| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 1mg |
|
||
| Other Sizes |
|
| 靶点 |
- μ-opioid receptor (MOR) (Ki = 2.3–3.1 nM, competitive antagonist) [2]
- κ-opioid receptor (KOR) (Ki = 4.5–5.2 nM, weak competitive antagonist) [2] - δ-opioid receptor (DOR) (Ki = 12.8–14.5 nM, minimal binding affinity) [2] - No significant central nervous system (CNS) penetration (brain/plasma concentration ratio = 0.08–0.12), indicating peripheral selectivity [2] |
|---|---|
| 体外研究 (In Vitro) |
1. 阿片受体拮抗作用(外周偏向性):
- 在表达人MOR的CHO细胞中,6β-羟基纳曲酮(1–10 nM)呈剂量依赖性阻断[³H]-吗啡结合,50%抑制浓度为2.7 nM(放射性配体置换实验);其亲和力比纳曲酮(Ki = 0.15 nM)低约18倍[2]
- 在豚鼠回肠平滑肌标本(外周MOR富集组织)中,6β-羟基纳曲酮(3 nM)抑制吗啡诱导的平滑肌舒张达70%(通过等长换能器测量张力);即使在100 nM浓度下,也未观察到对吗啡诱导的中枢镇痛作用(离体脑片热板实验)的显著抑制[2] 2. 代谢物鉴定(体外生物合成): - 纳曲酮(10 μM)与人类肝脏微粒体(0.5 mg蛋白/mL)在含NADPH(1 mM)的Tris-HCl缓冲液(pH 7.4,50 mM)中37°C孵育60分钟,生成的主要代谢产物为6β-羟基纳曲酮(HPLC分析:保留时间=8.2分钟,纳曲酮保留时间=12.5分钟)[1] |
| 体内研究 (In Vivo) |
. 抑制吗啡诱导的胃肠道转运减慢:
- 雄性Sprague-Dawley大鼠(250–300 g)经吗啡(5 mg/kg,皮下注射)预处理以降低胃肠道转运后,6β-羟基纳曲酮(1、3、10 mg/kg,腹腔注射)呈剂量依赖性逆转转运抑制。在10 mg/kg剂量下,炭末推进率从吗啡单独处理组的28 ± 4%提升至72 ± 6%(6β-羟基纳曲酮+吗啡组),与对照组(75 ± 5%)相当[2]
- 对吗啡诱导的镇痛作用无显著影响(热板潜伏期:吗啡单独组=25 ± 3秒;6β-羟基纳曲酮10 mg/kg+吗啡组=23 ± 2秒),证实无中枢活性[2] 2. 人体代谢特征: - 健康男性志愿者(n=6)单次口服纳曲酮(50 mg)后,血浆中1小时内可检测到6β-羟基纳曲酮,达峰浓度(Cₘₐₓ)为85 ± 12 ng/mL(达峰时间=2.5小时),终末半衰期(t₁/₂)为12.8 ± 1.5小时[1] - 48小时内,45 ± 5%的给药纳曲酮以6β-羟基纳曲酮(游离型+葡萄糖醛酸结合型)形式从尿液排出,占尿中总代谢产物的~80%[1] |
| 酶活实验 |
1. 人肝脏微粒体介导的纳曲酮羟基化实验:
- 反应体系(总体积1 mL)包含Tris-HCl缓冲液(50 mM,pH 7.4)、人肝脏微粒体(0.5 mg蛋白/mL)、纳曲酮(10 μM)、NADPH(1 mM)和MgCl₂(5 mM)。体系在37°C振荡水浴中孵育,分别在15、30、45、60分钟时加入2 mL冰浴乙腈终止反应。离心(3000×g,15分钟)去除沉淀蛋白,上清液通过HPLC(C18柱,流动相:甲醇-水-乙酸=60:40:0.1,流速=1 mL/min,280 nm紫外检测)定量6β-羟基纳曲酮的生成量[1]
2. μ-阿片受体结合实验: - 从表达人MOR的CHO细胞中提取膜蛋白(0.1 mg蛋白/孔),与[³H]-吗啡(0.5 nM)和6β-羟基纳曲酮(0.1–100 nM)在结合缓冲液(50 mM Tris-HCl,pH 7.4,100 mM NaCl,5 mM MgCl₂)中25°C孵育90分钟。通过快速过滤(经0.5%聚乙烯亚胺预处理的玻璃纤维滤膜)去除未结合配体,滤膜用冰浴结合缓冲液洗涤3次。液体闪烁计数法检测放射性,采用Cheng-Prusoff方程计算Ki值(每个浓度设3个复孔)[2] |
| 细胞实验 |
1. 豚鼠回肠平滑肌舒张实验:
- 取豚鼠回肠段(2–3 cm),置于含Krebs-Ringer碳酸氢盐缓冲液(37°C,95% O₂/5% CO₂通气)的器官浴中,连接等长换能器(静息张力1 g)。平衡30分钟后,用乙酰胆碱(1 μM)预处理组织以建立基础张力。6β-羟基纳曲酮(0.1–10 nM)在吗啡(10 nM)给药前10分钟加入,记录60分钟内的张力变化。舒张百分比以吗啡诱导的舒张幅度为100%计算[2]
|
| 动物实验 |
1. 吗啡诱导的胃肠道转运试验(大鼠):雄性Sprague-Dawley大鼠(250–300 g)在实验前禁食18小时(自由饮水)。大鼠随机分为5组(每组n=6):(1)生理盐水组(0.9%生理盐水,1 mL/kg,腹腔注射);(2)吗啡组(5 mg/kg,皮下注射);(3)6β-纳曲醇组(1 mg/kg,腹腔注射)+吗啡组;(4)6β-纳曲醇组(3 mg/kg,腹腔注射)+吗啡组;(5)6β-纳曲醇组(10 mg/kg,腹腔注射)+吗啡组。6β-纳曲醇溶于0.1% DMSO(v/v)生理盐水中,并在吗啡给药前30分钟给药。吗啡给药30分钟后,大鼠经口灌胃给予1 mL活性炭餐(5%活性炭溶于10%阿拉伯胶)。30分钟后处死大鼠,取出整个胃肠道。胃肠道转运率计算公式为(活性炭餐通过距离/小肠总长度)× 100% [2]
2. 人体代谢物药代动力学研究:- 健康男性志愿者(n=6,年龄25-35岁,BMI 20-25 kg/m²)单次口服纳曲酮(50 mg,片剂)。分别于给药前(0)、给药后0.5、1、1.5、2、2.5、3、4、6、8、12、24、36和48小时采集静脉血样本(5 mL),置于肝素化试管中。血浆经离心(2000×g,10分钟)分离后,保存于-20°C直至分析。分别于给药后0-4、4-8、8-12、12-24、24-36和36-48小时采集尿液样本,并记录尿量。采用高效液相色谱法(HPLC)定量分析血浆和尿液中6β-纳曲醇的浓度(方法见酶法测定[1])。 |
| 药代性质 (ADME/PK) |
吸收(作为纳曲酮代谢物):在人体内,口服纳曲酮后,6β-纳曲醇迅速生成,血浆浓度在1小时内即可检测到,达峰时间(Tₘₐₓ)为2.5 ± 0.3小时[1]
- 分布:在大鼠中,6β-纳曲醇的中枢神经系统渗透性极低:腹腔注射10 mg/kg后1小时,脑组织浓度(1.2 ± 0.2 ng/g)比血浆浓度(11.8 ± 1.5 ng/mL)低约10倍[2] - 代谢:6β-纳曲醇在人肝脏中经UGT2B7进行葡萄糖醛酸化,生成6β-纳曲醇葡萄糖醛酸苷(无活性结合物),占尿液代谢物的30 ± 4%[1] 排泄:在人体内,45 ± 5% 的纳曲酮给药剂量在 48 小时内以 6β-纳曲醇(20 ± 3% 为游离形式,25 ± 2% 为葡萄糖醛酸苷结合物)的形式经尿液排出 [1] - 半衰期:6β-纳曲醇在人体血浆中的末端半衰期 (t₁/₂) 为 12.8 ± 1.5 小时,比纳曲酮(t₁/₂ = 4–6 小时)长约 2.5 倍 [1] |
| 毒性/毒理 (Toxicokinetics/TK) |
血浆蛋白结合率:在人血浆中,6β-纳曲醇的蛋白结合率为65 ± 5%(通过超滤法测定:将血浆样本加入[³H]-6β-纳曲醇,以10,000×g离心30分钟,定量滤液中的放射性)[2]
- 急性毒性:在大鼠中,单次腹腔注射高达30 mg/kg的6β-纳曲醇后,未观察到死亡或明显的毒性(例如,嗜睡、体重减轻)[2] - 无显著肝毒性:在人体志愿者中,纳曲酮给药(以及随后的6β-纳曲醇生成)后48小时内,血浆ALT/AST水平保持在正常范围内(ALT < 40 U/L,AST < 35 U/L)[1] - 药物相互作用:未观察到显著的抑制作用在用 6β-纳曲醇 (1–100 μM) 处理的人肝微粒体中观察到了 CYP450 酶(CYP1A2、2C9、2C19、2D6、3A4)[2] |
| 参考文献 |
|
| 其他信息 |
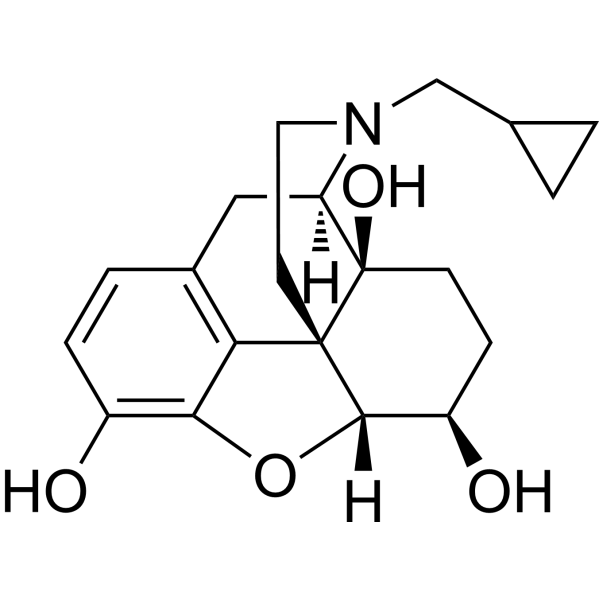
背景:6β-纳曲醇是纳曲酮的主要人体代谢产物,于1975年首次通过肝微粒体孵育和高效液相色谱/质谱(HPLC/MS)分析分离鉴定(分子量=341 g/mol,熔点=168–170°C)[1]
- 外周选择性机制:6β-羟基增加了化合物的极性,与纳曲酮(非羟基化)相比,降低了其通过血脑屏障(BBB)的被动扩散,从而优先作用于外周阿片受体[2] - 潜在临床应用:由于其外周选择性,6β-纳曲醇正被探索用于治疗阿片类药物引起的便秘(OIC)——阿片类镇痛药的常见副作用——而不会逆转中枢镇痛作用(纳曲酮的局限性)[2] - 生物合成途径:在人体内,纳曲酮在肝脏 CYP3A4 和 CYP2D6 酶的作用下于 6β 位羟基化,其中 CYP3A4 贡献了约 70% 的 6β-纳曲醇生成 [1] 6α-纳曲醇是菲类化合物的一员。 |
| 分子式 |
C20H25NO4
|
|---|---|
| 分子量 |
343.42
|
| 精确质量 |
343.178
|
| 元素分析 |
C, 69.95; H, 7.34; N, 4.08; O, 18.63
|
| CAS号 |
49625-89-0
|
| 相关CAS号 |
55488-86-3 (HCl); 49625-89-0
|
| PubChem CID |
5486554
|
| 外观&性状 |
Typically exists as solid at room temperature
|
| 密度 |
1.48g/cm3
|
| 沸点 |
557.5ºC at 760mmHg
|
| 熔点 |
90-96ºC
|
| 闪点 |
291ºC
|
| 折射率 |
1.719
|
| LogP |
1.255
|
| tPSA |
73.16
|
| 氢键供体(HBD)数目 |
3
|
| 氢键受体(HBA)数目 |
5
|
| 可旋转键数目(RBC) |
2
|
| 重原子数目 |
25
|
| 分子复杂度/Complexity |
582
|
| 定义原子立体中心数目 |
5
|
| SMILES |
C1CC1CN1CC[C@]23[C@@H]4[C@@H](CC[C@@]2(O)[C@H]1CC1=C3C(O4)=C(C=C1)O)O
|
| InChi Key |
JLVNEHKORQFVQJ-PYIJOLGTSA-N
|
| InChi Code |
InChI=1S/C20H25NO4/c22-13-4-3-12-9-15-20(24)6-5-14(23)18-19(20,16(12)17(13)25-18)7-8-21(15)10-11-1-2-11/h3-4,11,14-15,18,22-24H,1-2,5-10H2/t14-,15-,18+,19+,20-/m1/s1
|
| 化学名 |
(4R,4aS,7R,7aR,12bS)-3-(cyclopropylmethyl)-1,2,4,5,6,7,7a,13-octahydro-4,12-methanobenzofuro[3,2-e]isoquinoline-4a,7,9-triol
|
| 别名 |
6beta-Naltrexol; 49625-89-0; beta-Naltrexol; AIKO-150; 6beta-Hydroxynaltrexone; DTXSID80197942; J0W963M37T; .BETA.-NALTREXOL;
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
DMSO: ~100 mg/mL (291 mM)
|
|---|---|
| 溶解度 (体内实验) |
注意: 如下所列的是一些常用的体内动物实验溶解配方,主要用于溶解难溶或不溶于水的产品(水溶度<1 mg/mL)。 建议您先取少量样品进行尝试,如该配方可行,再根据实验需求增加样品量。
注射用配方
注射用配方1: DMSO : Tween 80: Saline = 10 : 5 : 85 (如: 100 μL DMSO → 50 μL Tween 80 → 850 μL Saline)(IP/IV/IM/SC等) *生理盐水/Saline的制备:将0.9g氯化钠/NaCl溶解在100 mL ddH ₂ O中,得到澄清溶液。 注射用配方 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (如: 100 μL DMSO → 400 μL PEG300 → 50 μL Tween 80 → 450 μL Saline) 注射用配方 3: DMSO : Corn oil = 10 : 90 (如: 100 μL DMSO → 900 μL Corn oil) 示例: 以注射用配方 3 (DMSO : Corn oil = 10 : 90) 为例说明, 如果要配制 1 mL 2.5 mg/mL的工作液, 您可以取 100 μL 25 mg/mL 澄清的 DMSO 储备液,加到 900 μL Corn oil/玉米油中, 混合均匀。 View More
注射用配方 4: DMSO : 20% SBE-β-CD in Saline = 10 : 90 [如:100 μL DMSO → 900 μL (20% SBE-β-CD in Saline)] 口服配方
口服配方 1: 悬浮于0.5% CMC Na (羧甲基纤维素钠) 口服配方 2: 悬浮于0.5% Carboxymethyl cellulose (羧甲基纤维素) 示例: 以口服配方 1 (悬浮于 0.5% CMC Na)为例说明, 如果要配制 100 mL 2.5 mg/mL 的工作液, 您可以先取0.5g CMC Na并将其溶解于100mL ddH2O中,得到0.5%CMC-Na澄清溶液;然后将250 mg待测化合物加到100 mL前述 0.5%CMC Na溶液中,得到悬浮液。 View More
口服配方 3: 溶解于 PEG400 (聚乙二醇400) 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.9119 mL | 14.5594 mL | 29.1189 mL | |
| 5 mM | 0.5824 mL | 2.9119 mL | 5.8238 mL | |
| 10 mM | 0.2912 mL | 1.4559 mL | 2.9119 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。