| 规格 | 价格 | |
|---|---|---|
| 500mg | ||
| 1g | ||
| Other Sizes |

| 靶点 |
Topoisomerase II; Topoisomerase IV
|
|---|---|
| 体外研究 (In Vitro) |
体外活性:莫西沙星通过捕获 DNA 药物酶复合物并特异性抑制 ATP 依赖性酶拓扑异构酶 II(DNA 旋转酶)和拓扑异构酶 IV 发挥作用。莫西沙星对结核分枝杆菌 H37Rv 具有体外效力,MIC 为 0.177 μg/mL。莫西沙星具有广泛的革兰氏阳性和革兰氏阴性活性。莫西沙星在体外和临床上显示出对抗金黄色葡萄球菌、肺炎链球菌、链球菌的功效。化脓性杆菌、流感嗜血杆菌、副流感嗜血杆菌、肺炎克雷伯菌、卡他莫拉菌、肺炎衣原体和肺炎支原体。除结核分枝杆菌外,莫西沙星还具有抗分枝杆菌活性;莫西沙星对堪萨斯分枝杆菌的活性比鸟分枝杆菌复合群的活性更高:特别是在 4、2 和 2 μg/mL 时,对鸟分枝杆菌 > 胞内分枝杆菌 > 堪萨斯分枝杆菌的 MIC90 分别为 4、2 和 2 μg/mL。龟分枝杆菌 > 偶然分枝杆菌的 MIC90 分别为 16 和 0.5 μg/mL。细胞分析:莫西沙星(盐酸盐)是一种合成的氟喹诺酮抗生素。抗菌莫西沙星是一种广谱氟喹诺酮类药物,与旧的氟喹诺酮类药物相比,它提高了对革兰氏阳性球菌和非典型病原体的覆盖率,同时保留了良好的抗革兰氏阴性菌活性。莫西沙星的抗菌谱包括所有主要的上呼吸道和下呼吸道病原体;它是对抗肺炎球菌(包括青霉素和大环内酯耐药菌株)最有效的氟喹诺酮类药物之一。莫西沙星的光毒性潜力有限。在临床试验中,莫西沙星的临床成功率为88-97%,细菌根除率为90-97%。莫西沙星是一种安全有效的抗菌药物,可用于治疗急性鼻窦炎、慢性支气管炎急性细菌性恶化和社区获得性肺炎。莫西沙星可能刺激脂质过氧化并增强吞噬作用,如 MDA 产生和生存延长所示,而无毒性(如白细胞计数所示)。临床适应症:腹腔脓肿;急性支气管炎;急性鼻窦炎;细菌感染 毒性:过量的症状包括中枢神经系统和胃肠道影响,例如活动减少、嗜睡、震颤、抽搐、呕吐和腹泻。
1. 对革兰氏阳性菌的抗菌活性: - 抑制90%的金黄色葡萄球菌(MSSA/MRSA,甲氧西林耐药株)菌株,MIC₉₀ = 0.5–1 μg/mL;与β-内酰胺类无交叉耐药。时间杀菌曲线显示浓度依赖性杀菌作用:4×MIC浓度下24小时内细菌计数减少>3 log₁₀ CFU/mL [2] 2. 抗结核活性: - 对药物敏感结核分枝杆菌(H37Rv):MIC₅₀ = 0.125 μg/mL,MIC₉₀ = 0.25 μg/mL;对异烟肼耐药株:MIC₉₀ = 0.5 μg/mL;对利福平耐药株:MIC₉₀ = 0.25 μg/mL [5] - 抑制结核分枝杆菌生物膜形成:2×MIC浓度下7天孵育后生物膜 biomass 减少60% [4] 3. 对革兰氏阴性菌的抗菌活性: - 对大肠杆菌(ATCC 25922):MIC = 0.06 μg/mL;对肺炎克雷伯菌:MIC₉₀ = 0.125 μg/mL。对产β-内酰胺酶菌株(如ESBLs)仍保留活性,MIC₉₀ ≤ 1 μg/mL [2] 4. 作用机制验证: - 0.5 μg/mL浓度下细菌DNA超螺旋活性降低50%(DNA旋转酶实验);抑制拓扑异构酶IV介导的DNA松弛作用,IC₅₀ = 0.3 μg/mL [3] |
| 体内研究 (In Vivo) |
在模拟人类疾病的小鼠模型中,与异烟肼 (INH)/RIF/PZA 方案相比,莫西沙星联合 RIF/吡嗪酰胺 (PZA) 的治疗时间最多可缩短 2 个月。每周两次使用 RIF/莫西沙星/PZA 治疗的小鼠在 4 个月后达到了类似的稳定治愈结果,而每天使用 RIF/INH/PZA 治疗则在 6 个月内治愈。 100 mg/kg 莫西沙星在小鼠体内的活性与 INH 相当;将小鼠莫西沙星剂量增加至每天 400 mg/kg 导致脾脏 CFU 计数低于 INH 25 mg/kg,但差异不具有统计学意义。 AUC/MIC 比值与氟喹诺酮类药物在小鼠结核病模型中的体内疗效最相关。
1. 小鼠结核模型中的抗结核疗效: - BALB/c雌性小鼠通过气溶胶感染结核分枝杆菌(H37Rv,100 CFU/肺),口服给予莫西沙星(10、20或40 mg/kg/天),连续4周。40 mg/kg/天剂量下,肺组织细菌计数(log₁₀ CFU/g)从溶剂组的6.8降至3.2;脾组织计数从5.5降至2.1。在清除持留菌方面,疗效优于异烟肼(25 mg/kg/天)[5] 2. 金黄色葡萄球菌败血症模型中的疗效: - C57BL/6雄性小鼠腹腔注射耐甲氧西林金黄色葡萄球菌(MRSA,10⁷ CFU/只),静脉给予莫西沙星(20 mg/kg,每12小时一次),连续3天。生存率从溶剂组的20%提升至80%;48小时后血中细菌计数低于检测限(<10 CFU/mL)[2] 3. 药代动力学-药效学(PK-PD)相关性: - 大鼠肺炎模型(肺炎克雷伯菌感染)中,AUC₀–24h/MIC(24小时药时曲线下面积与MIC的比值)≥30时,肺组织细菌清除率达90% [3] |
| 酶活实验 |
1. DNA旋转酶抑制实验:
将纯化的大肠杆菌DNA旋转酶(亚基A/B,各0.5 μM)与超螺旋pBR322 DNA(0.5 μg)、莫西沙星(0.01–10 μg/mL)在反应缓冲液(50 mM Tris-HCl、20 mM KCl、10 mM MgCl₂)中混合。37°C孵育30分钟后,加入SDS(终浓度0.5%)终止反应。通过1%琼脂糖凝胶电泳分离DNA,密度法定量超螺旋DNA条带。三次重复实验计算IC₅₀(抑制50%超螺旋活性的浓度)[3]
2. 拓扑异构酶IV抑制实验: 将纯化的金黄色葡萄球菌拓扑异构酶IV(亚基A/B,各0.3 μM)与松弛态pBR322 DNA(0.5 μg)、莫西沙星(0.05–5 μg/mL)在缓冲液(40 mM Tris-HCl、100 mM KCl、5 mM MgCl₂)中37°C孵育45分钟。加入EDTA(终浓度10 mM)终止反应,溴化乙锭染色DNA。定量松弛态DNA条带,确定抑制DNA松弛作用的IC₅₀ [2] 抗生素药物多西沙星(盐酸盐)是一种合成的氟喹诺酮类药物。与早期的氟喹诺酮类药物相比,抗菌多西沙星(一种广谱氟喹诺酮类药物)对革兰氏阳性球菌和非典型病原体具有更好的覆盖率,同时保持良好的抗革兰氏阴性菌活性。所有常见的上呼吸道和下呼吸道病原体都包含在莫西沙星的抗菌谱中,使其成为对抗肺炎球菌(包括对大环内酯类和青霉素耐药的菌株)最有效的氟喹诺酮类药物之一。莫西沙星的光毒性潜力是有限的。在临床试验中,莫西沙星的细菌根除率为 90-97%,临床成功率为 88-97%。莫西沙星是一种抗菌药物,可安全有效地治疗社区获得性肺炎、慢性支气管炎的急性细菌性恶化和急性鼻窦炎。 MDA 的产生和生存的延长表明,莫维沙星可以促进脂质过氧化并改善吞噬作用,而白细胞计数表明没有毒性。临床建议:急性鼻窦炎、细菌感染、急性支气管炎和腹部脓肿毒性中枢神经系统和胃肠道副作用,如活动减少、嗜睡、颤抖、抽搐、呕吐和腹泻,是服用过量的迹象。在大鼠和小鼠中,最小静脉注射致死剂量为 100 mg/kg。 |
| 细胞实验 |
1. MIC测定(肉汤微量稀释法):
将细菌(结核分枝杆菌、金黄色葡萄球菌或肺炎克雷伯菌)调整至5×10⁵ CFU/mL(快生长菌)或1×10⁴ CFU/mL(结核分枝杆菌),接种于Mueller-Hinton肉汤(MHB)或Middlebrook 7H9肉汤。在96孔板中对莫西沙星进行倍比稀释(0.001–64 μg/mL),然后接种细菌。37°C孵育(快生长菌24小时,结核分枝杆菌7天),MIC定义为无可见细菌生长的最低浓度 [2,5]
2. 时间杀菌曲线实验: 将金黄色葡萄球菌(MRSA,1×10⁶ CFU/mL)与莫西沙星(0.5×、1×、2×、4× MIC)在MHB中37°C孵育。分别在0、4、8、12、24小时取样,倍比稀释后接种于MHB琼脂,孵育24小时计数菌落形成单位(CFU/mL)。杀菌活性定义为较0时刻CFU/mL减少≥3 log₁₀ [2] 3. 生物膜抑制实验: 结核分枝杆菌在含10% OADC补充剂的Middlebrook 7H9肉汤中接种于24孔板(1×10⁵ CFU/孔),加入莫西沙星(0.125–2 μg/mL),37°C孵育7天。用0.1%结晶紫染色生物膜,乙醇溶解后在595 nm处测吸光度,计算相对于溶剂对照组的抑制率 [4] |
| 动物实验 |
144只雄性Wistar白鼠(18-22周龄;300-400克)感染嗜麦芽窄食单胞菌
12 mg/kg 静脉注射;每日一次、两次、三次;持续7天 为了研究莫西沙星对免疫抑制大鼠因嗜麦芽窄食单胞菌引起的软组织感染的存活率、脂质过氧化和炎症的影响,将144只雄性Wistar白鼠随机分为六组:A组和B组分别每日一次注射生理盐水或莫西沙星;C组和D组分别每日两次注射生理盐水或莫西沙星;E组和F组分别每日三次注射生理盐水或莫西沙星。分别于感染嗜麦芽窄食单胞菌后6小时和30小时采集血样。本研究评估了丙二醛(MDA)水平、白细胞计数、细菌组织过度生长、血清莫西沙星浓度以及生存率。生存分析表明,每8小时给予莫西沙星治疗组的生存期显著长于其他任何组。细菌感染30小时后,组织培养结果显示,莫西沙星治疗组动物脾脏和肺脏中的细菌过度生长显著低于生理盐水治疗组,但肝脏中的细菌过度生长无显著差异。感染6小时后,各组间无统计学差异。然而,感染30小时后,D组的MDA浓度显著高于C组(P = 0.044),白细胞计数显著低于C组(P = 0.026)。其他组间未观察到统计学差异。莫西沙星可能通过刺激脂质过氧化和增强吞噬作用来发挥作用,这可由MDA生成和生存期延长来证实;而白细胞计数显示其无毒性作用。因此,在适当条件下,莫西沙星可用于治疗免疫抑制患者的感染以及由嗜麦芽窄食单胞菌引起的感染。[2] 1. 小鼠结核病模型: - 感染:使用亨德森装置,通过气溶胶感染6-8周龄雌性BALB/c小鼠(H37Rv),目标感染量为100 CFU/肺。 - 给药:将莫西沙星悬浮于0.5%甲基纤维素溶液中;每日一次口服给药(10、20、40 mg/kg/天),持续4周(溶剂:0.5%甲基纤维素)。 - 取样:治疗结束后,处死小鼠;将肺和脾脏匀浆,进行系列稀释,并接种于Middlebrook 7H11琼脂平板上。在37°C培养21天后进行菌落计数[5] 2. 小鼠耐甲氧西林金黄色葡萄球菌(MRSA)脓毒症模型: - 感染:将金黄色葡萄球菌(MRSA,10⁷ CFU/只)溶于0.2 mL生理盐水中,腹腔注射至雄性C57BL/6小鼠(8-10周龄)。 - 给药:将莫西沙星溶于生理盐水中,每12小时静脉注射一次(20 mg/kg),持续3天(对照组:生理盐水)。 - 监测:每日记录小鼠存活情况,持续7天;分别于24小时和48小时采集血样进行细菌计数[2] 3. 大鼠肺炎模型: - 感染:将肺炎克雷伯菌(10⁶ CFU/只)溶于0.1 mL生理盐水中,经气管内感染雄性Sprague-Dawley大鼠(250-300 g)。 - 给药剂量:莫西沙星口服给药(5、10、20 mg/kg),每日一次,连续3天。- 疗效评估:采集肺组织,匀浆后接种于MHB琼脂平板上;24小时后测定细菌计数[3] |
| 药代性质 (ADME/PK) |
1. 口服吸收:- 在健康志愿者(n=12)中,单次口服莫西沙星(400 mg)的绝对生物利用度为 91%(范围:86–96%);血浆峰浓度 (Cmax) = 3.2 μg/mL(Tmax = 1.5 小时)[1]
- 食物(高脂餐)不影响吸收:与空腹相比,Cmax 和 AUC₀–∞ 的变化小于 10% [1] 2. 分布:- 分布容积 (Vd) = 3.5 L/kg(人体),表明组织渗透广泛。肺组织浓度 = 8.5 μg/g(口服 400 mg 后 2 小时),比血浆浓度高 2.7 倍 [1] - 血浆蛋白结合率 = 50%(人体,通过超滤法测定);无浓度依赖性结合(0.1–10 μg/mL)[3] 3. 代谢和排泄:- 代谢极少:口服剂量的70%以原形经粪便排出,20%经尿液排出(人体,给药后72小时)。无主要CYP450介导的代谢物[1] - 消除半衰期(t₁/₂)= 12.5小时(人体),可每日一次给药[1] 4. 特殊人群:- 在轻度至中度肾功能损害患者(肌酐清除率30–60 mL/min)中,AUC₀–∞较健康志愿者增加15%;无需调整剂量[1] |
| 毒性/毒理 (Toxicokinetics/TK) |
1. 体外毒性:- 在浓度高达 100 μg/mL 时,对人肝细胞(HepG2 细胞)无细胞毒性(IC₅₀ > 100 μg/mL,MTT 法)[6]
- 在 Ames 试验(鼠伤寒沙门氏菌 TA98、TA100 株)中,0.1–100 μg/平板剂量下无遗传毒性[3] 2. 体内毒性:- 在为期 4 周的大鼠口服毒性研究(100、300、600 mg/kg/天)中:无死亡;600 mg/kg/天剂量下肝酶(ALT/AST)轻度升高(2 周后恢复可逆)[3] - 心脏安全性:在犬遥测研究中,治疗剂量(20 mg/kg/天)下未观察到 QT 间期延长;仅在 10 倍治疗剂量(200 mg/kg/天)时观察到 QT 间期延长 [3] 3. 临床不良反应: - 常见不良事件(发生率 >5%):恶心(8%)、腹泻(6%)、头痛(5%)。罕见严重不良反应:肌腱断裂 (<0.1%)、肝毒性 (<0.5%) [1] 4. 药物相互作用: - 与华法林(抗凝血剂)无显著相互作用:与莫西沙星(400 mg/天)合用时,华法林的 AUC 变化 <5% [1] - 避免与含 Mg²⁺/Al³⁺ 的抗酸剂合用:莫西沙星的 Cmax 降低 40%(螯合作用)[1] 妊娠和哺乳期用药 ◉ 哺乳期用药概述 目前尚无关于哺乳期使用莫西沙星的信息。由于担心对婴儿发育中的关节产生不良影响,氟喹诺酮类药物传统上不用于婴儿。然而,最近的研究表明风险很小。牛奶中的钙可能阻止婴儿吸收牛奶中少量的氟喹诺酮类药物,但目前尚无足够数据证实或否定这一说法。哺乳期妇女可以使用莫西沙星,但需密切监测婴儿的胃肠道菌群,以防出现腹泻或念珠菌病(鹅口疮、尿布疹)等不良反应。然而,最好使用其他安全性信息更全面的药物。 母亲使用含有莫西沙星的滴眼液对哺乳婴儿的风险微乎其微。为大幅减少使用眼药水后进入母乳的药物量,请按压眼角泪管至少 1 分钟,然后用吸水纸巾擦去多余的药液。 ◉ 对母乳喂养婴儿的影响 截至修订日期,未找到相关的已发表信息。 ◉ 对哺乳和母乳的影响 截至修订日期,未找到相关的已发表信息。 |
| 参考文献 | |
| 其他信息 |
1. 作用机制:莫西沙星与细菌DNA促旋酶和拓扑异构酶IV的ATP结合口袋结合,阻止DNA超螺旋和松弛——这对细菌DNA复制、转录和修复至关重要。这会导致不可逆的DNA链断裂和细菌细胞死亡[3]
2. 适应症:已获准用于治疗社区获得性肺炎(CAP)、急性细菌性鼻窦炎(ABRS)、非复杂性皮肤及皮肤软组织感染(uSSSI)以及耐多药结核病(MDR-TB),作为联合疗法的一部分[1,5] 3. 耐药机制:结核分枝杆菌的耐药性源于DNA促旋酶亚基A(gyrA基因,密码子90/94)或拓扑异构酶IV亚基A(parC基因,密码子80)的突变。突变菌株的最低抑菌浓度(MIC)比野生型高8-16倍[5] 4.分析方法:采用高效液相色谱-紫外检测法(HPLC-UV,检测波长293 nm)定量测定血浆中莫西沙星的浓度:流动相为0.1%甲酸水溶液:乙腈=85:15,C18色谱柱(150×4.6 mm),定量限(LOQ)= 0.05 μg/mL [6]。 莫西沙星是一种氟喹诺酮类药物,可作为DNA拓扑异构酶II抑制剂,用作广谱抗菌剂。 另见:莫西沙星(含有活性成分)。 盐酸莫西沙星是由等摩尔量的莫西沙星和盐酸组成的盐酸盐。它是一种抗菌药物。它含有莫西沙星(1+)。 盐酸莫西沙星是一种处方抗菌药,经美国食品药品监督管理局 (FDA) 批准,用于治疗某些细菌感染,例如社区获得性肺炎、慢性支气管炎急性发作、急性鼻窦炎、鼠疫以及皮肤和腹部感染。 社区获得性肺炎是一种细菌性呼吸道感染,可能是 HIV 的机会性感染 (OI)。 盐酸莫西沙星是氟喹诺酮类抗菌抗生素的盐酸盐。莫西沙星与细菌的DNA促旋酶(拓扑异构酶II)和拓扑异构酶IV结合并抑制其活性,从而抑制敏感细菌的DNA复制和修复,最终导致细胞死亡。 一种氟喹诺酮类药物,作为DNA拓扑异构酶II抑制剂,用作广谱抗菌剂。 另见:莫西沙星(具有活性成分)。 药物适应症 慢性支气管炎急性发作、社区获得性肺炎、复杂性腹腔内感染、复杂性皮肤及皮肤软组织感染、盆腔炎、急性细菌性鼻窦炎的治疗 慢性支气管炎急性发作、社区获得性肺炎、复杂性腹腔内感染、复杂性皮肤及皮肤软组织感染、盆腔炎炎症性疾病,急性细菌性鼻窦炎的治疗 慢性支气管炎急性发作,社区获得性肺炎,复杂性腹腔内感染,复杂性皮肤及皮肤软组织感染,盆腔炎,急性细菌性鼻窦炎的治疗 慢性支气管炎急性发作,社区获得性肺炎,复杂性腹腔内感染,复杂性皮肤及皮肤软组织感染,盆腔炎,急性细菌性鼻窦炎的治疗。 本文综述了莫西沙星的活性、药代动力学、药效学、疗效、安全性、药物相互作用以及剂量和给药方法。莫西沙星是一种口服的8-甲氧基喹诺酮类抗菌药物,于1999年12月获批用于治疗急性细菌性鼻窦炎、慢性支气管炎急性细菌性加重和社区获得性肺炎。这种氟喹诺酮类药物对常见的社区获得性呼吸道病原体(肺炎链球菌、流感嗜血杆菌、卡他莫拉菌)、非典型病原体和多种厌氧菌均有效。口服莫西沙星的绝对生物利用度为90%,平均消除半衰期为12小时。该药不是肝细胞色素P-450同工酶系统的底物或抑制剂,因此避免了许多潜在的药物相互作用。莫西沙星的光毒性有限。在临床试验中,莫西沙星的临床成功率为88-97%,细菌清除率为90-97%。报告的不良反应主要为胃肠道反应(恶心、腹泻),程度为轻度至中度。莫西沙星可使QT间期平均延长6±26毫秒(平均值±标准差),因此在存在致心律失常因素的患者中应谨慎使用,并应避免与正在服用抗心律失常药物(如奎尼丁、普鲁卡因胺、胺碘酮和索他洛尔)的患者合用。标准口服剂量为每日一次,每次400毫克。肾功能不全或轻度至中度肝功能不全的患者无需调整剂量。莫西沙星是一种安全有效的抗菌药物,可用于治疗急性鼻窦炎、慢性支气管炎急性细菌性加重和社区获得性肺炎。[1] 莫西沙星是一种广谱氟喹诺酮类药物,与老一代氟喹诺酮类药物相比,它对革兰氏阳性球菌和非典型病原体的抗菌谱更广,同时对革兰氏阴性菌也保持良好的活性。莫西沙星的抗菌谱涵盖所有主要的上呼吸道和下呼吸道病原体;它是对肺炎球菌(包括耐青霉素和耐大环内酯类菌株)活性最强的氟喹诺酮类药物之一。体外研究表明,与其他一些氟喹诺酮类药物相比,莫西沙星引起的细菌耐药性发生率较低,但这需要在大规模临床研究中得到证实。与其他氟喹诺酮类药物一样,莫西沙星能够很好地渗透到呼吸道组织和体液中。该药药物相互作用的可能性较低,老年患者或肾功能或轻度肝功能损害患者无需调整剂量。大型、设计严谨的临床试验已证实口服莫西沙星对社区获得性肺炎、慢性支气管炎急性发作或急性鼻窦炎患者的疗效。每日一次服用400毫克莫西沙星,细菌学和临床治愈率均达到约90%或更高。在这些试验中,其疗效与克拉霉素、头孢呋辛酯和高剂量阿莫西林等对照药物相当或更优。服用莫西沙星的患者最常见的不良反应是胃肠道不适。莫西沙星还可能导致部分患者出现QTc间期延长;目前尚无关于高危患者QTc间期延长可能产生的临床后果的数据。与其他氟喹诺酮类药物相比,莫西沙星引起光毒性反应的倾向较低,动物实验数据表明,它引起中枢神经系统兴奋和肝毒性作用的可能性也较低。[3] |
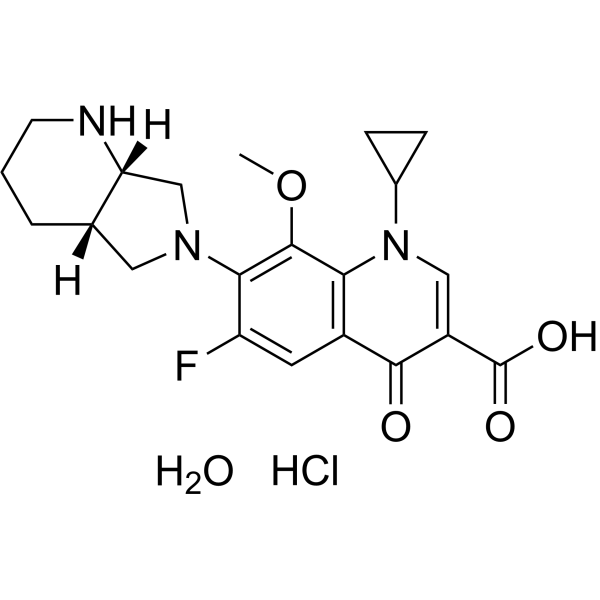
| 分子式 |
C21H27CLFN3O5
|
|---|---|
| 分子量 |
455.91
|
| 精确质量 |
455.162
|
| 元素分析 |
C, 55.32; H, 5.97; Cl, 7.78; F, 4.17; N, 9.22; O, 17.55
|
| CAS号 |
192927-63-2
|
| 相关CAS号 |
Moxifloxacin Hydrochloride;186826-86-8; 151096-09-2; 192927-63-2 (HCl hydrate) ; (Rac)-Moxifloxacin;354812-41-2;Moxifloxacin-d4;2596386-23-9;Moxifloxacin-d3 hydrochloride;2734919-98-1;Moxifloxacin-d3-1 hydrochloride;1246816-75-0;Moxifloxacin-13C,d3 hydrochloride;rac cis-Moxifloxacin-d4 hydrochloride;1217802-65-7
|
| PubChem CID |
9890250
|
| 外观&性状 |
Typically exists as solid at room temperature
|
| 熔点 |
243-246°C dec.
|
| 蒸汽压 |
4.56E-17mmHg at 25°C
|
| LogP |
3.502
|
| tPSA |
93.03
|
| 氢键供体(HBD)数目 |
4
|
| 氢键受体(HBA)数目 |
9
|
| 可旋转键数目(RBC) |
4
|
| 重原子数目 |
31
|
| 分子复杂度/Complexity |
727
|
| 定义原子立体中心数目 |
2
|
| SMILES |
Cl[H].FC1C([H])=C2C(C(C(=O)O[H])=C([H])N(C2=C(C=1N1C([H])([H])[C@]2([H])[C@@]([H])(C([H])([H])C([H])([H])C([H])([H])N2[H])C1([H])[H])OC([H])([H])[H])C1([H])C([H])([H])C1([H])[H])=O.O([H])[H]
|
| InChi Key |
SKZIMSDWAIZNDD-WJMOHVQJSA-N
|
| InChi Code |
InChI=1S/C21H24FN3O4.ClH.H2O/c1-29-20-17-13(19(26)14(21(27)28)9-25(17)12-4-5-12)7-15(22)18(20)24-8-11-3-2-6-23-16(11)10-24;;/h7,9,11-12,16,23H,2-6,8,10H2,1H3,(H,27,28);1H;1H2/t11-,16+;;/m0../s1
|
| 化学名 |
7-[(4aS,7aS)-1,2,3,4,4a,5,7,7a-octahydropyrrolo[3,4-b]pyridin-6-yl]-1-cyclopropyl-6-fluoro-8-methoxy-4-oxoquinoline-3-carboxylic acid;hydrate;hydrochloride
|
| 别名 |
Moxifloxacin hydrochloride monohydrate; 192927-63-2; Actira; DTXSID1049063; UNII-B8956S8609; B8956S8609; DTXCID2028989; 1-Cyclopropyl-6-fluoro-7-((4aS,7aS)-hexahydro-1H-pyrrolo[3,4-b]pyridin-6(2H)-yl)-8-methoxy-4-oxo-1,4-dihydroquinoline-3-carboxylic acid hydrochloride hydrate;
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples
|
|---|---|
| 溶解度 (体内实验) |
注意: 如下所列的是一些常用的体内动物实验溶解配方,主要用于溶解难溶或不溶于水的产品(水溶度<1 mg/mL)。 建议您先取少量样品进行尝试,如该配方可行,再根据实验需求增加样品量。
注射用配方
注射用配方1: DMSO : Tween 80: Saline = 10 : 5 : 85 (如: 100 μL DMSO → 50 μL Tween 80 → 850 μL Saline)(IP/IV/IM/SC等) *生理盐水/Saline的制备:将0.9g氯化钠/NaCl溶解在100 mL ddH ₂ O中,得到澄清溶液。 注射用配方 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (如: 100 μL DMSO → 400 μL PEG300 → 50 μL Tween 80 → 450 μL Saline) 注射用配方 3: DMSO : Corn oil = 10 : 90 (如: 100 μL DMSO → 900 μL Corn oil) 示例: 以注射用配方 3 (DMSO : Corn oil = 10 : 90) 为例说明, 如果要配制 1 mL 2.5 mg/mL的工作液, 您可以取 100 μL 25 mg/mL 澄清的 DMSO 储备液,加到 900 μL Corn oil/玉米油中, 混合均匀。 View More
注射用配方 4: DMSO : 20% SBE-β-CD in Saline = 10 : 90 [如:100 μL DMSO → 900 μL (20% SBE-β-CD in Saline)] 口服配方
口服配方 1: 悬浮于0.5% CMC Na (羧甲基纤维素钠) 口服配方 2: 悬浮于0.5% Carboxymethyl cellulose (羧甲基纤维素) 示例: 以口服配方 1 (悬浮于 0.5% CMC Na)为例说明, 如果要配制 100 mL 2.5 mg/mL 的工作液, 您可以先取0.5g CMC Na并将其溶解于100mL ddH2O中,得到0.5%CMC-Na澄清溶液;然后将250 mg待测化合物加到100 mL前述 0.5%CMC Na溶液中,得到悬浮液。 View More
口服配方 3: 溶解于 PEG400 (聚乙二醇400) 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.1934 mL | 10.9671 mL | 21.9342 mL | |
| 5 mM | 0.4387 mL | 2.1934 mL | 4.3868 mL | |
| 10 mM | 0.2193 mL | 1.0967 mL | 2.1934 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT05660720 | Active Recruiting |
Drug: Orelabrutinib and placebo (orelabrutinib tablet simulator) Drug: Orelabrutinib |
Healthy Subject | Beijing InnoCare Pharma Tech Co., Ltd. |
November 19, 2022 | Phase 1 |
| NCT05924815 | Active Recruiting |
Drug: Aficamten Drug: Moxifloxacin |
Healthy Participants | Cytokinetics | May 15, 2023 | Phase 1 |
| NCT03236961 | Active Recruiting |
Drug: Ertapenem Drug: Moxifloxacin |
Acute Appendicitis | Turku University Hospital | April 3, 2017 | Not Applicable |
| NCT05878522 | Active Recruiting |
Drug: moxifloxacin Drug: placebo |
Healthy | Pfizer | May 15, 2023 | Phase 1 |
| NCT04179500 | Active Recruiting |
Drug: moxifloxacin Drug: pyrazinamide |
Tuberculosis, MDR Tuberculosis |
Global Alliance for TB Drug Development |
September 16, 2021 | Phase 2 |