-β-CD in Saline)] 口服配方
口服配方 1: 悬浮于0.5% CMC Na (羧甲基纤维素钠) 口服配方 2: 悬浮于0.5% Carboxymethyl cellulose (羧甲基纤维素) 示例: 以口服配方 1 (悬浮于 0.5% CMC Na)为例说明, 如果要配制 100 mL 2.5 mg/mL 的工作液, 您可以先取0.5g CMC Na并将其溶解于100mL ddH2O中,得到0.5%CMC-Na澄清溶液;然后将250 mg待测化合物加到100 mL前述 0.5%CMC Na溶液中,得到悬浮液。 View More
口服配方 3: 溶解于 PEG400 (聚乙二醇400) 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.6008 mL | 13.0042 mL | 26.0085 mL | |
| 5 mM | 0.5202 mL | 2.6008 mL | 5.2017 mL | |
| 10 mM | 0.2601 mL | 1.3004 mL | 2.6008 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
Study to Compare the Level of Elafibranor in Blood After Repeat Administration in Japanese and Non-Asian Healthy Participants
CTID: NCT05543369
Phase: Phase 1 Status: Completed
Date: 2023-07-18