| 规格 | 价格 | |
|---|---|---|
| 500mg | ||
| 1g | ||
| Other Sizes |
| 靶点 |
Farnesyl diphosphate synthase (IC50 = 460 nM)
|
|---|---|
| 体外研究 (In Vitro) |
阿仑膦酸钠水合物直接作用于破骨细胞时,会抑制破骨细胞功能所必需的磷脂产生的限速阶段[1]。 Alendronate Sodium Hydrate 剂量依赖性地抑制 [3H]MVA 对甾醇的摄取,同时 IPP 和 DMAPP 的剂量标志物增加 [3]。阿仑膦酸钠水合物通过降低香叶基香叶基二磷酸(一种 18-25 kDa 的蛋白质和非皂化抑制剂,包括破骨细胞中的甾醇)的水平来抑制 [3H]甲瓦龙酸内酯 [2]。
|
| 体内研究 (In Vivo) |
在兔子中,阿仑膦酸钠水合物会导致胃糜烂,但不会导致胃窦发育。阿仑膦酸钠水合物可增加由卡美辛引起的胃窦的频率和幅度。阿仑膦酸钠水合物会延迟胃愈合,并放大碳水化合物胡萝卜素的作用[4]。当与紫杉醇(10-50 mg/kg/天,每天两次或两次)联合使用时,阿仑膦酸钠水合物(0.04-0.1 mg/kg,每周两次或每周 0.1 mg/kg)部分抑制人 PC-3 ML 的骨转移用它处理的小鼠的细胞。这可导致PC-3 ML在骨髓和软组织中致命性爆发肿瘤生长,但其发生率在4-5周内显着提高[5]。
|
| 酶活实验 |
阿仑膦酸盐是一种含氮的双膦酸盐,是一种强效的骨吸收抑制剂,用于治疗和预防骨质疏松症。最近的研究结果表明,阿仑膦酸盐和其他含氮双膦酸盐抑制类异戊二烯生物合成途径,并干扰蛋白质异戊二烯化,这是由于香叶基香叶基二磷酸水平降低的结果。本研究确定法尼醇二磷酸合酶是双膦酸盐抑制的甲羟戊酸途径酶。对肝脏细胞质提取物产物的HPLC分析将阿仑膦酸盐抑制的潜在靶点(IC(50)=1700 nM)缩小到异戊烯基二磷酸异构酶和法尼基二磷酸合酶。阿仑膦酸盐抑制重组人法尼烷基二磷酸合酶,IC(50)为460 nM(预孵育15分钟后)。阿仑膦酸盐不抑制异戊烯基二磷酸异构酶或GGPP合酶,部分从肝细胞质中纯化。重组法尼烷基二磷酸合酶也被帕米膦酸二钠(IC(50)=500 nM)和利塞膦酸二钾(IC(50中)=3.9 nM)抑制,被依替膦酸二铵可忽略(IC50=80微M),而完全不被氯膦酸二钙抑制。在破骨细胞中,阿仑膦酸盐抑制了[(3)H]甲羟戊酸内酯掺入18-25 kDa的蛋白质和非脂质体,包括甾醇。这些发现(i)确定法呢酰二磷酸合酶是甲羟戊酸途径中阿仑膦酸盐的选择性靶标,(ii)表明该酶被其他含氮双膦酸盐抑制,如利塞膦酸盐,但不被氯膦酸盐抑制,支持不同双膦酸盐的不同作用机制,以及(iii)在纯化的破骨细胞中记录了阿仑膦酸酯对异戊二烯化和甾醇生物合成的抑制作用。[2]
阿仑膦酸盐(ALN)是一种用于治疗骨质疏松症和其他骨吸收疾病的氨基双膦酸盐化合物,已被认为通过抑制GGPP的形成起作用。在本研究中,我们使用大鼠肝脏的S(10)匀浆部分来证明,ALN对[(3)H]MVA掺入甾醇具有剂量依赖性抑制作用,并伴随着放射性标记掺入IPP和DMAPP的增加。我们进一步表明,ALN是细胞质反式异戊二烯基转移酶(FPP合酶)的强效抑制剂。这种抑制作用与烯丙基焦磷酸盐底物具有竞争性,但与IPP没有竞争性,这表明ALN充当烯丙基焦磷酸类似物并与游离酶结合。K(i)在0.5微米范围内。 |
| 细胞实验 |
含氮双膦酸盐被证明可以通过抑制从甲羟戊酸到胆固醇的生物合成途径中的酶来引起巨噬细胞凋亡。这项研究表明,在破骨细胞中,香叶基香叶基二磷酸(大多数GTP结合蛋白的异戊二烯化底物)可能是受这些双膦酸盐影响的关键中间体。我们报告说,洛伐他汀(羟甲基戊二酰辅酶A还原酶抑制剂)和阿仑膦酸盐都能抑制培养中的小鼠破骨细胞形成。洛伐他汀的作用被甲羟戊酸完全阻断,而香叶基香叶醇的阻断效果较差,而阿仑膦酸钠的作用被甲羟戊酸部分阻断,被香叶基香叶醇更有效。阿仑膦酸钠对小鼠颅盖骨吸收的抑制作用也被甲羟戊酸阻断,而氯屈膦酸钠的抑制作用则没有。此外,洛伐他汀和阿仑膦酸钠也抑制了兔破骨细胞的形成和活性。甲羟戊酸或香叶基香叶醇可以阻止洛伐他汀的作用,而香叶基香叶醇可以防止阿仑膦酸盐的作用。法尼醇和角鲨烯没有效果。信号研究表明,洛伐他汀和阿仑膦酸盐在纯化的破骨细胞中激活了一种34kDa的激酶。洛伐他汀介导的激活被甲羟戊酸和香叶基香叶醇阻断,而阿仑膦酸钠的激活被香叶基香叶醇阻断。这些发现共同支持了阿仑膦酸盐直接作用于破骨细胞,抑制胆固醇生物合成途径中对破骨细胞功能至关重要的限速步骤的假设。外源性香叶基香叶醇可以阻止这种抑制作用,这可能是控制细胞骨架重组、囊泡融合和凋亡的GTP结合蛋白异戊二烯化所必需的,这些过程涉及破骨细胞的活化和存活[1]。
|
| 动物实验 |
非甾体抗炎药(NSAIDs)引起的胃溃疡最常见于老年女性,而老年女性也是骨质疏松症治疗的高发人群。由于一些抗骨质疏松药物被认为会刺激上消化道黏膜,我们评估了其中一种药物——阿仑膦酸钠——损伤胃黏膜的能力,以及其对啮齿动物胃溃疡严重程度和愈合的影响。我们评估了阿仑膦酸钠对吲哚美辛诱导的兔胃窦溃疡的影响,以及其对大鼠溃疡愈合和胃糜烂形成的影响。此外,我们还评估了阿仑膦酸钠对胃酸分泌、血流和前列腺素合成的影响。结果显示,阿仑膦酸钠可导致兔胃糜烂,但不会引起胃窦溃疡。然而,在最高测试剂量(80 mg)下,阿仑膦酸钠增加了吲哚美辛诱导的胃窦溃疡的发生率和溃疡面积。阿仑膦酸钠还加剧了吲哚美辛诱导的大鼠胃损伤,并延缓了胃溃疡的愈合。阿仑膦酸钠的这些作用并非由胃酸分泌、血流、前列腺素合成或吲哚美辛的药代动力学改变所致。阿仑膦酸钠对胃的损伤作用是由于其局部刺激作用,即使在口服或局部灌注后30分钟内,浓度低至4 mg/ml时即可观察到。这些结果支持了初步的临床证据,即阿仑膦酸钠可损伤胃黏膜。虽然服用该药物的患者发生胃损伤的情况可能较为罕见,但阿仑膦酸钠与非甾体抗炎药(NSAIDs)合用可能会增加溃疡的发生率或严重程度。[4]
本研究探讨了双膦酸盐类化合物阿仑膦酸钠与紫杉醇联合作用对经尾静脉注射到SCID小鼠体内的PC-3 ML亚克隆细胞的建立和生长的影响。预先用阿仑膦酸钠(每周两次,每次0.04-0.1 mg/kg;或每周一次,每次0.1 mg/kg)处理SCID小鼠,可部分抑制PC-3 ML细胞的骨转移,并导致腹膜和其他软组织肿瘤的形成。然而,对小鼠进行阿仑膦酸钠预处理(0.1 mg/kg,每周两次或每周一次),并与紫杉醇(10-50 mg/kg/天,每周两次或每周一次)联合给药,可显著抑制PC-3 ML肿瘤在骨髓和软组织中的生长,并在4-5周内显著提高生存率(p < 0.001)。体外和体内基质金属蛋白酶产生的ELISA和酶谱分析表明,阿仑膦酸钠和紫杉醇单独使用均可部分抑制基质金属蛋白酶的产生,但紫杉醇与阿仑膦酸钠联合使用可完全抑制蛋白酶的产生和释放。阿仑膦酸钠和紫杉醇的联合作用似乎抑制了SCID小鼠肿瘤的形成和生长,这可能部分是由于抑制了蛋白酶的产生和释放。[5] |
| 毒性/毒理 (Toxicokinetics/TK) |
妊娠期和哺乳期影响
◉ 哺乳期用药概述 有限的证据表明,长期服用双膦酸盐治疗后停止母乳喂养似乎不会对婴儿产生不良影响。由于目前尚无关于哺乳期使用阿仑膦酸钠的信息,因此可能更倾向于选择其他药物,尤其是在哺乳新生儿或早产儿时。然而,母乳喂养的婴儿不太可能吸收阿仑膦酸钠。如果母亲在妊娠期或哺乳期服用双膦酸盐,一些专家建议在产后前两个月监测婴儿的血清钙水平。 ◉ 对母乳喂养婴儿的影响 由于长期服用阿仑膦酸钠后,其在体内可持续存在数年,以下案例可能具有参考价值。一位女性在受孕前一年内,先服用阿仑膦酸钠6个月,然后每4个月服用一次帕米膦酸钠。她的婴儿母乳喂养了3个月(未说明喂养程度)。婴儿在2个月大时出现轻度低钙血症,但在5个月大时钙水平正常,长骨发育也正常。 ◉ 对哺乳和母乳的影响 截至修订日期,未找到相关的已发表信息。 |
| 参考文献 |
[1]. Fisher JE, et al. Alendronate mechanism of action: geranylgeraniol, an intermediate in the mevalonate pathway, prevents inhibition of osteoclast formation, bone resorption, and kinase activation in vitro. Proc Natl Acad Sci U S A. 1999 Jan 5;96(1):133-8.
[2]. Bergstrom JD, et al. Alendronate is a specific, nanomolar inhibitor of farnesyl diphosphate synthase. Arch Biochem Biophys. 2000 Jan 1;373(1):231-41. [3]. Keller RK, et al. Mechanism of aminobisphosphonate action: characterization of alendronate inhibition of the isoprenoid pathway. Biochem Biophys Res Commun. 1999 Dec 20;266(2):560-3. [4]. Elliott SN, et al. Alendronate induces gastric injury and delays ulcer healing in rodents. Life Sci. 1998;62(1):77-91. [5]. Stearns ME, et al. Effects of alendronate and taxol on PC-3 ML cell bone metastases in SCID mice. Invasion Metastasis. 1996;16(3):116-31 |
| 其他信息 |
阿仑膦酸钠是阿仑膦酸钠的钠盐,阿仑膦酸钠是一种第二代双膦酸盐,是焦磷酸盐的合成类似物,具有抗骨吸收活性。阿仑膦酸钠与香叶基转移酶(法尼基焦磷酸合成酶)结合并抑制其活性,该酶参与萜类化合物的生物合成。抑制该酶可阻止异戊二烯类脂质(FPP 和 GGPP)的生物合成,这些脂质是小 GTP 酶信号蛋白翻译后修饰过程中法尼基化和香叶基香叶基化的供体底物,而该修饰在破骨细胞的周转过程中至关重要。因此,破骨细胞活性受到抑制,骨吸收和周转减少。
一种用于治疗绝经后女性骨质疏松症的非激素类药物。这种药物可以促进骨骼健康生长,恢复因骨质疏松症造成的部分骨质流失。 另见:阿仑膦酸钠(注释已移至此处)。 药物适应症 用于治疗绝经后骨质疏松症,尤其适用于存在维生素D缺乏风险的患者。Adrovance可降低椎体和髋部骨折的风险。 |
| 分子式 |
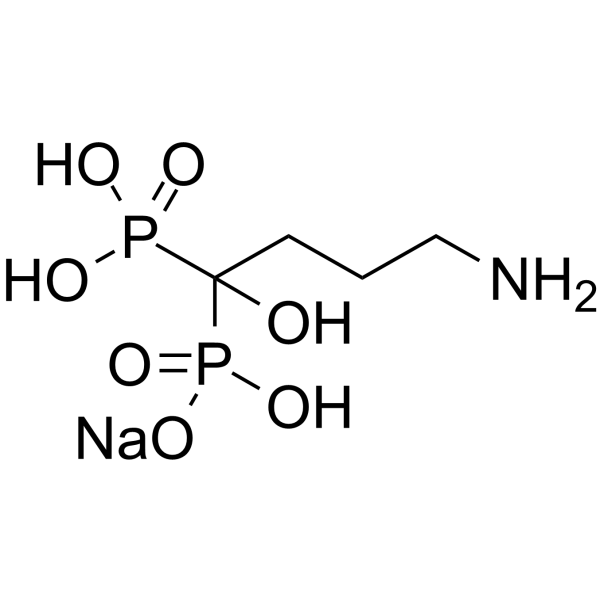
C4H12NNAO7P2
|
|---|---|
| 分子量 |
271.08
|
| 精确质量 |
270.998
|
| CAS号 |
129318-43-0
|
| 相关CAS号 |
Alendronate sodium hydrate;121268-17-5;Alendronic acid;66376-36-1
|
| PubChem CID |
16760285
|
| 外观&性状 |
Typically exists as solid at room temperature
|
| 沸点 |
616.7ºC at 760 mmHg
|
| 闪点 |
326.7ºC
|
| tPSA |
180.93
|
| 氢键供体(HBD)数目 |
5
|
| 氢键受体(HBA)数目 |
8
|
| 可旋转键数目(RBC) |
5
|
| 重原子数目 |
15
|
| 分子复杂度/Complexity |
293
|
| 定义原子立体中心数目 |
0
|
| SMILES |
C(CC(O)(P(=O)(O)O)P(=O)(O)[O-])CN.[Na+]
|
| InChi Key |
CAKRAHQRJGUPIG-UHFFFAOYSA-M
|
| InChi Code |
InChI=1S/C4H13NO7P2.Na/c5-3-1-2-4(6,13(7,8)9)14(10,11)12;/h6H,1-3,5H2,(H2,7,8,9)(H2,10,11,12);/q;+1/p-1
|
| 化学名 |
sodium;(4-amino-1-hydroxy-1-phosphonobutyl)-hydroxyphosphinate
|
| 别名 |
ALENDRONATE SODIUM; 129318-43-0; Fosamax; Binosto; Fosamac; Onclast; alendronate monosodium; Monosodium alendronate;
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples
|
|---|---|
| 溶解度 (体内实验) |
注意: 如下所列的是一些常用的体内动物实验溶解配方,主要用于溶解难溶或不溶于水的产品(水溶度<1 mg/mL)。 建议您先取少量样品进行尝试,如该配方可行,再根据实验需求增加样品量。
注射用配方
注射用配方1: DMSO : Tween 80: Saline = 10 : 5 : 85 (如: 100 μL DMSO → 50 μL Tween 80 → 850 μL Saline)(IP/IV/IM/SC等) *生理盐水/Saline的制备:将0.9g氯化钠/NaCl溶解在100 mL ddH ₂ O中,得到澄清溶液。 注射用配方 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (如: 100 μL DMSO → 400 μL PEG300 → 50 μL Tween 80 → 450 μL Saline) 注射用配方 3: DMSO : Corn oil = 10 : 90 (如: 100 μL DMSO → 900 μL Corn oil) 示例: 以注射用配方 3 (DMSO : Corn oil = 10 : 90) 为例说明, 如果要配制 1 mL 2.5 mg/mL的工作液, 您可以取 100 μL 25 mg/mL 澄清的 DMSO 储备液,加到 900 μL Corn oil/玉米油中, 混合均匀。 View More
注射用配方 4: DMSO : 20% SBE-β-CD in Saline = 10 : 90 [如:100 μL DMSO → 900 μL (20% SBE-β-CD in Saline)] 口服配方
口服配方 1: 悬浮于0.5% CMC Na (羧甲基纤维素钠) 口服配方 2: 悬浮于0.5% Carboxymethyl cellulose (羧甲基纤维素) 示例: 以口服配方 1 (悬浮于 0.5% CMC Na)为例说明, 如果要配制 100 mL 2.5 mg/mL 的工作液, 您可以先取0.5g CMC Na并将其溶解于100mL ddH2O中,得到0.5%CMC-Na澄清溶液;然后将250 mg待测化合物加到100 mL前述 0.5%CMC Na溶液中,得到悬浮液。 View More
口服配方 3: 溶解于 PEG400 (聚乙二醇400) 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 3.6889 mL | 18.4447 mL | 36.8895 mL | |
| 5 mM | 0.7378 mL | 3.6889 mL | 7.3779 mL | |
| 10 mM | 0.3689 mL | 1.8445 mL | 3.6889 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。