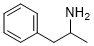
| 规格 | 价格 | |
|---|---|---|
| 500mg | ||
| 1g | ||
| Other Sizes |
| 药代性质 (ADME/PK) |
吸收、分布和排泄
安非他明在肠道中吸收良好。由于其为弱碱性物质,因此环境碱性越强,药物以脂溶性形式存在的比例越高,通过富含脂质的细胞膜的吸收也越容易。口服安非他明后1-3小时达到血药浓度峰值,注射后约15分钟达到血药浓度峰值,生物利用度超过75%。安非他明通常在4-6小时后完全吸收。 安非他明主要通过尿液排出,约40%的排泄剂量以原形安非他明的形式存在于尿液中。口服安非他明后3天内,约90%的给药剂量被排出体外。安非他明的消除速率高度依赖于尿液pH值,酸性pH值会促进安非他明的排泄,而碱性pH值则会降低其排泄。 据报道,安非他明的分布容积高达4 L/kg。 正常清除率为0.7 L/h/kg。肾功能不全患者的清除率显著降低,可达0.4 L/h/kg。 儿童:儿童清除安非他明的速度比成人快。 /乳汁/ 安非他明会分泌到人乳中。 安非他明易于从胃肠道吸收,其作用可持续4-24小时。安非他明分布于大多数身体组织,在大脑和脑脊液中浓度较高。口服后约3小时,尿液中即可检测到安非他明。苯丙胺的尿排泄受pH值影响,酸性尿液中排泄增加。口服消旋苯丙胺后,在最初12小时内,两种异构体的排泄量大致相等;12小时后,d-异构体的排泄比例持续下降。 已在人体汗液中测得苯丙胺的含量,中位数范围为每片15.5 ng(低剂量6.5-40.5 ng)和53.8 ng(高剂量34.0-83.4 ng)(1)。 有关苯丙胺(共7种)的更多吸收、分布和排泄(完整)数据,请访问HSDB记录页面。 代谢/代谢物 已知苯丙胺在CYP2D6的作用下经肝脏代谢。苯丙胺的代谢途径主要包括芳香族羟基化、脂肪族羟基化和N-去烷基化。该途径产生的代谢产物包括4-羟基苯丙胺、4-羟基去甲麻黄碱、马尿酸、苯甲酸、苄基甲基酮和对羟基苯丙胺(一种强效致幻剂)。然而,相当一部分原药保持不变。苯丙胺在肝脏中通过芳香族羟基化、N-去烷基化和脱氨作用进行代谢。尽管参与苯丙胺代谢的酶尚未完全明确,但已知细胞色素P450 (CYP-450) 2D6参与4-羟基苯丙胺的生成。由于CYP2D6具有遗传多态性,因此苯丙胺代谢可能存在人群差异。 苯丙胺的代谢途径包括芳香族羟基化、脂肪族羟基化和N-去烷基化,这些途径可产生活性代谢物,例如强效致幻剂对羟基苯丙胺。其他代谢途径,包括脱氨和随后的侧链氧化,则产生无活性的苯丙胺衍生物。 苯丙胺是芬普瑞克斯(Fenproporex)的已知人体代谢物。 肝脏 半衰期:10小时 生物半衰期 苯丙胺的半衰期高度依赖于其异构体。据报道,右旋苯丙胺的半衰期约为9-11小时,而左旋苯丙胺的半衰期约为11-14小时。尿液pH值会影响这一药代动力学参数,酸性尿液的半衰期为7小时,碱性尿液的半衰期为34小时。 成人生物半衰期为10-13小时,儿童为9-11小时。 |
|---|---|
| 毒性/毒理 (Toxicokinetics/TK) |
毒性概述
识别和用途:安非他明是一种无色液体,具有特征性的胺类气味(类似于天竺葵叶)和辛辣味。其适应症如下:精神兴奋剂:认可的适应症:发作性睡病;儿童多动症(作为心理、教育和社会干预措施的辅助手段)。该药物常被滥用以提高运动表现。口服或注射滥用极为常见。人体暴露和毒性:主要风险包括:急性中枢神经系统 (CNS) 兴奋、心脏毒性(可导致心动过速、心律失常、高血压和心血管衰竭)。具有高度依赖性和滥用风险。心血管效应包括:心悸、胸痛、心动过速、心律失常和高血压;严重中毒可导致心血管衰竭,以及心肌缺血、梗死和心室功能障碍。中枢神经系统效应包括:中枢神经系统兴奋、震颤、躁动不安、焦虑、失眠、运动增多、头痛、抽搐、昏迷和反射亢进。曾观察到中风和脑血管炎。胃肠道效应包括:呕吐、腹泻和痉挛。长期滥用甲基苯丙胺可导致急性短暂性缺血性结肠炎。泌尿生殖系统效应:膀胱括约肌张力增高可能导致排尿困难、排尿踌躇和急性尿潴留。脱水或横纹肌溶解可继发肾功能衰竭。可能出现肾缺血。可能出现短暂性高甲状腺素血症。代谢和肌肉活动增强可能导致过度通气和体温过高。长期使用常出现体重减轻。曾有低钾血症和高钾血症的报道。脱水常见。可能出现肌束颤动和肌强直。横纹肌溶解症是严重安非他明中毒的重要后果。典型的症状包括躁动、意识混乱、情绪高涨、觉醒度增加、话多、易怒和惊恐发作。长期滥用可导致妄想和偏执。长期使用后突然停药会出现戒断综合征。安非他明似乎主要或全部作用于中枢神经系统,通过促使神经末梢储存部位释放生物胺,尤其是去甲肾上腺素和多巴胺。它还可能通过抑制单胺氧化酶来减缓儿茶酚胺的代谢。儿童似乎比成人更容易受到影响,且不太可能产生耐受性。出于医疗目的使用安非他明不会对胎儿造成先天性畸形的显著风险。安非他明通常不被认为是人类致畸剂。新生儿可能会出现轻微的戒断症状,但少数针对婴儿的随访研究并未发现长期后遗症。孕妇非法使用或滥用安非他明会对胎儿和新生儿构成重大风险,包括宫内生长迟缓、早产以及增加母婴发病率的可能性。然而,宫内暴露于安非他明的新生儿所发生的脑损伤似乎与安非他明的血管收缩特性直接相关。一项研究调查了65名母亲在孕期(至少在孕早期)对安非他明成瘾的儿童。这些儿童在八岁时智力、心理功能、生长发育和身体健康状况均在正常范围内,但那些在整个孕期都暴露于安非他明的儿童往往更具攻击性。动物研究:视网膜毒性测试结果为阴性;每天给狗服用10 mg/kg,持续三个月,偶尔会出现轻微的眼底苍白,但未观察到视网膜组织学改变。一项研究调查了17只成年猫服用右旋安非他明后的行为效应。皮下注射安非他明的剂量分别为0.1、0.5、1.0和5.0 mg/kg。安非他明给药可引起剂量依赖性的活动减少,且高剂量组活动减少更为显著。此外,在安非他明处理的猫中观察到刻板行为模式,如头部节律性双侧缓慢运动、对环境漠不关心以及呼吸频率剂量依赖性增加。安非他明可损伤实验动物模型的脑动脉。生态毒性研究:在淡水双壳类动物斑马贻贝(Dreissena polymorpha)中,最高测试浓度(5000 ng/L)的安非他明处理下抗氧化剂呈钟形变化趋势,提示活性氧过度产生,导致氧化损伤,蛋白质羰基化和DNA片段化的显著增加证实了这一点。安非他明可刺激中枢肾上腺素能受体释放去甲肾上腺素。高剂量时,苯丙胺会促使中脑皮层边缘系统和黑质纹状体多巴胺系统释放多巴胺。苯丙胺也可能直接激动中枢5-羟色胺(5-HT)受体,并抑制单胺氧化酶(MAO)。在外周,苯丙胺被认为通过作用于肾上腺素能神经末梢以及α和β受体,促进去甲肾上腺素的释放。对血清素能通路的调节可能有助于其镇静作用。该药物与VMAT酶相互作用,增强囊泡中多巴胺(DA)和5-HT的释放。它还可能直接导致DAT和SERT的逆转。 毒性数据 LD50:180 mg/kg(皮下注射,大鼠)(A308) 相互作用 苯丙胺抑制藜芦生物碱的降压作用。 丙氧芬过量时,苯丙胺的中枢神经系统兴奋作用增强,可能导致致命性惊厥。 苯丙胺可能延缓苯妥英的肠道吸收;与苯妥英合用可能产生协同抗惊厥作用。 苯丙胺可能延缓苯巴比妥的肠道吸收。与苯巴比妥合用可能产生协同抗惊厥作用。 有关安非他明(共24项)的更多相互作用(完整)数据,请访问HSDB记录页面。 非人类毒性值 大鼠腹腔注射LD50:125 mg/kg 大鼠皮下注射LD50:39 mg/kg 小鼠口服LD50:22 mg/kg 小鼠腹腔注射LD50:16 mg/kg 有关安非他明(共6项)的更多非人类毒性值(完整)数据,请访问HSDB记录页面。 |
| 其他信息 |
治疗用途
肾上腺素能药物;肾上腺素能再摄取抑制剂;中枢神经系统兴奋剂;多巴胺能药物;多巴胺再摄取抑制剂;拟交感神经药 /临床试验/ ClinicalTrials.gov 是一个注册库和结果数据库,收录了全球范围内由公共和私人机构资助的人体临床研究。该网站由美国国家医学图书馆 (NLM) 和美国国立卫生研究院 (NIH) 维护。ClinicalTrials.gov 上的每条记录都提供了研究方案的概要信息,包括:疾病或病症;干预措施(例如,正在研究的医疗产品、行为或程序);研究的标题、描述和设计;参与要求(资格标准);研究开展地点;研究地点的联系方式;并提供其他健康网站的相关信息链接,例如美国国家医学图书馆 (NLM) 的 MedlinePlus(用于患者健康信息)和 PubMed(用于医学领域学术文章的引文和摘要)。数据库中包含安非他明。 Evekeo(硫酸安非他明片,USP)适用于:1. 发作性睡病;2. 注意力缺陷多动障碍,作为综合治疗方案的一部分,该方案通常包括其他补救措施(心理、教育、社会),以稳定儿童的行为综合征。该综合征的特征是存在以下一组发育不协调的症状:中度至重度注意力分散、注意力持续时间短、多动、情绪不稳定和冲动。如果这些症状出现时间相对较短,则不应最终确诊该综合征。非定位性(软性)神经系统体征、学习障碍和脑电图异常可能存在也可能不存在,因此可能需要也可能不需要诊断中枢神经系统功能障碍。 3. 外源性肥胖症:作为短期(几周)辅助疗法,用于基于热量限制的减重方案,适用于对其他疗法(例如反复节食、团体项目和其他药物)无效的患者。/美国产品标签包含/ 兽医:用于缓解麻醉剂过量,特别是巴比妥类药物过量。增强对外部刺激的反应,例如奶牛的抑郁状态和产后低血钙症。可能对某些脑脊髓炎(马)、癫痫(牛)或多动症病例有效。 药物警告 /黑框警告/ 安非他明具有很高的滥用潜力。长期服用安非他明可能导致药物依赖,必须避免。应特别注意患者可能获得安非他明用于非治疗用途或分发给他人,并且应谨慎处方或配药。滥用安非他明可能导致猝死和严重的心血管不良事件。 安非他明会分泌到乳汁中,其浓度可达母体血液浓度的3-7倍。应决定是停止哺乳还是停止用药。 只有当潜在益处大于对胎儿的潜在风险时,才可在孕期使用安非他明。孕期使用安非他明的潜在益处是否大于潜在风险尚存疑问。依赖安非他明的女性所生的婴儿早产、低出生体重和戒断症状(例如,烦躁不安、疲倦乏力、躁动)的风险增加。 安非他明的不良反应可能包括:紧张、失眠、易怒、话多、性欲改变、头晕、头痛、活动增多、畏寒、面色苍白或潮红、视力模糊、瞳孔散大和过度兴奋。服用安非他明的患者曾报告出现运动或发声抽动加重、图雷特综合征、运动障碍、癫痫发作、欣快感、烦躁不安、情绪不稳和阳痿等症状。服用推荐剂量安非他明的患者极少出现精神病发作。 有关安非他明(共21条)的更多药物警告(完整)数据,请访问HSDB记录页面。 药效学 根据其作用机制,已证实安非他明以剂量和时间依赖的方式增加前额叶皮层中去甲肾上腺素和纹状体中多巴胺的浓度。已知包括肾上腺素在内的神经递质的无序释放会产生心血管副作用。早期报告显示,服用安非他明可增强认知能力,并有智力测试分数提高的报道。在注意力缺陷多动障碍(ADHD)的治疗中,安非他明已被证实能显著改善患者的学习成绩、行为和举止。研究表明,安非他明的消旋体和外消旋体均能产生这种效果,而且至今为止,3:1(D:L)的消旋体仍然非常普遍。安非他明对血清素的治疗作用似乎对ADHD没有显著的临床疗效,这与安非他明和芬氟拉明(一种强效的血清素释放因子)的对比研究结果一致。然而,安非他明对血清素的间接影响可能对ADHD患者的抑郁和焦虑症状产生影响。针对安非他明非法使用的研究,特别是针对重度使用者的研究,证实了安非他明会引发妄想状态,这表明该药物具有精神危险性。抑郁症患者滥用安非他明的案例也印证了这一观点。 |
| 分子式 |
C9H13N
|
|---|---|
| 分子量 |
135.20622
|
| 精确质量 |
135.104
|
| CAS号 |
300-62-9
|
| 相关CAS号 |
60-13-9 (sulfate); 300-62-9; 2706-50-5 (HCl);
|
| PubChem CID |
3007
|
| 外观&性状 |
Mobile liquid
Colorless, volatile liquid |
| LogP |
1.8
|
| tPSA |
26
|
| 氢键供体(HBD)数目 |
1
|
| 氢键受体(HBA)数目 |
1
|
| 可旋转键数目(RBC) |
2
|
| 重原子数目 |
10
|
| 分子复杂度/Complexity |
84.7
|
| 定义原子立体中心数目 |
0
|
| InChi Key |
KWTSXDURSIMDCE-UHFFFAOYSA-N
|
| InChi Code |
InChI=1S/C9H13N/c1-8(10)7-9-5-3-2-4-6-9/h2-6,8H,7,10H2,1H3
|
| 化学名 |
alpha-Methylphenethylamine
|
| 别名 |
Amphetamine NSC-27159 NSC27159 NSC 27159
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples
|
|---|---|
| 溶解度 (体内实验) |
注意: 如下所列的是一些常用的体内动物实验溶解配方,主要用于溶解难溶或不溶于水的产品(水溶度<1 mg/mL)。 建议您先取少量样品进行尝试,如该配方可行,再根据实验需求增加样品量。
注射用配方
注射用配方1: DMSO : Tween 80: Saline = 10 : 5 : 85 (如: 100 μL DMSO → 50 μL Tween 80 → 850 μL Saline)(IP/IV/IM/SC等) *生理盐水/Saline的制备:将0.9g氯化钠/NaCl溶解在100 mL ddH ₂ O中,得到澄清溶液。 注射用配方 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (如: 100 μL DMSO → 400 μL PEG300 → 50 μL Tween 80 → 450 μL Saline) 注射用配方 3: DMSO : Corn oil = 10 : 90 (如: 100 μL DMSO → 900 μL Corn oil) 示例: 以注射用配方 3 (DMSO : Corn oil = 10 : 90) 为例说明, 如果要配制 1 mL 2.5 mg/mL的工作液, 您可以取 100 μL 25 mg/mL 澄清的 DMSO 储备液,加到 900 μL Corn oil/玉米油中, 混合均匀。 View More
注射用配方 4: DMSO : 20% SBE-β-CD in Saline = 10 : 90 [如:100 μL DMSO → 900 μL (20% SBE-β-CD in Saline)] 口服配方
口服配方 1: 悬浮于0.5% CMC Na (羧甲基纤维素钠) 口服配方 2: 悬浮于0.5% Carboxymethyl cellulose (羧甲基纤维素) 示例: 以口服配方 1 (悬浮于 0.5% CMC Na)为例说明, 如果要配制 100 mL 2.5 mg/mL 的工作液, 您可以先取0.5g CMC Na并将其溶解于100mL ddH2O中,得到0.5%CMC-Na澄清溶液;然后将250 mg待测化合物加到100 mL前述 0.5%CMC Na溶液中,得到悬浮液。 View More
口服配方 3: 溶解于 PEG400 (聚乙二醇400) 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 7.3959 mL | 36.9795 mL | 73.9590 mL | |
| 5 mM | 1.4792 mL | 7.3959 mL | 14.7918 mL | |
| 10 mM | 0.7396 mL | 3.6980 mL | 7.3959 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。