| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 1mg |
|
||
| 25mg |
|
||
| Other Sizes |
|
| 靶点 |
NAMPT/Nicotinamide phosphoribosyltransferase (IC50 = 0.09 nM)
|
||
|---|---|---|---|
| 体外研究 (In Vitro) |
体外活性:0.09-27 nM 的低浓度 APO866 可在 41 种血液恶性细胞中诱导剂量依赖性细胞毒性,包括急性髓系白血病 [AML]、急性淋巴细胞白血病 [ALL]、套细胞淋巴瘤 [MCL]、慢性淋巴细胞白血病 [ CLL]和T细胞淋巴瘤。 APO866 在 0-10 nM 的低浓度范围内会诱导细胞死亡,这种效应与 caspase 激活无关,但与线粒体膜的去极化有关。 APO866 的浓度范围为 0-10 nM,剂量依赖性地诱导各种血液癌细胞中细胞内 NAD 和 ATP 含量的消耗以及细胞死亡。浓度为 10 nM 的 APO866 可抑制 PBEF 诱导的 HFFF2 细胞中 MMP-3、CCL2 和 CXCL8 的分泌。细胞测定:对于 MTT 测定,将 0.5 × 106 个细胞/mL 在 96 孔板上一式三份铺板。将 APO866 (0.01 nM-100 nM) 添加到 50 μL 培养基中,仅用培养基作为对照。孵育 72 或 96 小时后,向每孔中添加 15 μL 染料溶液,并将细胞再孵育 4 小时。添加终止液(100 μL/孔)1 小时,并在分光光度计上读取 570 nm 处的吸光度。对于台盼蓝染料排除染色,在不存在或存在 APO866 的情况下,以 0.5 × 105 个细胞/孔在 6 孔板中使用 1 mL 培养基生长 96 小时。将每个样品的细胞与 10 μL 台盼蓝溶液一起孵育(以 1:1 的比例 [vol/vol] 孵育 1 分钟)。通过计算活(未染色)细胞的比例来确定细胞存活率。
通过选择性杀死 MM 细胞,(E)-Daporinad (FK866)抑制 Nampt 会导致细胞内 NAD+ 大幅减少。 MM 细胞中的基线 NAD+ 水平高于正常 PBMC,从而产生 (E)-Daporinad (FK866) 敏感性。 (E)-Daporinad (FK866) 诱导的细胞死亡与 Nampt 活性的抑制有关,而不是与蛋白质表达有关。 (E)-Daporinad (FK866) 消除了骨髓微环境的生存优势[1]。 (E)-Daporinad (FK866) 降低 Jurkat 和激活的 PBL 中 TG 响应性 Ca2+ 储存的 Ca2+ 含量,并抑制各种有丝分裂原引起的 [Ca2+]i 升高。 (E)-Daporinad (FK866) 会降低 Jurkat 细胞中 TG 响应性 Ca2+ 储备的 Ca2+ 含量,但在 Bcl2-Jurkat 细胞中不会降低 [2]。使用 p53 乙酰化途径,通过 (E)-Daporinad (FK866) 抑制 NAMPT 或通过烟酰胺抑制 SIRT 可减少增殖并导致 293T 细胞死亡[3]。 Nampt特异性化学抑制剂Daporinad (FK866)在MM细胞系和患者MM细胞中引发细胞毒性,但在正常供体和MM患者PBMCs中不会引发细胞毒性。重要的是,FK866以剂量依赖的方式引发了对传统和新型抗MM疗法耐药的MM细胞的细胞毒性,并克服了细胞因子(IL-6、IGF-1)和骨髓基质细胞的保护作用。RNAi敲除Nampt证实了其在维持MM细胞活力和细胞内NAD(+)储存中的关键作用。有趣的是,FK866的细胞毒性会触发自噬,但不会引发细胞凋亡。自噬介导的FK866 MM细胞毒性的转录依赖性(TFEB)和非依赖性(PI3K/mTORC1)激活。[1] 通过Daporinad(FK866)介导的烟酰胺磷酸核糖基转移酶抑制降低[NAD(+)](i),降低了Jurkat细胞和活化T淋巴细胞中丝裂原诱导的[Ca(2+)](i)升高。因此,在FK866存在的情况下,这些细胞中thapsigargin敏感的Ca(2+)库的Ca(++)含量大大降低。[2] 以293T细胞系(用大T抗原转化的HEK293细胞)为模型,我们提供了证据,表明p53是参与Daporinad(FK866)介导的293T细胞杀伤的关键下游靶点之一。在这些细胞中敲除p53后,凋亡率降低,S期细胞数量增加。FK866抑制NAMPT或烟酰胺抑制SIRT会降低涉及p53乙酰化途径的293T细胞的增殖并引发其死亡。此外,敲除p53减弱了FK866对细胞增殖、凋亡和细胞周期阻滞的影响。这里提供的数据揭示了两个重要事实:(1)293T细胞中的p53在NAMPT通路抑制剂FK866的存在下是活跃的;(2)FK866在293T细胞中诱导的凋亡与p53在Lys382处的乙酰化增加有关,这是p53功能活性所必需的[3]。 |
||
| 体内研究 (In Vivo) |
APO866 以 20 mg/kg 的剂量腹腔注射,每天两次,持续 4 天,每周重复一次,持续 3 周,可预防和消除人类 AML、淋巴母细胞淋巴瘤和白血病的 CB-17 SCID 小鼠异种移植模型中的肿瘤生长。 0.12 mg/kg/小时剂量的 APO866 通过抑制 CIA 小鼠的 PBEF 来防止关节破坏和白细胞浸润。
在 CB17-SCID 小鼠中,(E)-Daporinad (FK866)(30 mg/kg,腹腔注射)可减轻肿瘤负荷,并显着降低肿瘤组织中 ERK 磷酸化和 LC3 的蛋白水解裂解[1]。 Daporinad/FK866的体内抗MM疗效[1] 为了研究Daporinad/FK866对Nampt的抑制是否可以抑制体内MM细胞的生长,我们使用了皮下移植MM.1S细胞的CB17-SCID小鼠。14只荷瘤小鼠被随机分配接受30mg/kg的Daporinad/FK866腹腔注射(每天两次,连续4天,每个周期休息3天,重复3周)或载体对照。图7A显示了接受载体对照组(n=7)与治疗组(n=6)MM.1S增长的比较。与对照组小鼠相比,早在治疗的第7天就观察到肿瘤负荷显著降低,并在第21天得到证实。(分别为P=0.0061和P=0.0067)。重要的是,治疗耐受性良好,没有明显的体重减轻或神经系统变化,并导致总体生存期显著延长(图7B;P=0.0014)。对照组的中位总生存期为19.5天,而FK866治疗组为45天。收集肿瘤,对裂解物进行蛋白质印迹分析,以评估ERK和LC3B的磷酸化(图7C)。与我们的体外结果一致,与对照组相比,FK866治疗小鼠的肿瘤组织ERK磷酸化和LC3蛋白水解切割显著降低。这些结果为FK866治疗多发性骨髓瘤的研究提供了体内概念验证。 抗肿瘤活性[4] 没有发现客观的反应。在接受治疗的24名患者中,4名患者病情稳定至少3个月(前列腺4个月,黑色素瘤5个月,间皮瘤3个月,口咽5个月)。通过影像学检查,癌症前列腺患者病情稳定,但由于PSA升高,4个月后退出研究。口咽癌患者有一些临床益处,疼痛减轻。患者的CT扫描在首次疾病评估时是稳定的;然而,在5个月时出现了进展。 血管内皮生长因子测量[4] 在第二队列和更高队列的患者中测量了VEGF血清水平。在给药前、输注48小时和96小时再次记录VEGF水平。在MTD治疗的6名患者中,有5名患者的VEGF水平下降。由于收集的样本数量较少,VEGF的减少没有达到统计学意义(图1)。 小鼠静脉(IV)药代动力学(PK)研究的应用[5] 开发的LC-qTOF-MS方法成功应用于以5、10和30mg/kg的剂量静脉注射后,获得小鼠血浆中Daporinad(FK866)的PK参数。除早期时间点样品的一些PK样品外,大多数PK样品的浓度都在合格的校准曲线内。因此,早期时间点PK样品用空白小鼠血浆适当稀释,以确保每个样品浓度在校准曲线范围内。Daporinad (FK866)的浓缩时间曲线如图3所示。使用WinNonlin(版本8.0.0)通过非房室分析(NCA)计算PK参数,结果汇总在表4中。 |
||
| 酶活实验 |
小鼠和人肝微粒体中体外Met-ID的样品制备[5]
首先,通过混合NADPH溶液a和B、UDPGA、GSH和Daporinad(FK866)的工作溶液(2mg/mL)制备辅因子化合物混合物。将上述辅因子化合物混合物在37°C下预孵育5分钟。然后将380µL预孵育混合物转移到1.7 mL聚丙烯管中,并施加20µL的20 mg/mL小鼠或人肝微粒体。微粒体和辅因子化合物混合物在37°C下孵育0和120分钟,通过加入450µL ACN进行蛋白质沉淀来停止反应。在8000×g rpm下离心10分钟后,将550µL上清液转移到新鲜试管中,并在真空下使用旋转蒸发器蒸发至干。完全干燥的试管用110µL 30%ACN的DW溶液和0.1%FA复溶。复溶样品以12000×g rpm离心5分钟,其上清液转移到LC小瓶中进行体外Met-ID分析。 小鼠PK样品中体内Met-ID的样品制备[5] 对于体内Met-ID分析,分别根据汉密尔顿合并法合并30mg/kg静脉注射PK组的血浆样本。将210µL合并的血浆样品转移到聚丙烯管中,加入800µL ACN进行蛋白质沉淀。然后,将上述样品在10000×g rpm下离心10分钟,并在旋转蒸发器中真空蒸发900µL上清液至干。完全干燥的试管用110µL 30%ACN的DW溶液和0.1%FA复溶。复溶后的样品涡旋并以12000×g rpm离心5分钟,上清液转移到LC小瓶中用于体内Met-ID分析。 荧光法测定细胞内钙水平[2] PBL或Jurkat细胞(2×106/ml),无论是否用植物血凝素(PHA)(5μg/ml)刺激和/或在有或没有33nmDaporinad(FK866)或0.1mm NAM、NA或NMN的情况下处理24小时,在RPMI培养基中于37°C下用10μm FLUO-3AM或Fura-2AM加载45分钟,用含Ca2+的Hanks平衡盐溶液(HBSS)洗涤,并以2×106个细胞/ml的浓度重新悬浮在相同的溶液中。或者,在某些实验中,细胞被洗涤并重新悬浮在无Ca2+的HBSS中。在添加thapsigargin(TG)之前。在96孔板(105个细胞/孔)中用负载Fluo-3的细胞进行[Ca2+]i测量。调节基础荧光(激发,485 nm;发射,520 nm),使每个孔的基础强度相当(在±10%范围内)。每3秒用荧光板读数器测量一次荧光。将发射光的强度绘制为时间的函数。使用公式Δ/baseal×100计算每条迹线的钙变化,其中Δ是添加刺激后的最大荧光与基础荧光(基础)之间的差值,归一化为基础荧光(基本)。 将Fura-2负载的细胞接种在涂有聚赖氨酸的玻璃底细胞培养皿上,并在37°C下孵育20分钟。[Ca2+]i测量和校准使用微荧光系统进行。 细胞内NAD+和cADPR水平的测定[2] 如上所述,将PBL或Jurkat细胞培养24小时,并在存在或不存在Daporinad(FK866)(33 nm)、NAM(0.1、1或10 mm)、NA(0.1 mm)或NMN(0.1mm)的情况下,用PHA(5μg/ml)刺激或不刺激。每次孵育结束时,取出1ml细胞,在16000×g下离心15秒。细胞颗粒在4°C下用0.3ml 0.6m高氯酸溶解。细胞提取物在16000×g下离心3分钟;收集上清液,将等分试样在pH 8.0的100mm磷酸钠缓冲液中稀释200倍,以测定NAD+含量。通过将水样与4倍体积的含有1,1,2-三氯三氟乙烷和三正辛胺的溶液混合,从剩余的上清液中去除高氯酸,并测定cADPR含量。NAD+和cADPR值根据Bradford测定法测定的蛋白质浓度进行归一化。 细胞内ATP含量的测定[2] 如上所述,在存在或不存在<强>Daporinad(FK866)(33nm)、NAM(0.1mm)、NA(0.1mm。孵育结束时,取出1ml细胞,在16000×g下离心15秒。细胞颗粒在4°C下在0.3ml 0.6m高氯酸中裂解,中和的提取物通过HPLC进行分析(11)。ATP值根据Bradford测定法测定的蛋白质浓度进行归一化。 |
||
| 细胞实验 |
Daporinad (FK866)对BM旁分泌MM细胞生长的影响
在有或没有药物的情况下,MM1S细胞(2×104个细胞/孔)在BMSC包被的96孔板中培养72和96小时。通过(3H)-胸苷摄取来测量DNA合成,在培养的最后8小时内添加(3H)–胸苷(0.5μCi/孔)。
细胞死亡的特征[1] 细胞与Daporinad (FK866)(0.1nM-33nM)一起培养96小时。对于胱天蛋白酶抑制试验,在加入FK866之前,用泛胱天蛋白酶抑制剂(zVAD-fmk)、胱天蛋白酶3-(zDEVD-fmk”)和胱天蛋白酶9-(zLEHD-fmk)抑制剂预处理细胞至少2小时。为了抑制自噬,在FK866治疗前,将细胞与抑制剂渥曼青霉素(0.25μM)、LY294002(5μM),3-甲基腺嘌呤(3MA 100μM)和氯喹(20μM)一起孵育至少30分钟。根据制造商的方案,使用膜联蛋白-V–FITC染色和流式细胞术分析对细胞凋亡进行定量。 免疫荧光[1] U266和RPMI8226/S细胞用pEGFP-LC3B瞬时转染,并用载体或Daporinad(FK866)10nM处理24和48小时。使用配备Coolsnap CF彩色相机的尼康E800落射荧光显微镜记录GFP荧光。为了定量,使用10个字段,每个字段由40-100个GFP阳性细胞组成,计算GFP-LC3B斑点细胞相对于GFP阳性细胞总数的数量。 |
||
| 动物实验 |
|
||
| 药代性质 (ADME/PK) |
药代动力学[4]
达波林(FK866)及其代谢物FK866-N-氧化物的药代动力学存在较大的个体间差异。同一患者不同治疗周期间的个体内差异较小(表4和图2)。FK866和FK866-N-氧化物的稳态血药浓度(Css)均在输注开始后48小时达到;N-氧化物代谢物的Css比FK866低10倍。停止输注后,两者均迅速清除。两种化合物的稳态血药浓度(Css)均随剂量增加而升高,见表4和表5。 达波林(FK866)在最大耐受剂量(MTD)下的平均稳态血药浓度(±标准差)和AUC0-t分别为5.51 ± 2.57 ng/ml (14 nM) 和505.9 ± 249.8 ng·hr/mL。FK866的表观末端半衰期(t1/2)估计为7.9–76.5 h。FK866的稳态血药浓度可作为药物暴露量的合适预测指标,因为它与其AUC0-t以及其代谢物的稳态血药浓度和AUC0-t密切相关。根据FK866稳态血药浓度(Css)与输注速率和绝对用量之间幂方程乘数的95%置信区间,FK866的药代动力学被认为大致呈剂量依赖性。 主要剂量限制性毒性——血小板减少症与药物浓度的关系如图3所示。该图显示,随着达波林(FK866)浓度的增加,血小板计数呈比例下降。进一步比较血液学参数(特别是淋巴细胞计数和血红蛋白)与FK866水平,证实了FK866与毒性之间的剂量关系(数据未显示)。 达波林(FK866)是烟酰胺磷酸核糖转移酶(NAMPT)的高特异性抑制剂之一,其独特的作用机制可诱导肿瘤细胞凋亡。本研究开发了一种简便灵敏的液相色谱-四极杆-飞行时间质谱(LC-qTOF-MS)分析方法,用于评价达波瑞那在小鼠体内的药物代谢和药代动力学(DMPK)特性。采用乙腈(ACN)进行简单的蛋白质沉淀法进行样品前处理,预处理后的样品经C18色谱柱分离。校准曲线的浓度范围为1.02~2220 ng/mL,采用二次回归(加权1/浓度²)进行拟合,相关系数≥0.99。质控样品的准确度和精密度均在±25%以内,符合验收标准。对5倍、10倍和30倍稀释进行了稀释完整性验证,稀释质控样品的准确度和精密度也均在标称值的±25%以内。稳定性结果表明,达波林在以下条件下稳定:短期(4 小时)、长期(2 周)和冻融循环(3 次)。该合格方法已成功应用于达波林在小鼠体内 5、10 和 30 mg/kg 剂量下的静脉注射药代动力学 (PK) 研究。结果显示,在 5 至 10 mg/kg 剂量范围内,达波林的药代动力学呈线性趋势,而在 30 mg/kg 剂量下则呈非线性趋势。此外,还进行了体外和体内代谢物鉴定 (Met ID) 研究,以了解达波林的药代动力学特性。结果表明,在我们的实验条件下,共鉴定出 25 种代谢物,涉及 10 种不同的代谢类型。总之,本研究成功开发了LC-qTOF-MS分析方法,用于定量分析小鼠血浆中的达波林(Daporinad)及其体外和体内代谢物。[5] 本研究开发并验证了一种LC-qTOF-MS分析方法,用于定量分析小鼠血浆中的达波林(Daporinad,FK866)。使用二次回归法,在1.02至2200 ng/mL的浓度范围内,达波林的校准曲线均可接受,相关系数≥0.99。在短期(4小时)、冻融(3次)和长期(2周)等几种初步稳定性试验条件下,达波林在小鼠血浆中均保持稳定,并达到了稀释完整性。该方法已成功应用于定量分析体内静脉注射达波林(IV)的小鼠血浆药代动力学(PK)样品。 药代动力学结果表明,达波林的清除率较低至中等,具体数值取决于5至30 mg/kg的给药剂量范围。有趣的是,在10至30 mg/kg的剂量范围内,Cmax与剂量呈比例关系,但AUC似乎呈超比例增加。关于这一结果,有几种可能性。基于清除机制,我们推测与达波林消除途径相关的代谢酶或转运蛋白可能发挥作用。这促使我们开展体外和体内代谢物鉴定(MetID)研究,结果在目前的实验条件下新鉴定了25种代谢物。结果表明,达波林存在10种不同的代谢途径,其中大多数为Ⅰ相代谢反应,例如酰胺水解、氧化和去饱和作用。尽管本实验鉴定出许多有趣的新代谢物,但从体内代谢物的角度来看,不同剂量水平之间未观察到显著差异(数据未显示)。因此,其他机制,例如转运蛋白饱和等,可能在我们从体内小鼠药代动力学观察到的清除率变化现象中发挥作用。为了解消除途径,需要进行半质量平衡研究等进一步实验,或进行体外转运体分析以鉴定负责的转运体。[5] 总之,我们开发了一种灵敏、简便且可重复的LC-qTOF-MS分析方法,用于评估小鼠药代动力学样品中的达泊林,并评估了达泊林及其几种新型代谢物的体外和体内代谢谱。这项研究需要进一步的实验来更好地了解达泊林的体内清除机制。 |
||
| 毒性/毒理 (Toxicokinetics/TK) |
毒性[4]
毒性定义为至少可能与研究药物相关的不良事件。达波林(FK866)总体耐受性良好,唯一的剂量限制性毒性(DLT)是血小板减少症(低于25,000/μl)。该毒性在0.144 mg/m2/h剂量组的两例患者和0.126 mg/m2/h剂量组的一例患者中出现。此外,淋巴细胞计数也持续下降。然而,淋巴细胞减少症从未超过3级,且未发生机会性感染。除一例1级中性粒细胞减少症患者外,未观察到其他中性粒细胞减少症。非血液学毒性相对少见且程度较轻。出现一例3级疲乏和两例3级恶心/呕吐。使用五种HT3受体拮抗剂后,恶心和呕吐症状得到良好控制。唯一其他3级毒性反应是高血糖。所有2级或以上不良事件均按队列列于表3中。一名患者在研究期间发生脑血管意外;经评估,该事件与治疗无关。患者未主诉视力下降,且重复眼科检查(包括ERG)未显示视网膜病变迹象。研究期间未发生治疗相关死亡。 毒性反应和最大耐受剂量[4] 接受0.144 mg/m²/h剂量治疗的5名患者中有2名出现血小板减少相关的剂量限制性毒性(DLT)。这两名患者均接受了血小板输注,并恢复良好。根据降阶方案,随后对另一队列患者进行了0.108 mg/m²/h剂量的治疗。该队列未出现DLT,因此后续剂量递增试验测试了0.126 mg/m²/h的中间剂量。在此剂量水平下,六分之一的患者出现剂量限制性毒性(血小板减少症)。因此,该剂量为最大耐受剂量。 |
||
| 参考文献 |
|
||
| 其他信息 |
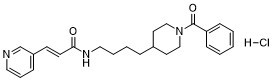
FK-866 属于苯甲酰胺类和 N-酰基哌啶类化合物。
达波林钠已用于黑色素瘤、皮肤 T 细胞淋巴瘤和 B 细胞慢性淋巴细胞白血病的治疗临床试验。 达波林钠是一种小分子化合物,具有潜在的抗肿瘤和抗血管生成活性。达波林钠可与烟酰胺磷酸核糖转移酶 (NMPRTase) 结合并抑制其活性,从而抑制烟酰胺(维生素 B3)合成烟酰胺腺嘌呤二核苷酸 (NAD+),这可能耗尽代谢活跃的肿瘤细胞的能量储备并诱导肿瘤细胞凋亡。此外,该药物还可能抑制肿瘤细胞产生血管内皮生长因子 (VEGF),从而抑制肿瘤血管生成。辅酶NAD+在细胞氧化还原反应中发挥着至关重要的作用,包括连接柠檬酸循环和氧化磷酸化的氧化还原反应。恶性细胞的烟酰胺腺嘌呤二核苷酸(NAD+)周转率高于正常细胞,这使得该生物合成途径成为癌症治疗的理想靶点。本研究探讨了NAD+合成限速酶Nampt在多发性骨髓瘤(MM)中的生物学作用。Nampt特异性化学抑制剂FK866可诱导MM细胞系和MM患者细胞的细胞毒性,但对正常供体和MM患者的外周血单核细胞(PBMC)无此作用。重要的是,FK866以剂量依赖的方式诱导对传统和新型抗MM疗法耐药的MM细胞的细胞毒性,并克服细胞因子(IL-6、IGF-1)和骨髓基质细胞的保护作用。通过RNAi敲低Nampt证实了其在维持MM细胞活力和细胞内NAD(+)储存中的关键作用。有趣的是,FK866的细胞毒性诱导了自噬,而非细胞凋亡。FK866的MM细胞毒性是通过转录依赖性(TFEB)和非转录依赖性(PI3K/mTORC1)的自噬激活介导的。最后,FK866在异种移植小鼠MM模型中表现出显著的抗MM活性,这与肿瘤细胞中ERK1/2磷酸化水平的下调和LC3的蛋白水解切割有关。因此,我们的数据揭示了Nampt在MM生物学中的关键作用,为一种新的靶向治疗方法奠定了基础。[1]细胞内NAD(+)水平([NAD(+)](i))在调节人T淋巴细胞的存活、细胞因子分泌以及对抗原刺激的反应能力方面发挥着重要作用。由CD38产生的NAD+衍生的Ca2+动员第二信使在T细胞活化中发挥关键作用。本文证明,T淋巴细胞内[NAD+]i的改变会影响细胞内Ca2+稳态,包括丝裂原诱导的[Ca2+]i升高和内质网Ca2+储存的补充。通过FK866介导的烟酰胺磷酸核糖转移酶抑制降低[NAD+]i,可降低Jurkat细胞和活化T淋巴细胞中丝裂原诱导的[Ca2+]i升高。相应地,在FK866存在的情况下,这些细胞中对thapsigargin敏感的Ca2+储存的Ca2+含量显著降低。当通过向外周血淋巴细胞补充 NAD(+) 前体烟酰胺、烟酸或烟酰胺单核苷酸来提高 NAD(+) 水平时,对毒胡萝卜素敏感的 Ca(2+) 储存库的 Ca(2+) 含量以及细胞对有丝分裂原的反应性(以 [Ca(2+)](i) 升高为指标)均上调。使用特异性 siRNA 表明,NAD(+) 前体诱导的 Ca(2+) 稳态变化是由 CD38 介导的,并随后通过 ADPR 介导的 TRPM2 门控发挥作用。最后,NAD(+) 前体的存在上调了重要的 T 细胞功能,例如对有丝分裂原的增殖和 IL-2 释放。[2] 组蛋白去乙酰化酶抑制剂 (HDACi) 是一类新型治疗药物,因为它们能诱导多种癌细胞的细胞毒性。通过抑制HDACs来重构基因表达程序是HDAC抑制剂发挥疗效的潜在机制。HDAC抑制剂如SAHA和VPA主要抑制I类和II类去乙酰化酶,具有强大的抗肿瘤活性,目前已进入II期临床试验。越来越多的证据表明,SIRTs是p53和FOXO3a等主要抑癌蛋白的关键调控因子,这促使人们开发出能够特异性靶向SIRTs的药物。癌细胞需要高周转率的NAD+来维持其生长,而SIRTs也需要NAD+来维持其活性,这一事实进一步凸显了FK866的重要性及其特异性靶向癌细胞的能力。本文所呈现的数据有助于理解FK866发挥抗癌作用的机制。 在最近的一篇论文中,我们发现FK866能够上调293T细胞中FOXO3a蛋白的乙酰化水平,从而诱导细胞凋亡。然而,这是首次在293T细胞中发现功能性p53的证据。293T细胞系因其与大T抗原相互作用而导致p53功能异常。总之,通过抑制NAMPT/SIRT通路增强p53乙酰化可改善大T抗原转化细胞中p53的功能活性,这对于以p53失活为特征的恶性肿瘤具有广泛的意义。[3] 背景:FK866是一种强效的NAD合成抑制剂。这项首次人体研究旨在确定96小时持续输注方案下的最大耐受剂量、毒性特征和药代动力学。材料和方法:24例对标准疗法无效的晚期实体瘤患者接受了递增剂量的FK866治疗,采用96小时持续输注,每28天给药一次。采集系列血浆样本以表征 FK866 的药代动力学。另采集血样用于测量血浆 VEGF 水平。结果:共有 12 名女性和 12 名男性,中位年龄为 61 岁(范围 34-78 岁),中位 KPS 评分为 80%,接受了为期 4 天的 FK866 输注,剂量水平分别为 0.018 mg/m2/h (n=3)、0.036 mg/m2/h (n=3)、0.072 mg/m2/h (n=3)、0.108 mg/m2/h (n=4)、0.126 mg/m2/h (n=6) 和 0.144 mg/m2/h (n=5)。血小板减少症是剂量限制性毒性,在最高剂量组的两例患者和推荐的 II 期剂量 0.126 mg/m²/h 的一例患者中观察到。除轻度淋巴细胞减少症和贫血外,未观察到其他血液学毒性。患者出现轻度疲乏和 3 级恶心;后者可通过止吐药控制,且不属于剂量限制性毒性。Css(72 小时和 96 小时血浆浓度的平均值)随剂量递增而增加。研究药物对 VEGF 血浆浓度无显著影响。未观察到客观缓解,但有四例患者病情稳定(治疗 3 个月或更长时间)。结论:推荐的 II 期剂量为 0.126 mg/m²/h,每 28 天持续输注 96 小时。FK866 的剂量限制性毒性是血小板减少症。药代动力学数据表明,随着 FK866 剂量的增加,血浆 Css 也随之增加。[4] |
| 分子式 |
C24H30CLN3O2
|
|---|---|
| 分子量 |
427.97
|
| 精确质量 |
427.202
|
| 元素分析 |
C, 67.36; H, 7.07; Cl, 8.28; N, 9.82; O, 7.48
|
| CAS号 |
1785666-54-7
|
| 相关CAS号 |
658084-64-1;201034-75-5;1785666-54-7 (HCl);1198425-96-5 (deleted);
|
| PubChem CID |
78243733
|
| 外观&性状 |
Typically exists as solid at room temperature
|
| tPSA |
62.3
|
| 氢键供体(HBD)数目 |
2
|
| 氢键受体(HBA)数目 |
3
|
| 可旋转键数目(RBC) |
8
|
| 重原子数目 |
30
|
| 分子复杂度/Complexity |
534
|
| 定义原子立体中心数目 |
0
|
| SMILES |
Cl.O=C(C1C=CC=CC=1)N1CCC(CCCCNC(/C=C/C2C=NC=CC=2)=O)CC1
|
| InChi Key |
MULSIBUGDPOSHV-CALJPSDSSA-N
|
| InChi Code |
InChI=1S/C24H29N3O2.ClH/c28-23(12-11-21-8-6-15-25-19-21)26-16-5-4-7-20-13-17-27(18-14-20)24(29)22-9-2-1-3-10-22/h1-3,6,8-12,15,19-20H,4-5,7,13-14,16-18H2,(H,26,28)1H/b12-11+
|
| 化学名 |
N-[4-(1-Benzoyl-4-piperidinyl)butyl]-3-(3-pyridinyl)-2-propenamide hydrochloride
|
| 别名 |
FK-866 Hydrochloride; APO-866 HCl; Daporinad HCl; Daporinad (hydrochloride); FK866 HCl; APO-866 hydrochloride; FK866 Hydrochloride; FK-866 HCl; FK 866 HCl
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples
|
|---|---|
| 溶解度 (体内实验) |
注意: 如下所列的是一些常用的体内动物实验溶解配方,主要用于溶解难溶或不溶于水的产品(水溶度<1 mg/mL)。 建议您先取少量样品进行尝试,如该配方可行,再根据实验需求增加样品量。
注射用配方
注射用配方1: DMSO : Tween 80: Saline = 10 : 5 : 85 (如: 100 μL DMSO → 50 μL Tween 80 → 850 μL Saline)(IP/IV/IM/SC等) *生理盐水/Saline的制备:将0.9g氯化钠/NaCl溶解在100 mL ddH ₂ O中,得到澄清溶液。 注射用配方 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (如: 100 μL DMSO → 400 μL PEG300 → 50 μL Tween 80 → 450 μL Saline) 注射用配方 3: DMSO : Corn oil = 10 : 90 (如: 100 μL DMSO → 900 μL Corn oil) 示例: 以注射用配方 3 (DMSO : Corn oil = 10 : 90) 为例说明, 如果要配制 1 mL 2.5 mg/mL的工作液, 您可以取 100 μL 25 mg/mL 澄清的 DMSO 储备液,加到 900 μL Corn oil/玉米油中, 混合均匀。 View More
注射用配方 4: DMSO : 20% SBE-β-CD in Saline = 10 : 90 [如:100 μL DMSO → 900 μL (20% SBE-β-CD in Saline)] 口服配方
口服配方 1: 悬浮于0.5% CMC Na (羧甲基纤维素钠) 口服配方 2: 悬浮于0.5% Carboxymethyl cellulose (羧甲基纤维素) 示例: 以口服配方 1 (悬浮于 0.5% CMC Na)为例说明, 如果要配制 100 mL 2.5 mg/mL 的工作液, 您可以先取0.5g CMC Na并将其溶解于100mL ddH2O中,得到0.5%CMC-Na澄清溶液;然后将250 mg待测化合物加到100 mL前述 0.5%CMC Na溶液中,得到悬浮液。 View More
口服配方 3: 溶解于 PEG400 (聚乙二醇400) 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.3366 mL | 11.6831 mL | 23.3661 mL | |
| 5 mM | 0.4673 mL | 2.3366 mL | 4.6732 mL | |
| 10 mM | 0.2337 mL | 1.1683 mL | 2.3366 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT00435084 | Completed | Drug: APO866 | B-cell Chronic Lymphocytic Leukemia | Valerio Therapeutics | February 2007 | Phase 1 Phase 2 |
| NCT00432107 | Completed | Drug: APO866 | Melanoma | Valerio Therapeutics | July 2006 | Phase 2 |
| NCT00431912 | Completed | Drug: APO866 | Cutaneous T-cell Lymphoma | Valerio Therapeutics | February 2007 | Phase 2 |
|
|---|
|
|
|
|---|
|