| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 5mg |
|
||
| Other Sizes |
|
| 靶点 |
Zuclomiphene acts as an estrogen receptor antagonist, binding to cytoplasmic and nuclear estrogen receptors [3]
|
|---|---|
| 体外研究 (In Vitro) |
在鸡输卵管制备物中,珠氯米芬(Zuclomiphene)通过与雌激素竞争结合胞质和核雌激素受体而发挥抗雌激素活性。它能抑制输卵管中雌激素诱导的反应,表现为雌激素依赖性生物活性降低 [3]
|
| 体内研究 (In Vivo) |
在雄性小鼠中,给予珠氯米芬(Zuclomiphene)(100 μg/天,皮下注射)28天,与对照组相比,睾丸重量显著增加。它还会导致附睾重量增加,并影响精子参数,包括精子数量和活力的变化。此外,它可调节生殖组织形态,包括曲细精管结构的改变 [1]
|
| 细胞实验 |
在鸡输卵管胞质和核组分实验中,将珠氯米芬(Zuclomiphene)与这些组分在放射性标记雌激素存在的条件下共同孵育。通过测量放射性标记雌激素的置换来评估珠氯米芬(Zuclomiphene)与雌激素受体的结合,从而量化其对受体的亲和力 [3]
|
| 动物实验 |
在雄性小鼠研究中,成年雄性小鼠皮下注射祖氯米芬,剂量为100 μg/天,持续28天。对照组注射赋形剂。治疗结束后,处死小鼠,并采集生殖组织(睾丸、附睾)用于称重、组织学分析和精子参数评估[1]
|
| 药代性质 (ADME/PK) |
吸收、分布和排泄
基于早期对14C标记的氯米芬的研究,该药物在人体内易于口服吸收。 基于早期对14C标记的枸橼酸氯米芬的研究,该药物在人体内易于口服吸收,并主要经粪便排泄。平均尿排泄率约为8%,粪便排泄率约为42%。 皮下注射14C标记的枸橼酸氯米芬……分布于雌性新生豚鼠的组织中……雌激素反应组织对14C表现出高亲和力。 (14)C 水平在子宫内保持稳定……在卵巢和血浆中下降……在肾上腺中升高。/氯米芬柠檬酸盐/ 约一半的摄入剂量在五天内排出;给药后六周内,粪便中仍可见微量药物。/氯米芬柠檬酸盐/ 口服氯米芬后吸收良好。药物及其代谢物主要经粪便排出,少量经尿液排出。较长的血浆半衰期(约 5 至 7 天)主要是由于血浆蛋白结合、肠肝循环和在脂肪组织中的蓄积。也可能产生半衰期长的活性代谢物。 代谢/代谢物 肝脏 将非甾体类抗雌激素氯米芬与大鼠肝微粒体孵育,结果生成了4-羟基、N-去乙基和N-氧化物代谢物,这与之前用兔微粒体进行类似实验的结果形成鲜明对比,后者仅检测到前两种代谢物。口服氯米芬后,未检测到药物或其代谢物的尿液排泄。 4-羟基氯米芬是粪便提取物中唯一可检测到的消除产物。 生物半衰期 5-7天 在健康志愿者单次口服氯米芬柠檬酸盐(其中含有异构体祖氯米芬)后,祖氯米芬的消除半衰期比另一种异构体(恩氯米芬)更长。它在血浆中持续存在较长时间,给药后数周仍可检测到[2] |
| 毒性/毒理 (Toxicokinetics/TK) |
肝毒性
关于氯米芬治疗期间血清转氨酶水平的信息很少,因为氯米芬通常仅以低剂量短期使用。有少数服用氯米芬的患者出现轻度血清酶升高的报道,但尚无确凿证据表明其会导致特异性、临床上明显的肝损伤。 用于治疗女性不孕症的药物通常通过刺激卵巢卵泡发挥作用,这可能导致卵巢过度刺激综合征(OHSS),有时可伴有血清酶升高甚至黄疸。该综合征通常在促性腺激素或氯米芬刺激卵巢后4至14天内出现,其特征是腹痛和腹胀,伴有腹水、卵巢增大和卵巢囊肿。可能出现明显的体液转移,导致血液浓缩,并迅速出现严重的腹水和胸腔积液。 25%至40%的卵巢过度刺激综合征(OHSS)患者会出现肝功能异常,通常表现为丙氨酸氨基转移酶(ALT)和天冬氨酸氨基转移酶(AST)轻度至中度升高,而血清胆红素和碱性磷酸酶水平升高不明显或无升高。肝功能异常会随着OHSS的消退而恢复正常,通常在发病后2至3周内。严重OHSS可危及生命,但死亡通常是由于脱水、休克和败血症,而非肝功能衰竭。在肝酶异常的典型病例中,肝脏组织学检查显示非特异性改变,包括肝窦扩张、轻度脂肪堆积以及以巨噬细胞和淋巴细胞为主的局灶性炎症浸润。与人绒毛膜促性腺激素 (hCG) 诱导排卵相比,使用氯米芬发生卵巢过度刺激综合征 (OHSS) 的概率较低。 可能性评分:C(可能是卵巢过度刺激综合征中临床表现明显的肝损伤的原因)。 妊娠和哺乳期影响 ◉ 哺乳期用药概述 一位女性的乳汁中检测到少量氯米芬。多项研究发现,氯米芬会抑制不愿哺乳的女性的泌乳。其作用机制似乎是降低血清催乳素水平,尤其是刺激后血清催乳素的峰值。氯米芬可能会干扰哺乳期母亲的泌乳。 ◉ 对母乳喂养婴儿的影响 一位每日服用 2.04 mg/kg 氯米芬的女性部分时间进行母乳喂养。她未观察到婴儿出现任何不良反应。 ◉ 对泌乳和母乳的影响 一项双盲研究比较了氯米芬每日50毫克,连续服用10天(n = 110)、每日100毫克,连续服用5天(n = 26)以及安慰剂(n = 41)在抑制泌乳和缓解非哺乳期产妇疼痛及乳房胀痛方面的效果。据受试者报告,两种剂量的氯米芬均优于安慰剂,但每日100毫克的剂量略优于每日50毫克的剂量。 一项研究比较了每日100毫克,连续服用5天的氯米芬(n = 60)与安慰剂(n = 30)在抑制泌乳和缓解乳房胀痛症状方面的效果。根据医生观察员的判断,产后12小时内开始服用氯米芬在所有指标上均优于产后12小时或更长时间后开始服用;两种治疗方法均优于单纯的机械措施,例如束胸。 一项随机试验比较了氯米芬50毫克每日两次,疗程14天(n=15)、溴隐亭2.5毫克每日两次,疗程14天(n=15)、己烯雌酚5毫克每日三次,疗程14天(n=15)、丙酸睾酮75毫克肌注一次(n=15)以及安慰剂每日三次口服(n=15)在降低产后血清催乳素水平和减少泌乳方面的作用。治疗三天后,氯米芬组患者的血清催乳素水平降至基线水平的65%,而溴隐亭组患者仅降至基线水平的35%。氯米芬在抑制泌乳和缓解乳房胀痛症状方面也不如溴隐亭有效。 一项研究比较了产后第一天开始服用氯米芬100毫克/天,持续7天(n=10)与安慰剂(n=12)的效果。结果显示,氯米芬在抑制泌乳或降低血清催乳素浓度方面并不比安慰剂更有效。 产后第一周不愿哺乳的妇女分别接受了氯米芬50毫克/天,每日两次(n=10)或安慰剂(n=10)治疗。服用氯米芬的妇女在使用吸奶器期间,血清催乳素水平没有高于基线值;而服用安慰剂的妇女则出现了正常的刺激后血清催乳素升高。 共有80名产后妇女参与了研究。其中40名妇女从产后第一天开始,连续5天服用氯米芬50毫克/天,每日两次; 20名产妇从产后第四天开始,每天两次服用50毫克氯米芬,疗程5天;另20名产妇服用安慰剂。所有服用氯米芬的产妇均出现泌乳抑制,乳房胀痛、不适感和血清催乳素水平降低。对于产后1天的产妇,其血清催乳素浓度在第3天显著低于基线水平;对于产后4天的产妇,其血清催乳素浓度在第5天显著低于基线水平。安慰剂组未出现泌乳抑制或血清催乳素水平降低的情况。 |
| 参考文献 |
|
| 其他信息 |
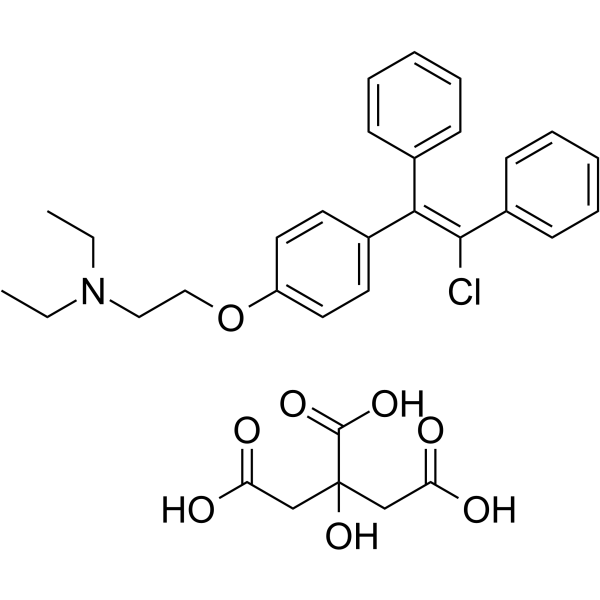
祖克洛米芬是氯米芬柠檬酸盐的几何异构体之一,氯米芬柠檬酸盐是一种三苯乙烯衍生物。其在生殖组织中的抗雌激素活性会影响男性生殖参数,包括睾丸重量和精子特征[1][3]。
根据州或联邦政府的标签要求,氯米芬柠檬酸盐可能致癌并具有发育毒性。 祖克洛米芬柠檬酸盐是氯米芬的顺式异构体,具有弱雌激素激动剂活性,并已评估其对乳腺癌的抗肿瘤活性。(NCI04) 氯米芬柠檬酸盐是氯米芬的柠檬酸盐形式,氯米芬是一种三苯乙烯类非甾体类促排卵药,已评估其对乳腺癌的抗肿瘤活性。氯米芬具有雌激素和抗雌激素的双重活性,可与雌激素竞争结合靶组织中的雌激素受体。该药物可促使垂体释放促性腺激素卵泡刺激素 (FSH) 和黄体生成素 (LH),从而导致排卵。(NCI04) 一种三苯乙烯芪衍生物,根据靶组织的不同,可作为雌激素激动剂或拮抗剂。请注意,恩克洛米芬和祖克洛米芬分别是氯米芬的 (E) 和 (Z) 异构体。 另见:枸橼酸氯米芬(注释已移至)。 |
| 分子式 |
C₃₂H₃₆CLNO₈
|
|---|---|
| 分子量 |
598.08
|
| 精确质量 |
597.213
|
| CAS号 |
7619-53-6
|
| 相关CAS号 |
Zuclomiphene-d4 citrate;2714316-71-7;Zuclomiphene-d5 citrate;1795132-80-7
|
| PubChem CID |
3033832
|
| 外观&性状 |
White to off-white solid powder
|
| LogP |
5.314
|
| tPSA |
144.6
|
| 氢键供体(HBD)数目 |
4
|
| 氢键受体(HBA)数目 |
9
|
| 可旋转键数目(RBC) |
14
|
| 重原子数目 |
42
|
| 分子复杂度/Complexity |
708
|
| 定义原子立体中心数目 |
0
|
| SMILES |
CCN(CC)CCOC1=CC=C(C=C1)/C(=C(/C2=CC=CC=C2)\Cl)/C3=CC=CC=C3.C(C(=O)O)C(CC(=O)O)(C(=O)O)O
|
| InChi Key |
PYTMYKVIJXPNBD-OQKDUQJOSA-N
|
| InChi Code |
InChI=1S/C26H28ClNO.C6H8O7/c1-3-28(4-2)19-20-29-24-17-15-22(16-18-24)25(21-11-7-5-8-12-21)26(27)23-13-9-6-10-14-23;7-3(8)1-6(13,5(11)12)2-4(9)10/h5-18H,3-4,19-20H2,1-2H3;13H,1-2H2,(H,7,8)(H,9,10)(H,11,12)/b26-25-;
|
| 化学名 |
2-[4-[(Z)-2-chloro-1,2-diphenylethenyl]phenoxy]-N,N-diethylethanamine;2-hydroxypropane-1,2,3-tricarboxylic acid
|
| 别名 |
Zuclomiphene citrate; Zuclomiphene citrate
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month 注意: 请将本产品存放在密封且受保护的环境中,避免吸湿/受潮。 |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
DMSO : ~100 mg/mL (~167.20 mM)
|
|---|---|
| 溶解度 (体内实验) |
注意: 如下所列的是一些常用的体内动物实验溶解配方,主要用于溶解难溶或不溶于水的产品(水溶度<1 mg/mL)。 建议您先取少量样品进行尝试,如该配方可行,再根据实验需求增加样品量。
注射用配方
注射用配方1: DMSO : Tween 80: Saline = 10 : 5 : 85 (如: 100 μL DMSO → 50 μL Tween 80 → 850 μL Saline)(IP/IV/IM/SC等) *生理盐水/Saline的制备:将0.9g氯化钠/NaCl溶解在100 mL ddH ₂ O中,得到澄清溶液。 注射用配方 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (如: 100 μL DMSO → 400 μL PEG300 → 50 μL Tween 80 → 450 μL Saline) 注射用配方 3: DMSO : Corn oil = 10 : 90 (如: 100 μL DMSO → 900 μL Corn oil) 示例: 以注射用配方 3 (DMSO : Corn oil = 10 : 90) 为例说明, 如果要配制 1 mL 2.5 mg/mL的工作液, 您可以取 100 μL 25 mg/mL 澄清的 DMSO 储备液,加到 900 μL Corn oil/玉米油中, 混合均匀。 View More
注射用配方 4: DMSO : 20% SBE-β-CD in Saline = 10 : 90 [如:100 μL DMSO → 900 μL (20% SBE-β-CD in Saline)] 口服配方
口服配方 1: 悬浮于0.5% CMC Na (羧甲基纤维素钠) 口服配方 2: 悬浮于0.5% Carboxymethyl cellulose (羧甲基纤维素) 示例: 以口服配方 1 (悬浮于 0.5% CMC Na)为例说明, 如果要配制 100 mL 2.5 mg/mL 的工作液, 您可以先取0.5g CMC Na并将其溶解于100mL ddH2O中,得到0.5%CMC-Na澄清溶液;然后将250 mg待测化合物加到100 mL前述 0.5%CMC Na溶液中,得到悬浮液。 View More
口服配方 3: 溶解于 PEG400 (聚乙二醇400) 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.6720 mL | 8.3601 mL | 16.7202 mL | |
| 5 mM | 0.3344 mL | 1.6720 mL | 3.3440 mL | |
| 10 mM | 0.1672 mL | 0.8360 mL | 1.6720 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。