| 规格 | 价格 | 库存 | 数量 |
|---|---|---|---|
| 50mg |
|
||
| 100mg |
|
||
| Other Sizes |
|
| 靶点 |
ROS; DNA topoisomerase; c-Jun; COX-2
|
|---|---|
| 体外研究 (In Vitro) |
小檗碱硫酸盐通过抑制细胞分裂蛋白(FtsZ)或与DNA/RNA结合并造成DNA/RNA损伤而发挥抗菌活性[3]。小檗碱硫酸盐通过抑制TNF-α及其下游通路AP-1和NF-kB的活化而发挥抗炎活性[4]。小檗碱硫酸盐通过抑制活性氧(ROS)的产生和胱天蛋白酶的活化,激活PI3K/Akt信号通路并上调血红素加氧酶-1(HO-1)的表达而发挥神经保护活性[5]。小檗碱硫酸盐通过调节脂质和抑制胰岛素抵抗来改善代谢疾病[6]。
硫酸小檗碱(1.25-160 μM;72 小时)可能会减少四种结直肠癌细胞系的生长:LoVo、HCT116、SW480 和 HT-29[1]。使用硫酸小檗碱 (10 - 80 μM) 24 小时生成 LoVo 细胞 (1.25-160 μM;24-72)。使用流式细胞术,在用 40 μM 小檗碱处理的 LoVo 细胞上进行实验。 24 小时后,硫酸小檗碱 (10-80 μM) 会抑制细胞周期蛋白 B1、cdc2 和 cdc25c 蛋白的表达,尤其是在 80.0 μM 水平时[1]。周期分析还揭示了 G2/M 期细胞的积累。
1. 人结直肠腺癌细胞抗增殖与凋亡活性: - 在HCT116和SW480细胞中,小檗碱(10–200 μM,72小时)呈剂量依赖性抗增殖:IC₅₀分别为42.5±3.2 μM(HCT116)和51.8±4.1 μM(SW480)(MTT法)。100 μM时,增殖抑制率达85±6%(HCT116)和78±5%(SW480)[1] - Annexin V-FITC/PI染色显示,50 μM(48小时)时细胞凋亡率为38±4%(HCT116)和32±3%(SW480)(对照组为5±1%)。Western blot显示,100 μM(HCT116)时caspase-3上调3.2±0.3倍、Bax上调2.5±0.2倍、Bcl-2下调至0.4±0.1倍[1] 2. 细菌FtsZ功能抑制活性: - 在大肠杆菌FtsZ聚合实验中,小檗碱(0–100 μM)剂量依赖性抑制FtsZ组装:30 μM时抑制率达50%(光散射法)。22 μM时,可破坏大肠杆菌内FtsZ环形成(FtsZ-GFP荧光标记显微镜观察)[3] 3. 多巴胺能神经元保护活性: - 在6-羟基多巴胺(6-OHDA)诱导的SH-SY5Y细胞(人多巴胺能神经元)中,小檗碱(1–20 μM,24小时)逆转细胞活力下降:20 μM时活力从45±5%(仅6-OHDA)升至82±7%(MTT法)。同时上调血红素氧合酶-1(HO-1)蛋白3.5±0.4倍(Western blot),减少活性氧(ROS)58±6%(DCFH-DA染色)[5] 4. 代谢紊乱相关药理活性(临床体外关联): - 在人脂肪细胞中,小檗碱(50 μM,48小时)促进葡萄糖摄取42±5%(2-NBDG法),上调GLUT4表达2.1±0.3倍(qPCR)[6] |
| 体内研究 (In Vivo) |
连续十天,用硫酸小檗碱(10、30或50毫克/公斤/天)进行胃肠道灌胃可抑制体内结直肠癌的生长。 (30 和 50 毫克/公斤/天);胃肠道灌注
1. 结直肠腺癌异种移植模型抗肿瘤疗效: - 在荷HCT116皮下瘤裸鼠(肿瘤体积~100 mm³)中,小檗碱(25/50/100 mg/kg,腹腔注射,每日1次,持续21天)呈剂量依赖性肿瘤生长抑制(TGI):100 mg/kg时TGI达68±7%,肿瘤重量降低65±6%,瘤内TUNEL阳性细胞比例升至35±4%(对照组为8±2%)[1] 2. 大鼠中小檗碱有机酸盐的生物利用度: - 在Sprague-Dawley大鼠中,口服小檗碱柠檬酸盐(100 mg/kg)的生物利用度(18.2±2.1%)高于盐酸小檗碱(6.5±0.8%)。药代参数:Cmax(柠檬酸盐89.5±9.2 ng/mL vs 盐酸盐32.1±3.5 ng/mL)、Tmax(均为1.5±0.2小时)、t₁/₂(柠檬酸盐4.2±0.3小时 vs 盐酸盐3.8±0.2小时)[2] 3. 代谢紊乱临床疗效(Meta分析): - 27项随机对照试验(n=2569)显示,口服小檗碱(500–1500 mg/天,8–24周)可降低2型糖尿病或血脂异常患者的空腹血糖(FBG)1.02 mmol/L、糖化血红蛋白(HbA1c)0.51%、总胆固醇(TC)0.65 mmol/L、甘油三酯(TG)0.34 mmol/L[6] |
| 酶活实验 |
1. FtsZ聚合抑制实验:
- 重组大肠杆菌FtsZ(2 μM)在聚合缓冲液(50 mM PIPES,pH 6.8,5 mM MgCl₂,1 mM GTP)中37°C孵育,加入小檗碱(0–100 μM),通过340 nm光散射监测30分钟内聚合情况,IC₅₀定义为抑制50%最大散射的浓度。FtsZ环破坏实验中,表达FtsZ-GFP的大肠杆菌用小檗碱(0–50 μM)处理2小时,甲醛固定后荧光显微镜观察FtsZ环形成[3]
蛋白质印迹和OPTDI分析用于检测细胞周期蛋白[1] 收获LoVo细胞,在100°C的裂解缓冲液[50 mmol/L TrisCl(pH 6.8)、100 mmol/L DTT、2%SDS、0.1%溴酚蓝、10%甘油]中裂解10分钟,并在−20°C下储存。蛋白质浓度通过BCA测定法测定。将等量的蛋白质装载到SDS聚丙烯酰胺凝胶上,并将蛋白质电泳转移到PVDF膜上。使用细胞周期蛋白B1、cdc2和cdc25c的特异性一级抗体(1:200稀释)分析免疫印迹,并与辣根过氧化物酶偶联的二级抗体(1:1000稀释)孵育,并使用增强化学发光检测试剂盒观察蛋白质。通过自动图像分析系统对光密度积分(OPTDI)进行分析。将细胞周期蛋白B1、cdc2和cdc25c的表达标准化为内部对照(GAPDH)。结果以处理与对照相比的百分比表示 DNA和蛋白质合成的测量[1] 通过3H-胸苷和L-[4,5-3H]-亮氨酸(分别为60 Ci/mg分子和0.5μCi/孔)的细胞掺入来评估DNA和蛋白质合成。将分离的细胞(每孔1×105个细胞)与含有一系列浓度的黄连素的培养基一起孵育。在24小时黄连素暴露前4小时,将放射性前体加入培养物中。在培养期结束时,将培养基移到一片滤膜上;用蒸馏水洗涤细胞三次。用液体闪烁光谱法测定3H-胸苷和L-[4,5-3H]-亮氨酸的掺入量。 |
| 细胞实验 |
细胞增殖实验[1]
细胞类型:四种结直肠癌细胞系LoVo、HCT116、SW480和HT-29 测试浓度:1.25、2.5、 5、10、20、40、80 和 160μM 孵育时间: 72 小时 实验结果: 抑制四种细胞的增殖细胞系。 IC50 范围为 40.8±4.1 μM (LoVo) 至 98.6±2.9 μM (HCT116)。 细胞增殖测定[1] 细胞类型: 结直肠癌细胞系 LoVo 测试浓度: 1.25、2.5、5、10 、20、40、80 和 160 μM 孵育时间:24、48、72 小时 实验结果:诱导时间和剂量 细胞生长依赖性抑制。 72 小时时,160.0 μM 在 LoVo 细胞中诱导 71.1±1.9% 的生长抑制。 细胞周期分析[1] 细胞类型: LoVo Cell 测试浓度: 0、10、20、40 或 80 μM 孵育持续时间:24 小时 实验结果:暴露于 40.0 μM 会诱导细胞周期停滞在 G2/M 期并增加 G2 /M期群体和G1期群体逐渐减少。 蛋白质印迹分析[1] 细胞类型: LoVo Cell 测试浓度: 10、20、40 或 80 μM 孵育持续时间:24小时 实验结果:循环抑制 1. 结直肠腺癌细胞实验(HCT116/SW480): - MTT实验:细胞(5×10³/孔)用含10%胎牛血清的RPMI 1640培养,小檗碱(10–200 μM)处理72小时,加入MTT(5 mg/mL)孵育4小时,DMSO裂解后测570 nm吸光度[1] - 凋亡实验:细胞(2×10⁵/孔)用小檗碱(25–100 μM)处理48小时,Annexin V-FITC/PI染色15分钟,流式细胞术分析[1] - Western blot:细胞用RIPA缓冲液裂解,30 μg蛋白SDS-PAGE分离,抗caspase-3/Bax/Bcl-2/GAPDH抗体孵育,ECL显色[1] 2. 多巴胺能神经元实验(SH-SY5Y): - 细胞活力实验:细胞(1×10⁴/孔)用小檗碱(1–20 μM)预处理2小时,再用6-OHDA(100 μM)处理24小时,MTT法测活力[5] - ROS检测:细胞负载DCFH-DA(10 μM)30分钟,小檗碱+6-OHDA处理后,测488/525 nm荧光[5] - HO-1 Western blot:细胞用小檗碱(5–20 μM)处理24小时,裂解后抗HO-1抗体检测[5] 3. 细菌FtsZ实验(大肠杆菌): - 表达FtsZ-GFP的大肠杆菌在LB培养基中培养,小檗碱(0–50 μM)处理2小时,4%多聚甲醛固定,共聚焦显微镜观察FtsZ环[3] |
| 动物实验 |
Animal/Disease Models: 5weeks old BALB/c nu/nu (nude) mice human colorectal adenocarcinoma LoVo xenograft [gastric] versus human colorectal adenocarcinoma nude mice The inhibition rates of xenograft growth were 33.1% and 45.3% respectively [1]. 1]
Doses: 10, 30 or 50 mg/kg/day Route of Administration: gastrointestinal gavage; 10 days Experimental Results: At the doses of 30 and 50 mg/kg/day, the inhibition rates were 33.1% and 45.3% respectively. In vivo anti-tumor effect of berberine in human colorectal adenocarcinoma (LoVo)[1] The in vivo antitumor efficacy of berberine was examined using human colorectal adenocarcinoma LoVo xenografts in a nude mouse model; 1 × 107 cells were implanted subcutaneous injection (s.c.) in the flanks of 5-week-old BALB/c nu/nu mice. After the tumors were grown up to about 1,000–1,500 mm3, the mice were sacrificed and the tumors were divided into equal fragments. Fragments (6–8 mm3) of colorectal adenocarcinoma were implanted s.c. in the flanks of 5-week-old BALB/c nu/nu mice. Tumors were allowed to develop for 2 weeks. Once tumors were established, the mice were divided randomly into five groups. The berberine-treated groups (ten mice each group) received 10, 30, or 50 mg kg−1 day−1 berberine by gastrointestinal gavage for 10 consecutive days. The 5-FU-treated group (10 mice) was given 30 mg kg−1 day−1 by intraperitoneal injection for 10 consecutive days. The control group (11 mice) was given sterile water. Measurements of body weights and tumor volumes were recorded every 1–3 days until the experimental endpoint, at which the tumors were debilitating to the mice. The long axis (L) and the short axis (S) were measured, and the tumor volume (V) was calculated using the following equation: V = S × S × L/2. Once the final measurement was taken, the mice were sacrificed by cervical dislocation. The inhibitory rates were determined by comparing the volume of the control group and the treatment group: (1 − V treatment/Vcontrol). Effect of the combination of berberine and 5-FU on the growth of human colorectal adenocarcinoma (HT-29) xenografts in nude mice[1] The in vivo antitumor efficacy of the combination of berberine and 5-FU was examined using human colorectal adenocarcinoma HT-29 xenografts in a nude mouse model; 1 × 107 cells were implanted subcutaneous injection (s.c.) in the flanks of 5-week-old BALB/c nu/nu mice. After the tumors were grown up to about 1,000–1,500 mm3, the mice were sacrificed and the tumors were divided into equal fragments. Fragments (6–8 mm3) of colorectal adenocarcinoma were implanted s.c. in the flanks of 5-week-old BALB/c nu/nu mice. Tumors were allowed to develop for 3 weeks. Once tumors were established, the mice were divided randomly into four groups. The berberine-treated group (ten mice) received 50 mg kg−1 day−1 berberine by gastrointestinal gavage for 10 consecutive days. The 5-FU-treated group (10 mice) was given 30 mg kg−1 day−1 by intraperitoneal injection for 10 consecutive days. The combination group (10 mice) was given berberine and 5-FU. The control group (10 mice) was given sterile water. Measurements of body weights and tumor volumes were recorded every 3–4 days until the experimental endpoint, at which the tumors were debilitating to the mice. The long axis (L) and the short axis (S) were measured, and the tumor volume (V) was calculated using the following equation: V = S × S × L/2. Once the final measurement was taken, the mice were sacrificed by cervical dislocation. The inhibitory rates were determined by comparing the volume of the control group and the treatment group: (1 − V treatment/V control). 1. Colorectal Adenocarcinoma Xenograft Model (Nude Mice): - Animals: Male nude mice (6–8 weeks, n=8/group) [1] - Tumor Induction: 5×10⁶ HCT116 cells (1:1 PBS:Matrigel) implanted subcutaneously into right flank [1] - Dosing: Berberine dissolved in 0.9% saline, administered i.p. at 25/50/100 mg/kg once daily for 21 d; vehicle group received saline [1] - Evaluation: Tumor volume (V=0.5×length×width²) measured twice weekly; tumors harvested for weight and TUNEL staining [1] 2. Bioavailability Model (Sprague-Dawley Rats): - Animals: Male rats (200–220 g, n=6/group) [2] - Dosing: Berberine citrate/hydrochloride dissolved in 0.5% CMC-Na, administered orally at 100 mg/kg; blood collected from orbital vein at 0.25–24 h [2] - Evaluation: Plasma berberine concentration measured by HPLC; pharmacokinetic parameters (Cmax, Tmax, t₁/₂, bioavailability) calculated by DAS software [2] |
| 药代性质 (ADME/PK) |
1. Oral bioavailability of berberine salts: - In rats, the bioavailability of berberine citrate (oral, 100 mg/kg) (18.2 ± 2.1%) was higher than that of berberine hydrochloride (6.5 ± 0.8%) [2]
- Cmax: 89.5 ± 9.2 ng/mL (citrate) vs. 32.1 ± 3.5 ng/mL (hydrochloride); Tmax: 1.5 ± 0.2 h (both); half-life: 4.2 ± 0.3 h (citrate) vs. 3.8 ± 0.2 h (hydrochloride) [2] - Plasma protein binding: 85 ± 3% for berberine citrate (determined by rat plasma ultrafiltration) [2] 2. Clinical pharmacokinetics: - In healthy volunteers (n=12), oral berberine (500 (mg, hydrochloride) showed Cmax = 28.6 ± 3.1 ng/mL, Tmax = 2.0 ± 0.3 h, t₁/₂ = 5.1 ± 0.4 h, oral bioavailability = 5.2 ± 0.6% [6] Absorption, distribution and excretion...may be absorbed through the skin... /berberine/ |
| 毒性/毒理 (Toxicokinetics/TK) |
1. Clinical safety (meta-analysis): - In 27 clinical trials (n=2569), the incidence of adverse events (AEs) with berberine (500–1500 mg/day, 8–24 weeks) was low (18.3% vs. 12.5% in the control group). Common adverse events were mild gastrointestinal reactions: diarrhea (6.2%), nausea (4.1%), and abdominal discomfort (3.8%); no serious adverse events (e.g., hepatotoxicity and nephrotoxicity) were reported [6]
2. Preclinical toxicity: - No significant changes in body weight, liver function (ALT/AST), or kidney function (BUN/Cr) were observed in rats treated with berberine citrate (200 mg/kg/day, orally for 4 weeks) [2] Non-human toxicity values> Oral LD50 in rats >1 g/kg Intraperitoneal LD50 in rats 88.5 mg/kg Intramuscular LD50 in rats 14.5 mg/kg |
| 参考文献 |
|
| 其他信息 |
1. Mechanism of action: - Antitumor: induces apoptosis of colorectal adenocarcinoma cells by activating caspase-3 and Bax/Bcl-2 imbalance[1] - Antibacterial: inhibits bacterial cell division by targeting FtsZ polymerization and cyclization[3] - Neuroprotective: protects dopaminergic neurons from 6-OHDA damage by upregulating HO-1 and reducing ROS[5] - Metabolic regulation: improves insulin sensitivity by upregulating GLUT4 and reduces blood lipids by inhibiting cholesterol synthesis[6] 2. Dosage optimization principle: - The development of berberine organic acid salts (e.g., citrate) aims to enhance oral bioavailability (18.2% compared to 6.5% of hydrochloride) by increasing water solubility and reducing intestinal metabolism[2] Therapeutic use
Experimental use (veterinary): Oral administration of berberine sulfate (350-700 mg/kg) is effective in treating intestinal Candida infection in mice. Experimental Applications: Topical application of ophthalmic solutions containing Coptis chinensis complexes (such as berberine) can achieve pupil dilation, local anesthesia, and/or fluorescent staining of corneal epithelial defects and/or fluorescence measurement using applanation tonometers. /China: Previous Uses/ Bitter stomachic; antibacterial agent; antimalarial agent; antipyretic/berberine/ Has a mild local anesthetic effect on mucous membranes. /berberine/ |
| 分子式 |
C20H18NO4.1/2O4S
|
|---|---|
| 分子量 |
384.40
|
| 精确质量 |
768.199
|
| CAS号 |
316-41-6
|
| 相关CAS号 |
2086-83-1 (cation);
117-74-8 (hydroxide); 1868138-66-2 (ursodeoxycholate); 633-65-8 (chloride); 633-66-9 (hydrosulfate); 316-41-6 (sulfate);
|
| PubChem CID |
9424
|
| 外观&性状 |
YELLOW CRYSTALS
|
| LogP |
5.935
|
| tPSA |
170.24
|
| 氢键供体(HBD)数目 |
0
|
| 氢键受体(HBA)数目 |
12
|
| 可旋转键数目(RBC) |
4
|
| 重原子数目 |
55
|
| 分子复杂度/Complexity |
551
|
| 定义原子立体中心数目 |
0
|
| SMILES |
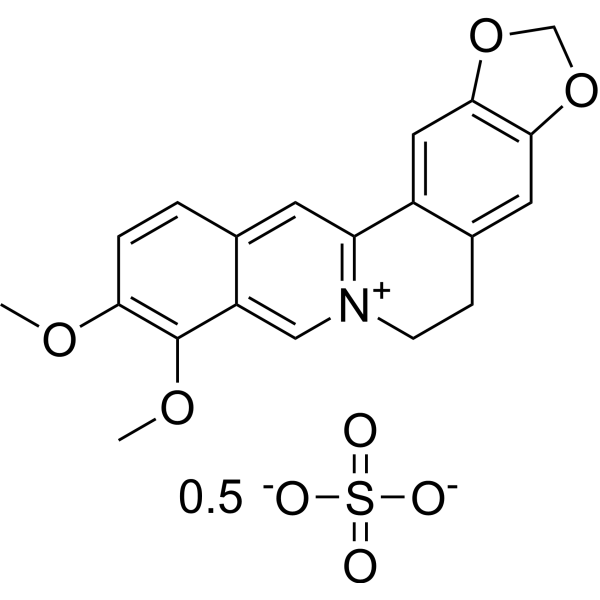
COC1=C(C2=C[N+]3=C(C=C2C=C1)C4=CC5=C(C=C4CC3)OCO5)OC.COC1=C(C2=C[N+]3=C(C=C2C=C1)C4=CC5=C(C=C4CC3)OCO5)OC.O=S(=O)([O-])[O-]
|
| InChi Key |
JISRTQBQFQMSLG-UHFFFAOYSA-L
|
| InChi Code |
InChI=1S/C20H18NO4.H2O4S/c1-22-17-4-3-12-7-16-14-9-19-18(24-11-25-19)8-13(14)5-6-21(16)10-15(12)20(17)23-2;1-5(2,3)4/h3-4,7-10H,5-6,11H2,1-2H3;(H2,1,2,3,4)/q+1;/p-2
|
| 化学名 |
16,17-dimethoxy-5,7-dioxa-13-azoniapentacyclo[11.8.0.02,10.04,8.015,20]henicosa-1(13),2,4(8),9,14,16,18,20-octaene;sulfate
|
| 别名 |
Natural Yellow 18 hemisulfate
|
| HS Tariff Code |
2934.99.9001
|
| 存储方式 |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month 注意: 请将本产品存放在密封且受保护的环境中,避免吸湿/受潮。 |
| 运输条件 |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| 溶解度 (体外实验) |
May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples
|
|---|---|
| 溶解度 (体内实验) |
注意: 如下所列的是一些常用的体内动物实验溶解配方,主要用于溶解难溶或不溶于水的产品(水溶度<1 mg/mL)。 建议您先取少量样品进行尝试,如该配方可行,再根据实验需求增加样品量。
注射用配方
注射用配方1: DMSO : Tween 80: Saline = 10 : 5 : 85 (如: 100 μL DMSO → 50 μL Tween 80 → 850 μL Saline)(IP/IV/IM/SC等) *生理盐水/Saline的制备:将0.9g氯化钠/NaCl溶解在100 mL ddH ₂ O中,得到澄清溶液。 注射用配方 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (如: 100 μL DMSO → 400 μL PEG300 → 50 μL Tween 80 → 450 μL Saline) 注射用配方 3: DMSO : Corn oil = 10 : 90 (如: 100 μL DMSO → 900 μL Corn oil) 示例: 以注射用配方 3 (DMSO : Corn oil = 10 : 90) 为例说明, 如果要配制 1 mL 2.5 mg/mL的工作液, 您可以取 100 μL 25 mg/mL 澄清的 DMSO 储备液,加到 900 μL Corn oil/玉米油中, 混合均匀。 View More
注射用配方 4: DMSO : 20% SBE-β-CD in Saline = 10 : 90 [如:100 μL DMSO → 900 μL (20% SBE-β-CD in Saline)] 口服配方
口服配方 1: 悬浮于0.5% CMC Na (羧甲基纤维素钠) 口服配方 2: 悬浮于0.5% Carboxymethyl cellulose (羧甲基纤维素) 示例: 以口服配方 1 (悬浮于 0.5% CMC Na)为例说明, 如果要配制 100 mL 2.5 mg/mL 的工作液, 您可以先取0.5g CMC Na并将其溶解于100mL ddH2O中,得到0.5%CMC-Na澄清溶液;然后将250 mg待测化合物加到100 mL前述 0.5%CMC Na溶液中,得到悬浮液。 View More
口服配方 3: 溶解于 PEG400 (聚乙二醇400) 请根据您的实验动物和给药方式选择适当的溶解配方/方案: 1、请先配制澄清的储备液(如:用DMSO配置50 或 100 mg/mL母液(储备液)); 2、取适量母液,按从左到右的顺序依次添加助溶剂,澄清后再加入下一助溶剂。以 下列配方为例说明 (注意此配方只用于说明,并不一定代表此产品 的实际溶解配方): 10% DMSO → 40% PEG300 → 5% Tween-80 → 45% ddH2O (或 saline); 假设最终工作液的体积为 1 mL, 浓度为5 mg/mL: 取 100 μL 50 mg/mL 的澄清 DMSO 储备液加到 400 μL PEG300 中,混合均匀/澄清;向上述体系中加入50 μL Tween-80,混合均匀/澄清;然后继续加入450 μL ddH2O (或 saline)定容至 1 mL; 3、溶剂前显示的百分比是指该溶剂在最终溶液/工作液中的体积所占比例; 4、 如产品在配制过程中出现沉淀/析出,可通过加热(≤50℃)或超声的方式助溶; 5、为保证最佳实验结果,工作液请现配现用! 6、如不确定怎么将母液配置成体内动物实验的工作液,请查看说明书或联系我们; 7、 以上所有助溶剂都可在 Invivochem.cn网站购买。 |
| 制备储备液 | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.6015 mL | 13.0073 mL | 26.0146 mL | |
| 5 mM | 0.5203 mL | 2.6015 mL | 5.2029 mL | |
| 10 mM | 0.2601 mL | 1.3007 mL | 2.6015 mL |
1、根据实验需要选择合适的溶剂配制储备液 (母液):对于大多数产品,InvivoChem推荐用DMSO配置母液 (比如:5、10、20mM或者10、20、50 mg/mL浓度),个别水溶性高的产品可直接溶于水。产品在DMSO 、水或其他溶剂中的具体溶解度详见上”溶解度 (体外)”部分;
2、如果您找不到您想要的溶解度信息,或者很难将产品溶解在溶液中,请联系我们;
3、建议使用下列计算器进行相关计算(摩尔浓度计算器、稀释计算器、分子量计算器、重组计算器等);
4、母液配好之后,将其分装到常规用量,并储存在-20°C或-80°C,尽量减少反复冻融循环。
计算结果:
工作液浓度: mg/mL;
DMSO母液配制方法: mg 药物溶于 μL DMSO溶液(母液浓度 mg/mL)。如该浓度超过该批次药物DMSO溶解度,请首先与我们联系。
体内配方配制方法:取 μL DMSO母液,加入 μL PEG300,混匀澄清后加入μL Tween 80,混匀澄清后加入 μL ddH2O,混匀澄清。
(1) 请确保溶液澄清之后,再加入下一种溶剂 (助溶剂) 。可利用涡旋、超声或水浴加热等方法助溶;
(2) 一定要按顺序加入溶剂 (助溶剂) 。